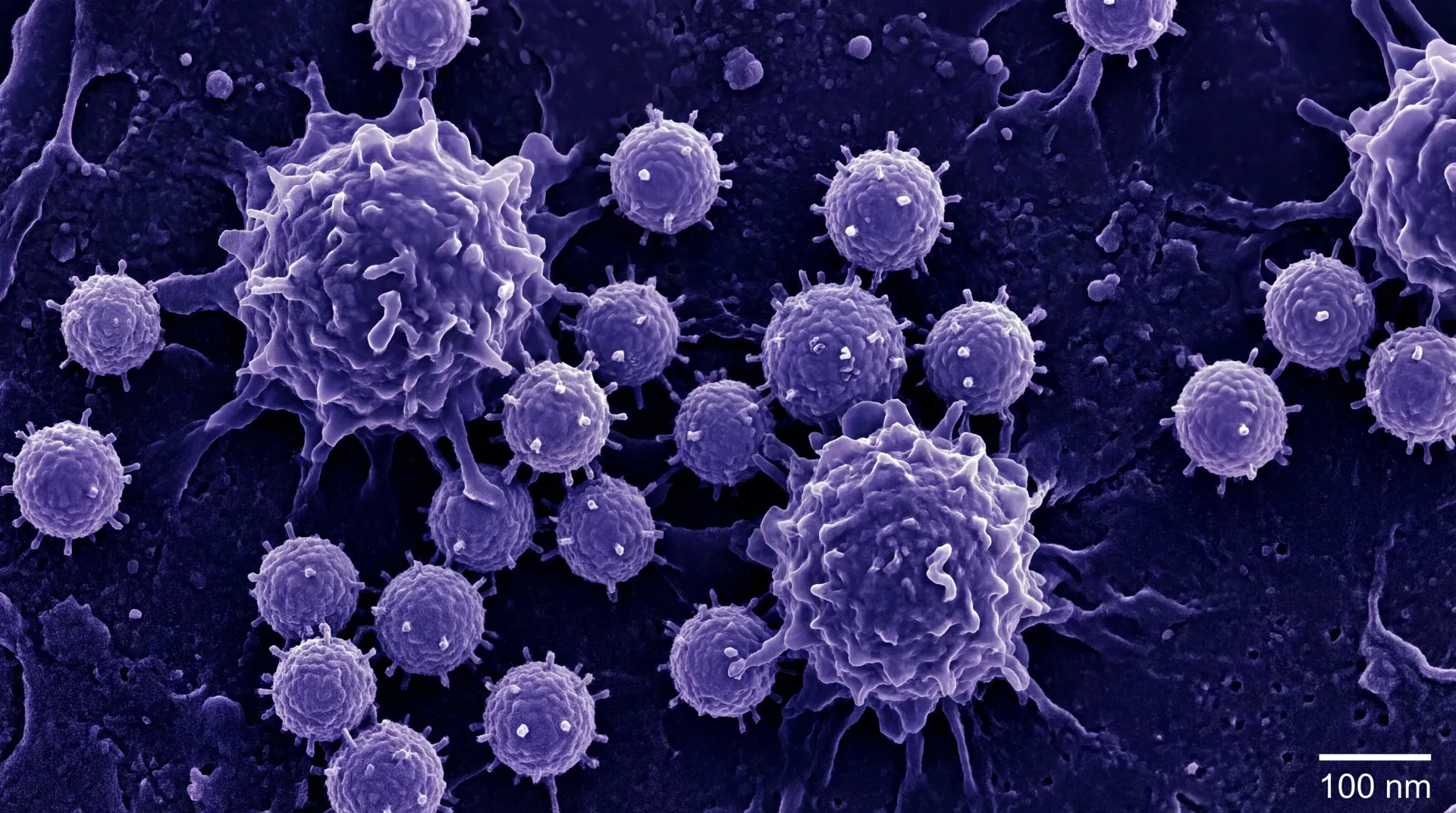
What Is Epstein-Barr Virus?
Epstein-Barr virus (EBV), also known as human herpesvirus 4, is one of the most common viruses in the world. First discovered in 1964 by Michael Anthony Epstein and Yvonne Barr, this member of the herpesvirus family has a unique ability to establish lifelong latent infection in B lymphocytes, the white blood cells responsible for producing antibodies.
Unlike many viruses that your body clears completely, EBV takes up permanent residence in your immune cells after the initial infection. It typically remains dormant, kept in check by a healthy immune system, but can reactivate during periods of stress, illness, or immune suppression. This lifelong persistence is what makes EBV particularly significant for long-term health.
Quick Fact: EBV spreads primarily through saliva, earning infectious mononucleosis the nickname "the kissing disease." It can also be transmitted by sharing utensils, drinks, or toothbrushes.
The virus primarily infects two cell types: B lymphocytes (immune cells) and epithelial cells lining the throat and nasal passages. Once inside B cells, EBV can manipulate the cell's normal growth controls, which is part of why the virus has been linked to certain cancers and autoimmune conditions. After an initial active infection, the virus retreats into a latent state within memory B cells, where it can persist for decades without causing symptoms. Maintaining a strong immune system through proper nutrition and lifestyle habits plays an important role in keeping EBV dormant.
Over 90% of Adults Carry This Virus
EBV is remarkably widespread. According to the Centers for Disease Control and Prevention, more than 90% of adults worldwide carry evidence of past EBV infection. In the United States, approximately half of all children are infected by age five, and the vast majority of the remaining population contracts the virus during adolescence or early adulthood.
The timing of infection matters more than you might think. In developing countries, most children encounter EBV early in life, when the infection is typically asymptomatic or causes only mild symptoms indistinguishable from a common cold. In developed nations, a larger proportion of people avoid infection until their teenage or young adult years, when the virus is far more likely to cause symptomatic infectious mononucleosis.
| Age Group | Infection Pattern | Symptom Likelihood |
|---|---|---|
| Under 5 years | Early childhood infection | Usually asymptomatic |
| 5-10 years | Gradual seroconversion | Mild or no symptoms |
| 11-19 years | Peak symptomatic mono | ~25% develop clinical mono |
| 20-29 years | Late primary infection | Moderate to severe mono |
| 30+ years | Rare new infection | Varies; reactivation possible |
Interestingly, research tracking EBV seroprevalence among U.S. college freshmen found a declining trend, with antibody positivity dropping from 64% in the class of 2010 to 52% in the class of 2025. This shift means more young adults may be encountering EBV for the first time during college, potentially leading to more cases of symptomatic mononucleosis on campuses.
Recognizing the Symptoms: From Mono to Chronic Fatigue
EBV infection presents differently depending on when you contract it and the state of your immune system. The most well-known manifestation is infectious mononucleosis, but EBV can also cause chronic symptoms that persist long after the initial infection.
Acute Mononucleosis
After an incubation period of four to six weeks, acute mono typically presents with a combination of these symptoms:
- Extreme fatigue that can last weeks to months
- High fever (101-104°F / 38.3-40°C)
- Severe sore throat often mistaken for strep
- Swollen lymph nodes in the neck and armpits
- Enlarged tonsils sometimes with white patches
- Swollen spleen (splenomegaly) in approximately 50% of cases
- Skin rash especially if incorrectly treated with amoxicillin
- Headache, body aches, and loss of appetite
Most people recover from acute mono within two to four weeks, though fatigue can linger for several months. Getting adequate quality sleep is one of the most important factors in recovery.
Chronic and Reactivation Symptoms
Because EBV never truly leaves the body, it can reactivate. Research has shown that psychological stress is a significant trigger, with a one-point increase in perceived stress correlating with a nearly 2% increase in EBV antibody titers. Other triggers include immunosuppressive medications, hormonal changes, concurrent infections, and physical overtraining.
Reactivation symptoms often include persistent fatigue, low-grade fever, recurring sore throat, brain fog, and muscle or joint pain. In rare cases, chronic active EBV infection (CAEBV) can develop, involving sustained high-level viral replication with potentially life-threatening complications.
The Surprising Link Between EBV, Autoimmune Disease, and Cancer
Perhaps the most alarming aspect of EBV is its connection to serious diseases that can emerge years or decades after the initial infection. The International Agency for Research on Cancer classified EBV as a Group 1 carcinogen in 1997, and subsequent research has strengthened the link between EBV and several autoimmune conditions.
EBV and Multiple Sclerosis
A landmark 2022 study published in Science by Bjornevik and colleagues provided the most compelling evidence yet that EBV is a leading cause of multiple sclerosis. The researchers followed over 10 million U.S. military service members for 20 years and found that EBV infection increased MS risk by an extraordinary 32-fold. No other virus tested, including the closely related cytomegalovirus, showed any association.
Key Finding: Biomarkers of nerve damage (neurofilament light chain) increased only after EBV seroconversion, suggesting the virus triggers the nerve damage that characterizes MS rather than being an innocent bystander.
EBV and Cancer
EBV contributes to an estimated 239,700 to 357,900 new cancer cases worldwide each year, representing approximately 1.5% of all human malignancies.
| Cancer Type | EBV Positivity Rate | Notable Details |
|---|---|---|
| Nasopharyngeal carcinoma | ~100% | Especially prevalent in Southeast Asia |
| Burkitt lymphoma (endemic) | >95% | Most common childhood cancer in equatorial Africa |
| NK/T-cell lymphoma | ~100% | Rare but aggressive |
| Hodgkin lymphoma | 30-50% | Higher rates in developing countries |
| Gastric carcinoma | ~10% | Approximately 75,000 cases annually |
| Post-transplant lymphoproliferative disorder | Variable | Occurs in immunosuppressed patients |
EBV and Lupus
The connection between EBV and systemic lupus erythematosus (SLE) is also significant. Studies have found that EBV infection rates are up to 50-fold higher in children with lupus compared to healthy children. Researchers believe molecular mimicry, where EBV proteins resemble human proteins, may trigger the autoimmune response characteristic of lupus. Chronic stress and hormonal dysregulation can further compound these autoimmune risks.
EBV and Chronic Fatigue Syndrome
Many individuals with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) report their illness began after a bout of infectious mononucleosis. While the relationship is complex and ME/CFS is considered multifactorial, EBV may contribute through chronic immune activation and periodic reactivation.
Decoding Your EBV Test Results
Understanding EBV test results can be confusing because the virus produces multiple antibodies at different stages of infection. The CDC recommends an EBV-specific antibody panel rather than relying solely on the rapid monospot test, which has a 25% false-negative rate during the first week of illness.
The Four Key EBV Antibodies
| Antibody | When It Appears | How Long It Lasts | What It Means |
|---|---|---|---|
| VCA IgM | Early acute infection | 4-6 weeks | Current or very recent infection |
| VCA IgG | Acute phase | Lifetime | Past or current infection |
| EA-D IgG | Acute phase | 3-6 months typically | Active infection or reactivation |
| EBNA IgG | 2-4 months post-onset | Lifetime | Past infection (confirms recovery) |
Reading Your Results
An evidence-based interpretation of your results depends on the combination of positive and negative markers:
- Never infected: All four markers negative. You are susceptible to primary infection.
- Acute infection: VCA IgM positive, VCA IgG positive or rising, EBNA negative. This confirms active mono.
- Recent infection: VCA IgM declining, VCA IgG positive, EA may be positive, EBNA developing.
- Past infection (immune): VCA IgM negative, VCA IgG positive, EBNA positive. This is the normal pattern for most adults.
- Possible reactivation: Elevated VCA IgG, EA-D positive, EBNA positive. May explain recurring symptoms.
Your doctor may also order EBV DNA PCR testing to quantify viral load, particularly if you are immunocompromised, or a complete blood count to check for atypical lymphocytes.
Treatment and Recovery: What Actually Works
There is currently no specific antiviral cure for EBV. Treatment focuses on managing symptoms and supporting your body's natural recovery process. Understanding what works and what does not can save you time, money, and frustration.
Myth vs. Fact: EBV Treatment
| Common Belief | Reality |
|---|---|
| Antibiotics can treat mono | No. Mono is viral; antibiotics are ineffective and amoxicillin can cause rash |
| Antiviral drugs cure EBV | Acyclovir reduces viral shedding but does not improve clinical symptoms in most patients |
| Steroids speed recovery | Only indicated for specific complications like airway obstruction or hemolytic anemia |
| You can exercise through mono | Contact sports and strenuous activity must be avoided for 3-8 weeks due to splenic rupture risk |
| Once you recover, EBV is gone | EBV remains latent in B cells for life and can reactivate |
What Actually Helps
The Cleveland Clinic recommends the following evidence-based approach to EBV recovery:
- Rest: Adequate sleep and reduced activity during the acute phase are essential
- Hydration: Drink plenty of fluids to support immune function and prevent dehydration from fever
- Pain management: Acetaminophen or ibuprofen for fever, sore throat, and body aches (avoid aspirin in children and teens)
- Gradual return to activity: Resume exercise slowly based on symptom resolution, not a fixed timeline
- Throat comfort: Warm saltwater gargles and lozenges can ease sore throat pain
For severe or complicated cases, treatments may include rituximab for EBV-related lymphoproliferative disorders, adoptive T-cell therapy, or in rare cases of chronic active EBV, hematopoietic stem cell transplantation, which is currently the only curative treatment for CAEBV.
Building Your Defense: Natural Support Strategies
While no natural compound has been proven to eradicate EBV from the body, several evidence-based strategies can support immune function and help manage symptoms. Most EBV-specific evidence comes from laboratory studies, so these should complement rather than replace medical care.
Supplements With Research Support
Quercetin: This plant flavonoid found in onions, apples, and berries has shown promising results in laboratory studies. Research published in Molecules demonstrated that quercetin inhibits EBV-induced STAT3 activation and reduces the inflammatory cytokine IL-6, potentially preventing EBV from immortalizing B cells.
Vitamin D: Low vitamin D levels are associated with increased susceptibility to viral infections and higher risk of autoimmune diseases linked to EBV, including MS. Adequate vitamin D supports both innate and adaptive immune function.
Zinc: Essential for immune cell function, zinc works together with quercetin, which acts as a zinc ionophore, helping transport zinc into cells where it can exert antiviral effects.
Curcumin: The active compound in turmeric exhibits anti-inflammatory and immunomodulatory properties that may help modulate the inflammatory response associated with EBV reactivation.
Probiotics: Supporting gut health through probiotic-rich foods may enhance immune response. Growing research interest in the gut-EBV-autoimmunity axis suggests the microbiome plays a role in how the body manages latent EBV infection.
Lifestyle Modifications
Stress management deserves special attention because psychological stress is a documented trigger for EBV reactivation. Practices like meditation, yoga, and maintaining strong social connections are associated with lower EBV antibody titers, indicating better viral control.
Following an anti-inflammatory eating pattern rich in fruits, vegetables, omega-3 fatty acids, and low in processed foods may help reduce the chronic inflammation that allows EBV to reactivate. Regular moderate exercise supports immune surveillance, though overtraining can paradoxically trigger reactivation.
Prevention and the Race for a Vaccine
There is currently no approved vaccine for EBV, but for the first time in decades, multiple candidates are advancing through clinical trials. The National Institutes of Health launched a Phase 1 trial of a gp350-ferritin nanoparticle vaccine, enrolling 40 adults aged 18-29. Additionally, ModeX Therapeutics (partnering with Merck) dosed its first participant in a Phase 1 trial of MDX2201 in January 2025, and Moderna has an mRNA-based EBV vaccine in development.
Until a vaccine becomes available, prevention relies on practical measures: avoiding sharing drinks and utensils, practicing good hand hygiene, and being aware that EBV can be shed in saliva intermittently for life even without symptoms.
Frequently Asked Questions
Can Epstein-Barr virus be completely cured?
No. Once infected, EBV establishes lifelong latency in memory B cells. There is no treatment that eliminates the virus entirely. However, a healthy immune system typically keeps the virus dormant, and most people with past EBV infection never experience problems from it. Treatment focuses on managing symptoms during active infection and supporting immune function to prevent reactivation.
How long does it take to recover from mononucleosis?
Most people feel significantly better within two to four weeks, though fatigue can persist for several months. You should avoid contact sports and strenuous physical activity for at least three to eight weeks due to the risk of splenic rupture. Full energy levels typically return within one to three months, but some individuals report lingering fatigue for up to six months.
Should I get tested for EBV if I have chronic fatigue?
It may be worthwhile, especially if your fatigue began after a viral illness. An EBV-specific antibody panel (VCA IgM, VCA IgG, EA-D, and EBNA) can reveal whether you have evidence of recent or reactivated infection. However, since over 90% of adults test positive for past EBV infection, a positive VCA IgG alone is not meaningful. The pattern of all four markers together tells the story.
Is Epstein-Barr virus contagious for life?
Technically, yes. EBV can be shed intermittently in saliva throughout life, even without symptoms. However, most adults already carry the virus, so the practical risk of transmission is most relevant for the small percentage of adults and adolescents who have not yet been infected. You are most contagious during the acute phase of illness and for several weeks afterward.
Can EBV reactivation be prevented?
While you cannot guarantee prevention of reactivation, you can reduce the risk. Key strategies include managing stress, getting adequate sleep, maintaining a nutrient-rich diet, exercising moderately, and avoiding immune-suppressing behaviors like excessive alcohol consumption. If you are on immunosuppressive medications, work with your doctor to monitor EBV status.
Related Articles
- Immune-Boosting Probiotic Foods — Discover how probiotic-rich foods can strengthen your immune defenses against viral infections.
- Nutrition for a Better, Stronger Immune System — A comprehensive guide to the vitamins, minerals, and dietary patterns that support immune health.
- Anti-Inflammatory Eating Patterns — Compare the Mediterranean, DASH, and plant-based approaches to reducing chronic inflammation.
- Chronic Stress, Hormones, and HPA Axis Recovery — Understand how chronic stress impacts your immune system and what you can do about it.
- 10 Simple Tips to Improve Your Sleep — Better sleep is essential for immune function and recovery from viral infections.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.