Bottom line: No single food or supplement can "boost" your immune system overnight. But eating enough of the right vitamins, minerals, and fiber-rich whole foods keeps the complex network of cells and signals running the way it should. The evidence points to dietary patterns, not magic ingredients, as the real foundation.
How Your Immune System Actually Works
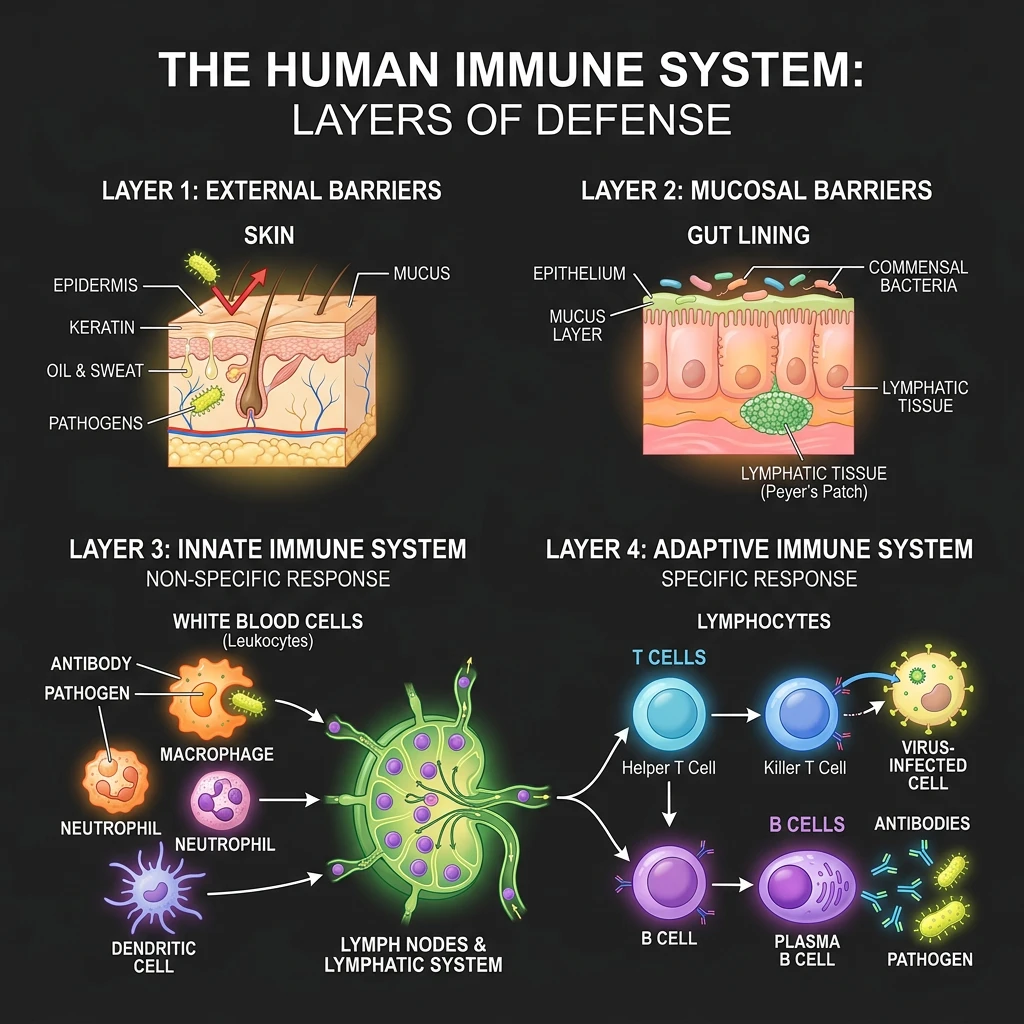
Your immune system is not a single organ you can tune up like an engine. It is a network of cells, tissues, and chemical signals spread across your whole body, from your skin and mucous membranes to your bone marrow, thymus, spleen, and lymph nodes. Every one of these components depends on a steady supply of specific nutrients to do its job, which is why what you eat matters more than most people realize.
The system works in two coordinated layers. Your innate immune system provides the immediate, non-specific first response: physical barriers like skin and gut lining, plus white blood cells such as neutrophils, macrophages, and natural killer cells that attack anything foreign. Your adaptive immune system learns from each encounter. B cells produce targeted antibodies, while T cells destroy infected cells and coordinate the broader response. The NIH Office of Dietary Supplements states that adequate intake of several vitamins and minerals is important for proper immune function, and clinical deficiencies weaken both of these layers.
When pathogens breach the barriers, the immune response generates inflammation (redness, swelling, heat) to contain and eliminate the threat. That process is normal. Problems start when inflammation becomes chronic or excessive, something that happens more often when the body lacks the nutrients to regulate the response. A 2021 review in Nutrients found that oxidative stress and poor nutrient status are closely linked to inflammatory responses that damage the body's own tissues.
Vitamins That Directly Support Immune Cells
Several vitamins are required for immune cell production, function, and regulation. If you are low on any of them, your ability to fight infection takes a measurable hit.
Vitamin C
Vitamin C supports both innate and adaptive immunity through its antioxidant effects, antimicrobial actions, and influence on immune modulators. It helps maintain the integrity of epithelial barriers, promotes phagocytosis (the process by which immune cells engulf pathogens), and normalizes cytokine production. According to the NIH, vitamin C deficiency, while uncommon in developed countries, significantly increases susceptibility to respiratory infections.
Your body can't produce or store vitamin C, so daily intake is a must. Bell peppers, citrus fruits, kiwifruit, broccoli, strawberries, and brussels sprouts are the richest food sources. For most people, food provides more than enough. The Cleveland Clinic notes that supplementation is rarely needed unless a physician specifically advises it.
Vitamin D
Vitamin D has become one of the most studied nutrients in immune research over the past decade. It supports multiple immune cell types, and some immune cells, including dendritic cells and macrophages, can produce the active form of vitamin D on their own. That detail alone tells you how tightly linked this vitamin is to immune function. Vitamin D also promotes the production of antimicrobial proteins like cathelicidin that fight pathogens directly.
A review by Calder (2021) in Nature Nutrition & Diabetes reported that meta-analyses of randomized controlled trials show vitamin D supplementation reduces the incidence of respiratory tract infections. A large Israeli study found that low vitamin D status increased both infection risk and hospitalization risk. Fatty fish (trout, salmon), egg yolks, mushrooms, and fortified foods are dietary sources, though direct sunlight remains the most efficient way to get enough.
Vitamin A
Vitamin A maintains the health of epithelial tissues, the protective linings of your lungs, gut, and urinary tract that serve as the body's first physical barriers against pathogens. It also supports macrophage function and T-cell maturation. The NIH documents that vitamin A deficiency is associated with increased susceptibility to infections and impaired barrier function, though deficiency is rare in developed countries.
Preformed vitamin A comes from animal sources: eggs, dairy, organ meats. Provitamin A carotenoids (beta-carotene) come from orange and yellow vegetables, leafy greens, and tomatoes. Spinach, sweet potatoes, and carrots are among the best plant sources.
Vitamin E
Vitamin E is a potent antioxidant that protects cell membranes, including those of immune cells, from oxidative damage. Deficiency impairs both humoral and cell-mediated immunity and reduces natural killer cell activity. The best food sources are sunflower seeds, almonds, avocado, and broccoli. The Cleveland Clinic specifically cautions against vitamin E supplements, noting that clinical research supporting supplementation is limited and that high-dose supplements may be harmful.
| Vitamin | Primary Immune Role | Top Food Sources | Deficiency Risk |
|---|---|---|---|
| Vitamin C | Antioxidant protection, T-cell and B-cell support | Bell peppers, citrus, kiwi, broccoli | Increased infection susceptibility |
| Vitamin D | Antimicrobial protein production, T-cell regulation | Fatty fish, egg yolks, sunlight | Higher respiratory infection rates |
| Vitamin A | Epithelial barrier maintenance, macrophage function | Sweet potatoes, carrots, spinach, eggs | Impaired barrier function |
| Vitamin E | Cell membrane antioxidant, NK cell activity | Sunflower seeds, almonds, avocado | Weakened humoral and cellular immunity |
| B6 | White blood cell and T-cell production | Chickpeas, salmon, tuna, tofu | Reduced lymphocyte count |
| B12 | Neutrophil phagocytic capacity | Meat, fish, dairy, fortified cereals | Impaired phagocytosis |
| Folate (B9) | Thymus and spleen function, T-cell levels | Leafy greens, legumes, fortified grains | Decreased T-lymphocytes |
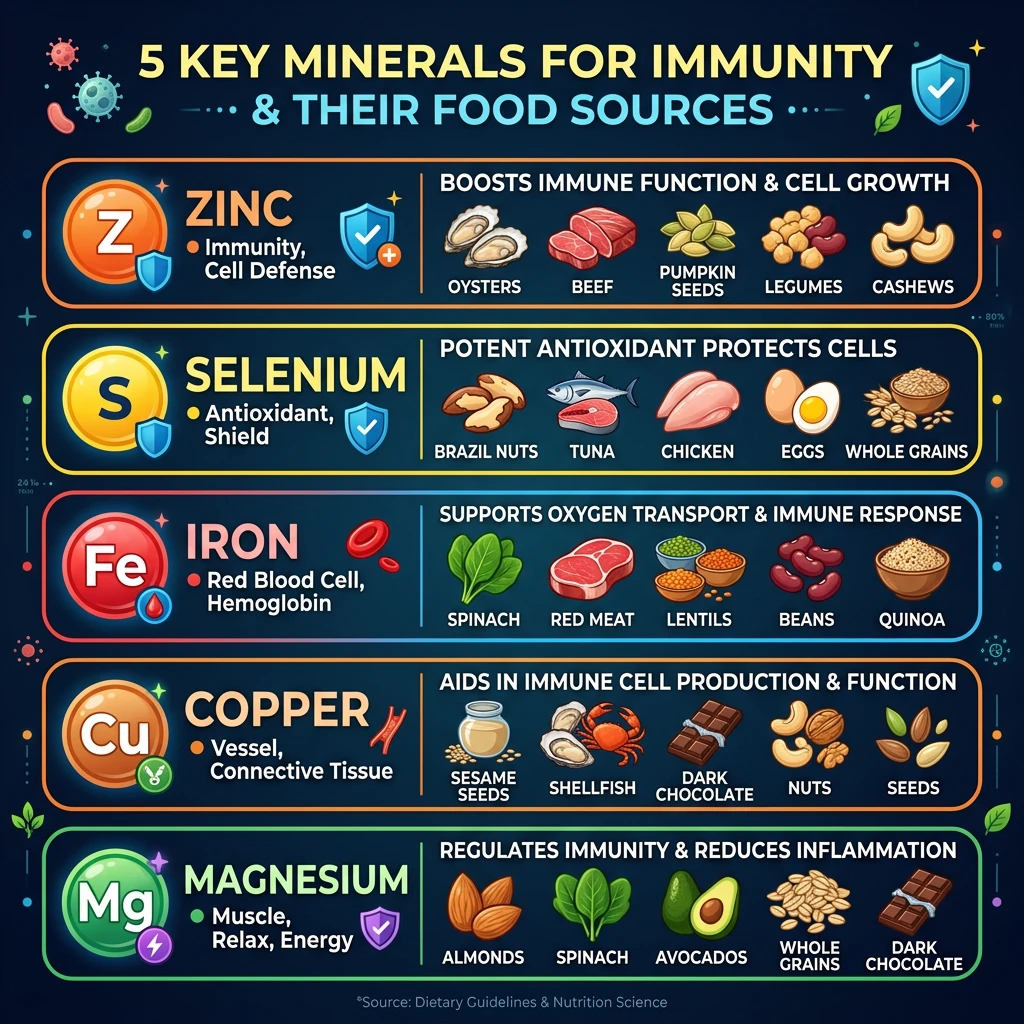
Minerals Your Immune System Cannot Function Without
Vitamins get most of the attention, but several minerals are just as important for immune defense. In some cases, even marginal deficiencies (not full-blown deficiency) measurably impair immune cell activity.
Zinc
Researchers call zinc the "gatekeeper" of the immune system because it is required for the proper function of virtually every type of immune cell. Zinc supports T-cell function, helps control oxidative stress and inflammation, and has direct anti-viral properties, including the ability to inhibit coronavirus replication, as noted in the Nature review by Calder. Meta-analyses of randomized controlled trials show zinc supplementation reduces the incidence of both diarrheal and respiratory infections.
But there is a catch: excess zinc can actually suppress immune function by inhibiting phagocytic cells. Getting zinc from food (oysters, lean beef, pumpkin seeds, turkey) is generally preferable to high-dose supplements. A balanced intake supports immunity. Too much disrupts it.
Selenium
Selenium has a unique dual role. It activates the immune system when threats arise, but also signals it to stand down when the threat passes, protecting against the chronic inflammation that drives autoimmune conditions. Selenium also prevents viral mutation. Extensive mouse research has shown that selenium deficiency allows normally weak viruses to mutate into more dangerous strains. A supplementation study in UK adults with marginal selenium status found that selenium improved anti-viral immune responses, promoted viral clearance, and decreased viral mutation rates.
Brazil nuts are the most concentrated food source. A single nut can provide more than a day's requirement. Tuna, halibut, and cottage cheese are other good options.
Other minerals worth watching
Several additional minerals support immune function in ways that often get overlooked:
- Iron is required for immune cell proliferation and maturation. Iron-deficient individuals show impaired antimicrobial responses.
- Copper deficiency is associated with altered immune responses and increased infection risk, particularly in infants and older adults.
- Magnesium at low levels is associated with decreased immune cell activity, increased oxidative stress, and elevated inflammatory cytokines including interleukin-6, according to the NIH.
| Mineral | Immune Function | Top Food Sources | Daily Need (Adults) |
|---|---|---|---|
| Zinc | T-cell function, anti-viral activity | Oysters, beef, pumpkin seeds | 8-11 mg |
| Selenium | Immune activation/regulation, viral mutation prevention | Brazil nuts, tuna, halibut | 55 mcg |
| Iron | Immune cell proliferation | Red meat, spinach, lentils | 8-18 mg |
| Copper | Immune response regulation | Shellfish, nuts, seeds, organ meats | 900 mcg |
| Magnesium | Reduces oxidative stress and inflammation | Dark chocolate, avocados, almonds | 310-420 mg |
Your Gut Runs Most of Your Immune Defense
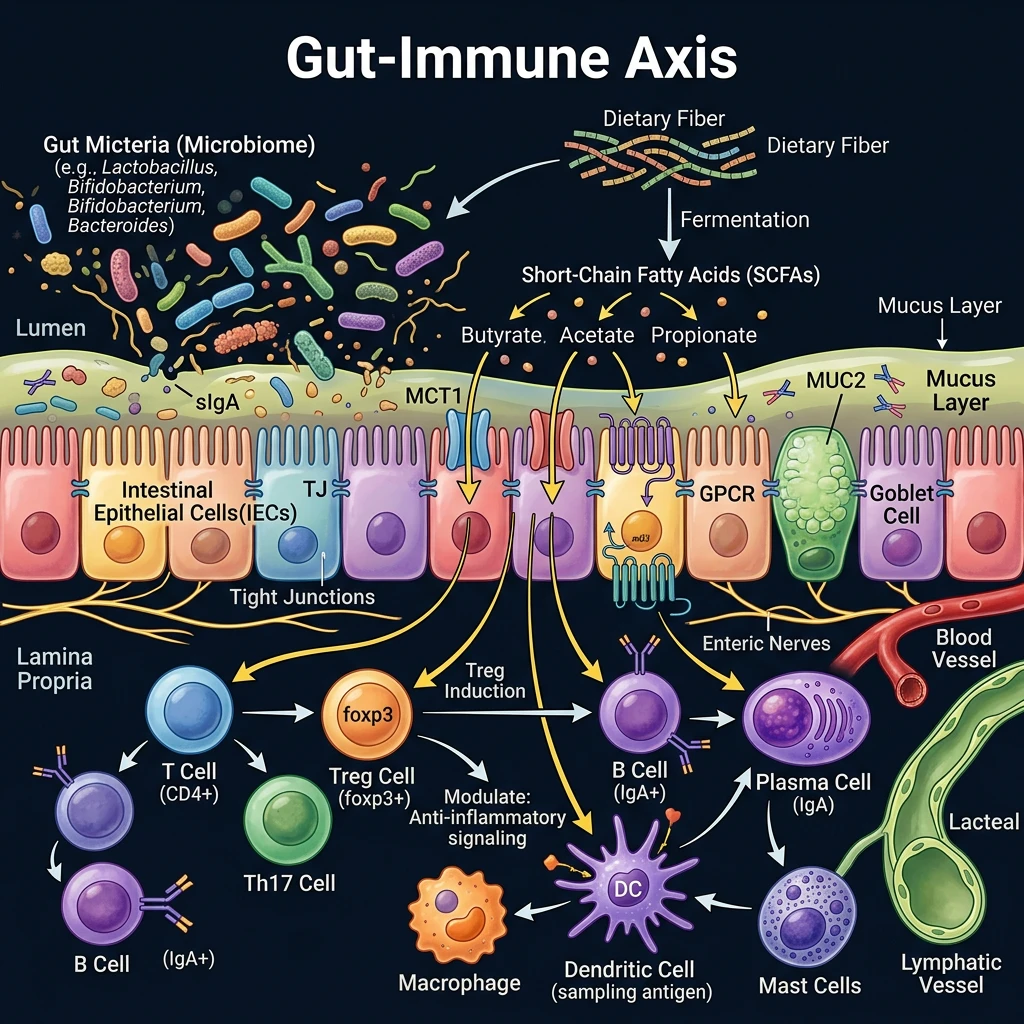
Somewhere between 70 and 80 percent of your immune cells reside in your gut. That number changes the conversation about immune nutrition entirely. A 2021 review in Nutrients documents how the intestinal microbiota, the gut epithelial layer, and the local mucosal immune system work together and influence systemic immunity throughout the body.
Your intestinal microbiota, trillions of bacteria, fungi, and viruses, isn't just passively living in your gut. These organisms actively compete with pathogens for resources (a process called colonization resistance), produce antimicrobial proteins, and generate metabolites that regulate immune cell behavior. The most important of these metabolites are short-chain fatty acids (SCFAs), produced when gut bacteria ferment dietary fiber. SCFAs stimulate antimicrobial peptide production, improve mucus output, promote regulatory T-cell maturation, and support intestinal barrier repair.
What you eat directly determines which microbial communities thrive. According to the Harvard T.H. Chan School of Public Health, a high-fiber, plant-rich diet with plenty of fruits, vegetables, whole grains, and legumes supports beneficial bacteria. Diets high in refined sugar, red meat, and ultra-processed foods do the opposite: they disrupt the gut microbiome, drive chronic intestinal inflammation, and suppress immunity.
Feeding your gut properly
Two categories of foods specifically support the gut-immune connection:
Prebiotic foods contain fiber and oligosaccharides that feed beneficial gut bacteria. Garlic, onions, leeks, asparagus, bananas, and Jerusalem artichokes all qualify. More broadly, any diverse intake of fruits, vegetables, beans, and whole grains provides prebiotic fuel.
Probiotic foods contain live beneficial bacteria. Kefir, yogurt with live active cultures, sauerkraut, kimchi, tempeh, kombucha, and miso all contribute to microbial diversity. The fiber these bacteria ferment into SCFAs completes the cycle: prebiotics feed the probiotics, and the probiotics produce the compounds that regulate immune cells.
Dietary Patterns That Strengthen or Weaken Immunity
Individual nutrients matter, but your overall dietary pattern matters more. Immune function tracks with the quality of your whole diet, not with any single supplement dose.
Patterns that support immunity
The Mediterranean diet, which emphasizes vegetables, fruits, whole grains, legumes, nuts, olive oil, and fish, repeatedly shows up in research as protective. That makes sense when you look at the nutrient profile: it delivers high amounts of vitamin C, vitamin E, zinc, selenium, and polyphenols while feeding gut bacteria with diverse plant fibers. Omega-3 fatty acids from fish also regulate inflammatory and immune processes by interacting with transcription factors related to anti-inflammatory signaling, according to the PMC review.
Plant polyphenols deserve a mention here too. Found in berries, tea, dark chocolate, and colorful vegetables, these compounds have both antioxidant and prebiotic properties. They shift gut microbiota composition toward beneficial Bifidobacterium species and away from potential pathogens. Quercetin, found in onions, apples, and berries, is one of the most studied polyphenols for immune modulation.
Patterns that undermine immunity
The Western diet, characterized by high intakes of refined sugar, processed foods, and saturated fat with low intakes of fruits, vegetables, and fiber, damages immune function through several mechanisms at once. It starves beneficial gut bacteria of the fiber they need, promotes inflammatory gut bacteria, drives chronic low-grade inflammation, and contributes to obesity, which itself is a significant immune impairment.
The Nature review documents that obesity is associated with impaired activity of helper T cells, cytotoxic T cells, B cells, and natural killer cells. During the 2009 H1N1 influenza pandemic, people with obesity showed delayed and weakened anti-viral responses compared with healthy-weight individuals. Vaccinated individuals with obesity had twice the risk of influenza compared with vaccinated healthy-weight individuals, meaning even vaccine effectiveness suffers.
| Factor | Immune-Supporting Pattern | Immune-Damaging Pattern |
|---|---|---|
| Fruits and vegetables | 5+ servings daily, diverse colors | Minimal intake, mostly potatoes |
| Protein sources | Fish, legumes, poultry, nuts | Predominantly processed meat |
| Fats | Olive oil, nuts, fatty fish (omega-3) | Fried foods, excess omega-6 |
| Fiber | 25-35g daily from whole foods | Under 15g from refined grains |
| Sugar | Minimal added sugars | High intake of sugary drinks and sweets |
| Fermented foods | Regular intake (yogurt, kimchi, kefir) | None or rarely consumed |
| Gut microbiome effect | Diverse, SCFA-producing communities | Reduced diversity, pro-inflammatory |
Immune Nutrition Myths Versus What Research Shows
The immune supplement industry thrives on oversimplification. Here is what the research actually supports.
| Myth | What Research Shows |
|---|---|
| Megadose vitamin C prevents colds | Regular vitamin C intake may slightly reduce cold duration (about 8% in adults), but megadoses taken after symptoms start show no benefit. Prevention requires consistent daily intake, not emergency loading. |
| Supplements are as good as food | Harvard and the Cleveland Clinic both stress that your body absorbs vitamins and minerals more effectively from food. Supplements should fill gaps, not replace diet. |
| Echinacea cures colds | Taking echinacea after catching a cold has not been shown to shorten duration. Taking it while healthy may offer marginal protection, but evidence remains inconclusive. |
| More zinc is better | Zinc deficiency impairs immunity, but excess zinc suppresses phagocytic cells. The therapeutic window is narrow. |
| You can "boost" immunity quickly | The immune system requires sustained nutritional support over weeks and months. No fast-track supplement protocol meaningfully changes immune function overnight. |
| Elderberry is proven to prevent flu | Some lab studies show elderberry can inhibit viral replication, but clinical evidence in humans is limited and mixed. It should not replace vaccination or standard medical care. |
The European Society for Clinical Nutrition and Metabolism puts it bluntly: in the absence of deficiency, routine micronutrient supplementation "probably does little to prevent or treat specific infections." The research supports correcting deficiencies and maintaining adequate intake, not stacking supplements hoping something sticks.
Building Your Immune-Supporting Plate
You don't need to overhaul your diet to eat for immune health. The goal is steady intake of the nutrients covered above, spread across your meals.
A practical daily framework
In the morning, go for foods that deliver vitamin C and fiber: berries, kiwi, or citrus alongside oats or whole-grain toast. A handful of almonds or sunflower seeds adds vitamin E.
At lunch, build around protein and zinc. Chickpeas, lentils, or lean meat with colorful vegetables works well. The more colors on the plate, the wider the range of polyphenols and carotenoids you're getting. Leafy greens like spinach bring folate, vitamin A, and iron.
For dinner, aim for fatty fish (salmon, trout, sardines) twice a week to cover vitamin D and omega-3 needs. Sweet potatoes or carrots for vitamin A. Garlic and onions in the cooking provide prebiotic fiber and antimicrobial compounds.
Daily, add one or two servings of fermented foods (yogurt, kefir, sauerkraut, kimchi) for probiotic support. A single Brazil nut handles selenium. And drink enough water.
Beyond the plate
Nutrition doesn't work in isolation. The Harvard Nutrition Source identifies several non-dietary factors that significantly affect immune function:
- Sleep: During sleep, the body releases cytokines that fight infection. Chronic sleep deprivation reduces these and other immune cells. Aim for 7-9 hours nightly.
- Physical activity: Moderate, regular exercise supports immune circulation and reduces chronic inflammation. Extreme endurance exercise can temporarily suppress immunity.
- Stress management: Chronic stress releases cortisol, which suppresses both inflammation and white blood cell activity. Meditation, breathing exercises, and physical activity all help regulate cortisol.
- Maintaining healthy weight: As the Nature review documents, obesity impairs multiple aspects of immune function and increases susceptibility to severe infection outcomes.
Frequently Asked Questions
Can you actually boost your immune system with food?
You can't supercharge your immune system beyond its normal capacity through food. What you can do, and what research supports, is provide the nutrients it needs to function at full capacity. Deficiencies in vitamins C, D, A, zinc, and selenium measurably impair immune responses, so correcting or preventing those deficiencies through diet keeps your defenses where they should be.
Should I take a multivitamin for immune support?
For most people eating a varied diet, a multivitamin isn't necessary. That said, older adults, pregnant women, people with restricted diets, and those with chronic diseases may benefit from a general multivitamin providing recommended daily allowances. Harvard and the Cleveland Clinic both recommend a food-first approach, with supplements used only to fill gaps identified by a healthcare provider.
How long does it take for dietary changes to improve immune function?
The immune system responds to sustained nutritional changes over weeks to months, not days. Correcting a specific deficiency like low vitamin D may take 8-12 weeks to fully normalize immune markers. Shifting to a more diverse, plant-rich diet begins improving gut microbiome composition within days, but the downstream immune benefits build gradually.
Does sugar really weaken your immune system?
Diets high in refined sugar promote disturbances in gut microbiome composition, drive chronic low-grade inflammation, and contribute to obesity, all of which impair immune function. The mechanism is indirect but well-documented: excess sugar feeds inflammatory gut bacteria, reduces microbial diversity, and triggers metabolic changes that suppress immune cell activity over time.
Is vitamin D the most important nutrient for immunity?
Vitamin D is one of the most studied nutrients for immune function, and deficiency clearly increases infection risk. But the immune system depends on multiple nutrients working together: zinc, selenium, vitamins C and A, iron, and others all have essential roles. No single nutrient is "most important" because the system fails when any critical piece is missing.
Related Articles
- Quercetin for Allergies, Immunity, and Inflammation — How this plant polyphenol modulates immune responses and reduces inflammation.
- Elderberry for Immune Support: Evidence, Dosage, and Safety — What the research says about elderberry's anti-viral properties and proper use.
- Omega-3 Benefits, Sources, and Supplements — The anti-inflammatory fatty acids that support immune regulation and gut health.
- Magnesium Types: Glycinate, Citrate, Threonate — Understanding the different forms of this immune-supporting mineral.
- Spinach Health Benefits and Nutritional Facts — A nutrient-dense source of folate, vitamin A, iron, and vitamin C for immune support.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.












