Quick takeaway: Hashimoto's thyroiditis is the number one cause of hypothyroidism, and women are 4 to 10 times more likely to develop it than men. Levothyroxine is the standard treatment, but research on selenium, vitamin D, gut health, and dietary changes suggests there are more levers to pull than medication alone.
A Tiny Gland Running Your Entire Metabolism
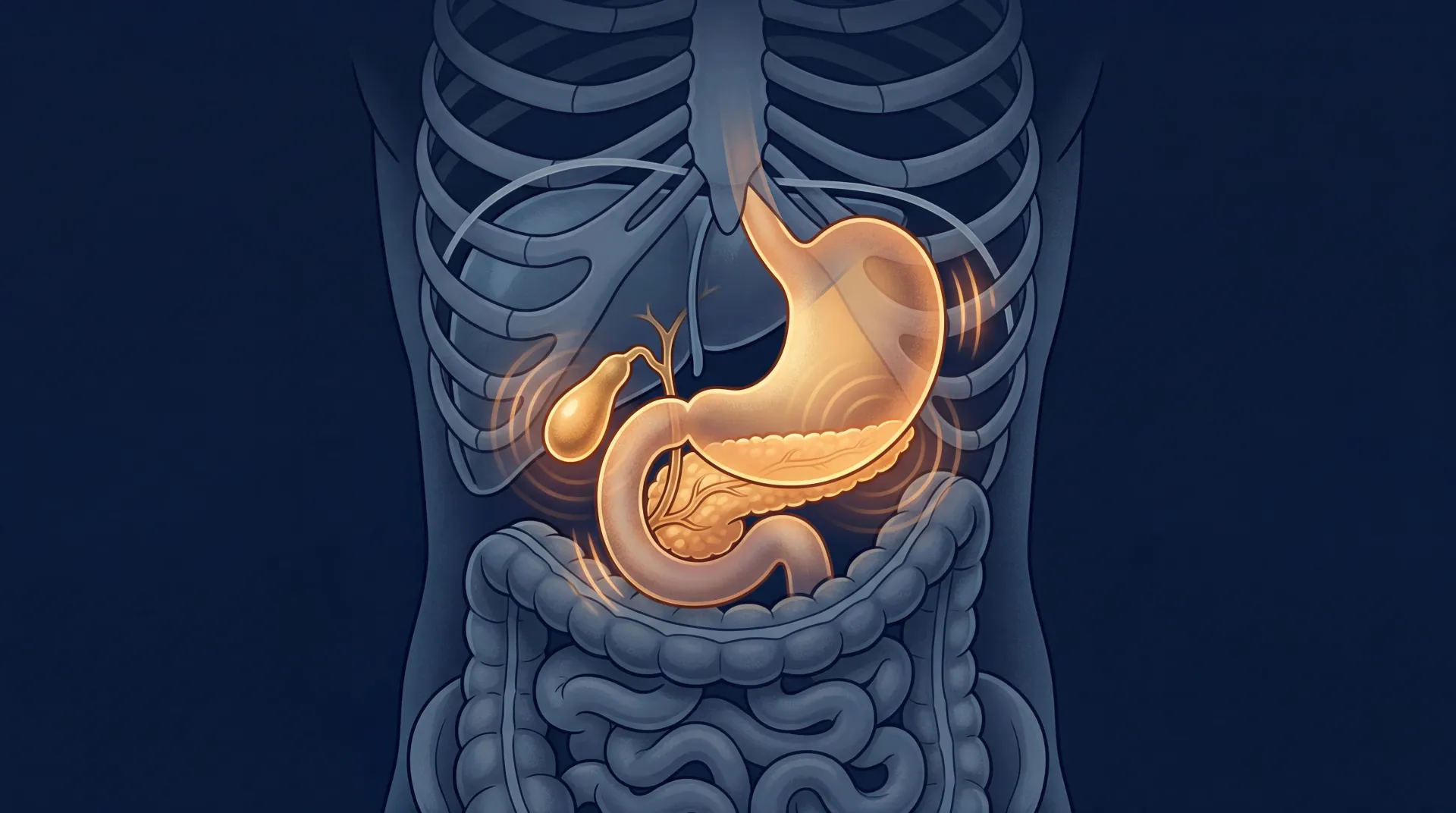
Your thyroid sits at the base of your neck and weighs about 20 grams, roughly the same as four nickels. Small gland. Massive job. It produces hormones that regulate heart rate, body temperature, energy production, weight, and even how quickly you replace dying cells.
The thyroid makes two hormones: thyroxine (T4) and triiodothyronine (T3). T4 is the storage form. It circulates in your blood until enzymes called deiodinases convert it into T3, which is what your cells actually use. That conversion requires specific micronutrients, particularly selenium, and happens mainly in the liver and kidneys.
The whole system runs on a feedback loop. Your pituitary gland monitors circulating thyroid hormones and releases thyroid-stimulating hormone (TSH) accordingly. When T3 and T4 drop, TSH rises to push the thyroid harder. When levels are adequate, TSH backs off. TSH testing is the first diagnostic step for thyroid disorders because it tells you whether this thermostat is functioning.
Iodine is a direct structural component of both T3 and T4. Without it, the thyroid literally cannot build its hormones. According to a review published in Endocrine, Metabolic and Immune Disorders — Drug Targets, approximately 800 million people worldwide are affected by iodine deficiency disorders, making it the most common cause of preventable brain damage globally.
Hashimoto's: When Your Immune System Targets the Thyroid
Hashimoto's thyroiditis is an immune system problem that happens to destroy the thyroid. White blood cells infiltrate the gland and produce antibodies, mainly thyroid peroxidase antibodies (TPOAb) and thyroglobulin antibodies (TgAb), that progressively damage the tissue responsible for making hormones.
The destruction unfolds gradually. According to the Endocrine Society, the hypothyroidism caused by Hashimoto's progresses slowly over months to years, which partly explains why so many cases go undetected for a long time. As the thyroid sustains cumulative damage, its ability to produce T4 and T3 diminishes, and TSH climbs higher in a failing attempt to compensate.
One counterintuitive wrinkle: early in the disease, the immune attack can actually cause a temporary surge of thyroid hormone. As thyroid cells are destroyed, they dump their stored hormones into the bloodstream, producing a phase called hashitoxicosis — a period of hyperthyroid-like symptoms including anxiety, rapid heartbeat, and sweating. The University of Michigan Health notes that this phase is almost always followed by the development of hypothyroidism.
The numbers are lopsided. The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) reports Hashimoto's is 4 to 10 times more common in women than men, with peak onset between ages 30 and 50. Family history raises the risk. And Hashimoto's tends to cluster with other autoimmune conditions: celiac disease, type 1 diabetes, rheumatoid arthritis, Sjögren's syndrome.
| Risk Factor | Details |
|---|---|
| Sex | 4-10x more common in women |
| Age | Peak onset ages 30-50 |
| Family history | Strong genetic component; runs in families |
| Existing autoimmune disease | Celiac, type 1 diabetes, RA, lupus, Sjögren's |
| Other associations | Addison's disease, pernicious anemia, premature menopause |
Symptoms That Often Fly Under the Radar
A lot of people carry Hashimoto's for years without knowing it. The symptoms overlap with dozens of other conditions, and they develop so gradually that you keep adjusting your baseline for what "normal" feels like. By the time you notice something is wrong, you may have been hypothyroid for a while.
The classic hypothyroid symptoms are well-documented: fatigue that sleep does not fix, unexplained weight gain, heightened sensitivity to cold, constipation, dry skin, and thinning hair. But several symptoms tend to get overlooked or attributed to other causes.
Depression and cognitive fog deserve particular attention. Johns Hopkins Medicine explicitly lists depression among Hashimoto's symptoms, and many patients report difficulty concentrating or a persistent mental sluggishness that gets dismissed as stress or poor sleep. If you have been managing depression or anxiety that does not fully respond to standard treatments, thyroid function is worth investigating. Your gut-brain axis also plays into this — the connection between digestive health, mood, and cognition is increasingly recognized in thyroid conditions.
Joint and muscle pain is another symptom that often gets sent down the wrong diagnostic path. The aches can mimic fibromyalgia or early arthritis, leading to years of treatment targeting the wrong condition.
| Common Symptoms | Less Recognized Symptoms |
|---|---|
| Fatigue and exhaustion | Depression and mood changes |
| Weight gain | Brain fog and poor concentration |
| Cold intolerance | Joint and muscle pain |
| Constipation | Brittle nails |
| Dry skin and thinning hair | Heavy or irregular periods |
| Slowed heart rate | Fertility difficulties |
| Goiter (neck swelling) | Puffy face, especially around eyes |
Menstrual irregularities and fertility problems deserve their own mention. Heavy periods, irregular cycles, and difficulty conceiving are all documented consequences of insufficient thyroid hormone. For women in their reproductive years — precisely the demographic most affected by Hashimoto's — these symptoms may be the first tangible sign that something is off.
Beyond TSH: Getting the Right Tests
A single TSH test can confirm hypothyroidism, but it cannot tell you why. For Hashimoto's, you need more information.
The NIDDK outlines the standard diagnostic approach: a medical history and physical exam (checking for a goiter), followed by blood tests for TSH, free T4, free T3, and critically, thyroid peroxidase antibodies (TPOAb). TPOAb are present in most people with Hashimoto's and serve as the key differentiator from other causes of hypothyroidism.

| Test | What It Measures | Why It Matters |
|---|---|---|
| TSH | Pituitary signal to thyroid | First-line screening; high TSH = underactive thyroid |
| Free T4 | Unbound thyroxine (storage hormone) | Shows actual thyroid output, not just pituitary response |
| Free T3 | Active thyroid hormone | Reveals conversion efficiency (T4→T3) |
| TPOAb | Thyroid peroxidase antibodies | Confirms autoimmune cause; present in most Hashimoto's cases |
| TgAb | Thyroglobulin antibodies | Additional autoimmune marker; can be elevated even with normal TPOAb |
| Thyroid ultrasound | Gland size and texture | Rules out nodules; confirms Hashimoto's if antibodies are absent |
This is the tricky part: you can have Hashimoto's with a normal TSH. In the early stages, the thyroid may still produce enough hormone to keep TSH within range, even while antibodies are actively attacking the gland. Testing only TSH in this scenario misses the autoimmune process entirely. This is why many endocrinologists recommend checking TPOAb in patients with thyroid symptoms, a family history of autoimmune disease, or other autoimmune conditions — regardless of TSH results.
If your doctor suspects Hashimoto's but your blood tests come back without detectable antibodies (which happens in a minority of cases), an ultrasound can show characteristic patterns of inflammation and texture changes in the thyroid tissue.
How Food Choices Shape Thyroid Function
Diet does not cause Hashimoto's, and no diet cures it. But what you eat can influence how the disease progresses and how well your thyroid functions. Some dietary factors have solid evidence behind them. Others are more speculative than the wellness internet would suggest.
Start with iodine. Your thyroid needs it to build hormones, but with Hashimoto's, more is not better. The NIDDK warns that people with autoimmune thyroid disorders may be sensitive to iodine, and consuming large amounts through kelp, seaweed, or iodine supplements can worsen hypothyroidism or trigger flares. You still need iodine (your body cannot make thyroid hormones without it), but concentrated sources and supplements deserve caution.
Then there is gluten, which gets a lot of attention in Hashimoto's circles. A 2023 meta-analysis published in Frontiers in Endocrinology found that a gluten-free diet improved TSH levels and free T4 in Hashimoto's patients, but the biggest benefits appeared in patients who also had gluten-related conditions. A more recent 2025 meta-analysis in Nutrients found something odd: gluten-free diets reduced thyroglobulin antibodies but actually increased TPO antibodies in non-celiac Hashimoto's patients. The researchers themselves rated the evidence quality as having serious concerns.
So if you have Hashimoto's and also get bloating, diarrhea, or abdominal pain after eating wheat, a trial gluten-free period is worth discussing with your doctor. But going gluten-free as a blanket strategy for all Hashimoto's patients? The data does not support that yet.
The gut connection is worth paying attention to. Research published in Frontiers in Immunology found that Hashimoto's patients had measurably different gut bacteria compared to healthy controls, with increased Bacteroides and decreased Bifidobacterium. The same study detected elevated zonulin levels, a marker of increased intestinal permeability (sometimes called leaky gut). The idea is that intestinal dysbiosis may contribute to autoimmune activation by letting antigens cross the gut barrier and trigger immune responses.
One concern you can probably stop worrying about: goitrogens. Cruciferous vegetables like broccoli, cauliflower, and kale contain thiocyanates that can theoretically interfere with thyroid iodine uptake. In practice, you would need to eat enormous raw quantities to see any real effect. Cooking deactivates most of these compounds. Skipping cruciferous vegetables deprives you of anti-inflammatory nutrients that actually help autoimmune conditions, which is a bad trade.
Key Nutrients Your Thyroid Depends On
Your thyroid's performance depends on a few specific micronutrients. Some of these relationships are well-established. Others are still being worked out.
Selenium has the strongest research backing of any nutrient for Hashimoto's. The thyroid contains more selenium per gram than any other organ in your body. It is required for the deiodinase enzymes that convert T4 into active T3 and is a core part of glutathione peroxidase, a family of enzymes that protect the thyroid from oxidative damage during hormone production.
A 2024 systematic review and meta-analysis of 35 randomized controlled trials involving over 2,300 participants found that selenium supplementation significantly reduced both TSH and TPO antibody levels in Hashimoto's patients who were not on thyroid hormone replacement. The effect on antibodies was large (standardized mean difference of -0.96), and adverse effects were comparable to placebo. A separate 2024 network meta-analysis in Frontiers in Endocrinology compared selenium against vitamin D and myo-inositol and concluded that selenium was the only supplement with significant evidence for reducing thyroid antibodies.

Most studies used selenomethionine at 200 micrograms per day for 3-6 months. Brazil nuts are the most concentrated food source — just 2-3 nuts daily can provide roughly this amount, though selenium content varies by soil conditions where the nuts were grown.
Vitamin D is a different story. The relationship with Hashimoto's is real but messier than selenium. A 2025 review in Frontiers in Endocrinology found that vitamin D deficiency (below 20 ng/mL) can increase TPO antibody levels by 40-60% and speed up the slide toward overt hypothyroidism. Supplementation at 2,000-4,000 IU daily reduced antibodies by 15-30%, but only in patients who were actually deficient. If your vitamin D levels are already fine, adding more does nothing.
How common is deficiency? A study of 461 Hashimoto's patients from the Croatian Biobank found that roughly 65% were vitamin D deficient during winter and spring. Get tested. If you are low, correcting it likely helps. If you are not, save your money.
Iron deserves attention too, especially for women. Hypothyroidism can impair iron absorption, and iron deficiency in turn hampers thyroid peroxidase activity, the enzyme responsible for hormone synthesis. Heavy menstrual periods, a common Hashimoto's symptom, further deplete iron stores. If your fatigue seems out of proportion to your thyroid hormone levels, an iron panel including ferritin is worth requesting.
Zinc contributes to thyroid hormone synthesis and immune regulation. The evidence for zinc supplementation specifically in Hashimoto's is thinner than for selenium, but maintaining adequate zinc status supports the system. Oysters, red meat, pumpkin seeds, and lentils are reliable food sources.
Evidence-Based Natural Support Strategies
Beyond specific nutrients, several lifestyle factors influence how Hashimoto's behaves. None of these replace levothyroxine (which remains the standard of care for hypothyroidism), but they can make a real difference alongside it.
Gut health is the one that makes the most biological sense given recent research. The altered microbiota and increased intestinal permeability found in Hashimoto's patients point toward practical interventions: fermented foods like yogurt, kefir, and sauerkraut to support Bifidobacterium populations; prebiotic-rich foods like garlic, onions, and asparagus to feed beneficial bacteria. Bone broth provides amino acids like glutamine and glycine that support gut lining repair. Probiotic supplementation is also worth considering.
Stress management matters more than most people realize with Hashimoto's. Chronic stress elevates cortisol, which suppresses TSH production and impairs T4-to-T3 conversion. The autoimmune process is already reducing hormone output. Stress makes what remains less effective. Meditation, walking, adequate sleep, setting boundaries: these are not optional feel-good extras for Hashimoto's patients. They protect a metabolic pathway that is already under pressure.
Exercise helps, but intensity matters. Walking, swimming, yoga, cycling: these generally improve energy and mood without overtaxing the system. High-intensity or prolonged endurance training, though, can temporarily suppress thyroid function and spike cortisol. If intense workouts leave you wrecked for days, that is your body telling you to pull back, not push through. Hormonal balance responds better to consistency than intensity.
If you take levothyroxine, how you take it matters as much as the dose. The NIDDK recommends an empty stomach, 30-60 minutes before eating. Grapefruit juice, espresso, soy products, and supplements containing iron or calcium can all interfere with absorption. If pills give you trouble, liquid and soft gel formulations are now available.
Sleep is more complicated with Hashimoto's because thyroid hormones influence sleep architecture, and poor sleep worsens thyroid function. It is a feedback loop. Aim for 7-9 hours, keep consistent sleep and wake times, and look into sleep-disrupting symptoms like restless legs (which can be related to iron deficiency in hypothyroid patients).
Finally, track your patterns, not just lab values. A simple log of energy levels, mood, digestive function, and menstrual patterns alongside your lab results helps you and your doctor spot trends that raw numbers miss. Some patients feel best at a TSH of 1.0. Others are fine at 3.0. There is no universal number.
Frequently Asked Questions
Can Hashimoto's be reversed or cured?
No. There is no cure. The autoimmune process cannot be fully stopped with current treatments. What you can do is manage the hypothyroidism it causes (levothyroxine works well for that) and potentially reduce antibody levels through selenium, stress management, and dietary changes. Some patients see meaningful drops in TPOAb with selenium, but the autoimmune tendency itself remains.
Should everyone with Hashimoto's go gluten-free?
Not necessarily. Current meta-analyses show mixed results for gluten-free diets in Hashimoto's patients without celiac disease. The strongest benefits appear in patients who also have gluten-related conditions. If you experience digestive symptoms alongside your thyroid issues, a trial elimination may be worthwhile — but blanket gluten avoidance for all Hashimoto's patients is not supported by the available evidence. Discuss this with your doctor before making major dietary changes.
How much selenium should I take for Hashimoto's?
Most clinical trials showing benefits used 200 micrograms per day of selenomethionine for 3-6 months. This is also achievable through food — 2-3 Brazil nuts daily provide roughly this amount, though content varies. Do not exceed 400 micrograms per day from all sources combined, as selenium toxicity can cause hair loss, nausea, and nerve damage. Always discuss supplementation with your healthcare provider, especially if you are already taking thyroid medication.
Can you have Hashimoto's with normal thyroid levels?
Yes. In the early stages of Hashimoto's, the thyroid may still produce sufficient hormones to keep TSH within the normal range, even while antibodies are actively attacking the gland. This is called euthyroid Hashimoto's. The autoimmune process may be detectable through elevated TPOAb or TgAb before any changes appear in TSH or thyroid hormone levels. This is one reason why antibody testing is important when Hashimoto's is suspected.
Does Hashimoto's affect pregnancy?
It can, yes. Untreated hypothyroidism raises the risk of miscarriage, preeclampsia, and preterm delivery. If you have Hashimoto's and are pregnant or trying to get pregnant, close thyroid monitoring is non-negotiable. Iodine needs go up during pregnancy, but too much iodine can cause a goiter in the baby, so work with your doctor on the right balance.
Related Articles
- Leaky Gut Syndrome — Symptoms, Causes, and Evidence-Based Healing — How intestinal permeability connects to autoimmune conditions like Hashimoto's.
- Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition — The gut-brain connection that influences depression and brain fog in thyroid conditions.
- Iron Deficiency in Women — Symptoms, Testing, and Recovery — Iron's role in thyroid function and why deficiency compounds Hashimoto's fatigue.
- Seed Cycling for Hormone Balance — Does It Work? — Selenium-rich seeds and their connection to thyroid hormone metabolism.
- Bone Broth Benefits for Gut Healing, Joints, and Skin — Gut-supportive amino acids that may benefit autoimmune thyroid conditions.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.