When does poor sleep become a sleep disorder?
Most adults have rough nights. That alone does not mean you have a medical disorder. A sleep disorder is usually diagnosed when sleep trouble is persistent, causes daytime problems, and does not improve with basic behavior changes. If you have trouble falling asleep three nights a week for months, if you wake unrefreshed despite enough time in bed, or if sleepiness is affecting your driving, mood, or job performance, it is time to look at this more seriously.
Public health data suggest this is common, not rare. The Centers for Disease Control and Prevention (CDC) notes that healthy sleep is linked to lower risk of chronic disease, better emotional regulation, and safer daily functioning. In other words, sleep is not a luxury layer on top of health. It is part of the foundation.
People often wait too long to seek help because they normalize exhaustion. They say things like, "I have always been a light sleeper," or "This is just stress." Sometimes that is true. Often it is not. Persistent insomnia, sleep apnea, circadian rhythm disorders, restless legs syndrome, parasomnias, and narcolepsy all have distinct patterns that can be identified and treated.
Quick reality check: if poor sleep is affecting your attention, mood stability, blood pressure, blood sugar control, or relationship quality, it has already crossed from inconvenience into health issue.
Another clue: if your sleep schedule keeps drifting later and later, and weekends become recovery marathons, your circadian system may be misaligned. If your partner reports loud snoring, gasping, or pauses in breathing, think sleep apnea until proven otherwise. If your legs feel impossible to keep still in the evening, restless legs syndrome may be in play. The point is simple: persistent patterns matter more than isolated nights.
Your sleep system in plain English
Sleep is controlled by two overlapping systems. First is the circadian clock, which helps time sleep and wake across roughly 24 hours. Morning light pushes that clock earlier. Bright light at night pushes it later. Second is sleep pressure, the biological drive that builds while you are awake and drops once you sleep. Good sleep usually happens when these two systems line up: strong sleep pressure at night, strong circadian alertness in the morning.
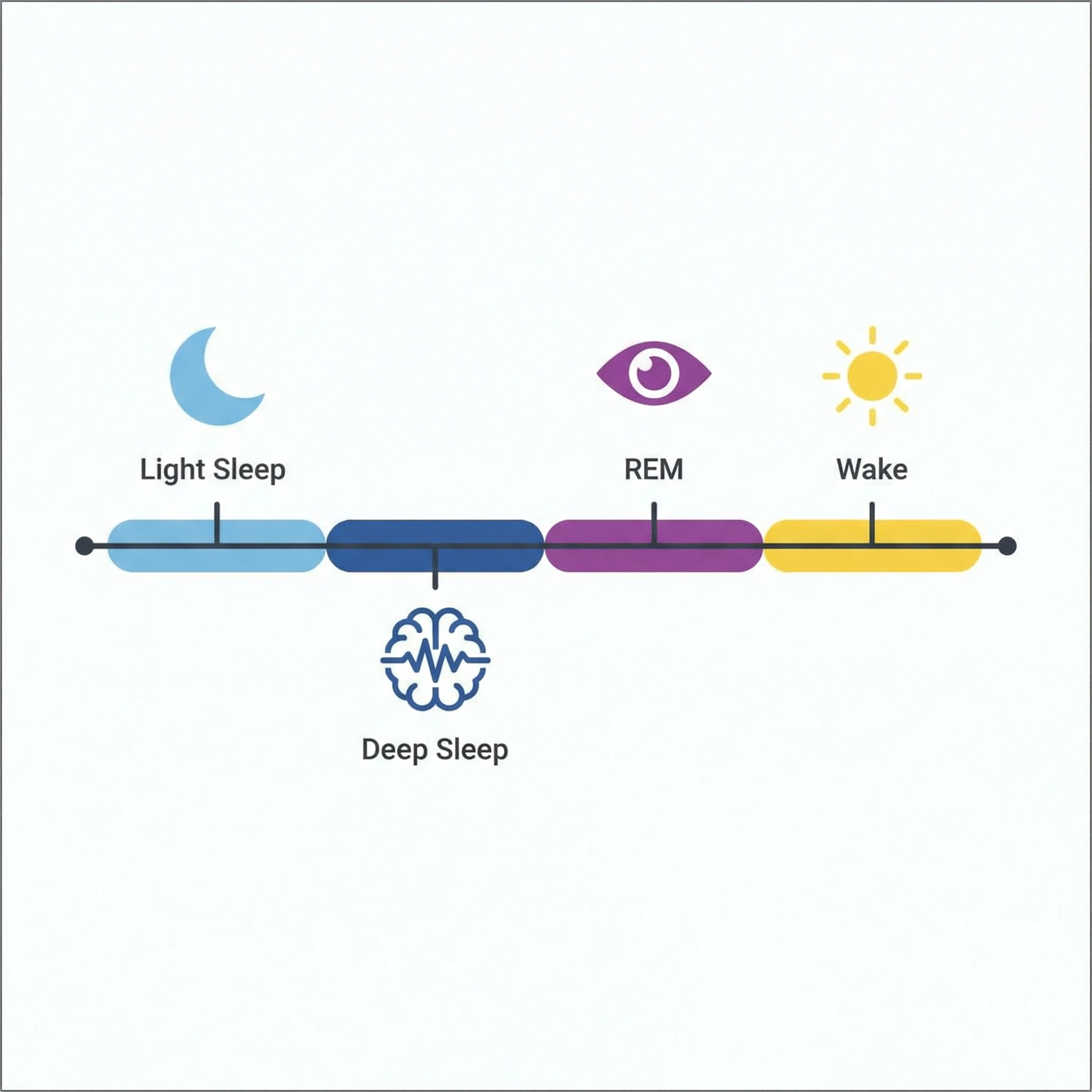
During a normal night, you cycle through non-REM and REM stages. Non-REM includes lighter sleep and deep slow-wave sleep. REM sleep is where vivid dreaming is common and emotional memory processing is active. The National Heart, Lung, and Blood Institute explains that reduced sleep quality and shorter sleep duration are linked with metabolic and cardiovascular risk, which is one reason fragmented sleep can feel so punishing even when total hours look acceptable.
| Sleep stage | What it does | What disruption feels like |
|---|---|---|
| Light non-REM (N1/N2) | Transition into stable sleep, reduced awareness of environment | Frequent awakenings, feeling like you were "half awake" all night |
| Deep non-REM (N3) | Physical recovery, immune and hormonal restoration | Morning heaviness, body fatigue, poor recovery from exercise |
| REM sleep | Memory integration, emotional processing, dream activity | Irritability, emotional reactivity, poor concentration |
When people say, "I slept eight hours but I still feel terrible," stage fragmentation is often part of the story. Sleep can look long on paper and still be low quality if breathing interruptions, limb movements, pain, or anxiety are repeatedly pulling the brain toward wakefulness.
This is also why one-size-fits-all advice fails. Someone with delayed sleep phase disorder may not need sedatives; they may need structured wake time plus morning light. Someone with obstructive sleep apnea may not need sleep teas; they may need airway treatment. The same symptom, "I am exhausted," can come from very different mechanisms.
The sleep disorders clinicians see most often
Insomnia disorder is the most frequent diagnosis. It means persistent difficulty falling asleep, staying asleep, or waking too early, with daytime consequences. It can be triggered by stress, illness, shift changes, or pain, then continue because the brain learns to associate bed with alertness and frustration. This is one reason cognitive behavioral therapy for insomnia (CBT-I) is considered first-line in many guidelines.
Obstructive sleep apnea is also common and often missed. It involves repeated upper-airway collapse during sleep, causing oxygen dips and micro-awakenings. Classic signs include loud snoring, choking or gasping, morning headaches, dry mouth, and severe daytime sleepiness. The NHLBI overview of sleep apnea and related guideline literature both emphasize that untreated apnea raises cardiovascular risk and can impair cognition and mood.
Circadian rhythm sleep-wake disorders include delayed sleep phase, shift work disorder, and irregular sleep-wake rhythm. These are timing disorders: the body clock and social obligations are out of sync. If you can sleep well on your preferred schedule but not on required schedules, this becomes more likely.
Narcolepsy is less common but important because it is frequently misinterpreted as laziness, depression, or burnout. The National Institute of Neurological Disorders and Stroke describes narcolepsy as a neurologic condition affecting sleep-wake regulation, often with overwhelming daytime sleepiness and, in some cases, cataplexy.
Parasomnias include behaviors such as sleepwalking, confusional arousals, night terrors, and REM sleep behavior disorder. These conditions can cause injury risk and severe sleep disruption for household members, so safety planning matters as much as symptom control.
| Disorder | Typical clues | First useful next step |
|---|---|---|
| Insomnia disorder | Sleep initiation/maintenance difficulty for months, daytime fatigue, worry about sleep | Sleep diary for 2 weeks and CBT-I referral |
| Obstructive sleep apnea | Loud snoring, witnessed apneas, daytime sleepiness, morning headaches | Clinical screening and home sleep apnea test or polysomnography |
| Circadian rhythm disorder | Sleep schedule drifts late, social jet lag, better sleep on free days | Fixed wake time, morning light timing plan, behavior coaching |
| Restless legs syndrome | Urge to move legs at rest, worse at night, temporary relief with movement | Clinical evaluation, iron status review, trigger reduction |
| Narcolepsy | Severe daytime sleepiness, sudden sleep episodes, possible cataplexy | Specialist sleep medicine workup with targeted testing |
If you are unsure where you fit, start by tracking a simple pattern: bedtime, wake time, awakenings, naps, caffeine timing, and next-day alertness. Good diagnostic conversations become much easier when this pattern is visible.
Why sleep problems become chronic
Early sleep disturbance is often caused by a real trigger: stress, grief, a new baby, pain flare, travel, menopause symptoms, medication side effects, or schedule changes. Chronic sleep disturbance is maintained by reinforcement loops. You start spending extra time in bed to "catch up." You nap long in the afternoon. You check the clock repeatedly at 2:40 a.m. You become hyper-alert to every awakening. All of that makes nighttime wakefulness more likely.
Mental health and sleep are deeply bidirectional. Anxiety increases arousal and rumination at bedtime. Depression can alter sleep architecture and wake timing. Chronic sleep loss increases emotional volatility, which then worsens anxiety and depression symptoms. If stress is a major factor for you, practical daytime regulation can help; resources like evidence-informed breathing routines and a structured meditation practice can support a broader treatment plan when used consistently.
Substances play a major role too. Caffeine blocks adenosine signaling and can delay sleep even when you feel "used to it." Alcohol may speed sleep onset but fragments second-half sleep. Nicotine is stimulating. Some over-the-counter sleep aids can leave next-day sedation, and regular use may create dependence patterns for some people.

| Risk factor | How it affects sleep biology | Action that usually helps |
|---|---|---|
| Late caffeine | Blocks sleep pressure buildup and delays sleep onset | Move last caffeine earlier in the day and taper dose |
| Irregular wake time | Weakens circadian stability | Set one wake time all week, including weekends |
| Long evening screen exposure | Evening light delays melatonin timing | Dim lights 1 to 2 hours before bed, use wind-down routine |
| Untreated pain or reflux | Increases nighttime arousals and micro-awakenings | Address underlying condition with clinician-guided plan |
| High cognitive arousal | Keeps autonomic system in alert mode at bedtime | Scheduled worry time, journaling, and structured relaxation |
Supplements are a common question. The NCCIH overview on sleep and complementary health approaches is useful because it separates what has decent evidence from what mostly has hype. Some people may get modest benefit from targeted approaches, but supplement quality, interactions, and correct indication matter. "Natural" does not mean low-risk.
If you are considering CBD products specifically, read labels carefully and talk with your clinician about medication interactions. We cover that nuance in our site’s broader CBD education, including this guide on potential CBD benefits and limits. For persistent insomnia or apnea symptoms, CBD should not replace diagnostic workup.
How diagnosis and treatment actually work
Good care starts with pattern recognition, not guesswork. A strong first visit usually includes symptom timeline, sleep schedule, medical and psychiatric history, medication review, and partner observations. A sleep diary and brief questionnaires are often enough to direct next steps. Objective tests are added when needed.
Home sleep apnea testing is commonly used when obstructive sleep apnea is strongly suspected and no major complicating factors are present. In-lab polysomnography is useful when cases are complex, when parasomnias or narcolepsy are suspected, or when previous testing is inconclusive. Actigraphy can help characterize timing and rest-activity rhythms in circadian cases.
For chronic insomnia, CBT-I is often more durable than medication alone. A landmark guideline paper indexed on PubMed (Sateia et al., 2017, AASM-focused insomnia guidance) helped solidify the move toward nonpharmacologic first-line care when appropriate. Sleep medications can still be useful, especially short term or in selected patients, but usually perform best as part of a broader plan.
For obstructive sleep apnea, positive airway pressure therapy remains a core treatment. Adherence is the hard part, so mask fitting, humidification, and troubleshooting support are not extras. They are central. Evidence syntheses such as Patil et al., 2019 and related AASM literature show that treatment quality depends on practical implementation, not only the prescription itself.

| Treatment path | Best fit | Strengths | Limitations |
|---|---|---|---|
| CBT-I | Chronic insomnia with conditioned arousal | Durable benefit, improves sleep behavior and anxiety loop | Requires consistency over weeks |
| PAP therapy | Obstructive sleep apnea | Targets root breathing problem, strong evidence base | Adherence challenges without support |
| Light and schedule therapy | Circadian rhythm disorders | Addresses timing mechanism directly | Timing errors can worsen misalignment |
| Medication | Selected cases, short-term symptom control | Can reduce acute distress and improve sleep onset | Side effects, tolerance, morning sedation risk |
| Complementary approaches | Mild symptoms or adjunct support | Can support relaxation and bedtime routine | Variable evidence and product quality concerns |
If your care plan is not helping after six to eight weeks, ask for reassessment rather than quietly abandoning treatment. Many sleep plans fail because one detail is off: wrong mask style, mistimed light exposure, excessive daytime napping, untreated reflux, or unresolved anxiety spikes before bed.
A practical 30-day reset plan
This is not a miracle protocol. It is a practical structure that works for many people because it targets the main levers: timing, arousal, and behavior consistency. If you already have diagnosed apnea, narcolepsy, or another condition, use this as adjunct support, not replacement care.

- Days 1-7: Lock one wake time. Pick a realistic wake time and keep it every day. Do not compensate with long naps. If you need a nap, cap it early and short.
- Days 8-14: Build a repeatable wind-down. For 45 to 60 minutes before bed, lower light, reduce stimulation, and do the same sequence nightly. Keep it boring and predictable.
- Days 15-21: Tighten the sleep window. Spend less extra time awake in bed. If you are awake for a prolonged period, get up briefly, reset with low light, and return when drowsy.
- Days 22-30: Add daytime anchors. Morning outdoor light, regular meals, and consistent physical movement stabilize circadian timing and improve nighttime sleep drive.
If you need extra structure, our site’s practical pieces on improving sleep habits and simple sleep tips can help you map this into real daily routines.
Use a lightweight troubleshooting approach rather than all-or-nothing thinking. One poor night does not erase progress. What matters is trend. Most people who improve do so gradually over several weeks, with a few setbacks along the way.
| If this happens | Common cause | Adjustment to try for 1 week |
|---|---|---|
| You fall asleep fast but wake at 3 a.m. | Early circadian timing, stress arousal, alcohol effects | Review evening alcohol/caffeine, add pre-bed decompression, keep wake time fixed |
| You cannot fall asleep until very late | Delayed circadian phase, late light exposure | Morning bright light, earlier caffeine cutoff, reduced late-night screens |
| You are exhausted despite enough hours | Fragmented sleep, possible apnea or limb movement disorder | Seek formal sleep evaluation instead of adding more time in bed |
| You crash into long weekend sleep-ins | Weekday sleep debt and social jet lag | Limit weekend drift, protect weekday bedtime routine |
The most overlooked piece is daytime behavior. People focus on bedtime but ignore what happens from morning to evening. Light timing, meal timing, movement, and stress regulation all shape sleep readiness at night.
Myth vs fact quick reference
Sleep advice online is full of partial truths. Here is a cleaner way to think about common claims.
| Myth | Fact | What to do instead |
|---|---|---|
| If I am in bed for 9 hours, I should feel rested | Sleep quality and continuity matter as much as duration | Track awakenings, snoring, and daytime function, not only hours in bed |
| Alcohol helps me sleep better | It may speed sleep onset but fragments second-half sleep | Reduce evening alcohol and compare next-day alertness |
| Snoring is annoying but harmless | Loud habitual snoring can signal sleep apnea | Get screened, especially with daytime sleepiness or witnessed apneas |
| Sleeping pills are the only serious treatment | Behavioral treatment and disorder-specific care often produce better long-term outcomes | Ask about CBT-I, apnea treatment, and circadian planning |
| Weekend catch-up fully fixes sleep debt | It helps partially but often worsens circadian instability | Keep wake time relatively stable across the week |
None of this requires perfection. It requires consistency and the right diagnosis. If your pattern has been persistent for months, skip random hacks and get a structured evaluation.
Frequently Asked Questions
How do I know if I need a sleep study or just better sleep habits?
If symptoms are mild and short-lived, improving sleep habits is a reasonable first step. If you have loud snoring, breathing pauses, dangerous daytime sleepiness, frequent nighttime behaviors, or persistent insomnia despite routine changes, request formal evaluation and discuss sleep testing with a clinician.
Can supplements replace insomnia treatment?
For most people with chronic insomnia, supplements are not a complete treatment. Some may offer modest support in selected cases, but high-quality behavioral treatment and diagnosis of underlying contributors usually provide stronger and more durable results.
Is it normal to wake up during the night?
Brief awakenings can be normal. The concern is repeated or prolonged awakenings that leave you unrefreshed, distressed, or impaired the next day. Pattern, frequency, and daytime impact determine whether this is likely a disorder.
How long does it take to improve a chronic sleep problem?
Meaningful improvement often starts within two to four weeks of consistent changes, with larger gains over six to twelve weeks. Progress is usually uneven, so trend matters more than any single night.
Can stress management really improve sleep, or is that overhyped?
Stress regulation is not a cure-all, but it is clinically relevant. Bedtime cognitive arousal is a major insomnia driver. Practical stress tools used consistently can reduce pre-sleep activation and improve treatment response when combined with disorder-specific care.
Related Articles
- Sleep Optimization and Circadian Rhythm Technology - A focused breakdown of how light timing, routines, and modern tools affect circadian stability.
- Best Ways to Improve Your Sleep - Practical habit changes you can apply immediately when sleep quality is inconsistent.
- 10 Simple Tips to Improve Your Sleep - A concise checklist for people who want a simpler starting plan.
- The Real Damage Anxiety and Burnout Do to Your Body - Useful context on how chronic stress biology can worsen sleep and recovery.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.