Your Small Intestine Produces One of the Most Powerful Appetite Hormones Known to Science
Every time you sit down to eat, a chain reaction begins in the lining of your small intestine. Specialized cells called L-cells detect incoming nutrients and release a hormone known as glucagon-like peptide-1, or GLP-1. This hormone sets off a cascade that touches nearly every aspect of how your body handles food, from how quickly your stomach empties to whether your brain signals that you've had enough.
GLP-1 does far more than manage appetite. It stimulates insulin secretion from the pancreas, suppresses the release of glucagon (a hormone that raises blood sugar), and slows gastric emptying so nutrients enter the bloodstream gradually rather than in a flood. Researchers estimate that GLP-1 is responsible for up to 70% of the insulin your body releases after a meal in healthy individuals. That makes it one of the single most important regulators of post-meal blood sugar.
The medications that have captured headlines recently, like semaglutide and tirzepatide, work by mimicking this very hormone at supraphysiological doses. But your body already manufactures GLP-1 every day. The real question is whether you can meaningfully influence how much your body makes and how effectively it works, without a prescription. The research says yes, and the tools are surprisingly accessible.
Key point: GLP-1 blood concentrations typically range from 5 to 15 pmol/L when fasting and increase two- to fourfold after eating. However, because the enzyme DPP-IV degrades GLP-1 rapidly, its half-life is only 1 to 2 minutes. Less than 15% of newly secreted GLP-1 reaches the bloodstream intact. This means the conditions under which you eat, and what you eat, can have outsized effects on whether GLP-1 reaches meaningful levels.
The Foods That Flip the Switch on Your Body's GLP-1 Production
L-cells in the gut wall are covered with specialized receptors called G-protein coupled receptors, or GPCRs, that act like molecular antennae tuned to specific nutrients. When the right molecules pass through the intestinal lumen, they bind to these receptors and trigger GLP-1 release. Not all foods are created equal in this regard. Some nutrients are potent activators, while others barely register.
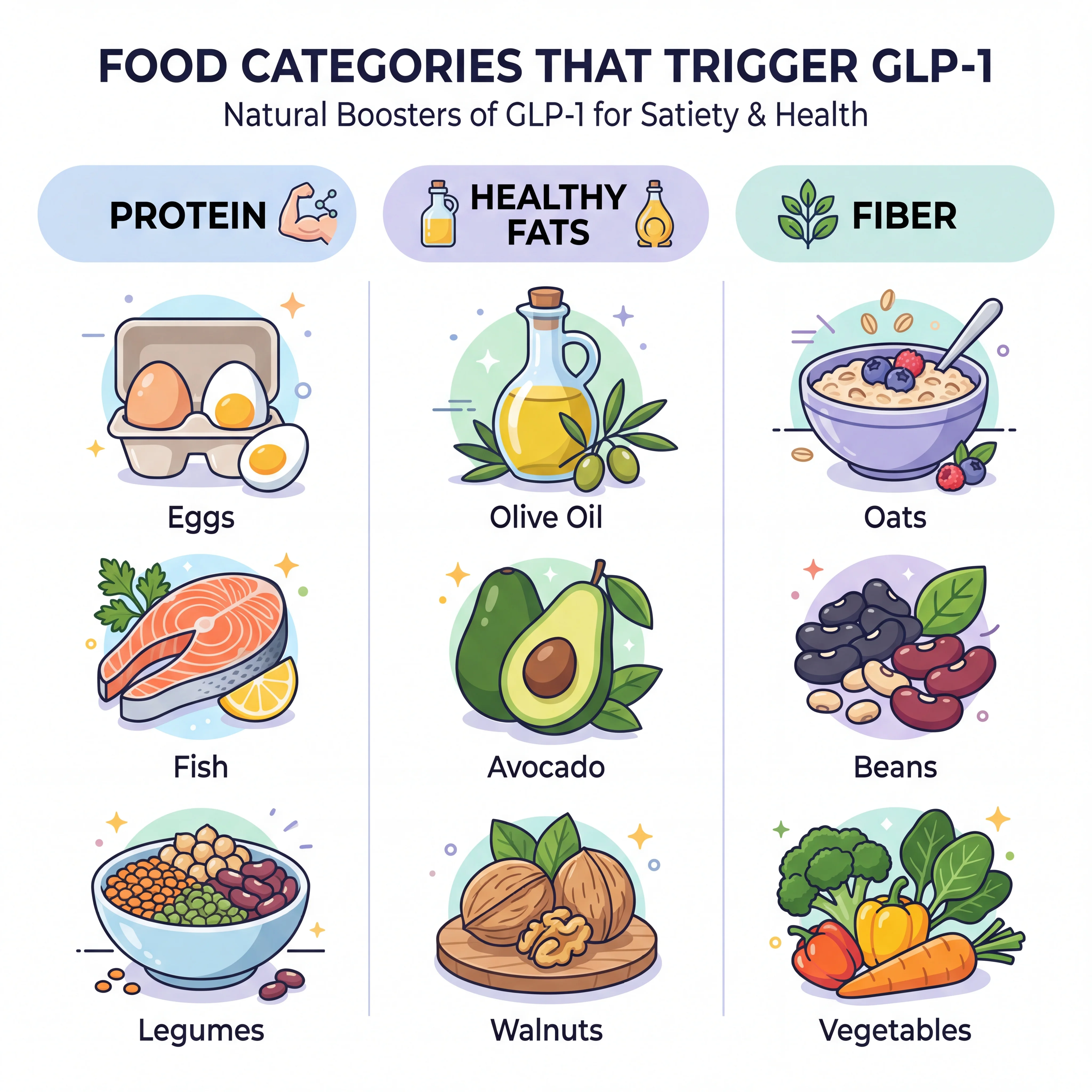
Protein: The Strongest Dietary Trigger
Of all macronutrients, dietary proteins and peptides have the most potent effect on stimulating GLP-1 secretion. When proteins break down into peptides and amino acids during digestion, they activate the calcium-sensing receptor (CaSR) on L-cells, which directly triggers hormone release. Some dietary peptides pull double duty by both stimulating GLP-1 and simultaneously reducing the activity of DPP-IV, the enzyme that destroys it. That means eating enough protein does not just produce more GLP-1 but may also help it last longer in your bloodstream.
The best options include eggs, lean poultry, wild-caught fish, legumes, and fermented soy products like tempeh. If you are focused on increasing your protein intake, aim for at least 25 to 30 grams at each meal to maximize the GLP-1 response.
Healthy Fats: Monounsaturated and Omega-3s Lead the Way
Fatty acids with chain lengths greater than 12 carbons activate two key receptors on L-cells: FFAR1 (also called GPR40) and FFAR4 (GPR120). Research published in the International Journal of Molecular Sciences found that olive oil-rich meals produced a measurably higher GLP-1 response than butter-rich meals, suggesting that unsaturated fatty acids are more effective stimulators than saturated ones. This makes sense physiologically because monounsaturated and polyunsaturated fatty acids bind more effectively to these receptors.
Prioritize extra-virgin olive oil, avocados, walnuts, chia and flax seeds, and fatty fish like salmon and sardines. These foods also slow gastric emptying, which keeps nutrients in contact with L-cells longer and extends the GLP-1 release window. Incorporating quality omega-3 fatty acids is a straightforward way to support this pathway.
Fiber: The Slow-Burn GLP-1 Activator
While protein and fat trigger GLP-1 in the upper small intestine, fiber works through a completely different mechanism in the colon. When soluble and fermentable fibers reach the large intestine, gut bacteria break them down into short-chain fatty acids (SCFAs), primarily acetate, propionate, and butyrate. These SCFAs bind to free fatty acid receptors FFAR2 and FFAR3 on colonic L-cells, triggering a sustained second wave of GLP-1 secretion.
A landmark study demonstrated that targeted delivery of propionate to the colon stimulated acute GLP-1 secretion and reduced energy intake at subsequent meals. When propionate delivery was sustained daily for six months, participants showed reductions in body weight, abdominal fat, and liver fat accumulation. Propionate proved to be the most potent activator of both FFAR2 and FFAR3 among all short-chain fatty acids.
| Nutrient Type | GLP-1 Mechanism | Best Food Sources | Where It Acts |
|---|---|---|---|
| Protein / Peptides | CaSR receptor activation + DPP-IV inhibition | Eggs, fish, legumes, tempeh | Small intestine |
| Monounsaturated fats | FFAR1 / FFAR4 receptor binding | Olive oil, avocados, almonds | Small intestine |
| Omega-3 fatty acids | FFAR4 (GPR120) activation | Salmon, sardines, walnuts, flaxseed | Small intestine |
| Fermentable fiber | SCFA production → FFAR2/FFAR3 binding | Oats, barley, beans, artichokes | Colon (large intestine) |
| Resistant starch | Bacterial fermentation → SCFA release | Cooled potatoes, green bananas, raw corn starch | Colon (large intestine) |
Eating the Same Foods in a Different Order Changes Your Hormonal Response
Here is something most people overlook: the sequence in which you eat the components of your meal can substantially alter how much GLP-1 your body releases. Eating protein and fat alongside dietary fiber before touching your carbohydrates creates a much stronger GLP-1 response compared to eating carbohydrates first. This is not a marginal difference. The downstream effects include higher insulin secretion, slower gastric emptying, and measurably lower post-meal blood sugar spikes.

The logic behind this is straightforward. When protein and fat reach L-cells first, they prime the GLP-1 system before a glucose load arrives. By the time carbohydrates begin breaking down into glucose, insulin secretion is already enhanced, and stomach emptying has already slowed. The net result is a smoother, more controlled glucose curve.
How You Eat Matters as Much as What You Eat
Eating speed also plays a measurable role. Research has shown that eating slowly leads to more pronounced GLP-1 secretion, higher satiety, and lower overall food intake. Taking smaller bites and chewing more thoroughly extends the time that nutrients spend in contact with the GLP-1-producing cells of the intestinal lining. Setting a timer for 20 to 30 minutes per meal, putting your fork down between bites, and focusing on the textures and flavors of your food are practical strategies that require zero supplements and zero expense.
Circadian Timing: Front-Load Your Calories
GLP-1 follows a circadian rhythm, with higher natural levels during the daytime and lower levels overnight. Eating your largest meal earlier in the day aligns with this biological pattern and may optimize GLP-1 function. Practical recommendations include eating your first meal within one to two hours of waking, distributing calories more heavily toward breakfast and lunch, and maintaining at least a two-hour gap between your last substantial meal and bedtime. If you practice intermittent fasting, timing your eating window to align with daylight hours may further support GLP-1 regulation.
| Eating Strategy | Effect on GLP-1 | How to Implement |
|---|---|---|
| Protein and vegetables before carbs | Enhanced GLP-1 secretion and lower blood sugar | Eat salad and protein portions first at each meal |
| Slower eating pace | More pronounced GLP-1 response | Set 20-30 min timer; put fork down between bites |
| Smaller bites, more chewing | Increased GLP-1 and reduced food intake | Chew each mouthful 20-30 times |
| Front-loaded calories | Aligns with circadian GLP-1 peak | Larger breakfast/lunch, lighter dinner |
| Consistent meal schedule | Supports circadian GLP-1 rhythms | Eat within a 12-hour window at regular times |
30 Minutes of Movement Reshapes Your GLP-1 Response for Hours
Exercise is one of the most well-studied natural amplifiers of GLP-1, but the relationship is more complex than just "work out more". A large cross-sectional study of 1,326 individuals found that for every additional hour of moderate-intensity physical activity performed daily, fasting GLP-1 concentrations were 20% lower while glucose-stimulated GLP-1 responses were 16 to 20% greater. In other words, habitual exercisers had a more efficient GLP-1 system: lower baseline levels but a stronger surge when it was actually needed, after eating.
Multiple studies confirm that both moderate-intensity exercise (50 to 75% of maximum oxygen uptake) and high-intensity exercise (85 to 90% of maximum heart rate) increase GLP-1 levels in healthy and overweight individuals. A 12-week supervised chronic exercise program was shown to increase postprandial GLP-1 levels in overweight and obese participants. High-intensity interval training appeared to have an edge over steady-state exercise in some studies, though consistency matters more than any single workout format.
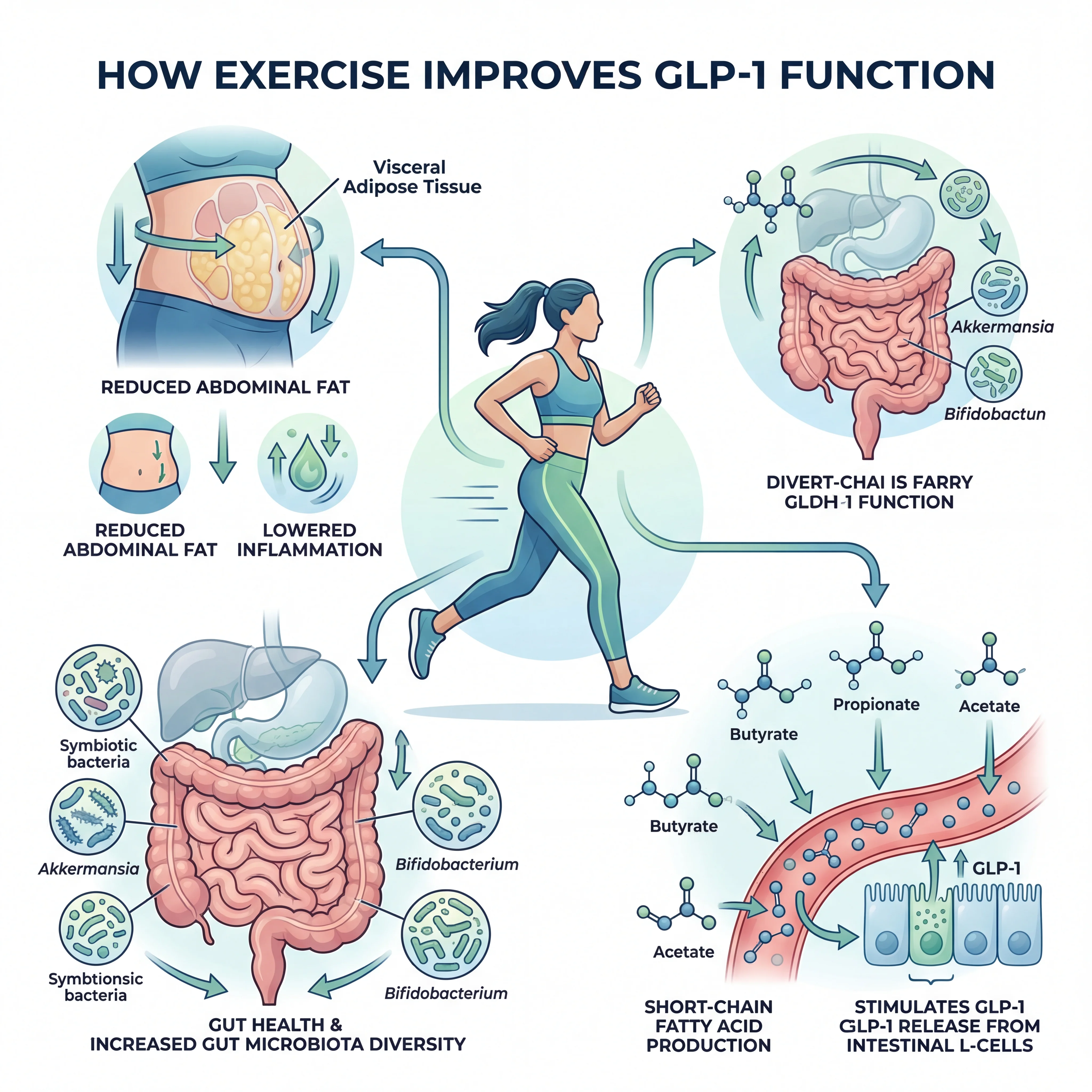
Exercise Fixes GLP-1 Resistance, Not Just GLP-1 Levels
The most interesting finding is not that exercise raises GLP-1 but that it may fix a deeper problem. In people with type 2 diabetes and obesity, the issue is often not inadequate GLP-1 production but GLP-1 resistance, a state where the hormone is present but the body fails to respond properly. Research published in the World Journal of Diabetes suggests that exercise improves GLP-1 resistance rather than simply increasing GLP-1 secretion. It does this through at least three mechanisms: reducing visceral fat (which itself causes GLP-1 resistance), increasing gut microbiota diversity, and boosting the production of short-chain fatty acids that activate L-cell receptors.
The combination of aerobic and resistance training appears particularly effective. Contracting skeletal muscle during exercise releases myokines, anti-inflammatory signaling molecules that reduce ectopic fat deposits around the pancreas and other organs. Research has shown that exercise training can decrease pancreatic fat and improve beta-cell function in individuals with prediabetes and type 2 diabetes.
The Trillions of Bacteria in Your Gut Directly Control GLP-1 Output
If there is one area of GLP-1 research generating the most excitement, it is the gut microbiome connection. The bacteria living in your large intestine are not passive bystanders. They are active participants in GLP-1 regulation, and when their community falls out of balance, the entire system breaks down.
A 2017 study published in Cell Metabolism demonstrated that gut microbiota dysbiosis directly causes GLP-1 resistance in the enteric nervous system of diabetic mice. The researchers found that the relative abundance of Lactobacillus species was positively correlated with GLP-1 receptor expression, while an overgrowth of Bacteroidales was negatively correlated. This means the composition of your gut bacteria literally determines how responsive your body is to the GLP-1 it produces.
Short-chain fatty acids are the key link. When beneficial bacteria ferment dietary fiber, they produce acetate, propionate, and butyrate. These SCFAs bind to FFAR2 and FFAR3 receptors on colonic L-cells. In cell culture studies, physiological concentrations of all three SCFAs stimulated GLP-1 secretion, and this effect was completely abolished when FFAR2 and FFAR3 receptors were knocked out. The colonic molar ratio of these fatty acids is approximately 50 to 60% acetate, 15 to 20% propionate, and 10 to 20% butyrate.
To support this system, focus on feeding your beneficial gut bacteria with fermentable fibers from whole grains, legumes, and vegetables. Fermented foods like yogurt, kefir, sauerkraut, kimchi, and miso supply live bacterial cultures that can shift microbiome composition. Research on Akkermansia and other metabolic health probiotics suggests that specific bacterial strains may have particularly strong effects on incretin hormone regulation.
| Microbiome Strategy | Mechanism | Timeline for Results |
|---|---|---|
| Fermentable fiber intake (16+ g/day) | Increases SCFA production → L-cell activation | 2-4 weeks for measurable GLP-1 changes |
| Daily fermented foods | Increases microbial diversity | 4-6 weeks for microbiome shifts |
| Regular exercise | Increases gut bacterial diversity and SCFA output | 6-12 weeks for sustained changes |
| Prebiotic-rich foods (onions, garlic, asparagus) | Selectively feeds beneficial bacteria | 2-4 weeks |
| Reducing processed food intake | Reduces dysbiosis and inflammation | 2-6 weeks |
Plant Compounds That Act as Natural GLP-1 Amplifiers
Beyond macronutrients and fiber, a growing body of research has identified specific plant compounds that influence GLP-1 pathways. A review published in Advances in Experimental Medicine and Biology cataloged several herbal-based constituents with modulatory effects on GLP-1 expression and secretion, including berberine, green tea catechins, curcumin, cinnamon, resveratrol, and soybean isoflavones.
Berberine deserves particular attention. This alkaloid, found in goldenseal and Oregon grape root, has demonstrated consistent GLP-1-enhancing effects in multiple studies. It appears to work through several parallel mechanisms: directly stimulating L-cell secretion, inhibiting DPP-IV activity to extend GLP-1 half-life, and improving gut microbiome composition. These overlapping effects make it one of the more compelling natural GLP-1 support options currently studied.
Quercetin, a flavonoid abundant in onions, apples, and berries, can directly stimulate GLP-1 secretion from enteroendocrine cells. Dark chocolate (at least 70% cacao) provides flavanols that may support GLP-1 activity, though it should be consumed in modest portions of about one ounce per day to avoid excess calories. Green tea catechins, particularly EGCG, and curcumin from turmeric have also shown GLP-1-enhancing properties in preclinical research.

Research spotlight: Scientists at Purdue University are developing a food-based supplement combining raw corn starch (which digests at the right rate to reach distal L-cells) with fermentable fiber that generates SCFAs in the large intestine. Early animal studies showed reduced food intake and activation of the hypothalamic appetite control center. Human trials are underway at an Indiana pediatric obesity clinic. As lead researcher Bruce Hamaker explains: "This is our natural system for appetite regulation. Triggering it naturally shouldn't have any side effects."
Myth vs. Fact: Separating Real GLP-1 Strategies from Wishful Thinking
The popularity of GLP-1 medications has spawned an enormous amount of misinformation about natural alternatives. It is important to set realistic expectations based on what the science actually shows.
| Claim | Verdict | What the Evidence Says |
|---|---|---|
| Natural methods can replace Ozempic | Myth | GLP-1 medications produce supraphysiological hormone levels with extended half-lives. Natural approaches work within normal physiological ranges and produce modest but meaningful benefits. |
| High-protein meals boost GLP-1 | Fact | Dietary peptides and amino acids are among the most potent direct stimulators of L-cell GLP-1 release via the CaSR receptor. |
| Any fiber increases GLP-1 | Partially true | Only fermentable fiber that produces SCFAs in the colon triggers the FFAR2/FFAR3 pathway. Insoluble fiber like wheat bran passes through without significant SCFA production. |
| Exercise raises GLP-1 levels | Fact (with nuance) | Exercise actually lowers fasting GLP-1 but increases the meal-stimulated response, making the system more efficient. It also reduces GLP-1 resistance. |
| Apple cider vinegar boosts GLP-1 | Unproven | While vinegar may improve blood sugar responses through other mechanisms, there is no strong evidence it directly increases GLP-1 secretion. |
| Gut health affects GLP-1 | Fact | Microbiota dysbiosis directly causes GLP-1 resistance. Restoring bacterial balance via fermented foods, fiber, and exercise improves GLP-1 signaling. |
The most important distinction to understand: GLP-1 medications like semaglutide act through a purely endocrine pathway at concentrations far beyond what the body naturally produces, while endogenous GLP-1 employs both endocrine and neuronal routes. This dual signaling means that natural GLP-1 may not need to reach the same astronomical blood levels to exert beneficial effects. After Roux-en-Y gastric bypass surgery, GLP-1 levels increase up to fourfold, which is still within normal physiological ranges, yet this increase is associated with meaningful improvements in dietary choices, weight loss, glycemic control, and even diabetes resolution in some cases.
Natural GLP-1 enhancement is not about replacing medication for people who need it. It is about optimizing a system that everyone has and that most people are underutilizing. For individuals who do not qualify for or choose not to take GLP-1 medications, and for those coming off them, these strategies can provide a meaningful foundation for gut health and metabolic function.
Frequently Asked Questions
How quickly can dietary changes affect GLP-1 levels?
Individual meals can alter your GLP-1 response immediately. A single protein-rich meal triggers measurably higher GLP-1 secretion compared to a carbohydrate-heavy one. Longer-term strategies like increasing fermentable fiber intake or incorporating fermented foods typically take two to six weeks to produce sustained changes in baseline GLP-1 function, as they depend on shifts in gut microbiome composition.
Can natural GLP-1 strategies cause the same side effects as GLP-1 medications?
Generally no. GLP-1 medications produce supraphysiological hormone levels, which is why nausea, vomiting, and gastrointestinal discomfort are common side effects. Natural approaches work within your body's normal physiological range, so the GLP-1 increases are modest and unlikely to cause these issues. That said, significantly increasing fiber intake too quickly can cause bloating and gas, so it is best to increase fiber gradually over two to three weeks.
Does intermittent fasting increase or decrease GLP-1?
The relationship is complex. Fasting itself lowers GLP-1 levels because there are no nutrients to stimulate L-cells. However, after a fasting period, the post-meal GLP-1 response may be enhanced, partly because insulin sensitivity improves with fasting. The key is timing your eating window to align with your circadian GLP-1 peak, which occurs during daytime hours.
Which type of exercise is best for GLP-1 improvement?
Both moderate-intensity cardio and high-intensity interval training have been shown to improve GLP-1 responses. The combination of aerobic and resistance training appears to be especially effective because it addresses GLP-1 resistance through multiple pathways: reducing visceral fat, improving gut microbiota diversity, and increasing SCFA production. Consistency matters more than intensity for most people.
Are there any supplements proven to increase GLP-1?
Berberine has the strongest evidence base for GLP-1 enhancement among supplements, with effects on L-cell secretion, DPP-IV inhibition, and microbiome composition. Green tea extract (EGCG), curcumin, and quercetin have shown GLP-1-stimulating effects in laboratory and some animal studies, but large-scale human trials are still limited. Prebiotic fiber supplements that increase colonic SCFA production also have reasonable evidence behind them.
Related Articles
- Berberine for Blood Sugar and Weight Management - A deep dive into one of the most studied natural compounds for metabolic health and GLP-1 support.
- Akkermansia: The Probiotic for Metabolic Health - How specific gut bacteria influence incretin hormone regulation and metabolic function.
- Intermittent Fasting Schedules: 16:8, 20:4, and OMAD Compared - Understanding how different fasting protocols interact with appetite hormones including GLP-1.
- Omega-3 Benefits, Sources, and Supplements - The essential fatty acids that activate GLP-1 receptors and support metabolic health.
- Gut Health Personalization and Microbiome Testing - How to assess and optimize the bacterial ecosystem that controls your GLP-1 response.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.