What GLP-1 drugs actually do inside your body
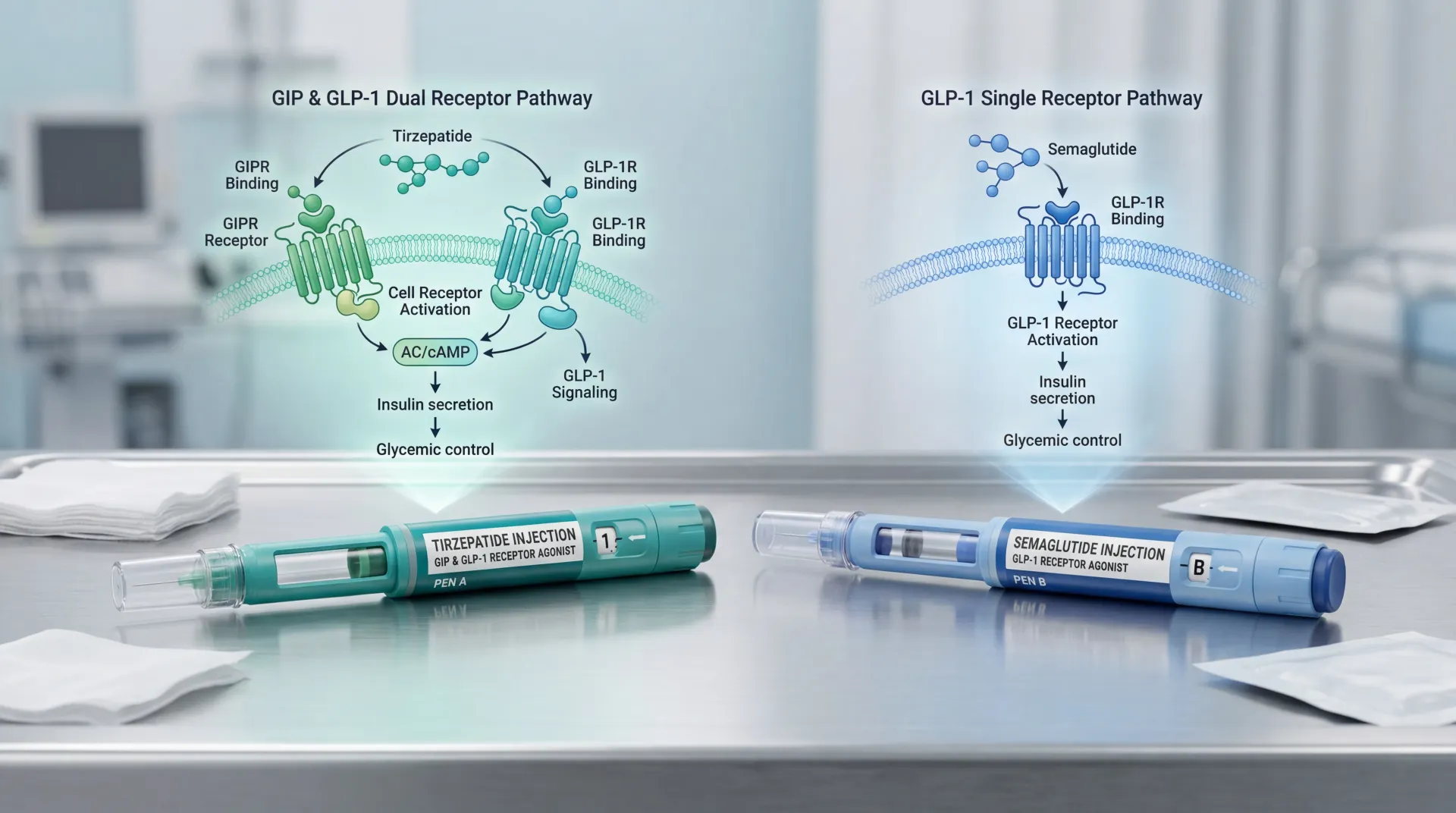
GLP-1 receptor agonists mimic a gut hormone called glucagon-like peptide-1. Your intestines release it naturally after eating, but drugs like semaglutide (Ozempic, Wegovy) and tirzepatide (Mounjaro, Zepbound) deliver a synthetic version that lasts much longer than the natural hormone, which breaks down in minutes.
These drugs work on three fronts simultaneously. In the pancreas, they boost insulin secretion and suppress glucagon, which lowers blood sugar. In the stomach, they slow gastric emptying so food sits longer, making you feel full faster. And in the brain, they act on the hypothalamus and reward centers, reducing what researchers call "food noise" -- the constant mental background chatter about eating.
Quick fact: Semaglutide produces roughly 15% total body weight loss. Tirzepatide, which targets both GLP-1 and GIP receptors, averages around 22.5% in the SURMOUNT-1 trial. The newest drug, retatrutide, which hits three receptors (GLP-1, GIP, and glucagon), showed nearly 29% weight loss in Phase III trials.
The weight loss numbers are real. But the conversation around these drugs rarely gets past those numbers into what else they do to the body, or how celebrity culture has turned a medical treatment into a cosmetic trend. If you're considering a GLP-1 drug for weight loss, the full picture is more complicated than the headlines suggest.
The muscle problem nobody talks about
Here's the part that gets buried in the marketing: up to 40% of the weight you lose on GLP-1 drugs isn't fat. It's lean body mass -- muscle, bone density, connective tissue. A Circulation study published in 2024 found this ratio is roughly consistent across semaglutide and tirzepatide.
A University of Virginia Health study found that GLP-1 drugs failed to improve body composition in the way researchers expected. Patients lost weight, yes, but the fat-to-lean ratio of that loss was concerning. The University of Utah raised similar flags, reporting measurable reductions in both muscle size and grip strength.
This matters for several reasons. Muscle drives your resting metabolic rate. Lose enough of it and your body burns fewer calories at rest, which sets up a metabolic trap when you stop the drug. For older adults, the musculoskeletal effects are especially risky, increasing fracture risk and accelerating sarcopenia.
| Drug | Receptors targeted | Average weight loss | Lean mass lost (% of total) |
|---|---|---|---|
| Semaglutide (Wegovy) | GLP-1 | ~15% | 25-39% |
| Tirzepatide (Zepbound) | GLP-1 + GIP | ~22.5% | 25-40% |
| Retatrutide (Phase III) | GLP-1 + GIP + Glucagon | ~28.7% | Under investigation |
Resistance training and adequate protein intake (1.2-1.6 g/kg daily) can slow muscle loss during GLP-1 therapy. A Massachusetts General Hospital program now requires both as part of any GLP-1 weight loss prescription. This should be standard practice, not an afterthought.
Ozempic face and the GI side effects
"Ozempic face" isn't just a social media buzzword. It's what happens when subcutaneous fat disappears from the face faster than skin can contract. The face loses volume in the cheeks, around the eyes, and along the jawline, producing a gaunt, aged appearance. Cleveland Clinic dermatologists attribute it to both fat loss and reduced collagen synthesis that accompanies rapid weight change.
According to Healio's dermatology reporting, the facial aging effect can add years to a patient's appearance in a matter of months. The PMC literature on the phenomenon confirms that the skin's elastic fibers simply cannot keep pace with the rate of subcutaneous fat depletion.
The gastrointestinal side effects are more medically concerning. These drugs slow your stomach to the point where food can sit for hours, sometimes days.
| Side effect | Frequency | Severity |
|---|---|---|
| Nausea | 30-44% of patients | Usually mild, fades over weeks |
| Vomiting | 15-25% | Moderate; dose-related |
| Gastroparesis | Rare but documented | Severe; case reports of prolonged paralysis |
| Intestinal obstruction | Rare | Severe; FDA added to label warnings |
| Pancreatitis | Rare | Potentially life-threatening |
A systematic review and meta-analysis of semaglutide and tirzepatide trials found gastrointestinal adverse events in a significant portion of patients. The University of British Columbia linked GLP-1 drugs specifically to gastroparesis, pancreatitis, and bowel obstruction at higher rates than previously reported. If you're evaluating semaglutide side effects, the GI risks deserve serious weight in that decision.
Why stopping means gaining it all back
The STEP 1 trial extension tracked what happened after patients stopped semaglutide. Within a year, they regained two-thirds of the weight they'd lost. A BMJ meta-analysis published in 2025 confirmed this pattern across multiple drugs: most weight comes back within 12-18 months of stopping.
An Oxford University study from January 2026 found something even more troubling: weight regain after stopping GLP-1 drugs was faster than regain after ending a conventional diet. The drugs don't fix the underlying metabolic drivers of obesity. They suppress appetite and slow digestion. Remove them, and the hunger returns -- along with a body that now has less muscle and a lower resting metabolic rate.
The math problem: If you lose 30 pounds on semaglutide but 12 of those pounds were muscle, and then you regain 20 pounds (almost entirely as fat), you end up with more body fat and less muscle than when you started. This is the "yo-yo" metabolic trap that researchers are calling a critical gap in the current treatment model.
This is why the pharmaceutical model increasingly assumes lifetime use. Novo Nordisk and Eli Lilly aren't marketing a treatment course. They're marketing a permanent prescription. At $1,000+ per month without insurance, that raises obvious questions about who gets to stay thin and who doesn't.
The eating disorder question
GLP-1 drugs quiet "food noise." For people with obesity and binge eating disorder, this can be genuinely therapeutic. A systematic review found preliminary evidence that GLP-1 receptor agonists reduce binge episodes. For some patients, the relief of not thinking about food constantly is life-changing.
But the same mechanism that helps binge eaters can be dangerous for people with restrictive eating disorders. The Guardian reported on eating disorder clinicians seeing patients use GLP-1 drugs to reinforce anorexic behavior -- the drug providing medical cover for what would otherwise be recognized as pathological restriction. ANAD (National Association of Anorexia Nervosa and Associated Disorders) and Penn Medicine have both published clinical guidance flagging this risk.
A 2026 ASU study found that body image dissatisfaction, not medical need, was the primary driver of GLP-1 interest among non-obese users. Research published in PubMed confirmed the same pattern: body image concerns predict GLP-1 interest more strongly than BMI does. When cosmetic weight loss becomes the primary use case for a metabolic drug, the line between treatment and harm gets hard to see. If you're working on your relationship with food and body image, our guide to daily mental health management covers evidence-based approaches that don't carry these risks.
Celebrity bodies, public shaming, and Selena Gomez
Selena Gomez lives with lupus. She had a kidney transplant in 2017. She takes immunosuppressants that cause weight fluctuation. She also has SIBO (small intestinal bacterial overgrowth), which causes bloating, abdominal distention, and unpredictable weight changes.
None of this has stopped the internet from speculating about whether she's on Ozempic every time her body changes. When she appeared thinner at the 2025 SAG Awards, commenters demanded she "admit" to using weight loss drugs. When she looked heavier at the Emilia Perez premiere, she was body-shamed for gaining weight. She has publicly addressed this, explaining her conditions. It hasn't stopped the scrutiny.
This is the cultural problem GLP-1 drugs have created. When a drug can produce dramatic weight loss, every thin celebrity becomes a suspect. And every celebrity who doesn't use it -- or whose body doesn't conform -- becomes a target. CBC News documented how the cycle works: fat-shaming pushes celebrities toward weight loss, then thin-shaming targets them if they succeed "too much" or "too fast."
The UCSD Guardian framed it directly: Hollywood's relationship with GLP-1 drugs has turned into an epidemic of its own, where the cosmetic use of medical treatments has become normalized among people who don't meet any clinical criteria for obesity. A PMC review called it the "prescription to trend" pipeline -- social media accelerating demand for a drug that many users don't medically need.
| Medical use | Cosmetic use |
|---|---|
| BMI 30+ (obesity) or 27+ with comorbidities | Often BMI under 27 with no metabolic condition |
| Prescribed after lifestyle interventions fail | Sought as first-line approach |
| Monitored by endocrinologist | Often obtained through telehealth without follow-up |
| Combined with nutrition and exercise plans | Rarely paired with muscle preservation strategies |
| Insurance may cover (for eligible patients) | Typically out-of-pocket ($1,000+/month) |
This isn't a simple "drugs bad" argument. For people living with obesity-related health conditions, GLP-1 drugs can reduce cardiovascular risk, improve systemic health markers, and extend life. The problem is that celebrity culture has flattened the conversation into before-and-after photos, erasing the medical nuance that should guide these decisions. Meanwhile, oral formulations of GLP-1 drugs are expanding access, which will only accelerate the tension between medical and cosmetic use.
GLP-1 drugs: myths vs facts
| Myth | Fact |
|---|---|
| GLP-1 drugs only burn fat | Up to 40% of weight lost is lean body mass including muscle |
| You can stop once you reach your goal weight | Most patients regain two-thirds of lost weight within 12-18 months of stopping |
| Side effects are mainly nausea | Serious risks include gastroparesis, bowel obstruction, pancreatitis, and muscle wasting |
| The drugs fix obesity permanently | They suppress appetite; they don't change the metabolic drivers of weight regain |
| Everyone loses the same amount | Response varies widely; some patients lose under 5% while others lose 25%+ |
| Cosmetic use is harmless | Non-obese users face the same side effect risks without the medical benefit that justifies them |
An anti-inflammatory eating approach combined with regular exercise remains the lowest-risk strategy for sustainable weight management. GLP-1 drugs are best understood as a medical intervention for metabolic disease, not a lifestyle choice.
Frequently Asked Questions
What percentage of weight lost on GLP-1 drugs is muscle?
Clinical data shows that 25-40% of total weight lost during GLP-1 therapy is lean body mass, not fat. This includes muscle tissue, which reduces resting metabolic rate and can increase frailty risk, especially in older adults. Resistance training and high-protein diets can slow but not fully prevent this loss.
Do you regain weight after stopping Ozempic or Wegovy?
Yes. The STEP 1 extension trial found that patients regained about two-thirds of their lost weight within one year of stopping semaglutide. A 2025 BMJ meta-analysis confirmed this pattern across multiple GLP-1 drugs, and an Oxford study found the regain rate was faster than after conventional dieting.
Can GLP-1 drugs trigger or worsen eating disorders?
GLP-1 drugs reduce appetite and quiet "food noise," which can help people with binge eating disorder. However, eating disorder specialists warn that the same appetite suppression can reinforce restrictive eating patterns in people with anorexia or a history of disordered eating. Screening for eating disorder history should happen before any GLP-1 prescription.
What is "Ozempic face" and can you prevent it?
Ozempic face refers to facial aging caused by rapid loss of subcutaneous fat in the cheeks, temples, and under-eye area. The skin loses volume faster than it can tighten. Cleveland Clinic notes that slower weight loss rates and maintaining adequate nutrition can reduce the severity, though some degree of facial volume loss is expected with significant weight loss from any cause.
Are GLP-1 drugs safe for people who aren't obese?
GLP-1 receptor agonists are FDA-approved for people with a BMI of 30+ or 27+ with at least one weight-related condition. Using them below these thresholds means accepting the same side effect risks -- muscle loss, GI complications, metabolic changes -- without the clinical benefit that makes those risks worthwhile. No long-term safety data exists for cosmetic use in non-obese populations.
Related Articles
- GLP-1 Weight Loss Drugs Safety Guide - A comprehensive look at what to expect from GLP-1 medications, including dosing, monitoring, and when to talk to your doctor.
- Ozempic Safety and Semaglutide Side Effects - Detailed breakdown of semaglutide's risk profile, from common nausea to rare but serious complications.
- Oral GLP-1 Receptor Agonist Advancements - How pill-form GLP-1 drugs are changing access and what the latest clinical trials show.
- Best Weight Loss Supplements - Evidence-based review of supplements marketed for weight loss, including what works and what doesn't.
- Anti-Inflammatory Eating Patterns - Comparing Mediterranean, DASH, and plant-based diets for sustainable weight management and overall health.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.