What Makes Lung Cancer So Difficult to Catch Early?
Lung cancer kills more people each year than colon, breast, and prostate cancers combined. According to American Cancer Society estimates, roughly 229,410 new cases and 124,990 deaths are projected in the United States alone this year. Globally, the World Health Organization reports that lung cancer is now the most frequently diagnosed cancer worldwide, accounting for about 2.5 million new cases annually.
The core problem is that lungs have very few nerve endings. A tumor can grow for months or even years without causing noticeable pain or discomfort. By the time symptoms appear, the cancer has often already spread beyond the lungs. Data from the National Cancer Institute's SEER program shows that 52% of all lung cancer cases are diagnosed at the distant (metastatic) stage, when five-year survival drops to just 9.7%.
Key takeaway: Lung cancer accounts for roughly 1 in 5 cancer deaths. Because symptoms tend to appear late, understanding the early warning signs and knowing your personal risk factors can genuinely save your life.
The Warning Signs Your Body May Be Sending
Most early lung cancer symptoms overlap with common respiratory conditions, which is exactly why they get dismissed. If any of the following persist for more than two to three weeks without a clear explanation, bring them to your doctor's attention.
A Cough That Won't Quit
A new cough that lingers, or a chronic cough that changes in character (becoming deeper, more frequent, or producing blood-tinged mucus), is one of the most reported early symptoms. This is different from a seasonal cold or allergies. If you notice blood in your sputum, even a small amount, seek medical evaluation promptly. Understanding your breathing patterns and respiratory health can help you notice when something changes.
Unexplained Shortness of Breath
Feeling winded during activities that used to be easy, like climbing a flight of stairs or walking across a parking lot, can signal that a tumor is narrowing an airway or that fluid is building up around the lungs (pleural effusion).
Persistent Chest, Shoulder, or Back Pain
Pain that worsens with deep breathing, coughing, or laughing may indicate that cancer has spread to the chest wall or lymph nodes. Some people describe it as a dull ache rather than sharp pain, which leads them to attribute it to muscle strain or aging.
Unexplained Weight Loss
Losing 10 pounds or more without changes to diet or exercise can be an early sign of several cancers, including lung cancer. Cancer cells divert energy and nutrients from normal body processes, and inflammatory molecules released by tumors can alter metabolism.
Hoarseness or Voice Changes
When a lung tumor presses on the nerve that controls the larynx (the recurrent laryngeal nerve), your voice may become hoarse or raspy. If hoarseness lasts longer than two weeks and is not related to a cold or allergies, it warrants investigation.
Recurring Respiratory Infections
Repeated bouts of bronchitis or pneumonia, especially in the same area of the lung, can suggest that a tumor is partially blocking an airway, creating conditions for infection to develop.
Wheezing
While wheezing is commonly associated with asthma or COPD, new-onset wheezing in someone without a history of these conditions could indicate a tumor obstructing part of an airway.
Bone Pain or Joint Aches
If lung cancer spreads to the bones, it can cause pain in the spine, ribs, hips, or other areas. This pain often worsens at night and may be mistaken for arthritis or the normal aches of aging. Bone metastases occur in roughly 30 to 40% of advanced lung cancer cases.
Fatigue That Rest Doesn't Fix
Cancer-related fatigue is different from normal tiredness. It persists despite adequate sleep and interferes with daily activities. This fatigue results from the body's immune response to the tumor and from the cancer consuming resources your body needs.
Swelling in the Face, Neck, or Arms
A tumor near the top of the lung (called a Pancoast tumor) or one pressing on the superior vena cava can cause swelling, discoloration, or a feeling of fullness in the face and upper body. This is less common but quite specific to lung cancer when it does occur.
| Warning Sign | What It May Feel Like | When to See a Doctor |
|---|---|---|
| Persistent cough | New cough or change in chronic cough; possibly bloody mucus | Lasts more than 2-3 weeks |
| Shortness of breath | Winded during routine activities | New onset or worsening pattern |
| Chest/back/shoulder pain | Dull ache worsening with breathing or coughing | Persistent without clear cause |
| Unexplained weight loss | 10+ pounds lost without trying | Within a few months, no diet change |
| Hoarseness | Raspy or weak voice | Persists beyond 2 weeks |
| Recurring infections | Repeated bronchitis or pneumonia | Two or more episodes in same lung area |
| Wheezing | New whistling sound when breathing | No history of asthma or COPD |
| Bone or joint pain | Deep aching in spine, ribs, or hips | Worsens at night, no injury history |
| Persistent fatigue | Exhaustion unrelieved by sleep | Lasting weeks, interfering with daily life |
| Face/neck swelling | Puffiness or discoloration in upper body | New onset, especially with other symptoms |
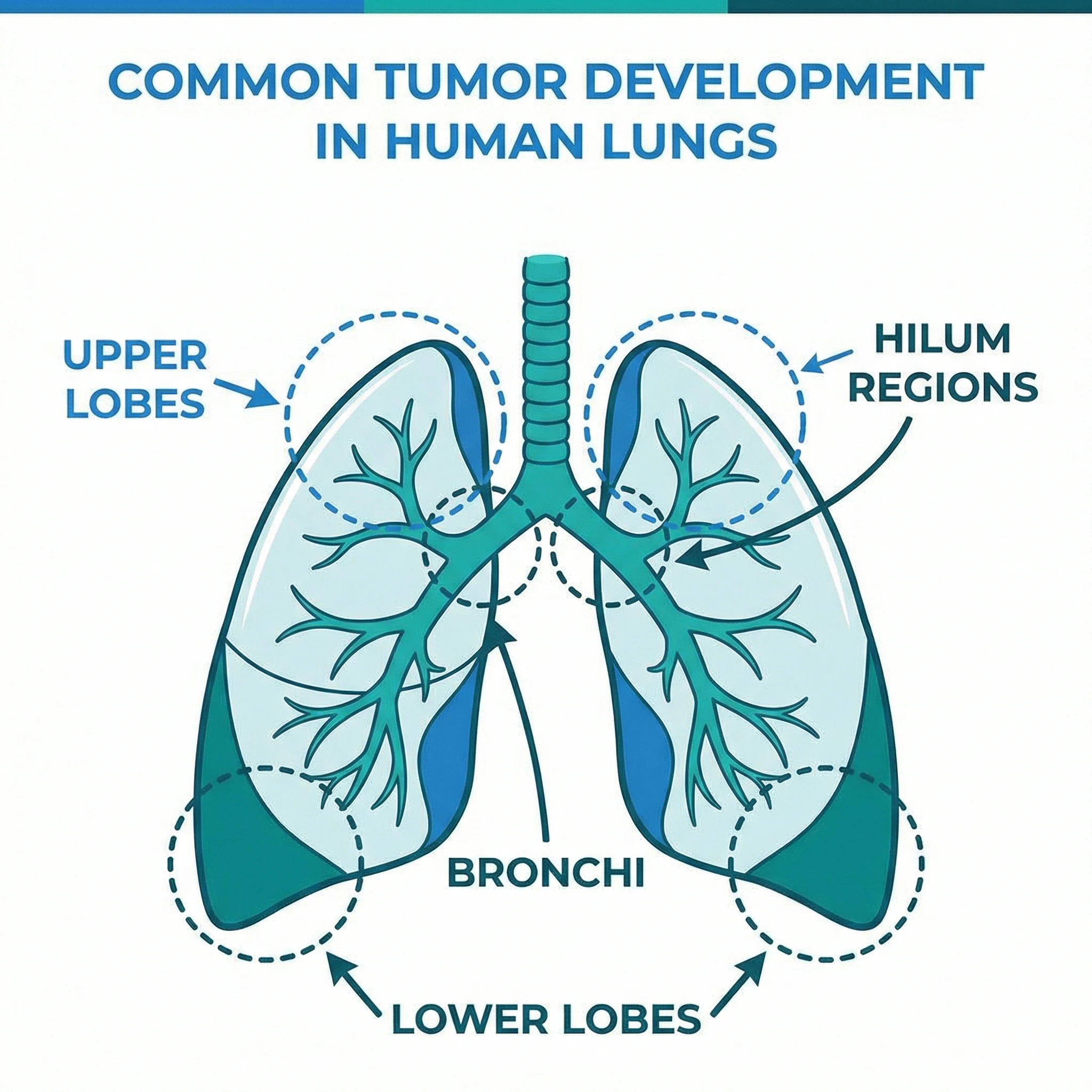
Who Gets Lung Cancer? It's Not Just Smokers
Smoking is responsible for 80 to 90% of lung cancer deaths, and smokers are 15 to 30 times more likely to develop the disease than non-smokers. But the assumption that only smokers get lung cancer is dangerous because it leads non-smokers to ignore symptoms.
Research from the American Cancer Society shows that more than 12% of people newly diagnosed with lung cancer have never smoked a cigarette. Among women, that figure rises to about 16%. Roughly 20% of annual lung cancer deaths occur in people who never smoked, according to the CDC.
| Risk Factor | Key Details | Relative Risk |
|---|---|---|
| Tobacco smoking | Linked to 80-90% of lung cancer deaths | 15-30x increased risk |
| Radon gas exposure | Second leading cause; #1 cause among never-smokers | Accounts for 15,000-22,000 US deaths/year |
| Secondhand smoke | Classified carcinogen | 20-30% increased risk |
| Asbestos exposure | Occupational carcinogen; risk multiplied with smoking | 5x increased risk (50x if smoker) |
| Air pollution | Particulate matter from vehicle exhaust, industry | Elevated risk in high-pollution areas |
| Family history | First-degree relative with lung cancer | Approximately 2x increased risk |
| Prior chest radiation | Radiation therapy for other cancers | Elevated risk in treated area |
Radon, a naturally occurring radioactive gas that seeps through cracks in foundations, is the second leading cause of lung cancer and the number one cause among people who have never smoked. The American Lung Association recommends testing your home, since radon is odorless and invisible. Combined radon and smoking exposure increases risk by 10 to 20 times.
Non-Small Cell vs. Small Cell: The Two Main Types
Understanding which type of lung cancer is present matters because it directly determines treatment options and prognosis. The American Cancer Society classifies lung cancer into two primary categories.
Non-small cell lung cancer (NSCLC) accounts for 80 to 85% of all lung cancer diagnoses. It grows and spreads more slowly than small cell, and it includes three main subtypes:
- Adenocarcinoma — the most common subtype, often found in outer lung areas. This is the type most frequently diagnosed in non-smokers.
- Squamous cell carcinoma — typically develops near the central bronchi and is closely linked to smoking history.
- Large cell carcinoma — can appear in any part of the lung and tends to grow rapidly.
Small cell lung cancer (SCLC) makes up 10 to 15% of cases. It is almost exclusively associated with heavy smoking, grows faster, and tends to spread earlier. While SCLC initially responds well to chemotherapy, it often returns aggressively.
Why Early Detection Changes Everything
The survival gap between early and late-stage lung cancer is among the widest of any cancer type. When caught at the localized stage, before it has spread beyond the lung, the five-year relative survival rate is 64.7%. When diagnosed at the distant stage, that number plummets to 9.7%.
The problem is that only about 23% of lung cancers are caught at this localized stage. The majority are found after the cancer has already metastasized. This pattern has been slowly improving due to screening programs. According to the American Lung Association's State of Lung Cancer report, the percentage of cases caught at an early stage rose from 17% in 2004 to 28% in 2018, and overall lung cancer survival rates improved by 26% over the past five years.
For NSCLC specifically, the five-year survival at the localized stage is 67%, dropping to 12% at the distant stage. SCLC shows even starker numbers: 34% survival when localized but just 4% when distant. Strengthening your immune system through evidence-based strategies is one piece of overall health maintenance, but screening remains the single most impactful action for high-risk individuals.
Screening Guidelines: When a Low-Dose CT Could Save Your Life
The U.S. Preventive Services Task Force (USPSTF) recommends annual low-dose computed tomography (LDCT) screening for adults who meet all three of the following criteria:
- Age 50 to 80 years
- A 20 pack-year smoking history (for example, one pack per day for 20 years, or two packs per day for 10 years)
- Currently smoke or have quit within the past 15 years
This recommendation was expanded in 2021 from the previous criteria of age 55 to 80 with a 30 pack-year history, broadening eligibility to include more people at risk. LDCT screening uses a low radiation dose to create detailed cross-sectional images of the lungs, and it can detect nodules as small as a few millimeters.
Screening reality check: Despite clear evidence that LDCT saves lives, only about 16% of eligible adults in the U.S. are currently being screened, according to the American Lung Association. If you meet the criteria, talk to your doctor about scheduling a scan.
Standard chest X-rays are not recommended for lung cancer screening because they lack the resolution to catch tumors at an early, treatable stage. The National Lung Screening Trial demonstrated that LDCT screening reduced lung cancer mortality by approximately 20% compared to chest X-ray in high-risk populations, which is why it remains the gold standard.
Myth vs. Fact: What Most People Get Wrong About Lung Cancer
| Myth | Fact |
|---|---|
| Only smokers get lung cancer | About 12.5% of newly diagnosed patients have never smoked. Radon, genetics, air pollution, and occupational exposures all contribute. |
| Lung cancer is always a death sentence | When caught early (localized stage), the five-year survival rate is nearly 65%. Newer immunotherapy and targeted treatments continue to improve outcomes. |
| If you quit smoking, the damage is done | Risk drops significantly after quitting. After 10 years, risk falls to about half that of a current smoker. Quitting at any age provides benefit. |
| Lung cancer only affects older people | While risk increases with age, lung cancer can develop at any age. Among women aged 20-49, about 28% of lung cancer patients never smoked. |
| A chest X-ray can detect early lung cancer | Chest X-rays miss small tumors. Low-dose CT is the only screening tool proven to reduce lung cancer mortality. |
| There's no point in screening if you feel fine | Most early lung cancers cause no symptoms. Screening eligible individuals before symptoms appear is the entire point. |
Prevention Strategies That Actually Reduce Your Risk
While no strategy can guarantee you'll never develop lung cancer, the following evidence-based approaches meaningfully reduce your risk.
Quit Smoking (or Never Start)
This is the single most impactful action. The CDC reports that smoking is linked to 80 to 90% of lung cancer deaths. Risk begins declining within years of quitting, and after 10 to 15 years, former smokers approach (but never quite reach) the risk level of never-smokers.
Test Your Home for Radon
Radon testing kits are inexpensive and widely available. If levels exceed 4 picocuries per liter (pCi/L), the EPA recommends mitigation, which typically involves installing a ventilation system beneath the foundation. This is especially important if you live in a region with naturally high radon levels.
Minimize Occupational Exposures
Workers exposed to asbestos, diesel exhaust, certain metals (chromium, nickel, arsenic), and other industrial carcinogens should follow workplace safety protocols, use proper protective equipment, and discuss their exposure history with their doctor.
Eat a Diet Rich in Fruits and Vegetables
Several large studies suggest that diets high in fruits and vegetables may help lower lung cancer risk. Cruciferous vegetables like broccoli and cauliflower contain sulforaphane, a compound studied for its potential anti-cancer properties. Adopting an anti-inflammatory eating pattern can support overall cellular health. Adequate vitamin D levels have also been associated with better outcomes in several cancer types, though research specific to lung cancer prevention is still evolving.
Stay Physically Active
Regular physical activity is associated with a modestly lower risk of lung cancer, even after adjusting for smoking status. The mechanism likely involves improved immune surveillance, reduced systemic inflammation, and better DNA repair processes.
Follow Screening Recommendations
If you meet the USPSTF criteria, annual LDCT screening can catch cancer at its most treatable stage. Discuss your personal risk profile with your healthcare provider. Learning about available cancer-preventing vaccines for other cancer types is also worth discussing with your doctor during these conversations.
Frequently Asked Questions
Can you have lung cancer with no symptoms at all?
Yes. Early-stage lung cancer frequently produces no symptoms. This is why the majority of cases are found at advanced stages when symptoms finally appear, and why screening with low-dose CT is so important for people who meet the eligibility criteria.
Does a persistent cough always mean lung cancer?
No. Most persistent coughs are caused by common conditions like postnasal drip, asthma, acid reflux, or lingering infections. However, a cough that lasts more than two to three weeks, changes in character, or produces blood should be evaluated by a doctor to rule out serious causes including lung cancer.
How effective is low-dose CT screening at saving lives?
The National Lung Screening Trial demonstrated that LDCT screening reduced lung cancer mortality by approximately 20% compared to chest X-ray screening in high-risk individuals. Subsequent studies have confirmed and even expanded on this benefit, making it the only screening tool recommended by the USPSTF for lung cancer.
Is lung cancer hereditary?
Having a first-degree relative (parent, sibling, or child) with lung cancer approximately doubles your risk, suggesting a genetic component. However, most lung cancer cases are driven by environmental exposures rather than inherited genetic mutations. Researchers are working to identify specific genetic markers that increase susceptibility.
What is the difference between a lung nodule and lung cancer?
A lung nodule is a small spot on the lung that appears on imaging. Most lung nodules are benign, caused by old infections, scar tissue, or inflammation. Only a small percentage turn out to be cancerous. If a nodule is found during screening, your doctor will typically monitor its size over time or recommend further testing like a biopsy if it shows concerning features.
Related Articles
- Cancer-Preventing Vaccines: HPV, Hepatitis B, and What You Should Know — Learn about the vaccines that can reduce your risk of cancer-causing viral infections.
- Anti-Inflammatory Eating Patterns: Mediterranean vs. DASH vs. Plant-Based — Compare evidence-based dietary approaches that may help reduce chronic disease risk.
- Natural Ways to Strengthen Your Immune System — Evidence-based strategies for supporting immune function year-round.
- Vitamin D Benefits, Deficiency Warnings, and Precautions — What the research says about vitamin D's role in health and disease prevention.
- Top Breathing Techniques to Relieve Stress — Practical breathing exercises for respiratory wellness and stress management.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.