GLP-1 medications have dominated health headlines since semaglutide first hit the mainstream. But the hormone they mimic is not a pharmaceutical invention. Glucagon-like peptide-1 is a natural gut hormone your intestinal cells produce every time you eat. The drugs work because the underlying biology works. So can you meaningfully increase your body's own GLP-1 production through food, supplements, and daily habits?
The short answer is yes, with caveats. Natural strategies will not replicate the supraphysiological doses of injectable medications. But the research shows that specific dietary choices, targeted supplements, and exercise patterns can measurably raise endogenous GLP-1 levels. For people who are not candidates for medication, who want to support their metabolic health proactively, or who want to maximize results alongside treatment, these strategies have real value.
What GLP-1 Actually Does in Your Body
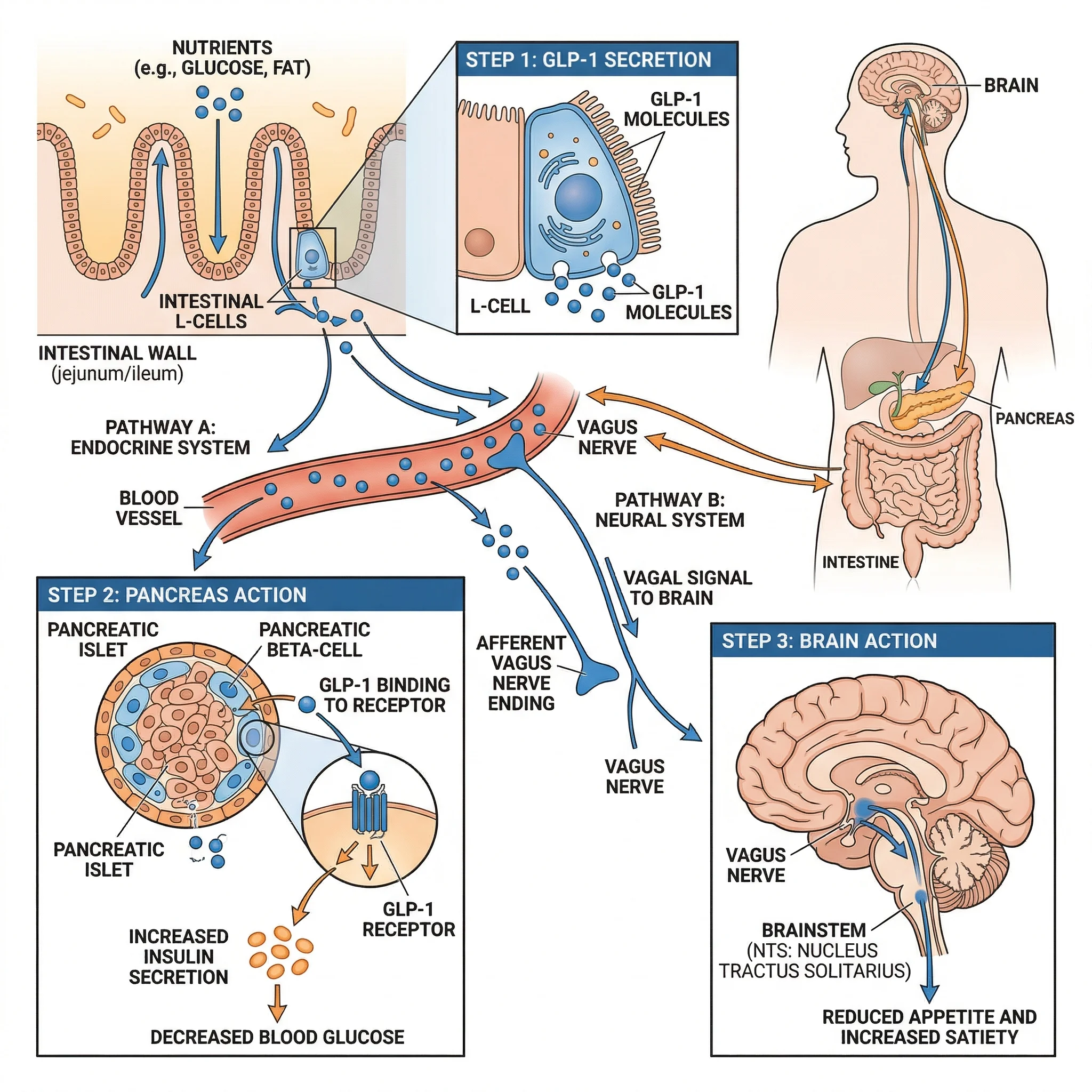
GLP-1 is produced by specialized enteroendocrine cells called L-cells, scattered throughout your small and large intestine. When food arrives in your gut, these cells release GLP-1 into the surrounding tissue and bloodstream within 15 to 30 minutes. The hormone then gets to work on multiple systems simultaneously.
In your pancreas, GLP-1 triggers insulin release in a glucose-dependent manner, meaning it ramps up insulin only when blood sugar is actually elevated. It also suppresses glucagon, the hormone that signals your liver to dump glucose into the blood. In your stomach, GLP-1 slows gastric emptying, which creates a more gradual rise in blood sugar after meals. And in your brain, it acts on appetite-regulating centers in the hypothalamus to reduce hunger and increase feelings of fullness.
GLP-1 has one major vulnerability: an extremely short half-life. The enzyme dipeptidyl peptidase-4 (DPP-4) chops it apart within one to two minutes of release. Only about 10 to 15 percent of newly secreted GLP-1 makes it through the liver to reach systemic circulation in its active form. This rapid degradation is precisely why pharmaceutical GLP-1 receptor agonists are engineered to resist DPP-4 and last hours or days instead of minutes.
Key distinction: Natural GLP-1 works through both bloodstream (endocrine) and nerve (vagal) pathways. Injected GLP-1 medications only use the endocrine route. This means even modest increases in your own GLP-1 production may carry outsized effects through vagal nerve signaling that pharmaceutical versions cannot replicate.
GLP-1 is also responsible for roughly half of your total postprandial insulin secretion. Researchers call this the "incretin effect," the amplified insulin response you get from oral glucose compared to the same amount delivered intravenously. When this incretin effect deteriorates, as it commonly does in type 2 diabetes, blood sugar control suffers. Supporting your natural GLP-1 output is one way to shore up that defense.
Foods That Trigger GLP-1 Release
The nutrients you eat interact directly with receptors on L-cells to trigger GLP-1 secretion. Three categories consistently outperform others in the research: fiber, protein, and healthy fats.
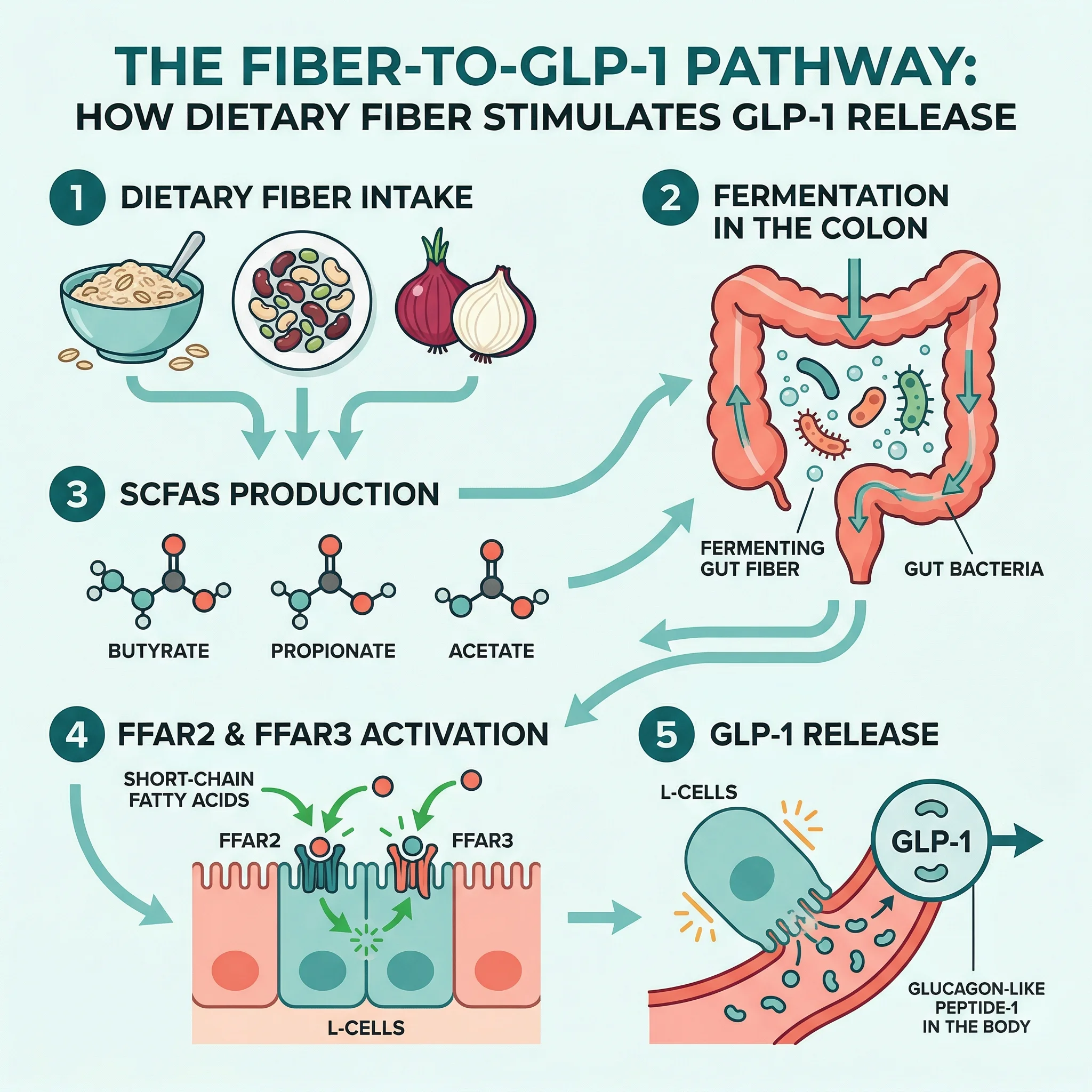
Dietary Fiber and Short-Chain Fatty Acids
Fermentable fiber may be the single most reliable dietary trigger for sustained GLP-1 release. When gut bacteria ferment fiber in your colon, they produce short-chain fatty acids (SCFAs) including butyrate, propionate, and acetate. These SCFAs bind to free fatty acid receptors (FFAR2 and FFAR3) on L-cells, directly triggering GLP-1 secretion. Animal studies have shown that fermentable fiber consumption for as little as 10 days increases GLP-1 concentrations in the colon and portal vein, while also increasing the actual number of L-cells and upregulating proglucagon gene expression.
In a human crossover study, daily supplementation with 16 grams of fermentable fiber (oligofructose) for two weeks increased postprandial satiety and decreased hunger, prospective food consumption, and 24-hour energy intake. The butyrate produced by fiber fermentation serves two purposes here: it nourishes your colon lining and stimulates GLP-1 production.
Propionate stands out among SCFAs for GLP-1 effects. When researchers delivered propionate directly to the colon via an inulin-propionate ester supplement, it acutely stimulated GLP-1 secretion. Over six months of daily use, participants saw reductions in body weight, abdominal fat, and hepatic lipid accumulation.
| Fiber Source | Type | SCFA Profile | GLP-1 Effect |
|---|---|---|---|
| Oats, barley | Beta-glucan (soluble) | High propionate | Strong |
| Jerusalem artichoke, chicory, onion | Inulin/FOS (prebiotic) | High butyrate, acetate | Strong |
| Green bananas, cooled rice/potatoes | Resistant starch | High butyrate | Moderate-strong |
| Beans, lentils, split peas | Mixed soluble/insoluble | Balanced SCFA | Moderate |
| Apples, pears, citrus | Pectin (soluble) | High acetate | Moderate |
Protein
High-protein meals stimulate GLP-1 release through multiple mechanisms. Intact proteins, their digested peptide fragments, and individual amino acids all activate different receptors on L-cells. Whey protein is particularly effective. In human studies, intraduodenal infusion of whey protein hydrolysates increased plasma GLP-1 levels in both lean and obese subjects. But whey has a bonus: it appears to simultaneously inhibit DPP-4 activity in mesenteric blood vessels, protecting the GLP-1 it just helped release from being degraded.
Among individual amino acids, glutamine stands out. Oral doses of 15 to 30 grams of glutamine stimulated GLP-1 secretion in lean individuals and in patients with obesity and type 2 diabetes, with accompanying reductions in blood sugar. Other proteins with demonstrated GLP-1 activity include casein, egg protein, codfish, and corn zein hydrolysate.
Healthy Fats
Long-chain fatty acids activate GLP-1 secretion through GPR40 and GPR120 receptors on L-cells. Chain length matters: fatty acids need at least 12 carbons to trigger the response. Unsaturated fats appear to be more potent than saturated ones. Human studies found that olive oil-rich meals induced higher GLP-1 responses than butter-rich meals of the same calorie content.
Omega-3 fatty acids from fish, walnuts, chia seeds, and flax seeds offer additional metabolic support beyond their GLP-1 effects. The monounsaturated fats in avocados and olive oil are another reliable source.
| Macronutrient | Best Sources for GLP-1 | Mechanism |
|---|---|---|
| Fiber | Oats, legumes, resistant starch, inulin-rich vegetables | SCFA production activates FFAR2/FFAR3 on L-cells |
| Protein | Whey, eggs, fish, casein, legumes | Peptides and amino acids activate CaSR and PepT1 on L-cells; whey also inhibits DPP-4 |
| Fat | Olive oil, avocado, salmon, nuts, seeds | Long-chain unsaturated fatty acids activate GPR40/GPR120 |
How You Eat Matters as Much as What You Eat
Your eating patterns and behaviors influence GLP-1 independently of food choices. According to dietitians at Ohio State Wexner Medical Center, eating protein and fat before carbohydrates in a meal enhances GLP-1 secretion and improves post-meal blood sugar responses compared to eating carbohydrates first. Eating slowly with thorough chewing also produces a more pronounced GLP-1 response and greater satiety.
GLP-1 follows a circadian rhythm, with higher levels during daytime hours. Eating within a consistent window, ideally about 12 hours, and front-loading nutrition earlier in the day aligns with this natural pattern. Leaving at least two hours between your last meal and bedtime gives your gut hormones a chance to complete their signaling cycle before sleep.
Supplements That Support GLP-1 Production
Several supplements have evidence supporting their ability to increase GLP-1 levels, though the strength of that evidence varies considerably.
Berberine
Berberine has been called "nature's Ozempic" in supplement marketing, which oversells its potency but is not completely off-base regarding its mechanism. This alkaloid compound, found in goldenseal, barberry, and Oregon grape, does genuinely interact with GLP-1 pathways. A 2015 study published in Biochemical Pharmacology demonstrated that berberine stimulates GLP-1 secretion by activating bitter taste receptors (TAS2R38) expressed on intestinal enteroendocrine cells. When researchers blocked these receptors or silenced the gene, berberine's GLP-1-stimulating effect disappeared.
A second study found that berberine also works indirectly. In diet-induced obese mice, berberine (100 mg/kg/day for 8 weeks) restored GLP-1 expression by protecting mitochondrial function in colon cells. The high-fat diet had caused mitochondrial stress, membrane rupture, and cristae loss in the colon cells that produce GLP-1. Berberine reversed this damage while also improving gut microbiota composition and increasing SCFA production. So berberine hits GLP-1 from two angles: it activates the taste receptors directly and repairs the cellular machinery that produces GLP-1.
A meta-analysis found that berberine reduces fasting blood sugar and HbA1c, which aligns with its GLP-1 activity. However, most berberine studies have been conducted in Chinese populations, and its effects on diverse populations need more investigation. If you take berberine for cardiovascular benefits, its GLP-1 support is an additional upside.
Flavonoids: Quercetin, EGCG, and Curcumin
Plant flavonoids are emerging as potent GLP-1 stimulators, and they work at surprisingly low concentrations. In cell and animal studies, curcumin stimulated GLP-1 secretion from enteroendocrine cells at concentrations of 10 to 50 micromoles, and a single oral dose in rats elevated plasma GLP-1 and improved glucose tolerance. EGCG (from green tea) stimulated GLP-1 release from both cultured intestinal cells and mouse intestinal tissue. Quercetin, found abundantly in onions, apples, and capers, has also shown GLP-1-stimulating activity in cell models.
Some flavonoids also inhibit DPP-4, the enzyme that breaks down GLP-1. Isoquercitrin and myricetin both showed DPP-4 inhibitory activity in addition to stimulating GLP-1 secretion directly.
The practical limitation: achieving effective concentrations through food alone is difficult. One study found that consuming applesauce with about 100 mg of quercetin from onion powder produced a maximum plasma quercetin concentration of just 0.9 micromoles. That suggests supplemental doses are needed for meaningful GLP-1 effects, though regular consumption of flavonoid-rich foods may produce cumulative benefits over time, especially when combined with fermentable fiber that enhances flavonoid bioavailability.
| Supplement | GLP-1 Mechanism | Evidence Strength | Typical Dose |
|---|---|---|---|
| Berberine | Activates bitter taste receptors (TAS2R38); protects L-cell mitochondria; improves gut microbiota | Moderate (human and animal) | 500 mg 2-3x daily |
| Curcumin | Stimulates GLP-1 via GPR40/GPR120 receptors | Moderate (mainly animal) | 500-1000 mg daily (with piperine) |
| EGCG (green tea extract) | Directly stimulates L-cell GLP-1 secretion | Moderate (cell and animal) | 400-500 mg daily |
| Quercetin | Stimulates GLP-1; also inhibits DPP-4 | Moderate (cell and animal) | 500-1000 mg daily |
| Prebiotic fiber (inulin/FOS) | Increases SCFA production that activates FFAR2/FFAR3 on L-cells | Strong (human trials) | 10-16 g daily |
| Probiotics | Modulates gut microbiome composition; supports GLP-1 signaling | Emerging | Strain-specific |
D-Allulose
This rare sugar deserves mention for a unique property. D-allulose, a non-metabolizable sweetener, stimulates GLP-1 secretion without triggering GIP, the other incretin hormone that promotes fat storage. In mouse models, oral D-allulose restricted overeating and hyperglycemia by increasing GLP-1. The selective GLP-1 stimulation without GIP activation is an attractive characteristic that no other natural compound appears to share.
Lifestyle Strategies for Higher GLP-1
Exercise Intensity and GLP-1
Exercise reliably increases GLP-1 levels, but intensity matters. A review in the World Journal of Diabetes found that moderate-intensity (50-75% of maximal oxygen uptake) and high-intensity (85-90% of max heart rate) acute exercise both increase GLP-1 compared to resting controls in healthy and obese individuals. A 12-week supervised exercise program also increased postprandial GLP-1 levels in overweight and obese participants. In adolescents with type 2 diabetes, high-intensity interval training elevated GLP-1 more effectively than low-intensity exercise matched for energy expenditure.
The GLP-1 benefit goes beyond calorie expenditure. Exercise increases gut microbiota diversity and boosts SCFA production. Those microbially produced SCFAs then interact with the same FFAR2 and FFAR3 receptors on L-cells that dietary fiber activates. Combine regular exercise with a high-fiber diet and you create a reinforcing loop: exercise feeds the bacteria, bacteria produce more SCFAs, SCFAs trigger more GLP-1.
Researchers have identified a state called "GLP-1 resistance," where excess visceral fat and gut microbiota imbalances reduce the body's responsiveness to GLP-1 signaling. Exercise may improve GLP-1 resistance through reducing visceral fat and improving microbiome diversity, meaning it helps the GLP-1 you already produce work better.
Aim for at least 150 minutes of moderate-intensity exercise per week. Combining aerobic and resistance training appears to offer the broadest metabolic benefit.
Sleep Quality
Poor sleep disrupts GLP-1 timing. Sleep deprivation delays the peak GLP-1 response after eating, which interferes with appetite regulation and blood sugar management. GLP-1 follows a circadian pattern, with higher production during daytime. Chronic sleep disruption throws off this pattern and can increase hunger hormones while blunting satiety signals.
Adults should target seven to nine hours per night. Going to bed at a consistent time, avoiding large meals close to bedtime, and keeping screens out of the bedroom for the last 30 minutes before sleep are straightforward interventions that support hormonal rhythms.
Stress Management
Chronic stress raises cortisol, which impairs GLP-1 release and shifts eating behavior toward calorie-dense comfort foods. The gut-brain axis connection is relevant here: stress affects gut microbiota composition, which in turn affects SCFA production and GLP-1 secretion. Practices like spending time outdoors, journaling, and mind-body exercises (yoga, tai chi, breathwork) can reduce cortisol and indirectly support GLP-1 function.

The GLP-1 Supplement Market: Myths vs. Evidence
The popularity of GLP-1 medications has spawned a booming market of supplements claiming to be "natural Ozempic." Products with names like "GLP-1 Daily" and "GLP-1 Assist" crowd online retailers. Some grounding is needed.
First, none of these products contain actual GLP-1. They contain ingredients that may, to varying degrees, support GLP-1 production. The distinction matters because supplements are not required to prove their marketing claims through clinical trials the way medications are. The FDA has issued hundreds of warnings about tainted weight loss products, and experts caution that combining unregulated supplements with prescription GLP-1 medications could lead to dangerous blood sugar drops.
Second, the dose gap is enormous. GLP-1 medications produce placebo-adjusted weight reduction of 5 to 18 percent in clinical trials. As Dr. Yvette-Marie Pellegrino, a board-certified obesity medicine specialist, has noted, "natural GLP-1 only improves weight and diabetes management by a small amount." The natural hormone operates at physiological concentrations while the drugs deliver supraphysiological doses with extended half-lives.
That said, some supplement ingredients do have genuine research behind them. Berberine's effects on fasting blood sugar and HbA1c are supported by meta-analyses. Prebiotic fiber supplements that boost SCFA production have strong evidence for increasing GLP-1. The problem is not that these ingredients are useless but that marketing routinely overstates what they can do.
A reasonable approach: treat supplements as one part of a broader strategy that includes fiber-rich whole foods, adequate protein, regular exercise, and good sleep. Do not expect them to replicate medication-level results. And always inform your healthcare provider before adding supplements, especially if you take blood sugar-lowering medications.
Putting It All Together
No single food or supplement will transform your GLP-1 levels. The approach that works is layering habits that each contribute a measurable push in the same direction.
Start with fiber. Adding 10 to 16 grams of prebiotic fiber daily from oats, legumes, or supplemental inulin creates the fermentation environment that drives SCFA-mediated GLP-1 release. Pair meals with adequate protein (whey, eggs, fish, or legumes) and include unsaturated fats from olive oil, avocados, or nuts.
Eat protein and vegetables before carbohydrates at meals. Take smaller bites and eat slowly. Keep meals within a consistent 12-hour window. These behavioral adjustments require no supplements or purchases, only awareness.
Add exercise. Moderate to vigorous physical activity three to five times per week improves both GLP-1 secretion and GLP-1 sensitivity. The combination of aerobic training and resistance training offers the broadest metabolic benefit.
Protect sleep and manage stress. Both affect cortisol, gut microbiome composition, and the circadian rhythm of GLP-1 production.
Consider supplements judiciously. Berberine, curcumin, and quercetin have mechanistic evidence for GLP-1 support, but set expectations appropriately. Prebiotic fiber supplements have the strongest human evidence for boosting GLP-1 via SCFA production.
If you are already taking or considering GLP-1 medications, these same strategies may enhance treatment outcomes. A joint advisory from four major US medical societies emphasized that evidence-based nutritional and lifestyle interventions are critical complements to GLP-1 medication, not optional extras. The combination of medication plus structured lifestyle change consistently outperforms either approach alone.

Frequently Asked Questions
Can natural GLP-1 boosters replace Ozempic or similar medications?
No. Natural strategies produce modest, physiological increases in GLP-1, while medications deliver supraphysiological doses with extended duration. GLP-1 drugs produce 5 to 18 percent weight reduction in trials. Natural approaches cannot match that magnitude. They work best as a complement to medication or as a standalone strategy for people who want metabolic support without prescription drugs.
How quickly can dietary changes affect GLP-1 levels?
GLP-1 release is an acute response to each meal, so specific food choices affect GLP-1 within that same meal. Eating fiber and protein triggers GLP-1 release within 15 to 30 minutes. However, structural changes like increased L-cell numbers from chronic fiber intake take weeks. Animal studies showed increased L-cell density and proglucagon gene expression after 10 days to several weeks of fermentable fiber consumption.
Is berberine safe to take with diabetes medications?
Berberine lowers blood sugar through multiple pathways including GLP-1 stimulation. Taking it alongside insulin or other glucose-lowering medications increases the risk of hypoglycemia. Always consult your healthcare provider before combining berberine with diabetes medications. Monitoring blood sugar more frequently during the initial period is advisable.
Does intermittent fasting increase GLP-1?
The relationship is indirect. Intermittent fasting improves insulin sensitivity and can shift gut microbiome composition favorably, which may support GLP-1 signaling. Time-restricted eating that aligns with circadian rhythms (eating during daylight hours) may also optimize the natural circadian pattern of GLP-1 production. However, fasting itself does not directly stimulate GLP-1 release, since the hormone is specifically triggered by food intake.
Which single change has the biggest impact on GLP-1?
If you had to pick one change, increasing dietary fiber intake has the broadest evidence base. Fermentable fiber feeds beneficial gut bacteria, produces SCFAs that directly stimulate L-cells, increases L-cell numbers over time, and has been shown in human studies to improve satiety and reduce food intake. Start with 10 to 16 grams of prebiotic fiber daily from foods like oats, beans, and onions.
Related Articles
- Berberine for Heart Health: A Natural Cholesterol Fighter — A deeper look at berberine's cardiovascular benefits and its metabolic mechanisms.
- Butyrate: The Gut Metabolite That Heals Your Colon and Protects Your Brain — How the short-chain fatty acid produced by fiber fermentation supports gut and brain health.
- The Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition — The bidirectional communication between your gut and brain that influences GLP-1 signaling.
- Autophagy, Fasting, Exercise, and Diet — How fasting and exercise trigger cellular renewal processes that overlap with metabolic health.
- Inflammation, Chronic Disease, and Anti-Inflammatory Living — The role of chronic inflammation in metabolic dysfunction and strategies to reduce it.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.