More Than Half of All Deaths Worldwide Trace Back to One Process
The number sounds almost too large to believe. According to a major review published in Nature Medicine, more than 50 percent of all deaths globally are now attributable to diseases rooted in chronic inflammation. Heart disease, stroke, cancer, diabetes, kidney disease, liver disease, and neurodegenerative conditions all trace back to the same biological problem: persistent, low-grade inflammatory activity that accumulates damage over months and years without producing symptoms you can point to.
What makes this statistic even more striking is a finding from a study of 210 healthy twins aged 8 to 82. Researchers discovered that non-heritable factors — diet, exercise habits, sleep quality, stress exposure, and environmental conditions — were the strongest contributors to differences in chronic inflammation between individuals. Put differently, your genes set the baseline, but your daily habits have more influence over your inflammatory status than your DNA does.
Below, we break down what chronic inflammation actually is, how it differs from the redness and swelling you see after a cut, which conditions it feeds, and the dietary and lifestyle changes that clinical evidence supports for bringing it down.
Why Your Body's Defense System Sometimes Turns Against You
Inflammation itself is not the villain. When you twist an ankle or catch a respiratory infection, your immune system launches an acute inflammatory response: blood vessels dilate, white blood cells rush in, and the area swells with protective fluid. The process starts fast, hits hard, and usually resolves within days as healing kicks in. This is inflammation doing exactly what evolution designed it to do.
Chronic inflammation works differently. According to the National Library of Medicine's StatPearls reference, it is a slow, low-grade response that can persist for months to years. Think of it less as a fire and more as a slow leak. It damages tissues and organs gradually, often without producing obvious symptoms until a disease has already taken hold.
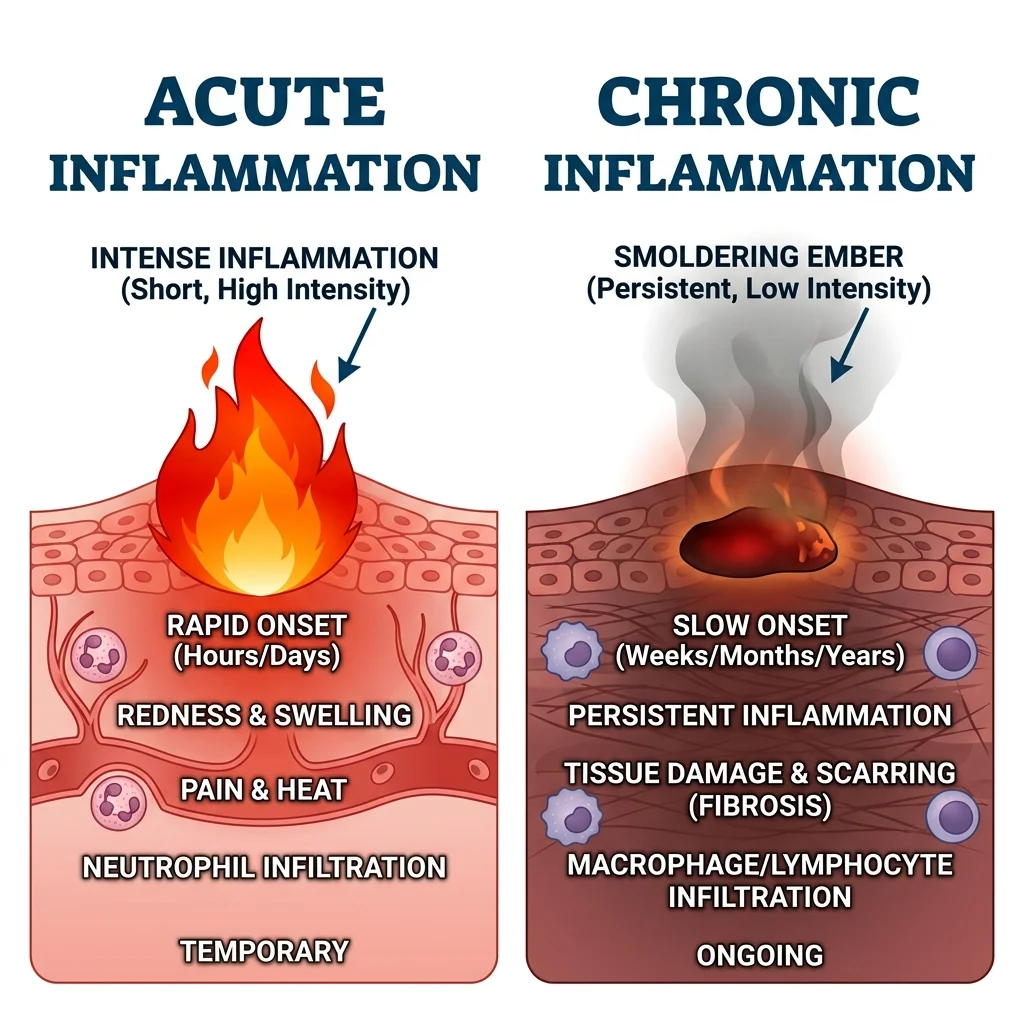
The triggers differ, too. Acute inflammation responds to pathogens and injuries (called PAMPs and DAMPs in immunology). Chronic inflammation, however, is often driven by persistent metabolic dysfunction, visceral fat accumulation, gut microbiome imbalances, ongoing psychological stress, environmental toxicant exposure, and poor dietary patterns, all without any infection present.
| Feature | Acute Inflammation | Chronic Inflammation |
|---|---|---|
| Duration | Hours to days | Months to years |
| Intensity | High-grade, localized | Low-grade, systemic |
| Trigger | Infection, injury | Metabolic dysfunction, lifestyle factors |
| Outcome | Healing and resolution | Ongoing tissue damage |
| Symptoms | Visible (redness, swelling, pain) | Often invisible until disease develops |
| Primary cells | Neutrophils | Macrophages, lymphocytes |
The Web of Diseases Connected by a Single Thread
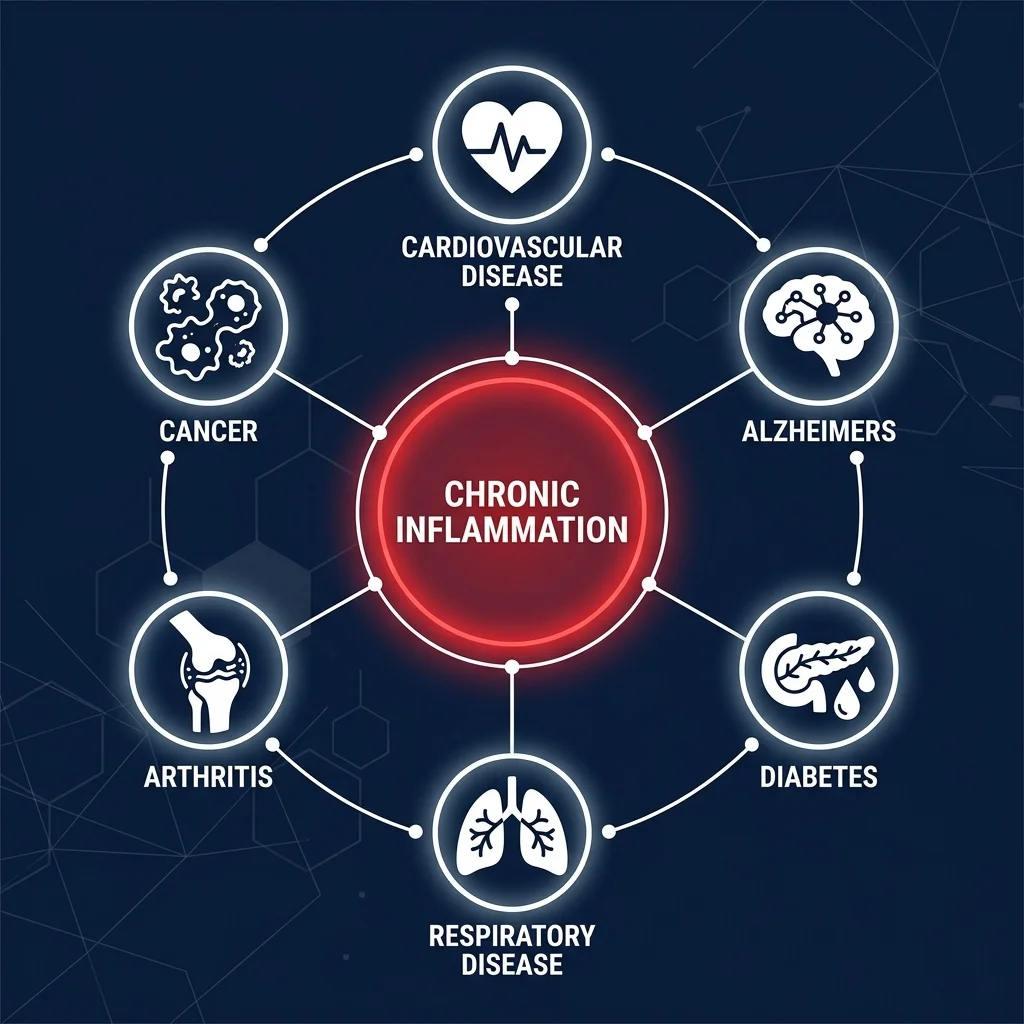
Chronic inflammation touches nearly every medical specialty. A 2024 editorial in Cells listed the conditions it feeds: cardiovascular disease, type 2 diabetes, cancer, autoimmune conditions, gastrointestinal disorders, respiratory diseases, neurodegenerative diseases, hormonal imbalances, and sleep disorders. That is a remarkably long list for a single biological process.
Consider the numbers behind individual conditions. The WHO ranks chronic diseases as the greatest threat to human health. Cardiovascular disease alone accounts for roughly 31 percent of all deaths globally, with atherosclerosis (the plaque buildup in arteries) now understood as a fundamentally inflammatory process. Data from a meta-analysis of more than 160,000 people across 54 prospective studies confirmed that higher levels of the inflammatory marker C-reactive protein (CRP) are directly associated with increased risk of coronary heart disease and cardiovascular death.
Key Takeaway: Three of every five people worldwide die from chronic inflammatory diseases, including stroke, heart disorders, cancer, respiratory diseases, obesity, and diabetes — according to WHO data cited in StatPearls.
The strongest evidence that inflammation causes cardiovascular events, not just accompanies them, came from the CANTOS trial. This double-blind randomized controlled trial gave over 10,000 adults with a history of heart attack and elevated CRP an antibody that blocks the inflammatory molecule IL-1 beta. Patients who received the drug had lower rates of repeat heart attacks, strokes, and cardiovascular deaths compared to placebo, despite zero change in their LDL cholesterol. That result separated inflammation from cholesterol as an independent driver of heart disease.
The connection extends beyond the heart. In the pancreas, macrophages infiltrate tissue and release pro-inflammatory molecules, which contributes to insulin resistance and type 2 diabetes. In the brain, chronic low-grade inflammation is linked to cognitive decline, dementia, and depression. A growing body of research shows that disruption of the gut-brain axis through intestinal dysbiosis can trigger endotoxemia and neuroinflammation, linking gut health directly to mood and cognitive function.
| Disease | How Inflammation Contributes | Key Inflammatory Marker |
|---|---|---|
| Cardiovascular disease | Drives atherosclerotic plaque formation | hs-CRP, IL-6 |
| Type 2 diabetes | Macrophage infiltration impairs insulin signaling | TNF-alpha, IL-1beta |
| Alzheimer's disease | Neuroinflammation damages neurons | IL-6, CRP |
| Cancer | Promotes cell proliferation and tumor microenvironment | NF-kB, TNF-alpha |
| Rheumatoid arthritis | Autoimmune attack on joint tissue | CRP, IL-17 |
| Inflammatory bowel disease | Chronic mucosal immune activation | CRP, calprotectin |
How Doctors Measure Inflammation You Cannot Feel
Chronic inflammation rarely announces itself with obvious symptoms. Fatigue, joint stiffness, brain fog, digestive irregularities, and unexplained weight changes can all signal its presence, but these symptoms overlap with dozens of other conditions. Laboratory testing provides a more objective window.
The most widely used marker is high-sensitivity C-reactive protein (hs-CRP). The CDC and American Heart Association have endorsed hs-CRP as the most reliable clinical assay for evaluating cardiovascular risk related to inflammation. Normal levels fall below 0.55 mg/L in men and below 1.0 mg/L in women. Values above 3.0 mg/L indicate elevated cardiovascular risk, and levels above 10 mg/L typically suggest an acute inflammatory process requiring investigation.
Beyond CRP, clinicians may measure fibrinogen (normal range 200-300 mg/dL), erythrocyte sedimentation rate (ESR), and specific pro-inflammatory cytokines including TNF-alpha, IL-1 beta, and IL-6 , though cytokine panels are more expensive and less standardized. A major study in Glasgow found that combining CRP, albumin, and neutrophil count predicted all-cause mortality over eight years, including cancer and cardiovascular deaths.
| Marker | What It Measures | Normal Range | Limitations |
|---|---|---|---|
| hs-CRP | General systemic inflammation | <1.0 mg/L (women), <0.55 mg/L (men) | Also elevated in acute illness/injury |
| Fibrinogen | Clotting protein linked to inflammation | 200-300 mg/dL | Less specific than CRP |
| IL-6 | Pro-inflammatory cytokine | Varies by lab | Expensive, not standardized |
| TNF-alpha | Key inflammatory signaling molecule | Varies by lab | Expensive, not standardized |
| ESR | Rate of red blood cell settling | 0-20 mm/hr (varies by age) | Non-specific; slow to change |
What 18 Clinical Trials Say About Eating to Reduce Inflammation
Changing what you eat is one of the most studied and most accessible ways to lower chronic inflammation. A 2025 systematic review and meta-analysis pooled data from 18 randomized controlled trials (2,602 participants total) and found that anti-inflammatory dietary patterns produced statistically significant reductions in systolic blood pressure (approximately 4 mmHg), diastolic blood pressure (approximately 1.8 mmHg), LDL cholesterol, total cholesterol, and hs-CRP when compared to standard omnivorous diets.
The dietary patterns that qualified as anti-inflammatory included the Mediterranean diet, DASH diet, Nordic diet, vegetarian approaches, and even ketogenic protocols . All of them share an emphasis on whole, minimally processed foods.
There is no single "anti-inflammatory diet." What matters are the shared principles across these eating patterns. The Cleveland Clinic describes anti-inflammatory eating not as a specific regimen but as an overall style centered on whole foods and minimally processed ingredients.

Foods that reduce inflammation — and why they work:
- Fatty fish (salmon, mackerel, sardines): Rich in omega-3 fatty acids EPA and DHA, which serve as precursors to specialized pro-resolving mediators — resolvins, maresins, and protectins that actively shut down inflammatory cascades
- Extra-virgin olive oil: Contains oleocanthal, which suppresses the NF-kB signaling pathway, reducing production of TNF-alpha and IL-6
- Berries and colorful vegetables: Packed with polyphenol compounds that neutralize free radicals and modulate inflammatory gene expression
- Leafy greens (kale, spinach, Swiss chard): High in folate, fiber, and antioxidant vitamins that support methylation and reduce oxidative stress
- Whole grains and legumes: Dietary fiber feeds beneficial gut bacteria, which produce anti-inflammatory short-chain fatty acids like butyrate
- Nuts (especially walnuts): Contain alpha-linolenic acid (plant-based omega-3) and vitamin E
- Turmeric and ginger: Curcumin from turmeric has been shown to improve outcomes in inflammatory conditions in animal models
- Fermented foods (yogurt, kefir, kimchi): Supply beneficial bacteria that support intestinal barrier integrity
Foods that promote inflammation:
- Ultra-processed foods: A cohort study of 44,551 French adults found that a 10 percent increase in ultra-processed food consumption was associated with a 14 percent greater risk of all-cause mortality
- Refined carbohydrates and added sugars: Create oxidative stress that activates inflammatory genes
- Trans fats and processed seed oils: Aggravate inflammatory pathways
- Processed meats (bacon, sausage, deli meats): Contain advanced glycation end products that stimulate immune reactions
- Excessive alcohol: Disrupts gut barrier integrity and promotes endotoxemia
Magnesium deserves special attention. StatPearls identifies it as "one of the most anti-inflammatory dietary factors," with research linking adequate magnesium intake to lower levels of hs-CRP, IL-6, and TNF-alpha. Yet most adults fall short of recommended intake because processed foods are stripped of this mineral during manufacturing.
What Else Matters When Diet Alone Is Not Enough
Food matters, but it is not the whole story. Several lifestyle factors lower inflammation independently of what you eat.
Physical activity. Exercise lowers pro-inflammatory molecules and cytokines independently of weight loss. A meta-analysis including data from over 1.6 million participants found that achieving the recommended 150 minutes per week of moderate-intensity aerobic activity was associated with a 23 percent lower risk of cardiovascular mortality, a 17 percent lower incidence of cardiovascular disease, and a 26 percent reduction in type 2 diabetes incidence. Separate data showed that meeting minimum physical activity guidelines corresponded to a 40 percent lower risk of Alzheimer's disease. Even modest daily walking makes a difference: an umbrella review in BMJ Open found that each additional 1,000 daily steps was linked to a 17 percent reduction in systemic inflammation as measured by CRP.
Sleep quality and circadian alignment. Both physical and emotional stress trigger inflammatory cytokine release, but disrupted sleep and circadian rhythm problems compound the damage independently. Exposure to artificial blue light after sundown disrupts circadian biology and promotes inflammation. Night-shift work has been associated with increased risk for metabolic syndrome and is suspected of contributing to several cancers, including breast, prostate, and colorectal. Seven to eight hours of consistent, quality sleep each night helps regulate hormonal repair processes and keeps inflammatory signaling in check.
Stress management. Chronic psychological stress disrupts the ability of cortisol to effectively down-regulate inflammatory activity , a phenomenon called glucocorticoid resistance. Over time, this creates a biochemical environment where the body's natural anti-inflammatory braking system no longer works efficiently. Practices that activate the parasympathetic nervous system — including deep breathing exercises, meditation, and activities that support gut health — can help restore this balance.
Body composition. Visceral adipose tissue is not passive storage. It is an active endocrine organ that secretes pro-inflammatory cytokines including IL-1 beta, IL-6, and TNF-alpha. As fat cells enlarge, areas of hypoxia develop, triggering immune cell infiltration and a self-perpetuating cycle of inflammation. This is why weight management, particularly reducing visceral fat, is considered the single most effective intervention for reducing chronic inflammation.
Environmental exposures. The US Federal Tox21 Program has tested more than 9,000 chemicals and found that numerous compounds commonly encountered in daily life significantly alter inflammatory signaling pathways. These include phthalates, bisphenols, polycyclic aromatic hydrocarbons, and flame retardants , found in plastics, personal care products, and household goods. Tobacco smoking remains a potent inflammatory trigger, both lowering anti-inflammatory molecule production and directly inducing inflammatory pathways.
What People Get Wrong About Inflammation
| Myth | Fact |
|---|---|
| All inflammation is bad | Acute inflammation is essential for healing. Only chronic, unresolved inflammation causes disease. |
| You can cure chronic inflammation with a single supplement | No single supplement eliminates chronic inflammation. Sustained dietary and lifestyle patterns produce measurable reductions in inflammatory markers, as shown in meta-analyses of randomized trials. |
| Inflammation is caused by genetics | A twin study published in Cell found that non-heritable factors (lifestyle, diet, environment) are the strongest drivers of inflammatory differences between people. |
| Only overweight people have chronic inflammation | While visceral obesity is a major driver, lean individuals can experience chronic inflammation from stress, poor sleep, smoking, or environmental exposures. |
| Anti-inflammatory diets require extreme restriction | Evidence-based anti-inflammatory eating (Mediterranean, DASH, Nordic patterns) emphasizes adding whole foods rather than eliminating food groups. |
| CRP testing tells you everything about inflammation | hs-CRP is the most validated single marker, but it also rises during acute illness. Clinicians often use multiple markers for a complete picture. |
Frequently Asked Questions
Can you actually reverse chronic inflammation?
Yes, to a meaningful degree. Chronic inflammation is driven primarily by modifiable factors. Clinical trials show that anti-inflammatory dietary patterns reduce hs-CRP and other markers within weeks to months. Regular physical activity independently lowers pro-inflammatory cytokines regardless of weight loss. The key is sustained behavioral change rather than short-term interventions. Researchers recommend giving dietary changes three to six months to produce measurable results.
What is the fastest way to know if you have chronic inflammation?
Ask your doctor for an hs-CRP blood test. It is inexpensive, widely available, and endorsed by the CDC and American Heart Association as the most reliable clinical marker for inflammation-related cardiovascular risk. Normal values are below 1.0 mg/L for women and below 0.55 mg/L for men. Values consistently above 3.0 mg/L warrant further investigation.
Is the Mediterranean diet really the best anti-inflammatory diet?
It has the strongest and most extensive evidence base, but a 2025 meta-analysis found that several patterns — including the DASH diet, Nordic diet, and plant-forward approaches — all produced significant reductions in blood pressure, cholesterol, and inflammatory markers compared to standard Western diets. The underlying principle matters more than the label: prioritize whole foods, healthy fats, fiber, and omega-3s while minimizing ultra-processed foods, refined sugars, and trans fats.
Does exercise reduce inflammation even without weight loss?
Yes. Human clinical trials demonstrate that physical activity lowers multiple pro-inflammatory molecules and cytokines independently of changes in body weight. Skeletal muscle functions as an endocrine organ that produces anti-inflammatory myokines during contraction. Even moderate walking (just 150 minutes per week) is associated with a 23 percent reduction in cardiovascular mortality risk.
How long does it take for an anti-inflammatory diet to show results?
Registered dietitians note that some people notice improvements in symptoms like joint pain, energy, and digestive comfort within two to three weeks of eliminating inflammatory trigger foods. However, measurable changes in blood markers like CRP and lipid profiles typically require three to six months of consistent dietary change.
Related Articles
- Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition — Explores how gut dysbiosis and intestinal permeability drive neuroinflammation and mental health changes.
- Polyphenol-Rich Foods for Heart Health — A deep dive into the plant compounds that modulate inflammatory gene expression and protect cardiovascular tissue.
- Best Magnesium for Heart Health — Covers the evidence behind magnesium as one of the most potent anti-inflammatory minerals and how to choose the right form.
- Sleep Timing and Heart Health — Examines how circadian rhythm disruption fuels inflammation and increases cardiovascular risk.
- Bone Broth Benefits for Gut Healing, Joints, and Skin — Looks at how supporting intestinal barrier integrity can reduce systemic inflammatory load.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.












