Something like 30 million American adults have tried acupuncture, and annual usage has more than doubled since 2002. The American College of Physicians now recommends it for back pain. The UK's NICE guidelines include it for chronic pain. The WHO lists 28 conditions with proven efficacy. That kind of institutional backing would have been unthinkable 20 years ago. But the clinical picture is more complicated than the headlines suggest, and "it works" and "it doesn't work" are both oversimplifications. Here's what 39 randomized trials, 845,637 tracked patients, and several decades of mechanistic research actually tell us.
What Is Acupuncture and How Does It Work?
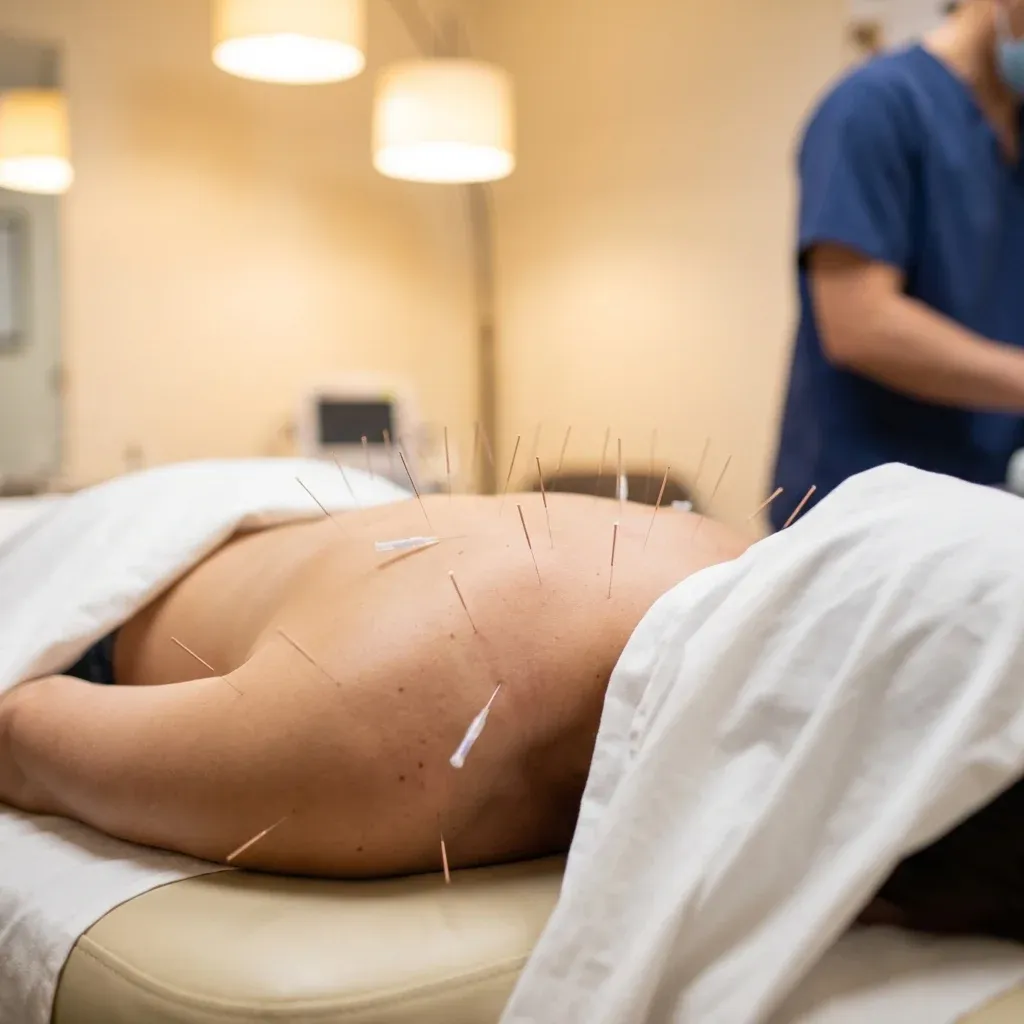
Acupuncture involves inserting thin, sterile needles at specific points on the body. It originated in China roughly 3,000 years ago and was traditionally explained through the concept of qi (pronounced "chee"), a life force said to flow through pathways called meridians. When qi becomes blocked or unbalanced, illness follows. Needle stimulation at key points was believed to restore that flow.
That traditional framework still guides point selection in most clinics. But the modern scientific picture looks quite different. Researchers have pinpointed several biological mechanisms, and in 2021 a Harvard team published in Nature what may be the most important acupuncture paper in a decade: they mapped the exact neural pathway through which electroacupuncture at the hindlimb drives a vagal-adrenal anti-inflammatory response. The anatomical precision mattered: stimulating abdominal points did not produce the same effect. This was the first study to identify the exact sensory neuron population (PROKR2-expressing neurons in deep fascia) responsible for the anti-inflammatory action.
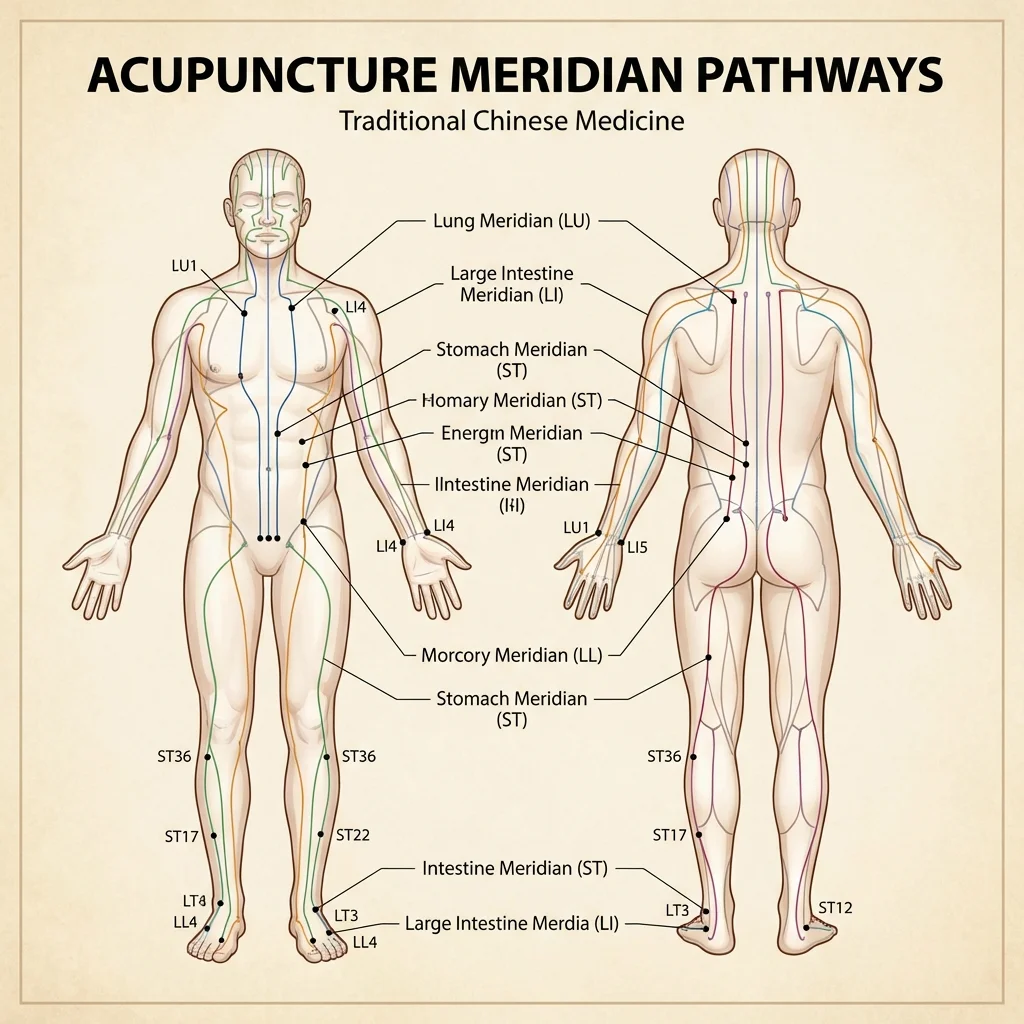
Today, the practice exists in several forms. Traditional Chinese acupuncture uses manually inserted needles retained for 15 to 30 minutes. Electroacupuncture adds mild electrical stimulation to the needles. Auricular acupuncture targets points on the ear. Dry needling, though technically distinct, borrows from acupuncture principles to target myofascial trigger points. The clinical evidence varies depending on which form is studied and for which condition.
The Science Behind Acupuncture: From Adenosine to Brain Imaging
One of the clearest breakthroughs came from a 2010 study published in Nature Neuroscience. Researchers found that rotating an acupuncture needle caused a 24-fold increase in adenosine concentration at the insertion site. Adenosine is a naturally occurring molecule that dampens pain signaling. When the team used mice lacking adenosine A1 receptors, the analgesic effect disappeared entirely. Blocking the enzymes that break down adenosine tripled how long the pain relief lasted.
That local chemical story is only part of the picture. Several central nervous system mechanisms operate simultaneously:
| Mechanism | What Happens | Key Evidence |
|---|---|---|
| Adenosine release | 24-fold local increase dampens pain signaling | Goldman et al., Nature Neuroscience, 2010 |
| Endogenous opioid release | Triggers enkephalin, beta-endorphin, and dynorphin production | Multiple studies since the 1970s |
| Vagal-adrenal anti-inflammatory axis | Electroacupuncture drives catecholamine release that suppresses systemic inflammation | Liu et al., Nature, 2021 |
| Cytokine modulation | Decreases TNF-alpha, IL-1beta, IL-6; increases anti-inflammatory IL-4 and IL-10 | Journal of Inflammation Research, 2022 |
| Brain network changes | Modulates default mode network, anterior cingulate cortex, insula, and thalamus | fMRI meta-analysis, 2019 |
Functional MRI studies have repeatedly shown that acupuncture alters activity in brain regions tied to pain processing, including the anterior cingulate cortex, insula, and thalamus. Sham acupuncture triggers overlapping but weaker brain changes, which helps explain why placebo-controlled trials sometimes show modest effect sizes. The sham procedure is not truly inert.
This distinction matters. A 2014 analysis published in PLoS ONE found that non-penetrating sham devices yielded an effect size gap of 0.43 between real and sham acupuncture. When the sham involved penetrating needles (which themselves trigger some adenosine release and neural activation), the gap shrank to 0.17. The sham isn't truly a placebo, and it partially masks acupuncture's real therapeutic effect.
Conditions With Strong Clinical Evidence
The strongest body of evidence comes from the Acupuncture Trialists' Collaboration, an individual patient data meta-analysis covering 20,827 patients across 39 randomized controlled trials. Published in the Journal of Pain in 2018, it's the closest thing the field has to a definitive answer. Acupuncture was statistically superior to both sham and no-treatment controls for every pain condition studied. Effects persisted at one year with only about a 15% decline.
| Condition | Effect Size vs. Sham (SMD) | Effect Size vs. No Treatment (SMD) |
|---|---|---|
| Shoulder pain | 0.57 (medium) | Not separately reported |
| Musculoskeletal pain | 0.30 (small-medium) | 0.54 (medium) |
| Knee osteoarthritis | 0.24 (small) | 0.63 (medium) |
| Chronic headache | 0.16 (small) | 0.44 (medium) |
Chronic low back pain has the most guideline support. The American College of Physicians recommends acupuncture as a first-line nonpharmacologic treatment for both acute and chronic low back pain, giving it a strong recommendation grade. A 2024 systematic review of acupuncture versus oral medications (including NSAIDs) for low back pain found acupuncture to be slightly more effective across 14 studies and 1,263 participants. If you deal with persistent back pain, our guide on desk job back pain and posture exercises covers complementary approaches.
Migraine prevention stands out for its number needed to treat (NNT) values. Cochrane review data shows an NNT of 4 versus usual care and 11 versus sham. In concrete terms: 50 out of 100 people getting real acupuncture saw their headache frequency cut in half, compared to 41 with sham and 17 with usual care alone. Compared head-to-head with prophylactic drugs, acupuncture performed comparably (59 vs. 54 out of 100) with fewer side effects.
Tension-type headache results are even stronger, with an NNT of 3 versus usual care and 13 versus sham. At least six sessions over a month are needed for best results. If stress triggers your headaches, breathing techniques for stress relief work well alongside acupuncture.
Knee osteoarthritis evidence is extensive: a 2024 systematic review covered 80 trials with 9,933 participants. A separate durability analysis of 10 RCTs with 3,221 patients found benefits lasting approximately 4.5 months after treatment ended. The American College of Rheumatology and Arthritis Foundation conditionally recommend acupuncture for knee, hip, and hand osteoarthritis.
Chemotherapy-induced nausea and vomiting shows a more nuanced picture. A 2023 meta-analysis of 38 RCTs covering 2,503 patients found acupuncture plus usual care improved delayed vomiting control (RR 1.47). But when compared specifically to sham acupuncture, the difference was not statistically significant. The certainty of evidence here is low.
The pattern across conditions: acupuncture consistently beats doing nothing by a meaningful margin. It also beats sham, but by a smaller margin. That gap between sham and real acupuncture is genuine, just not as dramatic as the gap between acupuncture and no treatment at all.
How Acupuncture Compares to Conventional Pain Treatments
The practical question for most people is not whether acupuncture outperforms a sham needle. It is whether acupuncture competes with the standard options their doctor would otherwise prescribe.
| Treatment | Effectiveness for Chronic LBP | Common Side Effects | Long-term Risks |
|---|---|---|---|
| Acupuncture | Slightly superior to oral meds in 14-study review | Minor bruising (9.3%), needle-site pain | Serious AE: 1 per 10,000 patients |
| NSAIDs (ibuprofen, naproxen) | Moderate short-term relief | GI upset, ulcers, bleeding | Cardiovascular risk, kidney damage |
| Opioids | Moderate short-term, no long-term benefit | Constipation, sedation, nausea | Dependence, overdose risk |
| Physical therapy | Strong evidence for LBP | Soreness, time commitment | Minimal |
The NIH's National Center for Complementary and Integrative Health (NCCIH) characterizes acupuncture's pain-relieving effect as comparable to that of NSAIDs for several chronic pain conditions. The advantage lies in the side effect profile: acupuncture does not carry the gastrointestinal, cardiovascular, or renal risks associated with long-term NSAID use.
For people managing chronic pain through multiple approaches, our guide to natural pain relief remedies covers additional evidence-based options that pair well with acupuncture.
What the Safety Data Actually Shows
The largest safety analysis to date drew on 21 prospective studies covering 845,637 patients and 12.9 million treatments. Across that entire dataset, no deaths or permanent disabilities were reported when acupuncture was performed by qualified practitioners.
| Event Type | Rate | Context |
|---|---|---|
| Minor adverse events (bruising, bleeding, needle-site pain) | 9.31% of patients per treatment course | About half considered normal intended reactions |
| Serious adverse events | 1.01 per 10,000 patients (0.01%) | 7.98 per 1 million treatments |
| Pneumothorax | 1-3 per million treatments | 7 cases across 4.4 million treatments in 13 studies |
| Nerve injury | 0.05% (Taiwan database) | Usually temporary |
A 2025 analysis of Taiwan's national health insurance database covering millions of treatments confirmed a pneumothorax rate of 0.87 per million treatments, consistent with the global estimates. The German study by Witt et al. tracked 229,230 patients across 2.2 million sessions: 8.6% reported any adverse event, 2.2% needed treatment, and zero deaths occurred.
The risk is not zero. Pneumothorax (collapsed lung from a needle inserted too deeply near the chest) is the most serious documented complication, but it occurs at roughly 1 in a million treatments. For perspective, the risk of serious GI bleeding from regular NSAID use is substantially higher.
Across 12.9 million documented treatments by qualified practitioners, zero deaths and zero permanent disabilities. That's a safety record most interventional procedures would envy. The catch: "qualified practitioner" and "sterile single-use needles" are doing a lot of work in that sentence.
What to Expect During an Acupuncture Session
A first acupuncture visit typically lasts 60 to 90 minutes. The practitioner takes a detailed health history, often asking about things a conventional doctor might skip: sleep patterns, digestion, emotional state, temperature preferences. In traditional Chinese medicine, these details guide the treatment plan.
The needles themselves are hair-thin, far smaller than hypodermic needles used for injections. Most people feel a mild pinch at insertion, followed by a sensation described as heaviness, warmth, or tingling at the needle site. This sensation, called de qi, is considered a sign of proper needle placement. The needles stay in for 15 to 30 minutes while you rest.
Treatment frequency depends on the condition:
- Acute issues (recent injury, acute headache): 1-2 sessions per week for 2-4 weeks
- Chronic conditions (persistent back pain, recurring migraines): Weekly sessions for 8-12 weeks, then tapering
- Maintenance care: Monthly sessions once symptoms stabilize
The NICE guideline specifically recommends a single course of up to 5 sessions in a community setting for chronic primary pain. Most clinical trials showing significant results used 6 to 15 sessions over several weeks.
Post-session, people commonly report feeling relaxed or mildly fatigued. Some notice improvement after the first session; others need several visits before the cumulative effect becomes apparent. Research from the Vickers meta-analysis shows treatment effects build over time and persist for at least a year with only about 15% decline.
If stress and tension are part of what drives your symptoms, incorporating strategies for HPA axis recovery from chronic stress can complement what acupuncture does in the treatment room.
Finding a Qualified Practitioner and Understanding Costs
Practitioner credentials vary by state, but the most recognized credential in the US is the Licensed Acupuncturist (L.Ac.) credential. As of 2023, there are 34,524 active licensed acupuncturists practicing across the country. Forty-seven states plus the District of Columbia use exams administered by the National Certification Commission for Acupuncture and Oriental Medicine (NCCAOM).
What to look for:
- L.Ac. (Licensed Acupuncturist): Completed a master's or doctoral program in acupuncture (typically 3-4 years) and passed the NCCAOM exam
- Dipl.Ac. (NCCAOM Diplomate): National board certification, required in most states
- DAOM (Doctor of Acupuncture and Oriental Medicine): Advanced clinical doctorate
- MD or DO with acupuncture training: Some physicians complete 200-300 hour programs
Cost expectations: Sessions typically run $75 to $150, with initial consultations sometimes higher. Some practitioners offer sliding-scale fees or package discounts. The US acupuncture industry reached $825.9 million in market size in 2025 across 8,165 practices.
Insurance coverage: Medicare Part B covers acupuncture for chronic low back pain only, allowing up to 12 sessions in 90 days and 20 per year if improvement is documented. However, Medicare does not allow licensed acupuncturists to bill directly; the treatment must be provided or supervised by an MD, DO, NP, or PA. Major private insurers including Aetna, Cigna, UnitedHealthcare, and many Blue Cross Blue Shield plans cover acupuncture for various conditions, though specifics vary by plan and state.
Acupuncture Myths vs. Research-Backed Facts
| Common Myth | What the Evidence Shows |
|---|---|
| "Acupuncture is just a placebo." | The Vickers meta-analysis of 20,827 patients found acupuncture statistically superior to sham across all conditions. However, part of the sham response may be due to sham needles triggering biological effects (adenosine release, neural activation), not purely psychological placebo. |
| "The needles are painful." | Acupuncture needles are 0.12-0.35 mm in diameter, far thinner than injection needles (0.7-0.8 mm). Most patients report a mild sensation, not pain. |
| "You need dozens of sessions to feel anything." | Migraine trials showed meaningful improvement within 4-6 sessions. NICE recommends as few as 5 sessions for chronic pain benefit. |
| "It only works for pain." | Clinical trials support use for nausea (especially post-surgery and during chemotherapy), insomnia, anxiety, and allergic rhinitis, though the evidence is strongest for pain conditions. |
| "Any acupuncturist will do." | Individualized treatment by experienced practitioners consistently outperforms standardized protocols. Training and licensing matter. |
For those exploring other wellness therapies alongside acupuncture, infrared sauna therapy operates through a different mechanism (heat stress) but shares some of the same pain-relief and anti-inflammatory pathways.
Frequently Asked Questions
Does acupuncture hurt?
Most people describe a brief pinch at insertion, followed by a dull ache, warmth, or tingling called de qi. The needles used are hair-thin (0.12-0.35 mm diameter), much smaller than those used for blood draws or injections. The majority of patients find the experience relaxing rather than painful.
How many sessions do I need before seeing results?
It depends on the condition. Migraine prevention trials show meaningful improvement within 4 to 6 sessions. For chronic low back pain, most clinical protocols run 8 to 12 weekly sessions. The NICE guideline recommends trying a course of up to 5 sessions to assess your individual response before committing to longer treatment.
Is acupuncture covered by insurance?
Medicare Part B covers acupuncture for chronic low back pain (up to 12 sessions in 90 days, 20 per year). Major private insurers such as Aetna, Cigna, and UnitedHealthcare include acupuncture in many plans, though coverage varies. Check your specific plan or call your insurer before scheduling.
Can acupuncture be combined with other treatments?
Yes. Acupuncture is commonly used alongside physical therapy, medication, and other approaches. Several clinical guidelines, including those from the American College of Physicians, position acupuncture as part of a multimodal pain management strategy. Inform your acupuncturist about all medications and treatments you are using.
What is the difference between acupuncture and dry needling?
Acupuncture uses traditional Chinese medicine theory to select needle points along meridian pathways. Dry needling specifically targets myofascial trigger points (muscle knots) and is based on Western anatomy. Both involve thin needles, but the treatment philosophy, point selection, and practitioner training requirements differ. Licensed acupuncturists complete 3-4 year graduate programs, while dry needling certifications for physical therapists typically involve shorter courses.
Related Articles
- Natural Remedies for Pain Relief — Evidence-based alternatives to over-the-counter and prescription painkillers, including herbal and lifestyle approaches.
- Sciatica Management and Recovery Guide — Sciatica causes, treatment options, and rehabilitation strategies that actually work for lasting relief.
- Chronic Stress, Hormones, and HPA Axis Recovery — How prolonged stress rewires your hormonal system and what steps restore healthy cortisol rhythms.
- Desk Job Back Pain and Posture Exercises — Targeted exercises and ergonomic adjustments for people who spend long hours sitting at a desk.
- Infrared Sauna Health Benefits — What the research says about infrared heat therapy for pain, recovery, and cardiovascular health.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.