What a full-body MRI scans (and how it differs from diagnostic imaging)
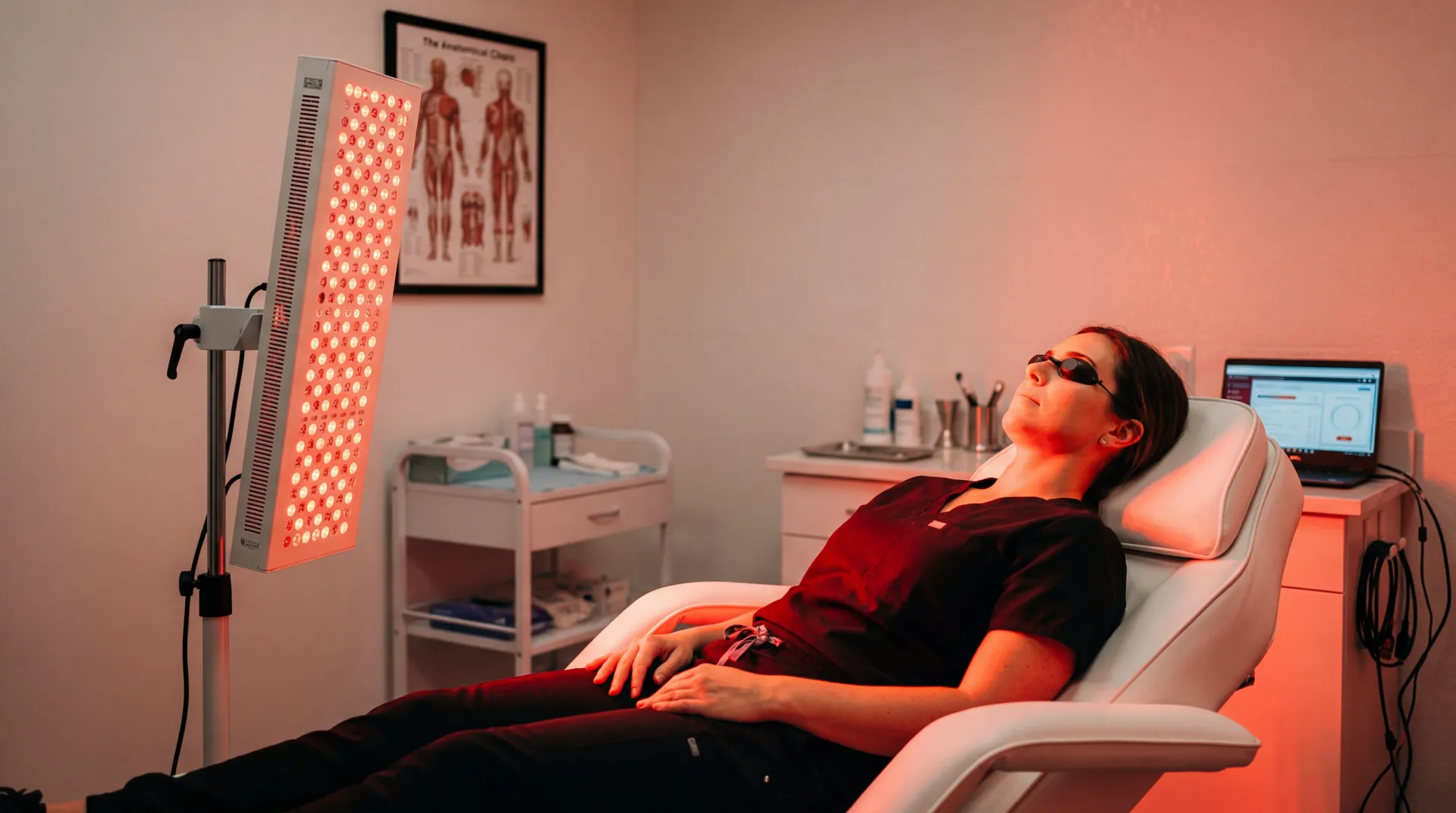
A full-body MRI works the way all MRI machines do: strong magnetic fields and radio waves create detailed images of your internal structures without ionizing radiation or contrast dyes. You lie still for 30 to 60 minutes while the machine captures cross-sectional images of your organs, bones, and soft tissues. No needles, no radiation. You walk in healthy, change into scrubs, and walk out the same way -- ideally with confirmation that everything looks fine.
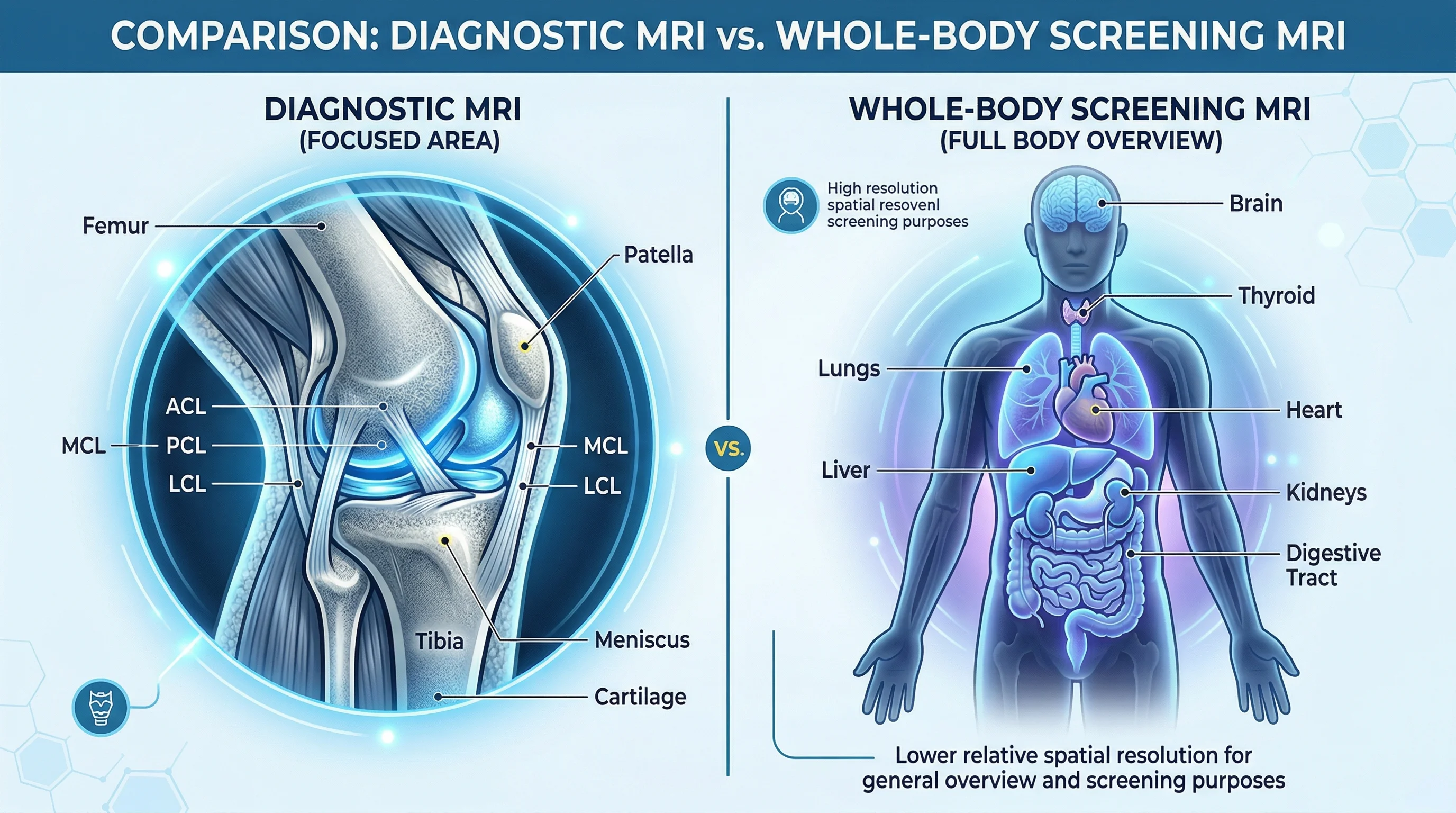
But screening MRI differs from diagnostic MRI in a way that matters. When your doctor orders an MRI of your knee or brain, the machine spends its entire scan time on that one area, using protocols tuned for that anatomy. A screening whole-body MRI has to cover everything from skull to pelvis in the same timeframe, so each region gets less attention. Like the difference between a building inspector spending a full day on your foundation versus walking through every room of a 30-story building in an hour. Both inspections have value, but they catch different things.
Prenuvo says its scan captures over one billion data points and produces 10 times more clinical-grade images than traditional MRIs, covering 49 organs and body systems. SimonMed uses clinical-grade 3T MRI machines -- the same field strength used at major academic medical centers. Both use AI-assisted interpretation alongside board-certified radiologists.
One limitation to understand: screening whole-body MRIs skip intravenous contrast agents for safety reasons. Contrast helps light up even tiny tumors and reveals their boundaries with surrounding tissue. Without it, certain cancers -- particularly breast cancers -- are harder to spot. The breast portion of Prenuvo's scan does not meet the American College of Radiology's accreditation standards for breast MRI, which require contrast. That distinction gets buried in the marketing.
Prenuvo vs SimonMed: the two biggest players compared
Prenuvo and SimonMed take different approaches to the same market. Prenuvo is the premium brand: a dedicated screening company with its own facilities, proprietary protocols built over 15 years of practice since co-founder Dr. Raj Attariwala launched the concept in 2018, and $120 million in venture funding from investors including former Google CEO Eric Schmidt and 23andMe co-founder Anne Wojcicki. SimonMed is the value play: an established imaging company with hundreds of existing radiology centers that added whole-body screening as a new service line through its simonONE brand.
The pricing gap between them is substantial.
| Provider | Scan type | Coverage | Price | Scan time |
|---|---|---|---|---|
| SimonMed | Core MRI | Chest, abdomen, pelvis | $899-$999 | ~30 min |
| SimonMed | Core Plus Head/Neck | Core + brain, MRA | $1,599-$1,799 | ~45 min |
| SimonMed | Core Plus Head/Neck/Spine | Most comprehensive | $2,199-$2,499 | ~60 min |
| Prenuvo | Full-body | Head to pelvis, 49 organs | $2,499 | ~60 min |
| Ezra | Full-body Flash | Full body | $1,350 | ~30 min |
| Ezra | Full-body | Full body + lungs | $1,950-$2,350 | ~60 min |
Prenuvo's edge is volume. By December 2024, the company had completed 100,000 whole-body MRI scans -- more than any competitor. That scan volume feeds into its AI development and gives its radiologists more experience reading screening results. The company also employs more than 80 board-certified radiologists dedicated exclusively to whole-body MRI interpretation.
SimonMed's advantage is accessibility. With locations across Arizona, Florida, California, New York, and several other states, it already has the infrastructure. Its Core MRI at $899 is the lowest price point from a major provider. Both SimonMed and Prenuvo accept HSA and FSA payments, which helps soften the out-of-pocket cost.
Neither company's scans are covered by health insurance. That probably won't change soon given current medical consensus, though Prenuvo did announce a partnership with insurer John Hancock, whose Vitality members receive a $500 discount on whole-body scans.
The clinical data gap: Prenuvo launched Project Hercules in June 2024 -- a 10-year study aiming to enroll 100,000 participants to assess whether its screening approach improves health outcomes. This is the first prospective trial of its kind. Until it produces long-term data, the question of whether these scans save lives remains unanswered.
What the scans catch -- and what they miss
Early data from Prenuvo's Polaris study offers the most specific look at what these scans find. Among 1,011 mostly asymptomatic individuals, about 2.2% were diagnosed with biopsy-confirmed cancers, including kidney, bladder, and ovarian cancers that standard screening programs would not have targeted. That cancer detection rate aligns with an independent peer-reviewed study of 576 asymptomatic participants where 2.6% had cancers and 4.8% had intracranial aneurysms, with 11.2% receiving treatment triggered by the scan.
A broader Prenuvo study of over 3,000 patients found that 93% had at least one previously undiagnosed finding, and 2% had potentially life-threatening conditions including aneurysms and early-stage cancers. Among patients with clear scans, 99.8% remained cancer-free for at least one year.
Those numbers need context. Finding something on a scan is not the same as finding something that would have hurt you. In the Polaris study, about half the biopsies prompted by scan findings turned out to be cancer. The other half were benign. And that 93% finding rate includes everything from a slightly herniated disc to a small liver cyst -- conditions that might never cause a single symptom.
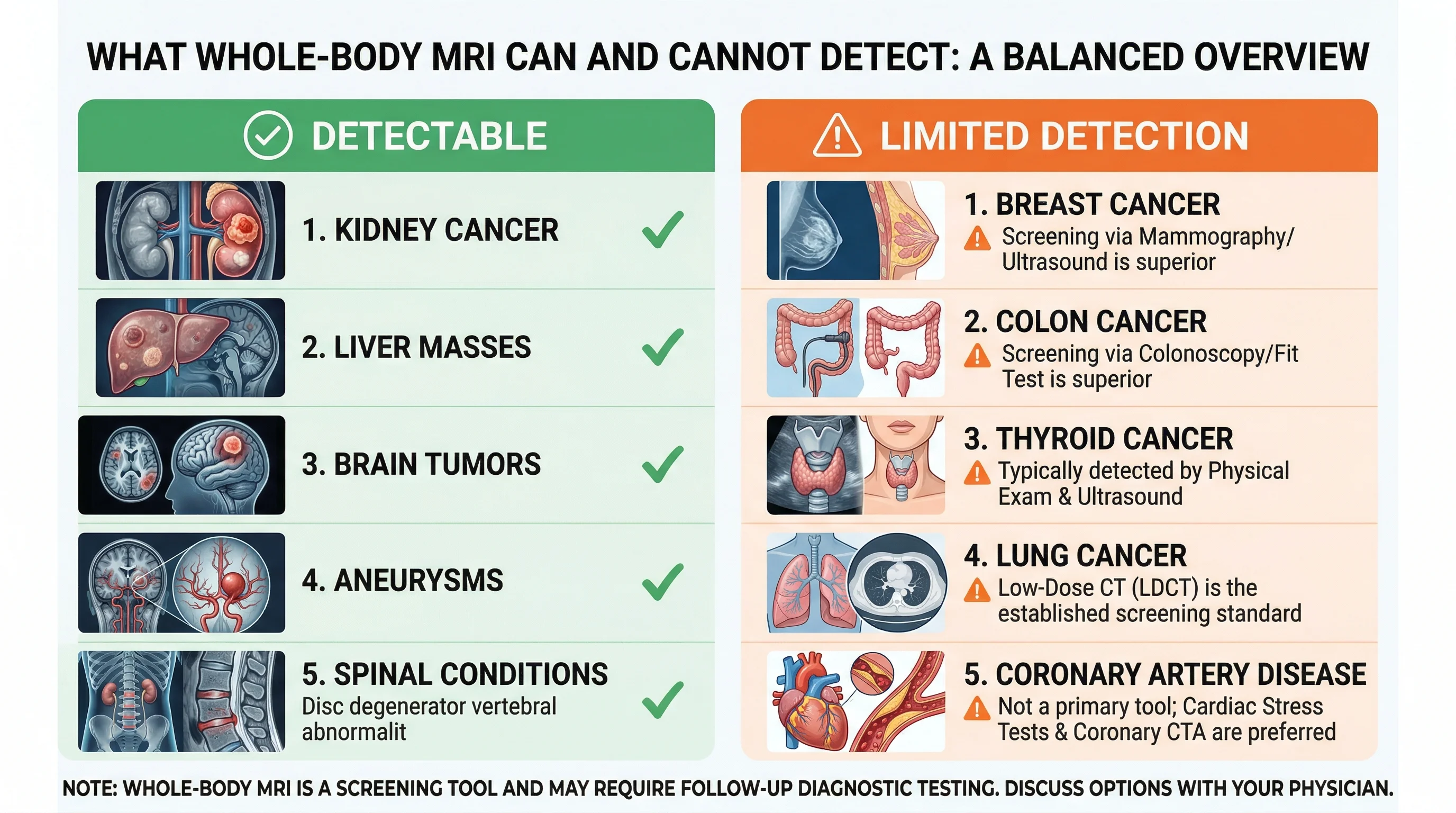
What whole-body MRI struggles with:
| Cancer/Condition | WB-MRI limitation | Better screening alternative |
|---|---|---|
| Breast cancer | No contrast = missed lesions | Mammography + dedicated breast MRI |
| Colon cancer | Bowel imaging poor without prep | Colonoscopy |
| Thyroid cancer | Small nodules often missed | Thyroid ultrasound |
| Lung cancer | MRI less sensitive than CT for lungs | Low-dose CT (for eligible patients) |
| Coronary artery disease | Not designed for cardiac assessment | CT calcium scoring, stress tests |
Prenuvo itself acknowledges this, including disclaimers that its MRI does not replace mammograms, colonoscopies, or pap smears. But the "500 conditions detected" marketing creates an impression of comprehensiveness that the technology can't deliver. Dr. Christopher Hess, chair of radiology at UCSF, was direct: "Screening MRI is not as good as other techniques we have to detect the most common killers, such as coronary artery disease, breast cancer, colon cancer, and stroke."
The false positive problem nobody warns you about
In a systematic review of 12 studies covering 5,373 asymptomatic subjects, 32.1% had critical or indeterminate incidental findings. One in three people walked away from their scan with something that needed further investigation. The pooled false-positive rate across six of those studies was 16%. Roughly one in six got a finding that eventually proved to be nothing.
A separate review by Zugni and colleagues examined 6,214 patients and found that 95% had at least one abnormal finding, but 91% of those findings were not clinically relevant. Only 1.8% had confirmed malignancy. For every person whose scan finds a real cancer, roughly 50 people get findings that generate anxiety, trigger follow-up tests, and cost additional money for nothing medically useful.
Dr. Matthew Davenport, a professor of radiology at the University of Michigan, has studied this problem extensively. In his clinical experience, 20% to 40% of cross-sectional imaging studies like MRIs have incidental findings. He described the psychological shift bluntly: "It makes healthy people think of themselves as patients."
A small study drives the point home. When 22 healthy adults underwent whole-body MRI, 20 had incidental findings and only two had completely clean reports. Those findings required follow-up including eight ultrasounds, six CT scans, two mammograms, two additional MRIs, and one biopsy. The patients needed referrals to urologists, rheumatologists, internists, pulmonologists, surgeons, and gynecologists. One person had cancer. The other 19 went through a medical gauntlet for nothing.
South Korea offers a cautionary parallel. In 1999, the country expanded ultrasound screening for thyroid cancer after noticing rising death rates. Detection increased more than six-fold, but most of what they found were small, indolent tumors that would never have caused harm. Patients underwent biopsies, surgeries, and follow-up monitoring for years. Some had surgical complications. The overall death rate from thyroid cancer did not change.
The overdiagnosis trap: Screening is most likely to find slow-growing, indolent conditions rather than the fast-moving aggressive cancers that kill people. The aggressive cancers tend to appear between screening intervals, which means a once-a-year scan has a narrow window to catch them at a treatable stage. Dr. Davenport estimates the chance of a whole-body scan detecting a fast-growing, treatable cancer in an asymptomatic person at roughly one in 10,000.
Who should consider paying for a scan
Medical consensus is skeptical, but it paints with a broad brush. Some people have a different risk profile than the average healthy adult.
If you have a strong family history of cancers that are hard to detect through standard screening -- particularly kidney, pancreatic, or ovarian cancers -- a whole-body MRI can survey organs that no existing screening program targets. Dr. Davenport at Michigan noted that "imaging is appropriate for patients who have a genetic risk of life-threatening cancer or have a sign or symptom of significant disease." People with Li-Fraumeni syndrome, Lynch syndrome, or other hereditary cancer predisposition conditions already use regular MRI as part of established surveillance protocols.
Longitudinal monitoring also changes the math. Dr. Daniel Sodickson, chief scientist at Ezra and director of advanced imaging research at NYU, argues that the real value of whole-body MRI appears when you stop thinking of it as a single test and start thinking of it as a baseline. "The way to start thinking about full-body MRI is not as a one-shot, yes-or-no test but as a kind of longitudinal monitoring," he said. "That's the best way to rule out false positives -- not by doing a full-court press for every uncertain and low-risk finding, but by comparing with previous scans and assessing whether there has been a change."
In that model, the first scan establishes what "normal" looks like for your body. The second scan, a year or two later, shows what changed. A cyst that was there last year and hasn't grown is likely benign. A new mass that wasn't present before warrants investigation. This approach reduces anxiety and unnecessary follow-up testing, though it also doubles or triples the total cost.
| Scenario | WB-MRI may be reasonable | Standard screening likely better |
|---|---|---|
| Strong family history of rare cancers | Yes -- targets unscreened organs | -- |
| Known cancer predisposition syndrome | Yes -- often covered by insurance | -- |
| General anxiety about health, no risk factors | Uncertain benefit, high false positive risk | Age-appropriate screenings first |
| Establishing a baseline for longitudinal monitoring | Reasonable if committing to repeat scans | -- |
| Healthy 30-year-old, no family history | Low yield, high risk of unnecessary follow-up | Annual physical, routine bloodwork |

The cost-benefit math for healthy people
Medical organizations haven't minced words. The American College of Radiology stated in April 2023: "To date, there is no documented evidence that total body screening is cost-efficient or effective in prolonging life." The FDA does not recommend full-body scans for healthy people. No insurance plan in the United States covers these scans for screening purposes.
Dr. Davenport raised a pointed question in Radiology Today: "If whole-body scans were worthwhile as a screening tool in low-risk patients, respected medical societies would be in favor of performing them. Yet, no respected medical society, no government agency, and no payer group supports it."
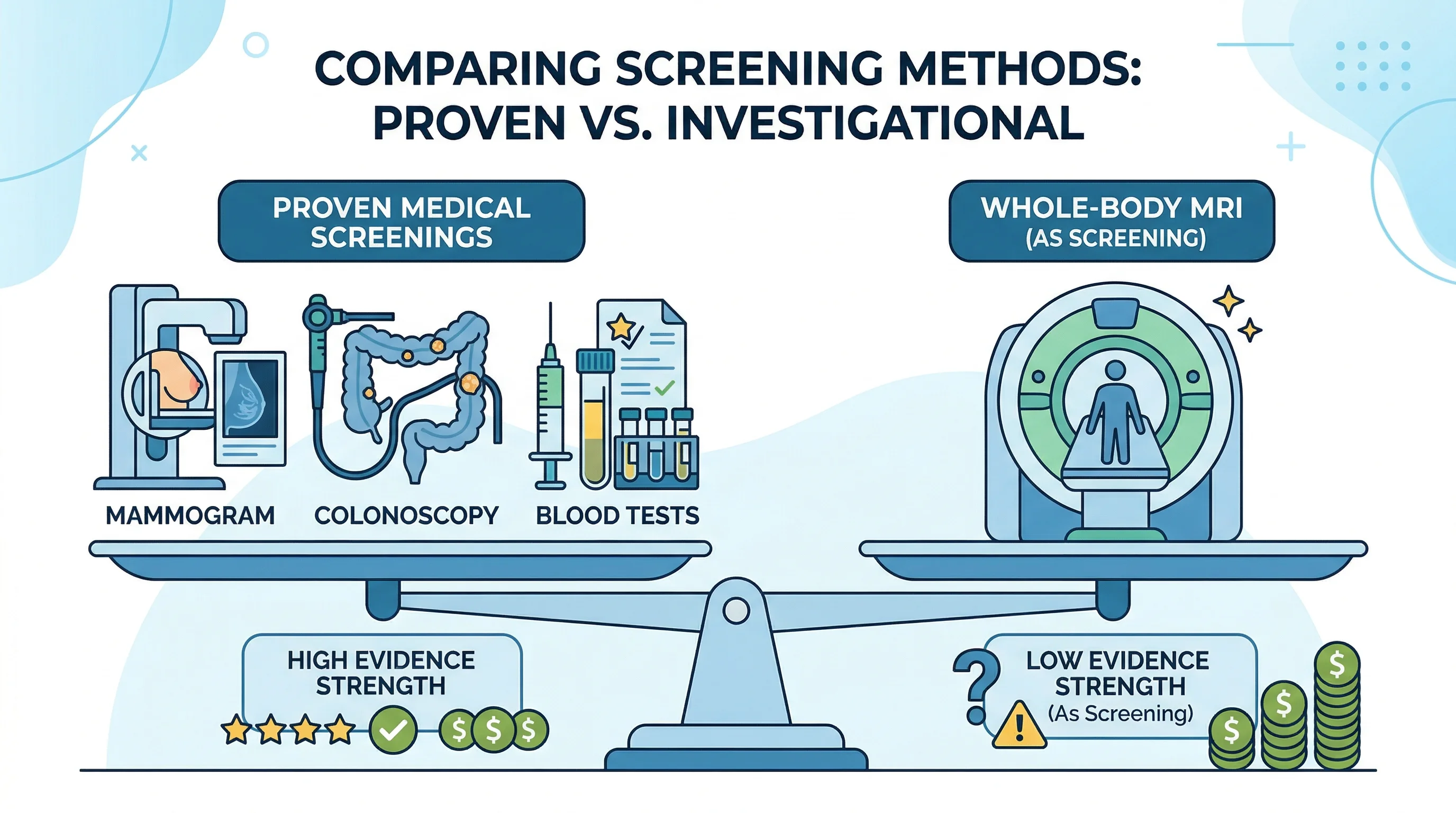
The cost comparison against proven screening says a lot. For $2,499 -- one Prenuvo scan -- you could pay for a colonoscopy ($600-$800 out of pocket without insurance), a mammogram ($150-$300), an annual physical with comprehensive bloodwork ($200-$400), a low-dose chest CT for lung cancer screening ($100-$300 if eligible), and still have money left over. Each of those tests has decades of evidence showing they reduce mortality for their target conditions. The whole-body MRI has no such evidence.
Dr. Mizra Rahman, president of the American College of Preventive Medicine, framed the incentive structure frankly. He said the greatest beneficiaries of whole-body scans "are the people who own [the scanners] and promote [the scans] because they collect the fees for doing them."
Prenuvo and its supporters counter with a different calculation: the cost of catching a cancer at stage I versus stage IV. Late-stage cancer treatment can cost hundreds of thousands of dollars and carries far worse survival rates. If a $2,499 scan catches one treatable cancer that would have become terminal, the economic and human argument for screening is overwhelming. The problem is that we don't yet know how often that scenario plays out versus the one where the scan generates expensive, anxiety-producing false alarms.
Dr. Anteo Pashaj, a kidney-care specialist who counsels patients on screening decisions, put it in practical terms: "Just like everything else in life, it's a risk-benefit analysis." He recommends asking yourself four questions before booking: What will you do if the scan finds something? Have you completed all recommended standard screenings first? What does your doctor think? And can you afford it without financial strain?
The bottom line: If you've already done your colonoscopy, mammogram, and other age-appropriate screenings, have discretionary income, understand that a clean scan isn't a guarantee and an abnormal one isn't necessarily a crisis, and are prepared for possible follow-up testing -- a whole-body MRI scan is a reasonable personal choice. If you're skipping proven screenings to pay for a Prenuvo scan instead, you're spending more money on less evidence.
Frequently asked questions
Is a full-body MRI scan safe?
MRI itself is safe for most people -- it uses magnetic fields and radio waves rather than radiation. The physical risks are minimal. The main concern is what happens after: false positive findings can trigger unnecessary biopsies, additional imaging, specialist visits, and psychological stress. People with certain metal implants, pacemakers, or cochlear implants cannot undergo MRI.
How often should you repeat a whole-body MRI?
There's no medical consensus on frequency for asymptomatic screening. Prenuvo recommends annual scans based on its internal analysis. Some imaging experts argue that the real value comes from a baseline scan followed by a comparison in one to two years, rather than treating each scan as a standalone event. The optimal interval hasn't been established by independent research.
Can a whole-body MRI replace my regular cancer screenings?
No. Whole-body MRI has specific blind spots for breast cancer (no contrast), colon cancer (poor bowel visualization), and lung cancer (CT is more sensitive). Every major medical organization and the screening companies themselves say that whole-body MRI should complement, not replace, established screenings like mammograms, colonoscopies, and pap smears.
Why don't insurance companies cover whole-body MRI screening?
Insurance coverage requires evidence that a test improves health outcomes cost-effectively. No published study has yet shown that whole-body MRI screening extends life or is cost-efficient for asymptomatic people. Prenuvo's Project Hercules study may eventually provide that data, but results from the 10-year trial are years away. You can use HSA or FSA funds to pay for the scan.
What is the difference between Prenuvo and SimonMed pricing?
Prenuvo charges $2,499 for its full-body scan. SimonMed offers a tiered approach starting at $899 for a core body scan (chest, abdomen, pelvis), $1,599 for core plus head and neck, and $2,199 for the most comprehensive option including spine imaging. Ezra falls between them at $1,350 to $2,350. All use AI-assisted interpretation and board-certified radiologists.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.