Your body runs on collagen more than you think
Collagen accounts for roughly 30% of your body's total protein. That percentage makes it more abundant than any other protein you carry around, and it shows up in places you might not expect: the walls of your blood vessels, the lining of your intestines, the cornea of your eyes, and the dentin inside your teeth.
Scientists have cataloged 28 distinct collagen types in vertebrates, each numbered with Roman numerals. But for most people weighing supplement options, only three matter: Type I, Type II, and Type III. These three account for the overwhelming majority of collagen in the human body, and they differ in where they concentrate, what they do mechanically, and how supplement manufacturers source them.
All collagen shares a signature architecture: three polypeptide chains wound into a left-handed triple helix, stabilized by glycine at every third position plus high concentrations of proline and hydroxyproline. What changes between types is the specific amino acid sequence of those chains, which dictates how each collagen assembles into larger structures. Some form thick, banded fibrils. Others create mesh-like networks. A few anchor one tissue layer to another. The structural diversity is what allows a single protein family to hold your body together from your Achilles tendon to the filter in your kidneys.
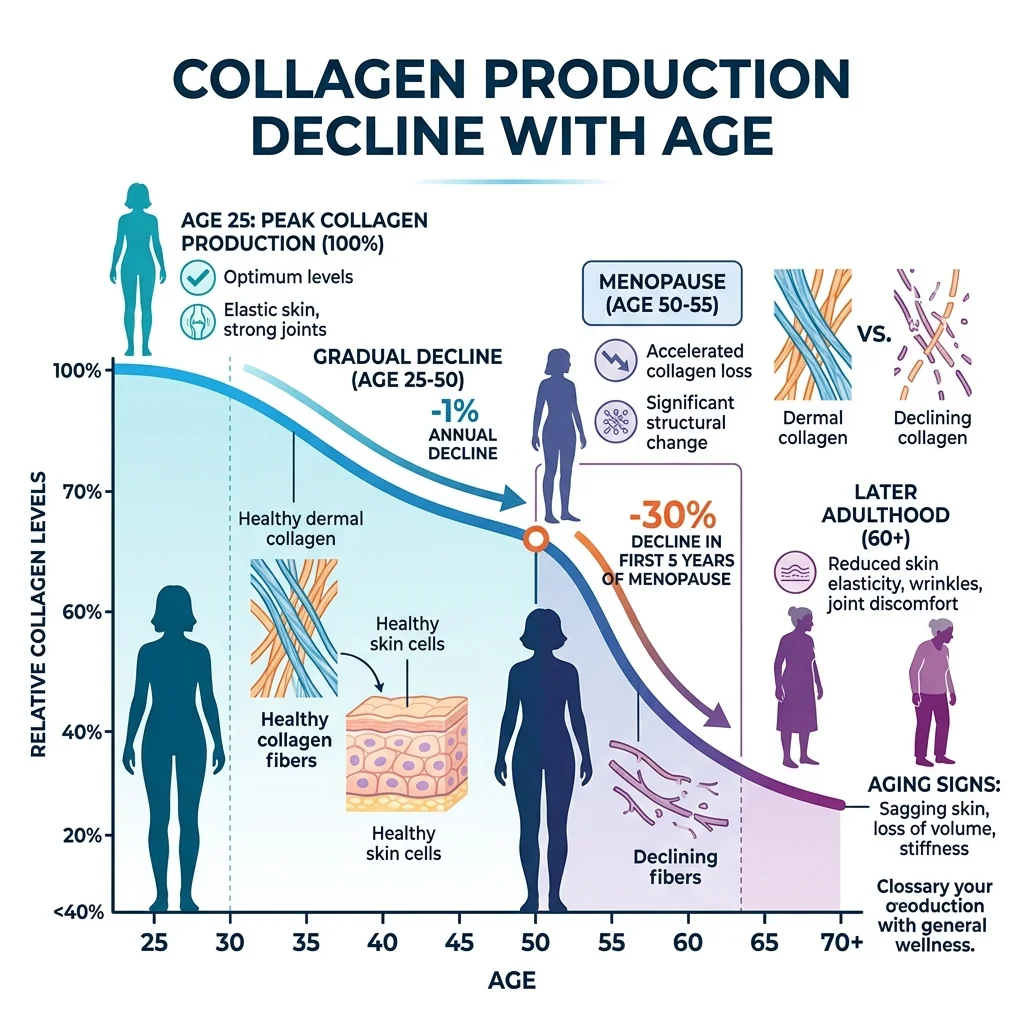
Production starts declining around your mid-twenties, dropping roughly 1% per year. Women lose about 30% of their skin's collagen in the five years after menopause, according to the American Academy of Dermatology. Smoking, excessive UV exposure, and diets high in refined sugar accelerate the loss further, because each interferes with the enzymatic processes that stabilize collagen's triple helix.
Type I: the one doing 90% of the heavy lifting
Type I collagen makes up approximately 90% of your body's total collagen. It forms densely packed fibrils with a characteristic banding pattern visible under electron microscopy, and those fibrils provide tensile strength to tissues ranging from skin to bone to cornea.
Its location tells you its function. In skin, Type I is the scaffold that keeps the dermis firm. In bone, it forms the organic matrix (roughly 80% of bone's organic component) where calcium and phosphate crystals deposit. In tendons and ligaments, Type I fibrils align along the direction of mechanical loading, resisting the pull of muscle on bone.
| Tissue | Type I collagen role | Approximate collagen content |
|---|---|---|
| Skin (dermis) | Structural scaffold for elasticity | 70-80% of dry weight |
| Bone | Organic matrix for mineral deposition | ~80% of organic matrix |
| Tendons | Tensile strength along loading axis | >80% of dry weight |
| Cornea | Transparent structural lattice | >90% of dry weight |
| Teeth (dentin) | Framework for mineralization | ~90% of organic matrix |
Type I collagen is a heterotrimer, meaning it contains two different kinds of alpha chains: two alpha-1(I) chains and one alpha-2(I) chain twisted together. This specific chain composition gives it mechanical properties distinct from homotrimeric collagens like Type II. Research on the collagen family has shown that Type I's triple helix comprises 96% of the molecule's length, making it essentially a long, stiff rod. Cross-links between adjacent molecules further stiffen the fibrils as tissue matures, which is why older tendons are tougher (but less elastic) than younger ones.
In supplements, Type I typically comes from bovine hide or fish skin. Marine collagen from fish has become popular partly because its amino acid sequence has slightly higher hydroxyproline content, though studies on bioavailability have not shown this translates into meaningfully different absorption.
For skin firmness, bone density, or tendon recovery, Type I is the collagen you'll encounter most often in supplement formulas, and the one with the most supporting clinical data for skin and aging benefits.
Type II: the cartilage collagen
Type II collagen dominates cartilage tissue, where it can make up nearly 80% of the total collagen content. Unlike Type I's role in resisting tension, Type II fibrils interweave with proteoglycans (especially aggrecan) to create a sponge-like matrix that resists compression. Every step you take compresses the cartilage in your knees, and it's this Type II collagen network that springs back after the load passes.
Type II is a homotrimer, built from three identical alpha-1(II) chains. Its fibrils are thinner than Type I fibrils, which matters mechanically: the smaller diameter allows them to form the tight, interlocking meshwork that gives cartilage its gel-like resilience. Research on human tendons has confirmed that Type II concentrates specifically in regions experiencing compressive loading, such as where the supraspinatus tendon passes under the coracoacromial arch.
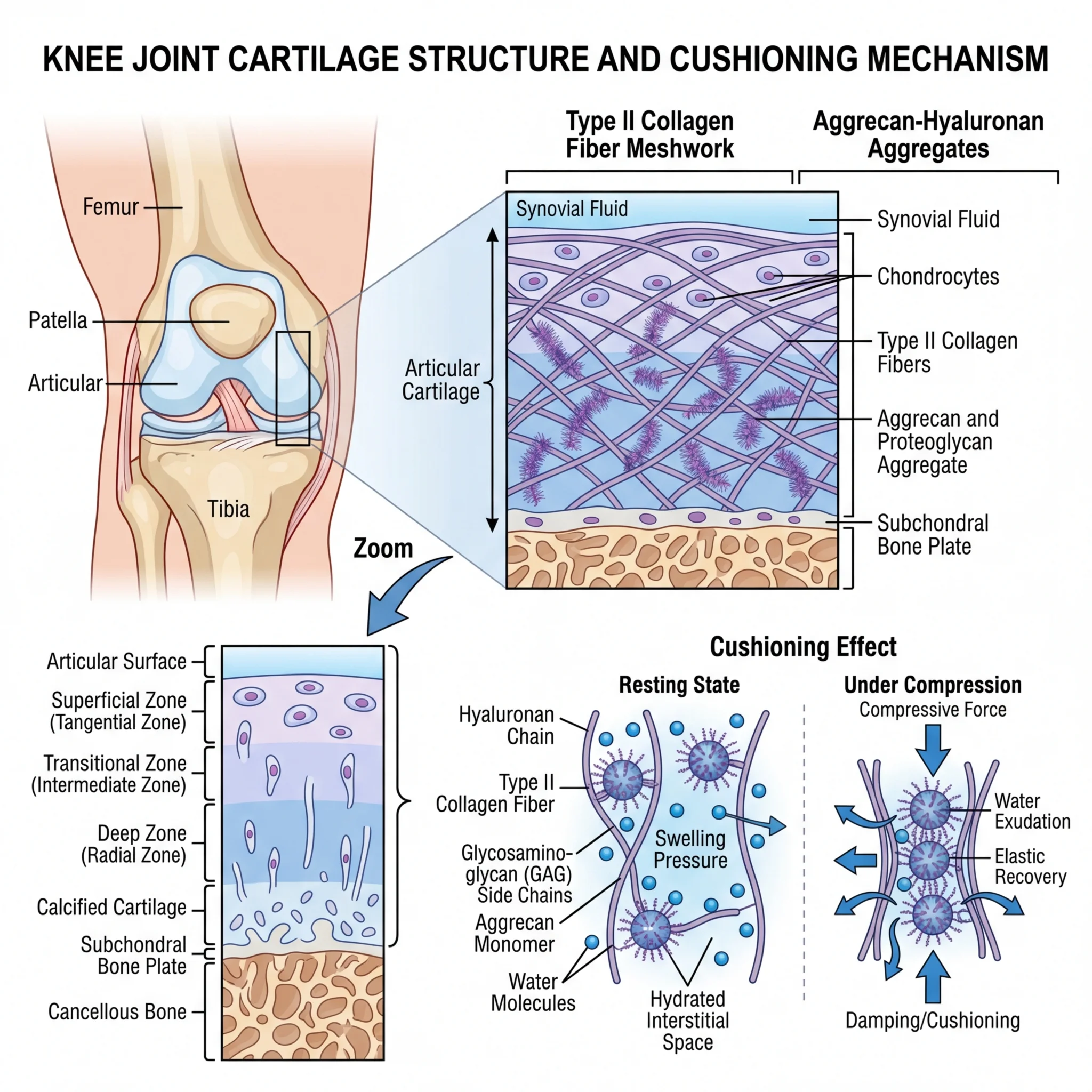
In articular cartilage, the architecture is zonal. The surface layer contains tightly packed, horizontally aligned collagen fibrils that resist shear. The middle zone has randomly oriented, thicker fibrils that absorb compression. The deep zone contains the largest-diameter fibrils arranged perpendicular to the joint surface, anchoring cartilage to the underlying bone. All three zones are predominantly Type II collagen, supported by smaller amounts of Types IX and XI that regulate fibril diameter and spacing.
Supplement forms of Type II collagen split into two categories with different mechanisms:
| Form | Source | Proposed mechanism | Typical dose |
|---|---|---|---|
| Hydrolyzed Type II | Chicken sternum cartilage | Provides peptides that may stimulate chondrocyte activity | 5-10 g/day |
| Undenatured Type II (UC-II) | Chicken sternum cartilage | Oral tolerance mechanism: small dose trains immune system to stop attacking joint cartilage | 40 mg/day |
The undenatured form is the more interesting of the two. UC-II works through a different pathway than hydrolyzed collagen: instead of flooding the body with amino acids, a 40 mg daily dose exposes gut-associated lymphoid tissue to intact Type II collagen epitopes, which may reduce the inflammatory immune response that damages cartilage in osteoarthritis. Several clinical trials have shown improved joint function with this approach, though study sizes remain modest.
If joint comfort is your primary goal, especially for age-related cartilage wear, Type II collagen (in either form) is the specific type to consider. People dealing with joint stiffness may also benefit from the anti-inflammatory compounds found in bone broth, which naturally contains multiple collagen types.
Type III: elastic fibers and wound repair
Type III collagen forms thin, elastic fibers and almost always appears alongside Type I. You find it in skin, blood vessel walls, the gut lining, and internal organs like the lungs and liver. Where Type I provides rigid tensile strength, Type III forms an elastic network that stores kinetic energy as an elastic rebound.
The biological relationship between Types I and III is dynamic, not static. During wound healing, Type III collagen production spikes first, laying down a quick provisional matrix. Over weeks and months, the body gradually replaces that Type III scaffold with stiffer Type I collagen as the wound matures, restoring roughly 50-80% of the original tissue's tensile strength. The ratio of Type I to Type III at any given site reflects the tissue's age and repair status.
Type III collagen shows up first at wound sites and in rapidly growing tissues. Over time, the body swaps it out for the more durable Type I as tissue matures. Blood vessels, intestinal walls, and the uterus all depend on Type III for elasticity.
This matters for cardiovascular health. In the myocardium, collagen Types I and III together form the structural framework around muscle cells. Type I comprises about 85% of cardiac collagen and confers stiffness, while Type III contributes resilience. When the ratio shifts too far toward Type I (as happens in fibrotic heart conditions), the heart muscle becomes excessively stiff and loses pumping efficiency. Research on patients with dilated cardiomyopathy has found abnormal accumulations of both Type I and Type III collagen in the myocardium, with the I/III ratio serving as a marker of disease progression.
In supplements, Type III collagen typically comes from bovine sources and is often found alongside Type I, since the two occur together in the tissues used for extraction (particularly bovine hide). If your focus is on skin elasticity, vascular health, or gut lining integrity, look for products that include both Types I and III. These work together in the body, so supplementing them together mirrors their natural distribution. Supporting your body's ability to manage chronic inflammation may also help preserve the Type III collagen in your blood vessels and organs.
Matching collagen types to your goals
Supplement labels don't always make this easy. Below is a mapping of common goals to collagen types, based on where each type concentrates in the body:
| Your goal | Primary type | Why | Common supplement source |
|---|---|---|---|
| Firmer, more hydrated skin | Type I (often with Type III) | Types I and III are the dominant collagens in the dermis | Bovine hide, fish skin |
| Stronger bones | Type I | Type I forms the organic matrix of bone | Bovine hide, fish skin |
| Joint comfort and cartilage support | Type II | Type II is the primary structural collagen in cartilage | Chicken sternum cartilage |
| Tendon and ligament recovery | Type I | Tendons are predominantly Type I collagen | Bovine hide, fish skin |
| Gut lining integrity | Types I and III | Both types are present in the intestinal wall | Bovine hide, multi-collagen blends |
| Blood vessel elasticity | Type III (with Type I) | Type III provides vascular elasticity | Bovine sources |
| Hair and nail strength | Type I | Provides structural protein for hair follicle dermal papilla | Bovine or marine |
One persistent myth: that you can direct collagen peptides to a specific body part by taking the "right" type. As MD Anderson dietitian Lindsey Wohlford explains, your body breaks down collagen supplements into amino acids and reassembles them wherever it sees fit. You cannot steer those amino acids to your knees any more than you can steer vitamin C to your left hand. What you can do is supply the raw materials that your body's collagen-building machinery needs, then trust the biological triage system to allocate them.
That said, the form of Type II collagen matters for joint applications. Undenatured Type II collagen works through immune modulation rather than amino acid supply, so its mechanism is distinct from hydrolyzed collagen peptides. For that reason, joint-focused supplementation does have a more type-specific rationale than skin or bone supplementation does.
How your body actually absorbs collagen supplements
A persistent misunderstanding drives collagen marketing: that eating collagen gives you collagen. Your gastrointestinal tract breaks it down before it can enter circulation.
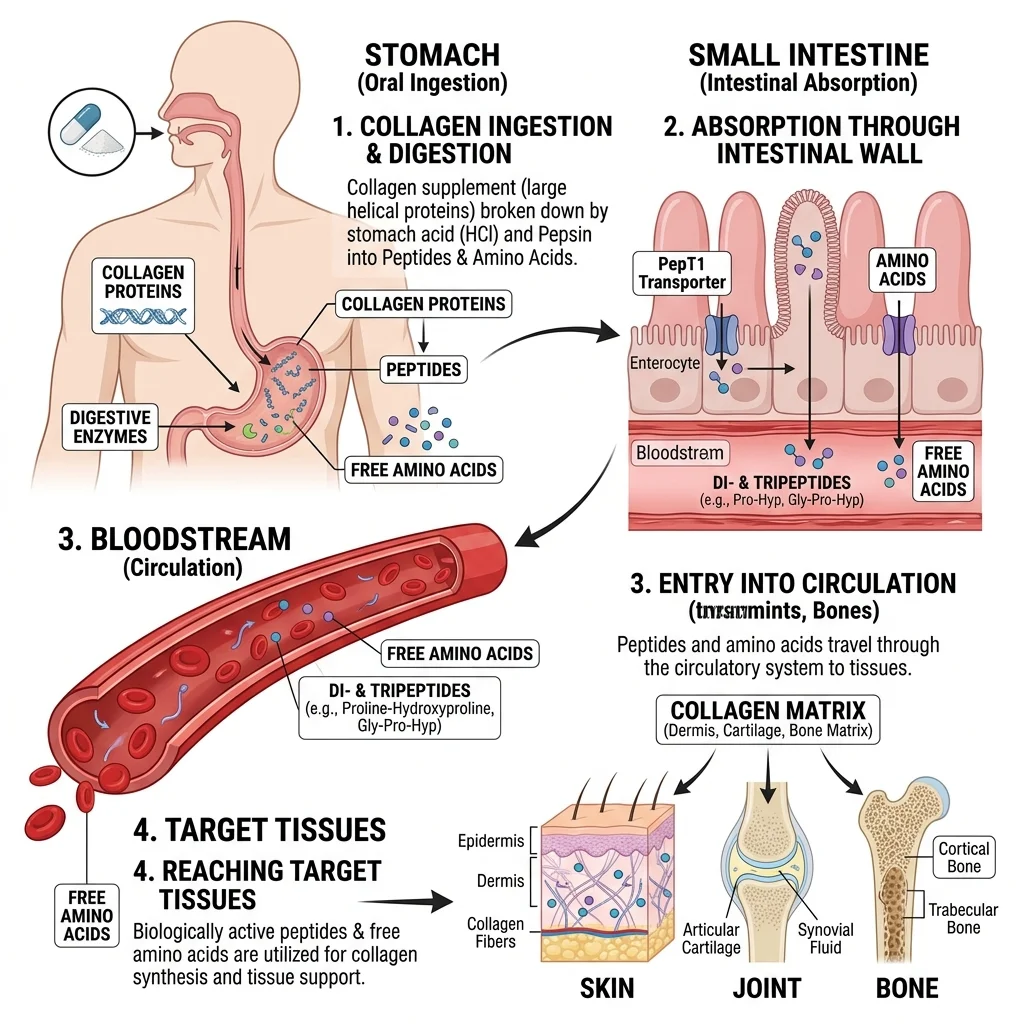
But the breakdown products aren't just random amino acids. A 2024 randomized, double-blind crossover study published in Frontiers in Nutrition measured what actually reaches the bloodstream after ingesting 10 grams of collagen hydrolysate. The results showed that both free amino acids and bioactive di- and tripeptides like Pro-Hyp and Gly-Pro-Hyp appear in human blood after ingestion. These small peptides are absorbed intact through a specific intestinal transporter called PepT1, and they may act as signaling molecules that stimulate fibroblast activity rather than simply serving as building blocks.
The same study compared fish, porcine, and bovine collagen hydrolysates of different molecular weights. Free hydroxyproline absorption was comparable across all sources. Total hydroxyproline (which includes peptide-bound forms) was 36-47% higher than free hydroxyproline alone, confirming that a substantial portion reaches the blood as peptides rather than individual amino acids. The lower molecular weight bovine product (2,000 Da) showed slightly higher total hydroxyproline bioavailability than the higher molecular weight version (5,000 Da).
| Supplement form | How it works | Molecular weight | Absorption |
|---|---|---|---|
| Gelatin | Partially hydrolyzed collagen; gels in liquid | ~50,000-100,000 Da | Slower; requires more GI breakdown |
| Hydrolyzed collagen (collagen peptides) | Enzymatically broken into small peptides | 2,000-5,000 Da | Absorbed as peptides and amino acids |
| Undenatured Type II collagen (UC-II) | Intact collagen epitopes for immune modulation | Native structure preserved | Acts on gut-associated lymphoid tissue |
A recent systematic review analyzing over 60 clinical studies found that hydrolyzed collagen peptides at doses of 2.5-10 grams per day improved skin elasticity and hydration within 4-12 weeks, with effects enhanced when co-supplemented with vitamin C. Vitamin C matters here because it's a required cofactor for prolyl hydroxylase, the enzyme that converts proline to hydroxyproline during collagen synthesis. Without adequate vitamin C, your body cannot properly stabilize the collagen it produces regardless of how much collagen supplement you take.
As Mayo Clinic's nutrition team notes, the triple helix structure of collagen cannot be absorbed in its whole form. It gets broken down into individual amino acids and peptides in the GI tract, and your body reassembles these into whatever proteins it needs. This means the restructured proteins may not target the area a supplement manufacturer advertises.
What to look for on the label
The collagen supplement market has reached approximately $2 billion in annual sales, but the FDA does not regulate these products the way it regulates medications. That places the burden of quality evaluation squarely on you.
Here is what actually matters when choosing a collagen supplement:
Third-party testing. Look for NSF International, USP, or Informed Sport certification on the label. These certifications verify that the product contains what it claims and screens for contaminants including heavy metals. Collagen supplements can contain toxins and heavy metals since they're made from animal connective tissues, bones, and skin. If a product hasn't been third-party tested, you're guessing about purity.
Hydrolyzed form. Collagen peptides (hydrolyzed collagen) absorb more efficiently than gelatin. The molecular weight should be listed, ideally in the 2,000-5,000 Da range. You'll sometimes see "collagen peptides" and "hydrolyzed collagen" used interchangeably; they're the same thing.
Source matches your goal. Bovine and marine collagen provide predominantly Types I and III, suitable for skin, bone, and general connective tissue. Chicken-derived collagen provides Type II, relevant for joint cartilage. Multi-collagen blends exist, but they dilute each type, meaning you get less of any single one per serving.
Dosing. Clinical trials showing measurable outcomes typically use 2.5-15 grams per day of hydrolyzed collagen. Lower doses (2.5-5 g) have shown joint and skin benefits; higher doses (10-15 g) may be more relevant for body composition and muscle support. For undenatured Type II collagen (UC-II), the effective dose is much lower at approximately 40 mg/day because the mechanism is immunological rather than nutritional.
Complementary nutrients. Vitamin C is required for collagen synthesis. Some products include it; otherwise, pair your supplement with a food source of vitamin C. Copper, zinc, and manganese also participate in collagen cross-linking. A diet rich in fruits and vegetables generally covers these, but bone-supporting minerals like vitamin K2 also play a role if you're taking collagen for skeletal health.
Myth vs. fact: The idea that marine collagen is "better absorbed" than bovine collagen has entered common belief, but the 2024 bioavailability study found that free hydroxyproline uptake was comparable across fish, porcine, and bovine sources. Source preference should be based on your health goal and any dietary restrictions (fish for pescatarians, bovine for those avoiding poultry), not absorption claims.
Frequently Asked Questions
Can you take Type I and Type II collagen at the same time?
Yes. Types I and II serve different tissues and have no known negative interactions when taken together. Many people take a hydrolyzed collagen (Types I/III) alongside a small dose of undenatured Type II collagen (UC-II) for joint support. If combining, take them at different times of day, since the UC-II works best on an empty stomach and the hydrolyzed collagen can be taken with food.
How long does it take for collagen supplements to work?
Clinical trials measuring skin hydration and elasticity improvements typically show results within 4-12 weeks of daily supplementation at 2.5-10 grams. Joint function improvements in osteoarthritis studies often take 8-12 weeks. Nail changes take longer, with some studies requiring 6 months before measurable improvement in brittleness. These timelines reflect the slow turnover rate of collagen in the body, which can be 80-120 days depending on the tissue.
Does cooking destroy collagen in food?
Cooking partially denatures collagen, converting it to gelatin. This is actually helpful for absorption since gelatin is easier to digest than raw collagen fibers. Slow-cooked bone broth, braised meats, and stewed connective tissues all provide collagen-derived amino acids. The heat breaks the triple helix structure, but the amino acid content remains intact and available for your body to use.
Are plant-based collagen supplements real collagen?
No. Collagen is an animal protein and does not exist in plants. Products marketed as "plant-based collagen" or "vegan collagen" are typically blends of vitamin C, zinc, amino acids, and plant extracts intended to support your body's own collagen production. They are not collagen itself. A separate category of lab-produced collagen uses genetically modified yeast or bacteria to produce human collagen sequences, but these are not widely available in consumer supplements.
Is collagen safe for people with food allergies?
Collagen supplements are derived from animal tissues, so the source matters for allergy considerations. Fish collagen is unsuitable for people with fish allergies. Bovine collagen is generally well-tolerated, but people with red meat sensitivities (alpha-gal syndrome) should consult their physician. No significant adverse effects have been reported in clinical trials using standard doses, but the lack of FDA regulation means contaminants are a possibility in untested products.
Related Articles
- Glycine: the amino acid that supports sleep, collagen synthesis, and longevity — A closer look at glycine's role as one of collagen's three primary building blocks.
- Bone broth benefits for gut healing, joints, and skin — How slow-cooked broth provides natural collagen types alongside other joint-supporting compounds.
- Chronic inflammation and anti-inflammatory living — Why managing systemic inflammation protects the collagen in your blood vessels and joints.
- Vitamin K2 for heart and bone health — The mineral co-factors that work alongside collagen to maintain bone density.
- Autophagy: fasting, exercise, and cellular renewal — How cellular cleanup processes affect collagen turnover and tissue repair.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.












