Why Your Heart Runs on Magnesium
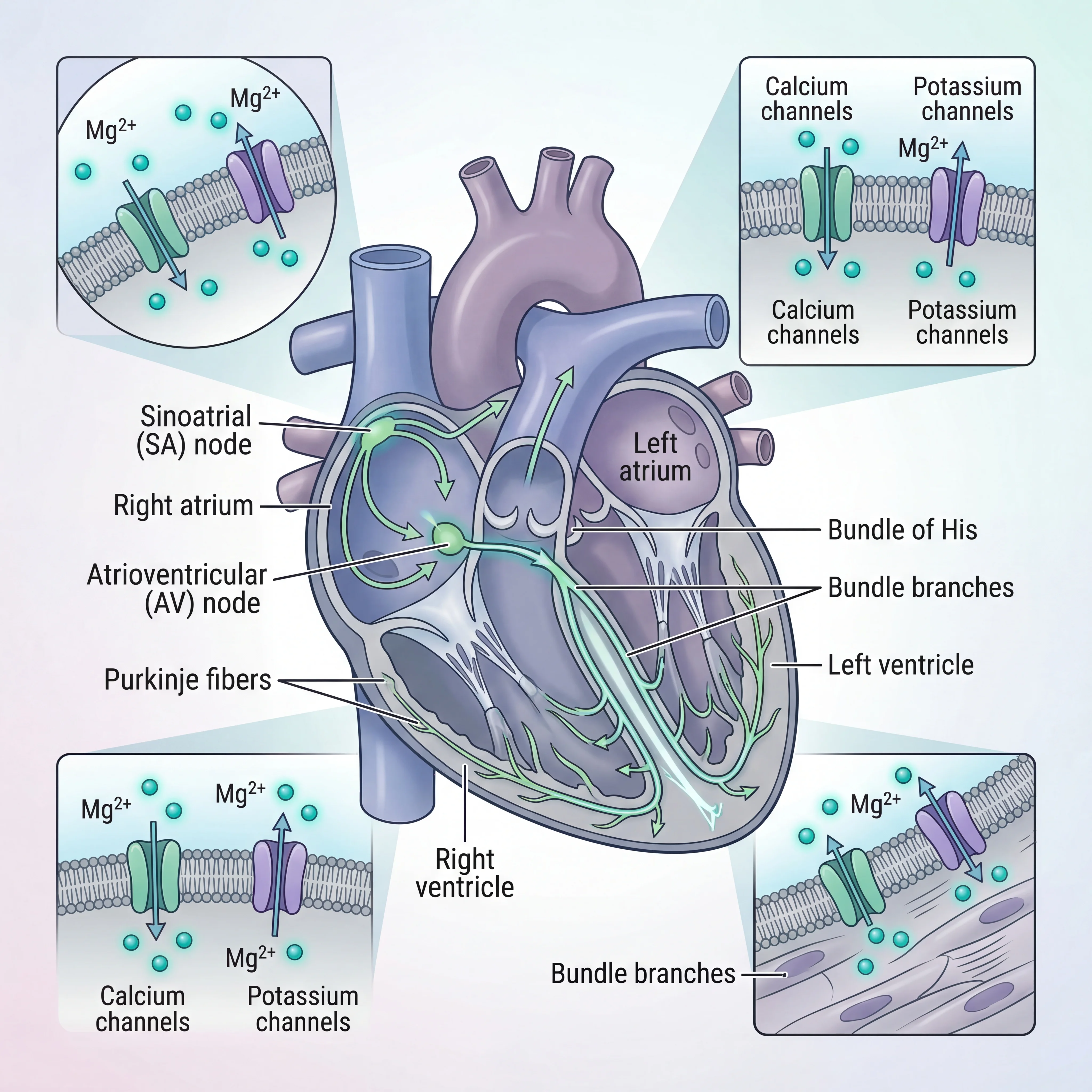
Every single heartbeat depends on a precisely timed electrical signal. That signal travels through a small cluster of cells called the atrioventricular (AV) node, which acts as the heart's internal pacemaker. Magnesium, carrying a positive electrical charge, directly participates in this process by regulating the movement of calcium, potassium, and sodium ions across cardiac cell membranes. Without adequate magnesium, these electrical signals can misfire, skip, or race out of control.
The mineral's influence extends far beyond rhythm control. As a cofactor in more than 300 enzyme systems, magnesium governs everything from blood vessel relaxation and blood pressure regulation to energy production within cardiac muscle cells. It functions as a natural calcium channel blocker, preventing the excessive intracellular calcium buildup that can trigger coronary artery spasms and damage heart tissue during periods of reduced blood flow.
Your body contains roughly 25 grams of magnesium at any given moment, with about half stored in your bones and most of the rest distributed across soft tissues. Less than one percent circulates in your blood serum, and the body works hard to keep those levels tightly controlled between 0.75 and 0.95 millimoles per liter. This narrow range matters because even subtle drops below the threshold can set the stage for cardiovascular trouble long before a standard blood test raises any flags.
Key takeaway: Magnesium regulates your heartbeat at the cellular level by controlling ion flow through calcium, potassium, and sodium channels. It also relaxes blood vessels, reduces inflammation, and protects cardiac tissue from oxidative damage.
Not All Magnesium Is Created Equal
Walk into any supplement aisle and you will find a bewildering array of magnesium products. The differences between them are not just marketing — each form pairs elemental magnesium with a different compound, and that pairing dramatically affects how much of the mineral your body actually absorbs, where it concentrates, and what secondary benefits it provides.
Understanding these distinctions matters for heart health because the wrong form could leave you with little more than a laxative effect, while the right one could deliver magnesium exactly where your cardiovascular system needs it most.
| Magnesium Form | Bioavailability | Primary Cardiovascular Benefit | Common Side Effects |
|---|---|---|---|
| Magnesium Taurate | High | Anti-arrhythmic, blood pressure support, cardioprotective | Generally well tolerated |
| Magnesium Glycinate | High | Stress reduction, indirect heart rate support | Rare; gentle on stomach |
| Magnesium Citrate | High | General cardiovascular support, blood pressure | Loose stools at higher doses |
| Magnesium Orotate | Moderate-High | Cellular energy production in cardiac tissue | Generally well tolerated; expensive |
| Magnesium Oxide | Low (4-5%) | Minimal at typical doses due to poor absorption | Significant GI distress |
| Magnesium Chloride | High | Blood pressure support (well studied in clinical trials) | Mild GI effects possible |
| Magnesium L-Threonate | Moderate | Limited cardiovascular data; primarily brain-focused | Generally well tolerated |
The National Institutes of Health notes that forms of magnesium which dissolve well in liquid tend to have higher absorption rates, with citrate, aspartate, lactate, and chloride forms consistently outperforming magnesium oxide and sulfate in bioavailability studies. This is not a trivial distinction: magnesium oxide — one of the cheapest and most widely sold forms — delivers as little as 4 to 5 percent of its elemental magnesium to your bloodstream, meaning you would need to take dramatically more to match the absorption of a well-formulated taurate or citrate product.
Matching the Right Form to Your Heart Concern
Choosing a magnesium supplement for heart health is not a one-size-fits-all decision. The form that serves someone dealing with occasional palpitations may be entirely different from what benefits a person managing high blood pressure or recovering from cardiac surgery. Here is how to think about matching the right type to your specific concern.
For Palpitations and Irregular Heartbeat
Magnesium taurate stands out as the most promising form for rhythm-related heart concerns. The reason lies in its dual-action mechanism: you get the electrical-stabilizing effects of magnesium itself, combined with the amino acid taurine, which independently lowers elevated blood pressure, retards atherogenesis, prevents arrhythmias, and stabilizes platelets. Taurine increases systolic calcium transients in cardiac cells, giving it positive inotropic activity while simultaneously reducing the excess cytoplasmic calcium that drives arrhythmias.
Magnesium glycinate serves as a strong alternative, particularly for people whose palpitations are stress-driven. The glycine component has calming properties that can reduce the sympathetic nervous system overdrive that often triggers awareness of heart rhythm irregularities. If your palpitations tend to worsen during periods of anxiety or poor sleep, glycinate may address multiple contributing factors simultaneously.
For High Blood Pressure
Clinical trials have used a variety of magnesium forms to study blood pressure effects, but magnesium chloride and magnesium citrate appear most frequently in studies showing positive results. In multiple randomized controlled trials, magnesium chloride supplementation significantly decreased both systolic and diastolic blood pressure in hypertensive patients, including those with diabetes and metabolic syndrome.
Magnesium taurate again deserves consideration here because animal studies have demonstrated that it significantly restored blood pressure while also protecting cardiac tissue from oxidative damage. The taurine component adds its own vasodilatory properties, creating a complementary effect that neither magnesium nor taurine achieves alone.

For Post-Surgical Arrhythmia Prevention
In hospital settings, intravenous magnesium sulfate remains the standard for acute arrhythmia management and post-surgical prevention. One clinical study found that perioperative magnesium supplementation during coronary artery bypass grafting reduced postoperative atrial fibrillation from 21 percent in the control group to just 2 percent in the magnesium group. For oral supplementation following discharge, magnesium taurate or citrate would be reasonable choices to discuss with a cardiologist.
| Heart Concern | Best Magnesium Forms | Why |
|---|---|---|
| Palpitations / PVCs | Taurate, Glycinate | Dual electrical stabilization; calming properties reduce stress-triggered episodes |
| High Blood Pressure | Chloride, Citrate, Taurate | Well-studied in clinical trials; good bioavailability; complementary vasodilatory effects |
| Atrial Fibrillation | Taurate | Both magnesium and taurine independently demonstrate anti-arrhythmic properties |
| General Heart Protection | Citrate, Taurate | Broad cardiovascular support with high absorption rates |
| Post-Surgical Recovery | IV Sulfate (acute); Taurate or Citrate (maintenance) | Clinical evidence for arrhythmia prevention; good oral bioavailability for ongoing use |
What 38 Clinical Trials Reveal About Magnesium and Blood Pressure
The question of whether magnesium supplements actually lower blood pressure has been debated for decades. A landmark meta-analysis published in Hypertension — the American Heart Association's premier journal for blood pressure research — analyzed 38 randomized controlled trials involving 2,709 participants and provided the clearest picture yet.
Across all participants, magnesium supplementation reduced systolic blood pressure by 2.81 mmHg and diastolic blood pressure by 2.05 mmHg compared to placebo. Those numbers might sound modest, but the story changes dramatically when you look at specific subgroups.
Critical finding: Hypertensive individuals already taking blood pressure medication saw systolic reductions of 7.68 mmHg when they added magnesium — nearly three times the overall average. People with confirmed hypomagnesemia experienced systolic drops of 5.97 mmHg and diastolic drops of 4.75 mmHg.
The median dose across studies was 365 mg of elemental magnesium per day, with interventions lasting a median of 12 weeks. One surprising finding: the researchers found no clear dose-response relationship, meaning higher doses did not automatically produce greater blood pressure reductions. This suggests that correcting an underlying deficiency matters more than flooding the body with excess magnesium.
For normotensive individuals — those with already-normal blood pressure — the effect did not reach statistical significance. This is actually reassuring: magnesium appears to lower blood pressure when it is pathologically elevated without dropping it dangerously low in healthy people. The mechanism likely involves magnesium's ability to reduce vascular tone, inhibit the renin-angiotensin-aldosterone system, and increase nitric oxide release — processes that are most impactful when blood vessels are already constricted.
For those interested in other evidence-based strategies for improving blood flow and vascular function, dietary nitric oxide boosters offer a complementary approach that works through similar vasodilatory pathways.
| Population | Systolic BP Change | Diastolic BP Change | Significance |
|---|---|---|---|
| All participants (pooled) | -2.81 mmHg | -2.05 mmHg | Significant (P<0.05) |
| Hypertensive on BP meds | -7.68 mmHg | -2.96 mmHg | Significant (P<0.05) |
| Hypomagnesemia confirmed | -5.97 mmHg | -4.75 mmHg | Significant (P<0.05) |
| Normotensive individuals | Not significant | Not significant | P>0.05 |
The Silent Deficiency Driving Heart Rhythm Problems
Nearly half of Americans — roughly 48 percent — fail to meet the recommended daily intake of magnesium, according to data cited by dietitians at Keck Medicine of USC. Yet most of these people will never know they are deficient, because standard blood tests measure serum magnesium, which represents less than one percent of the body's total magnesium stores. You can have dangerously depleted tissue levels while your bloodwork appears perfectly normal.
This testing gap creates a troubling scenario for heart health. Magnesium deficiency often manifests first as subtle electrical disturbances in the heart — occasional skipped beats, a fluttering sensation in the chest, or a heart rate that feels too fast or too slow. Because these symptoms overlap with dozens of other conditions, the underlying mineral deficiency often goes undiagnosed for months or years.
Certain groups face disproportionately higher risk of inadequate magnesium. People with gastrointestinal conditions that impair absorption, those taking proton pump inhibitors or loop diuretics, older adults with declining kidney function, individuals with type 2 diabetes, and anyone with a history of alcohol dependence all tend toward chronically low magnesium stores. The mineral's role in modulating neuronal excitation, intracardiac conduction, and myocardial contraction means that these populations face elevated cardiovascular risk from a cause that is both preventable and treatable.
The recommended dietary allowances set by the National Academies tell a clear story about how much we need: adult men require 400 to 420 mg daily, while adult women need 310 to 320 mg. Rich dietary sources include dark leafy greens like spinach, nuts, seeds, legumes, and whole grains. The body absorbs roughly 30 to 40 percent of dietary magnesium, a rate that declines with age and certain medications.

When Supplementation Makes Sense
A whole-food diet rich in magnesium remains the foundation. But supplementation becomes worth discussing with a healthcare provider in several scenarios: confirmed or suspected hypomagnesemia, a history of cardiac arrhythmias, current use of medications known to deplete magnesium, persistent heart palpitations without an identified structural cause, or treatment-resistant hypertension.
The tolerable upper intake level for supplemental magnesium is 350 mg per day for adults, set primarily to avoid gastrointestinal side effects. This limit applies to supplements only — not to magnesium consumed through food, which carries no established upper limit. Going above 350 mg supplementally can cause diarrhea, nausea, and cramping, and in extreme cases, very high doses can paradoxically trigger the very cardiac irregularities you are trying to prevent.
Myths vs. Facts About Magnesium and Your Heart
| Myth | Fact |
|---|---|
| All magnesium supplements work the same for heart health | Forms differ dramatically in bioavailability and cardiovascular-specific benefits. Magnesium oxide, the most commonly sold form, delivers as little as 4-5% of its elemental magnesium, while citrate and taurate forms are far more absorbable. |
| Higher doses always produce better results | A meta-analysis of 38 RCTs found no dose-response relationship between magnesium intake and blood pressure reduction. Correcting a deficiency appears to matter more than taking massive doses. |
| If your blood test shows normal magnesium, you are fine | Serum magnesium reflects less than 1% of total body stores. Tissue-level depletion can exist alongside normal-appearing lab values, making standard blood tests an unreliable marker of true magnesium status. |
| Magnesium supplementation benefits everyone's blood pressure equally | Clinical evidence shows significant blood pressure reductions only in hypertensive individuals and those with confirmed hypomagnesemia. Normotensive people see no meaningful effect. |
| Magnesium can replace blood pressure medication | Magnesium may enhance the effectiveness of existing antihypertensive drugs, but it is not a substitute for prescribed medication. The greatest BP reductions were seen in people already taking BP medication who added magnesium. |
| You cannot get too much magnesium | Excessive supplemental magnesium (above 350 mg/day from supplements) can cause GI distress and, in extreme cases, may worsen cardiac irregularities. Food sources carry no established upper limit. |
One persistent misconception deserves special attention: the idea that magnesium is a proven cure for arrhythmias. While intravenous magnesium sulfate has strong clinical evidence for converting atrial fibrillation to normal sinus rhythm in acute settings, reviews of major supplementation trials report inconsistent benefits and note that there is currently no firm recommendation for routine oral magnesium supplementation except when hypomagnesemia has been proven or is strongly suspected as a contributor to cardiac arrhythmias. This does not mean supplementation is useless — it means the evidence supports targeted use rather than blanket recommendations.
Maintaining overall cardiovascular resilience involves multiple strategies beyond mineral supplementation. Practices like regular sauna bathing and ensuring adequate vitamin K2 intake for arterial health work through different but complementary mechanisms to protect the heart and blood vessels.

Frequently Asked Questions
What is the best type of magnesium for heart palpitations?
Magnesium taurate is generally considered the best form for heart palpitations because it combines the electrical-stabilizing properties of magnesium with taurine, an amino acid that independently prevents arrhythmias and stabilizes cardiac cell membranes. Magnesium glycinate is a reasonable alternative, especially when palpitations are linked to stress or anxiety, since the glycine component has calming effects on the nervous system.
How long does it take for magnesium to help with heart rhythm issues?
Most clinical trials studying magnesium and cardiovascular outcomes used intervention periods of 8 to 12 weeks before assessing results. Some people notice improvements in palpitation frequency within days to weeks of correcting a deficiency, but measurable changes in blood pressure typically require at least 4 weeks of consistent supplementation. Individual response varies based on the severity of the deficiency and overall health status.
Can magnesium supplements interact with heart medications?
Magnesium can interact with several medications commonly used in cardiovascular care. It may enhance the effects of calcium channel blockers and certain antihypertensive drugs, potentially lowering blood pressure more than expected. Loop and thiazide diuretics can increase magnesium loss through urine, potentially worsening a deficiency. Always discuss magnesium supplementation with your prescribing physician, particularly if you take digoxin, antiarrhythmic drugs, or blood pressure medications.
Is it safe to take magnesium with blood pressure medication?
In most cases, yes — and research suggests it may actually be beneficial. The largest meta-analysis on this topic found that hypertensive individuals already on blood pressure medication experienced the greatest systolic blood pressure reduction (7.68 mmHg) when they added magnesium supplementation. However, because the combined effect could potentially lower blood pressure too much, monitoring and medical supervision are important, especially when starting supplementation.
Should I take magnesium if my blood test shows normal levels?
Normal serum magnesium does not guarantee adequate tissue stores, since less than 1% of the body's magnesium circulates in blood. If you have symptoms suggestive of deficiency — persistent muscle cramps, heart palpitations, fatigue, or anxiety — supplementation may still be warranted even with normal blood levels. A healthcare provider can consider your full clinical picture, dietary intake, and medication use to determine whether supplementation makes sense for you.
Related Articles
- Nitric Oxide Foods: The Complete Guide to Eating for Better Blood Flow and Lower Blood Pressure — Discover how dietary nitrates can complement magnesium's vasodilatory effects for comprehensive cardiovascular support.
- Vitamin K2 and Arterial Calcification: Can This Overlooked Vitamin Protect Your Arteries? — Explore another mineral-dependent mechanism that influences cardiovascular health through calcium metabolism.
- Sauna Bathing for Heart Health: What 20 Years of Finnish Research Actually Proves — Learn how regular heat exposure supports the same blood pressure and vascular outcomes that magnesium targets.
- Berberine: Nature's Metformin for Blood Sugar and Weight — Understand how berberine addresses metabolic risk factors that overlap with magnesium deficiency-related cardiovascular concerns.
- Spinach Health Benefits and Nutritional Facts — One of the richest dietary sources of magnesium, spinach provides both the mineral and additional cardiovascular-protective nutrients.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.