What Are Electrolytes and Why Do They Matter?
Electrolytes are minerals that carry an electrical charge when dissolved in body fluids like blood and sweat. They include sodium, potassium, magnesium, calcium, chloride, bicarbonate, and phosphate. Every cell in your body needs these charged particles to fire nerve impulses, contract muscles, and keep your heart beating steadily.
Your body maintains electrolyte concentrations within narrow ranges. According to StatPearls clinical reference, electrolytes are "essential for basic life functioning, such as maintaining electrical neutrality in cells and generating and conducting action potentials in the nerves and muscles." Even small deviations from normal blood concentrations can trigger serious symptoms and, in severe cases, increase mortality risk.
The short version: Sodium, potassium, and magnesium work as a team. Fixing one deficiency often fails unless the others are also addressed, especially magnesium, which controls how your cells handle both potassium and calcium.
For hydration, three electrolytes do the heavy lifting. Sodium controls how much water your body retains. Potassium balances fluid inside your cells. And magnesium acts as a gatekeeper for how the other two cross cell membranes. Once you understand what each one actually does, it becomes pretty clear that a sports drink after a 20-minute walk is mostly sugar water, and a spinach salad would serve you better.
Sodium — Your Body's Fluid Regulator
Sodium is the most abundant electrolyte in your extracellular fluid, the liquid surrounding your cells. It regulates fluid volume. When sodium levels rise, your body holds onto water to dilute the concentration. When they drop, your kidneys dump water to compensate. Salty meals make you thirsty for exactly this reason. And drinking too much water without replacing sodium can actually become dangerous.
The Cleveland Clinic notes that sodium "plays a critical role in helping your cells maintain the right balance of fluid" and supports nutrient absorption in the gut. Normal blood sodium ranges from 136 to 145 mEq/L.
How Much Sodium Do You Need?
The Adequate Intake for sodium is 1,500 mg per day for adults aged 19–50, according to the National Academies Dietary Reference Intakes. The Chronic Disease Risk Reduction level is 2,300 mg — the amount most public health guidelines treat as an upper target. Most Americans consume 3,000 to 4,500 mg daily, roughly double to triple the AI.
Athletes and heavy sweaters have different needs. Sweat contains 400 to 700 mg of sodium per liter. A two-hour training session in heat can drain 2,000+ mg through sweat alone. At that point, plain water isn't enough. Replacing fluid without replacing sodium dilutes blood concentration and can cause hyponatremia.
When Sodium Goes Wrong
| Condition | Blood Level | Common Symptoms |
|---|---|---|
| Hyponatremia (low) | <135 mmol/L | Headache, nausea, confusion, muscle cramps, fatigue, seizures |
| Hypernatremia (high) | >145 mmol/L | Rapid breathing, restlessness, sleep disruption, excessive thirst |
Hyponatremia happens more often than you'd think. It can come from drinking too much water during long runs, chronic diuretic use, or prolonged vomiting and diarrhea. The Mayo Clinic lists overhydration as a major cause, which is ironic given how much we're told to "just drink more water."
Potassium — The Cellular Counterbalance
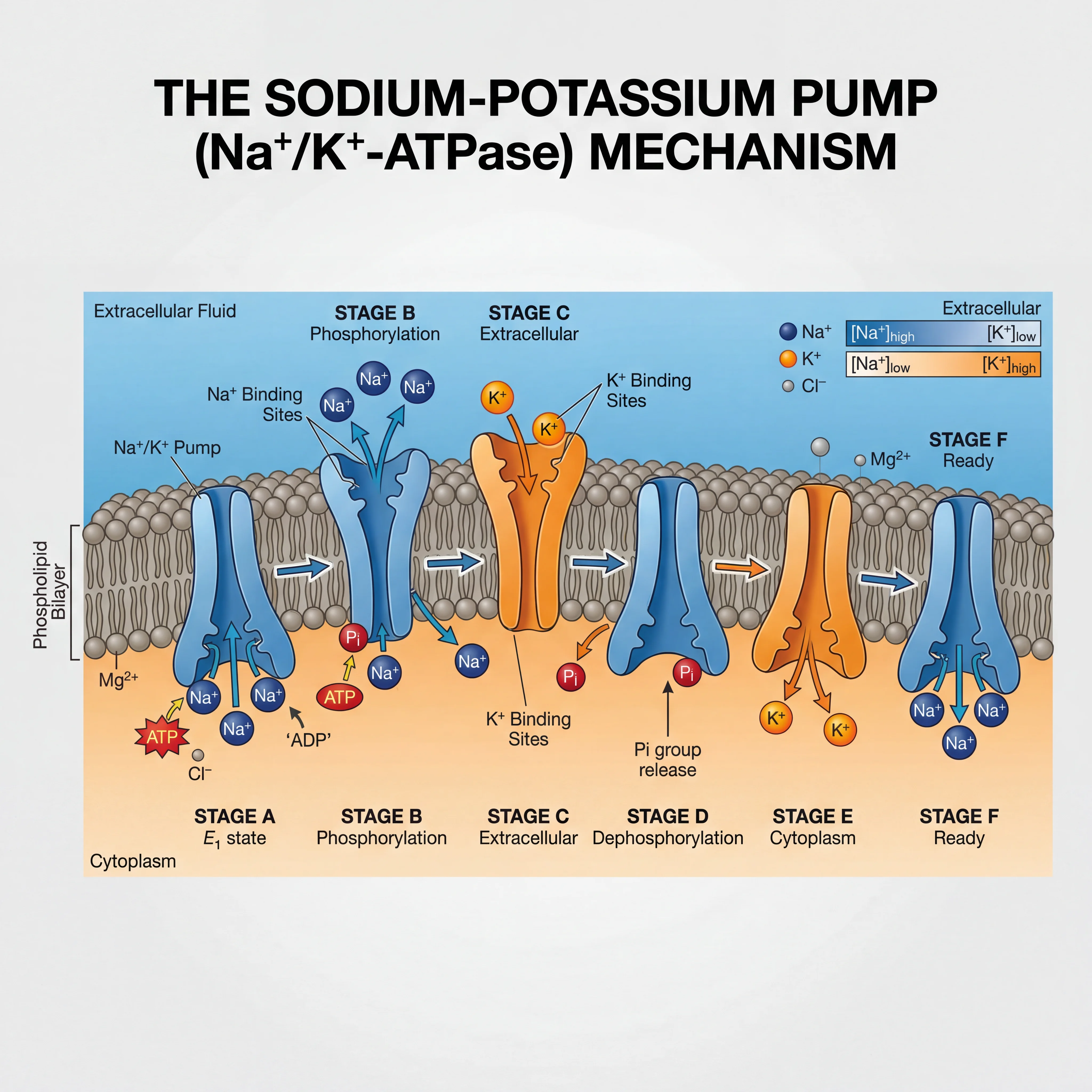
Sodium handles fluid outside your cells. Potassium handles fluid inside. About 98% of your body's potassium sits within cells, kept there by the sodium-potassium pump, an enzyme that pushes three sodium ions out of each cell for every two potassium ions it pulls in. That electrochemical gradient is what makes nerve signals fire and muscles contract, including your heart.
Potassium also pushes back against sodium when it comes to blood pressure. The NIH Office of Dietary Supplements cites meta-analyses showing that potassium supplementation (1,173 to 4,692 mg/day) drops systolic blood pressure by 4.48 mmHg and diastolic by 2.96 mmHg in people with hypertension. Higher potassium intake also tracks with a 21% lower stroke risk.
The Potassium Shortfall
The Adequate Intake for potassium is 3,400 mg/day for adult men and 2,600 mg/day for adult women. The 2020-2025 Dietary Guidelines for Americans identifies potassium as a "nutrient of public health concern" because most people fall short. Adult men average 3,016 mg and women average 2,320 mg — both below target.
About those bananas: They're the poster food for potassium, but one medium banana has only 422 mg, about 12% of the male AI. A baked potato gives you 610 mg. A cup of cooked lentils hits 731 mg. If potassium is actually your goal, legumes and starchy vegetables beat fruit every time.
Potassium and Heart Health
Potassium does more for your heart than just move fluid around. It directly affects the electrical signals that keep each heartbeat on rhythm. When potassium drops too low or spikes too high, the heart can start misfiring, which is why ERs check potassium levels in cardiac patients before almost anything else. There's a bone angle too: higher potassium reduces how much calcium you lose through urine. A 6-month trial found that potassium citrate supplementation (2,346 to 3,519 mg/day) cut calcium loss in older adults.
Hypokalemia Warning Signs
Mild potassium deficiency causes constipation, fatigue, and muscle weakness. Moderate to severe depletion (serum below 2.5 mmol/L) can trigger excessive urination, glucose intolerance, muscle paralysis, impaired breathing, and dangerous cardiac arrhythmias — particularly in people with existing heart conditions. Observational research also links chronically low potassium intake with increased type 2 diabetes risk, though controlled trials haven't fully confirmed the relationship.
Magnesium — The Most Overlooked Electrolyte

Magnesium participates in over 300 enzymatic reactions, yet a 2019 review published in the journal Medicina calls it "the forgotten electrolyte." The reason: roughly 48% of Americans consume less magnesium than their Estimated Average Requirement. And because 99% of body magnesium is stored in bones, muscles, and soft tissues — not blood — standard blood tests often miss deficiencies entirely.
This has a direct effect on hydration. Magnesium controls the ROMK channels that regulate potassium movement in and out of cells. When magnesium runs low, potassium leaks out of cells and into urine. You can take all the potassium supplements you want, but the deficiency won't resolve until magnesium comes back up. The same thing happens with calcium. If the root cause is low magnesium, calcium supplements won't fix the problem.
Magnesium RDAs
| Group | Age | RDA (mg/day) |
|---|---|---|
| Males | 19–30 | 400 |
| Males | 31+ | 420 |
| Females | 19–30 | 310 |
| Females | 31+ | 320 |
| Pregnant women | 19–30 | 350 |
| Pregnant women | 31+ | 360 |
Source: NIH Office of Dietary Supplements.
Why Deficiency Is So Common
The reasons are stacked against us. Processing strips most magnesium from food. Proton pump inhibitors (PPIs), some of the most commonly prescribed medications in the world, raise hypomagnesemia risk by a factor of 1.43. Loop and thiazide diuretics push magnesium out through the kidneys. And alcohol dependence depletes magnesium in roughly 30% of heavy drinkers.
Beyond hydration, magnesium deficiency links to elevated blood pressure, increased type 2 diabetes risk (13.5–47.7% prevalence of hypomagnesemia in diabetic populations versus 2.5–15% in non-diabetic groups), migraine frequency, and reduced bone mineral density. Only 30–40% of dietary magnesium is typically absorbed, and supplement forms vary wildly in bioavailability — magnesium citrate and chloride absorb far better than the widely sold magnesium oxide.
How Electrolyte Imbalances Affect Your Body
Mild electrolyte depletion is sneaky. It looks like general fatigue, a flat mood, or a workout that just didn't feel right. Most people blame sleep or stress. The Cleveland Clinic lists the early signs as muscle cramps, weakness, irregular heartbeat, nausea, and numbness in your hands or feet.
The tricky part is that these minerals are interdependent. You can't fix potassium without adequate magnesium. You can't hydrate by drinking water alone if sodium is depleted. And piling on sodium without enough potassium raises blood pressure. They work as a system. Treat one in isolation and you'll probably miss the actual problem.
| Electrolyte | Normal Range | Low Symptoms | High Symptoms |
|---|---|---|---|
| Sodium | 136–145 mEq/L | Headache, confusion, nausea, seizures | Thirst, restlessness, rapid breathing |
| Potassium | 3.5–5.0 mEq/L | Fatigue, cramps, constipation, arrhythmias | Muscle weakness, tingling, cardiac arrest |
| Magnesium | 1.7–2.2 mg/dL | Tremors, cramps, arrhythmias, numbness | Nausea, low blood pressure, cardiac arrest |
Who Faces the Highest Risk?
Endurance athletes lose all three electrolytes through prolonged sweating. Older adults face declining absorption efficiency and increased medication use (diuretics, PPIs). People with gastrointestinal conditions — chronic diarrhea, Crohn's disease, celiac disease — lose electrolytes through malabsorption. And anyone following a highly restrictive diet may cut out key electrolyte sources without realizing it.
Diabetic populations deserve particular mention. The Medicina review reports that 13.5% to 47.7% of people with type 2 diabetes have hypomagnesemia — compared to just 2.5% to 15% in non-diabetic populations. Insulin resistance and magnesium depletion appear to reinforce each other, creating a cycle where low magnesium worsens glucose control and poor glucose control increases magnesium loss through urine.
Best Natural Food Sources for Each Electrolyte

Before you buy another tub of electrolyte powder, know that whole foods deliver these minerals alongside cofactors that actually improve absorption: fiber, vitamins, and other minerals that work in concert. The research on whole-food nutrition keeps pointing in the same direction: food first, supplements second.
Top Potassium Sources
| Food | Serving | Potassium (mg) |
|---|---|---|
| Dried apricots | ½ cup | 755 |
| Cooked lentils | 1 cup | 731 |
| Baked potato (with skin) | 1 medium | 610 |
| Kidney beans (canned) | 1 cup | 607 |
| Orange juice | 1 cup | 496 |
| Banana | 1 medium | 422 |
| Low-fat milk | 1 cup | 366 |
Source: NIH Office of Dietary Supplements, Potassium Fact Sheet.
Top Magnesium Sources
| Food | Serving | Magnesium (mg) |
|---|---|---|
| Pumpkin seeds | 1 oz | 156 |
| Chia seeds | 1 oz | 111 |
| Almonds (dry roasted) | 1 oz | 80 |
| Spinach (boiled) | ½ cup | 78 |
| Cashews | 1 oz | 74 |
| Black beans (cooked) | ½ cup | 60 |
| Brown rice (cooked) | ½ cup | 42 |
Source: NIH Office of Dietary Supplements, Magnesium Fact Sheet.
Sodium Sources — A Different Problem
Unlike potassium and magnesium, sodium deficiency from diet alone is rare. Most people get far more than needed from processed foods, restaurant meals, and added table salt. For athletes losing significant sodium through sweat, adding a pinch of salt (about 575 mg sodium per quarter teaspoon) to water or meals can bridge the gap without relying on sugary sports drinks.
Building an Electrolyte-Rich Plate
A practical approach to covering all three electrolytes through food: pair a leafy green (spinach or Swiss chard for magnesium) with a starchy vegetable (potato or sweet potato for potassium) and season with salt to taste. Add a handful of pumpkin seeds or almonds as a snack. One cup of cooked spinach alone delivers 157 mg of magnesium and 839 mg of potassium — nearly 40% of the female magnesium RDA and a quarter of the potassium AI in a single serving.
Common Electrolyte Myths the Science Doesn't Support

Marketing has shaped what people believe about electrolytes more than clinical research ever did. A few common claims that don't hold up.
Myth: You Need Electrolyte Drinks After Every Workout
For exercise lasting under one hour at moderate intensity, water is sufficient. Sports dietitian Kate Patton of the Cleveland Clinic states plainly: "H2O will get the job done in most cases." Electrolyte drinks become relevant during sessions exceeding 60 minutes, high-intensity training, hot weather, or for naturally heavy sweaters. The American Academy of Pediatrics discourages routine sports drink consumption for children.
Myth: Bananas Are the Best Source of Potassium
At 422 mg per fruit, bananas are a decent source — but hardly the best. Dried apricots deliver nearly double the potassium per serving (755 mg per half cup). A baked potato with skin provides 610 mg. Lentils hit 731 mg per cup. Bananas earned their reputation through marketing, not nutritional superiority.
Myth: More Electrolytes Are Always Better
Excess intake carries its own risks. Hyperkalemia (elevated potassium) can cause cardiac arrest. Hypernatremia (elevated sodium) drives dangerous fluid retention and hypertension. Hypermagnesemia, while rare, causes nausea, low blood pressure, and cardiac complications. The body regulates electrolytes within tight ranges for a reason — flooding the system disrupts that balance as much as depletion does.
Myth: You Can Correct One Electrolyte Without Affecting the Others
These minerals are interdependent. Research published in Medicina confirms that low potassium won't respond to potassium supplements until magnesium is back to normal. The magnesium-dependent ROMK channels control potassium retention. Same story with calcium: if the root issue is magnesium, loading up on calcium won't move the needle. You have to treat the system, not individual parts.
Myth: Salt Is Always Bad for You
"Salt is bad" is too simple. Most desk workers eat way too much sodium, yes. But athletes and people working outside in heat may genuinely need to add salt to their food or water. Sodium helps your gut absorb water and keeps blood volume up during hard effort. The problem is overconsumption in people who don't sweat much, not sodium itself.
Frequently Asked Questions
How do I know if I have an electrolyte imbalance?
Common signs include persistent muscle cramps, unusual fatigue, irregular heartbeat, tingling in hands or feet, and frequent headaches. A basic metabolic panel blood test measures sodium, potassium, and other electrolyte levels. If you experience these symptoms regularly — especially after exercise, illness, or medication changes — ask your healthcare provider about testing.
Can drinking too much water cause electrolyte problems?
Yes. Excessive water intake without electrolyte replacement dilutes blood sodium, causing hyponatremia. This is most common during endurance events when athletes drink large volumes of plain water over several hours. Symptoms range from headache and nausea to confusion and seizures. The solution is matching water intake to sweat losses and including sodium when drinking large volumes.
Should I take electrolyte supplements every day?
Most people who eat a varied diet rich in vegetables, fruits, legumes, nuts, and seeds get adequate electrolytes from food alone. Daily supplementation makes sense for specific populations: endurance athletes, people on diuretic medications, those with chronic digestive conditions, or anyone whose doctor has identified a documented deficiency. Routine supplementation without a clear need can push levels too high.
What is the best form of magnesium supplement?
Magnesium citrate, chloride, and lactate have the highest bioavailability at roughly 12% absorption. Magnesium glycinate is well-tolerated and popular for sleep support. Magnesium oxide, despite containing 60% elemental magnesium, absorbs at only 4% — making it a poor choice for correcting deficiency. The NIH recommends choosing forms based on absorption rate rather than elemental content.
Are coconut water or pickle juice good electrolyte sources?
Coconut water contains moderate potassium (about 600 mg per cup) but relatively little sodium (roughly 250 mg), making it a partial solution at best. Pickle juice provides sodium and has some evidence supporting cramp relief, though the mechanism may involve nerve reflexes rather than electrolyte replenishment. Neither replaces a balanced approach to mineral intake through whole foods and targeted supplementation when needed.
Related Articles
- Magnesium Types Explained (Glycinate, Citrate, Threonate) — Which to Take and When — A deeper look at how different magnesium forms compare for absorption, sleep, and specific health goals.
- Top 10 Health Benefits of Drinking Water — Why water matters for everything from digestion to joint health, and how much you actually need daily.
- Nitric Oxide Foods: The Complete Guide to Eating for Better Blood Flow — How dietary nitrates from beets, leafy greens, and other foods support cardiovascular function and blood pressure.
- Evidence-Based Nutrition: What the Latest Research Actually Shows — Cutting through nutrition confusion with research-backed guidance on macros, micros, and meal timing.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.











