TL;DR: Yoga has moved well beyond the wellness trend category. A 2025 umbrella review identified improvements across 12 chronic disease outcomes, the American College of Physicians now recommends it as a first-line treatment for chronic low back pain, and controlled trials show meaningful reductions in blood pressure and stress hormones. The evidence is strongest for musculoskeletal pain, hypertension, and psychological stress — thinner for clinical anxiety and depression disorders. If you're physically able to practice safely, the risk-benefit ratio is hard to argue with.
Yoga has been practiced for thousands of years, but the scientific case for it is relatively new — and more interesting than the wellness industry usually conveys. For a long time, Western medicine treated yoga as a vague feel-good activity: probably harmless, hard to study rigorously. That changed as researchers started running proper randomized controlled trials, and then systematic reviews, and now umbrella reviews that synthesize dozens of studies at once.
What's emerged is a nuanced picture. For some outcomes — chronic low back pain, blood pressure, psychological stress — the evidence is genuinely solid. For others — clinical depression, anxiety disorders, diabetes management — the data is more preliminary, with smaller samples and mixed results. This guide tries to be straight about both, because the health claims attached to yoga have gotten ahead of the research in some areas while the research in others has outpaced public awareness.
A 2025 umbrella review in BMC Complementary Medicine and Therapies synthesized existing meta-analyses and found yoga practice improved outcomes across 12 chronic disease categories — not in anecdotal case reports, but in aggregated controlled trial data. That breadth of effect is unusual for a single lifestyle intervention.
What yoga actually does to the body
Yoga isn't a single thing. The term covers a family of practices with different physical demands — Iyengar focuses on alignment and holds, Ashtanga is aerobically demanding, restorative yoga involves almost no muscular effort. The research tends to cluster around Hatha yoga, a moderate-intensity style that combines physical postures (asanas), breathing exercises (pranayama), and meditation or relaxation.
At the physiological level, yoga works through several mechanisms simultaneously. The physical postures build and lengthen muscle, improve joint range of motion, and challenge proprioception and balance. The breathing component activates the parasympathetic nervous system — slowing heart rate, lowering cortisol, and shifting the body out of sympathetic (fight-or-flight) dominance. The meditative component recruits the prefrontal cortex and down-regulates the amygdala's stress response over time.
According to the National Center for Complementary and Integrative Health, yoga supports stress management, mental health, mindfulness, weight maintenance, healthy eating, sleep quality, and balance. That's a wide list, but each mechanism is traceable to the specific components of a yoga practice — the combination of movement, breath, and attentional focus that distinguishes yoga from simple stretching or conventional exercise.
| Yoga component | Primary physiological mechanism | Downstream benefit |
|---|---|---|
| Physical postures (asanas) | Muscle activation, eccentric loading, range-of-motion work | Strength, flexibility, balance, injury resilience |
| Breathing exercises (pranayama) | Parasympathetic nervous system activation via vagus nerve | Lower heart rate, reduced cortisol, blood pressure regulation |
| Meditation / mindfulness | Prefrontal cortex engagement, amygdala down-regulation | Stress reduction, improved emotional regulation, better sleep |
| Relaxation practices (Savasana, yoga nidra) | HPA axis modulation, cortisol lowering | Reduced allostatic load, improved recovery |
One key distinction: yoga is not aerobic exercise in the traditional sense. A Hatha class burns fewer calories than a jog and doesn't produce the same cardiovascular adaptations as sustained cardio. But it produces adaptations cardio doesn't — flexibility, balance, stress response, parasympathetic tone. The comparison isn't yoga versus exercise; it's two different training modes with overlapping but distinct effects.

Cardiovascular health and blood pressure
Of all yoga's proposed benefits, the cardiovascular evidence is some of the most compelling — and most specific. We're not talking about vague improvements in "heart health." Controlled trials show measurable reductions in blood pressure, and the mechanisms are reasonably well understood.
A study highlighted by Johns Hopkins Medicine found that yoga practitioners experienced a 10-point drop in systolic blood pressure, compared to just 4 points for those who only did stretching. That 6-point difference is meaningful — not pharmacological-magnitude, but in the range where it shifts someone from borderline high to normal. For context, the DASH diet, one of the most rigorously studied blood pressure interventions, produces reductions of around 8 to 11 mmHg in clinical trials. Yoga's effect is in the same neighborhood.
The mechanism involves both the physical and breathing components. Slow, controlled breathing activates the baroreceptor reflex and increases heart rate variability, which signals cardiovascular system flexibility and health. Yoga's postures and holds also reduce arterial stiffness over time — a factor that contributes to elevated blood pressure independently of plaque or vessel narrowing.
Beyond blood pressure, the Johns Hopkins cardiovascular review notes that yoga may help reduce levels of LDL cholesterol, total cholesterol, and inflammation markers in some populations, though this evidence is less consistent. The anti-inflammatory pathway is plausible — chronic stress drives systemic inflammation, yoga demonstrably reduces stress markers, and chronic inflammation underlies most cardiovascular disease. But the direct lipid-lowering evidence is thinner than the blood pressure data and shouldn't be overstated.
| Cardiovascular marker | Effect | Evidence strength |
|---|---|---|
| Systolic blood pressure | Decreases ~5-10 mmHg | Moderate-Strong |
| Diastolic blood pressure | Decreases ~2-6 mmHg | Moderate |
| Heart rate variability | Increases | Moderate |
| Arterial stiffness | Decreases | Preliminary |
| LDL / total cholesterol | Mixed results | Weak-Moderate |
| Resting heart rate | Decreases slightly | Moderate |
For people at elevated cardiovascular risk — those with hypertension, metabolic syndrome, or high baseline stress — yoga may offer a practical adjunct to medication and dietary changes rather than a replacement. The Harvard Health analysis of yoga and blood pressure recommends it as a complementary strategy, particularly when paired with reduced sodium intake and regular aerobic exercise. Worth noting: if you're already on blood pressure medication, don't substitute yoga for it — add it, and monitor your numbers.
Pain, flexibility, and musculoskeletal function
This is where the research is clearest. Yoga for chronic low back pain now has enough trial data that the American College of Physicians includes it in its clinical guidelines as a first-line treatment — meaning doctors are encouraged to recommend yoga before moving to medication for most cases of chronic low back pain.
A systematic review in the Cochrane Database, covering randomized controlled trials on yoga for chronic low back pain, found moderate-certainty evidence that yoga produces meaningful improvements in back-related function and pain intensity compared to no exercise. The effects were particularly consistent at 3 to 6 months of practice. Importantly, these weren't just subjective pain ratings — functional disability scores improved as well, meaning participants could do more with less difficulty.
A 2024 randomized controlled trial tested 12 weeks of virtual yoga instruction against a wait-list control group in adults with chronic low back pain. The yoga group showed significantly greater improvements in pain intensity, disability, and pain catastrophizing — a cognitive pattern that amplifies pain perception — compared to those waiting for treatment. The virtual delivery also matters: it removes the barrier of finding a local studio, and the effects were clinically meaningful despite the remote format.
The NCCIH's evidence review on yoga and pain extends the findings beyond back pain to include neck pain, knee osteoarthritis, headaches, and fibromyalgia — though with decreasing confidence as you move down that list. The back pain evidence is the most robust; for fibromyalgia, for example, we're looking at smaller trials with shorter follow-up periods.

On the flexibility and strength side, the evidence is straightforwardly positive. Meta-analyses show that regular yoga practice produces moderate improvements in hamstring and lower-body flexibility, spinal flexibility, shoulder mobility, and balance. The strength effects are real but smaller — yoga builds the kind of functional bodyweight strength that matters for daily movement, not the hypertrophic muscle growth from progressive resistance training. These two types of training complement each other; they're not competing.
Balance is where yoga may have its strongest case among older adults. Falls are a leading cause of injury and death in people over 65, and the balance and proprioception training yoga provides — particularly standing poses that challenge single-leg stability — directly addresses that risk. Johns Hopkins notes that yoga's regular practice of standing poses, balance challenges, and body-awareness training meaningfully improves older adults' fall risk profiles.
Mental health and stress regulation
The stress-reduction evidence for yoga is consistent across studies, and the mechanisms are concrete. Yoga practice reduces cortisol — the primary stress hormone — measurably after even a single session. Over weeks and months of regular practice, it shifts baseline cortisol patterns, lowers perceived stress scores, and improves self-reported wellbeing. This isn't a placebo story; cortisol is a biomarker you can measure in blood and saliva.
According to Harvard Medical School's review, yoga's mental health benefits operate through two pathways: the biological (cortisol reduction, inflammation markers, autonomic nervous system balance) and the behavioral (mindfulness, social connection in group classes, reduced avoidance of physical sensations). Both matter. People who practice yoga regularly report lower perceived stress and higher sense of agency over their health — which itself has downstream effects on behavior and health outcomes.
For general anxiety and stress, the evidence is strong. For clinically diagnosed anxiety disorders or major depressive disorder, the picture is more cautious. Harvard's mental health review notes that yoga shows promise as an adjunct treatment for these conditions but isn't yet established as a standalone treatment for clinical disorders. The studies tend to be smaller, less rigorously controlled, and have shorter follow-up periods. People with clinical-level anxiety or depression should treat yoga as a complement to evidence-based care, not a substitute.
One specific mechanism worth noting: yoga's emphasis on controlled breathing (particularly slow exhales) directly activates the parasympathetic nervous system via the vagus nerve. This is the same pathway that some adaptogenic supplements like ashwagandha target through HPA axis modulation — except yoga does it mechanically, without ingesting anything. The combination of regular yoga and an evidence-based adaptogen like ashwagandha KSM-66 might theoretically stack, though the research on combined approaches is thin.
Sleep quality also improves with regular yoga practice, particularly in older adults and people dealing with chronic conditions. The relaxation and cortisol-lowering effects translate into faster sleep onset and fewer awakenings. A meta-analysis of yoga and sleep quality found significant improvements in both subjective sleep quality and insomnia severity across several populations — cancer survivors, women during menopause, older adults with chronic conditions.
| Mental health outcome | Evidence quality |
|---|---|
| Perceived stress reduction | Strong |
| Cortisol reduction (biomarker) | Moderate-Strong |
| Sleep quality improvement | Moderate |
| General anxiety symptoms | Moderate |
| Clinical anxiety disorders | Preliminary |
| Major depressive disorder | Preliminary (adjunct only) |
| PTSD symptoms | Emerging |
Brain health and cognitive function
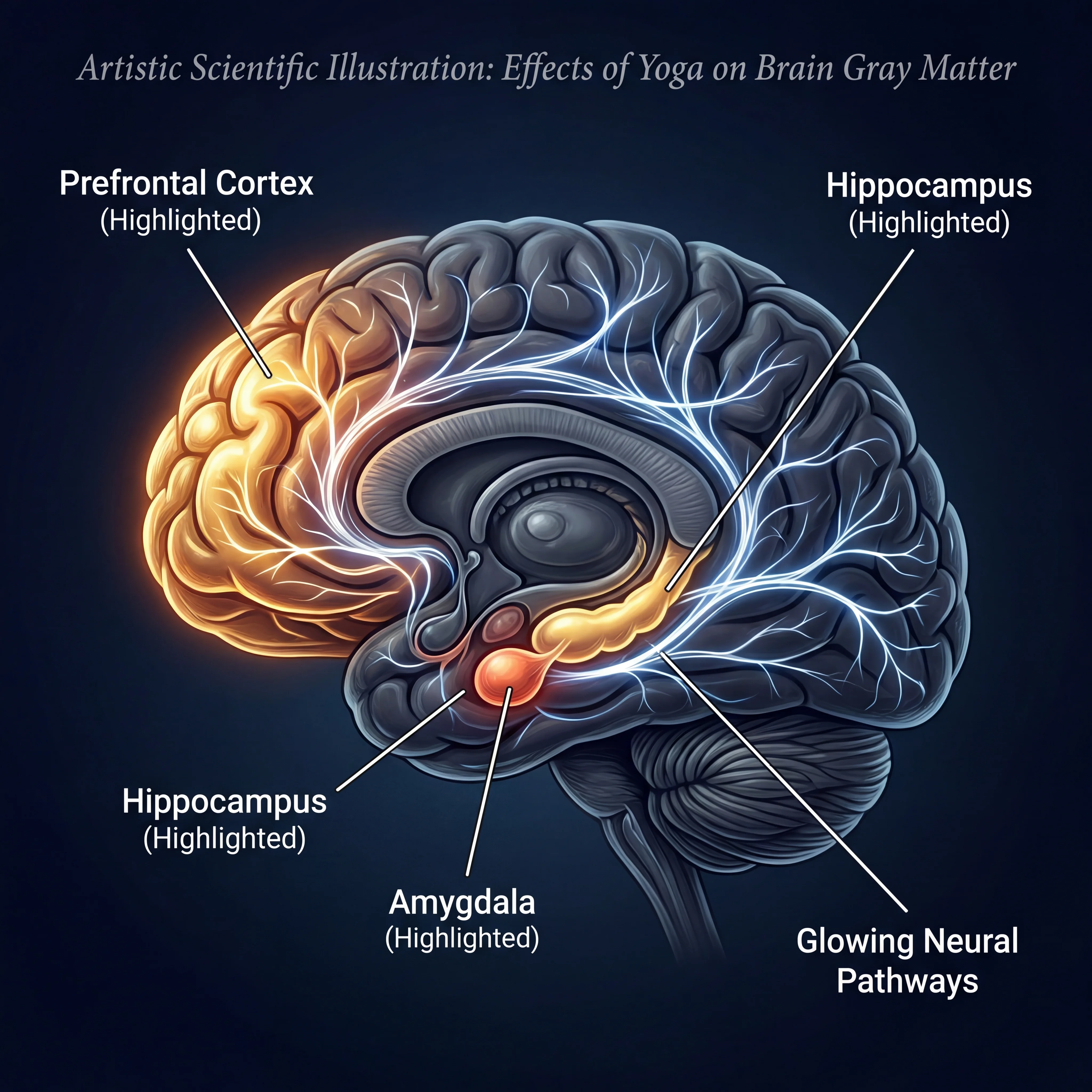
This is perhaps the most surprising area in yoga research. A systematic review in Brain Plasticity examined neuroimaging and cognitive studies and found that regular yoga practice is associated with larger gray matter volume in regions involved in attention, interoception, and emotional regulation — including the prefrontal cortex, hippocampus, and insula.
The hippocampus stands out. It shrinks with age, is disproportionately damaged in Alzheimer's disease, and is critical for memory consolidation. Aerobic exercise increases hippocampal volume via BDNF upregulation — yoga may produce a similar effect through a different route: chronic cortisol directly damages hippocampal tissue, and yoga demonstrably lowers cortisol over time. The same review found that yoga affects the default mode network (DMN) — the brain network linked to rumination and mind-wandering. Overactivation of the DMN is associated with anxiety and depression; yoga appears to reduce it and strengthen intentional attentional control.
Long-term cognitive protection from yoga remains an open question — most studies are short-term. The cognitive case sits alongside other lifestyle interventions: aerobic exercise, quality sleep, social engagement. The Mediterranean diet, which supports brain health through overlapping anti-inflammatory mechanisms, makes a natural pairing.
Chronic disease management
The 2025 umbrella review in BMC Complementary Medicine found consistent positive signals for yoga as an adjunct management strategy across multiple chronic conditions. The key word is adjunct — yoga isn't replacing medication, but it's a meaningful addition that improves outcomes in populations who practice regularly.
Hypertension. Multiple meta-analyses show systolic reductions of 5-10 mmHg. For people in Stage 1 hypertension (130-139 mmHg), this may be sufficient to avoid or delay medication when combined with dietary changes.
Type 2 diabetes and metabolic syndrome. Yoga improves insulin sensitivity, fasting glucose, and HbA1c — likely through stress reduction (cortisol directly impairs insulin sensitivity), physical activity, and modest weight management effects. Effect sizes are modest but consistent.
COPD and asthma. Pranayama (breathing exercises) improves respiratory muscle strength, exercise tolerance, and quality of life in COPD patients. Asthma data is less consistent — some trials show symptom improvement, others don't, and methodological quality varies widely.
Arthritis. Johns Hopkins notes that gentle yoga improves physical function and psychological wellbeing in arthritis patients. The key is style selection — vigorous or extreme-range poses can worsen joint symptoms while gentle, prop-supported styles help.
Parkinson's disease. Emerging trial data shows yoga improves motor function, balance, and quality of life in people with Parkinson's — particularly meaningful given progressive balance impairment and fall risk in this population.
Yoga integrates well with other evidence-based lifestyle changes. Adequate magnesium intake, for example, supports the same nervous system pathways yoga activates. Combined approaches aren't well-studied, but the mechanisms are complementary.
| Chronic condition | Evidence for yoga (adjunct) |
|---|---|
| Hypertension | Moderate-Strong |
| Chronic low back pain | Strong |
| Type 2 diabetes / metabolic syndrome | Moderate |
| COPD | Moderate |
| Arthritis | Moderate |
| Asthma | Preliminary-Moderate |
| Parkinson's disease | Emerging |
| Cancer (supportive care) | Moderate |
Getting started safely
Yoga's adverse event rate is low, but not zero. Most injuries involve the lower back, shoulders, neck, and knees — nearly always from pushing into positions the body isn't prepared for, or from inadequate instruction. Beginners who start with certified instructors and beginner classes have very low injury risk; problems arise when people skip fundamentals and rush to advanced postures.
A few populations need specific caution:
Osteoporosis. Spinal flexion postures can stress vertebrae with significant bone loss. Yoga is generally beneficial for bone health through weight-bearing poses, but look for instructors with osteoporosis-specific experience.
Glaucoma. Inversions temporarily raise intraocular pressure. Avoid full inversions and consult your ophthalmologist.
Pregnancy. Many yoga styles are fine during pregnancy, but hot yoga and abdominal compressions should be avoided. Certified prenatal instructors are the safest option.
Recent surgery or acute injuries. Wait for medical clearance before resuming practice after surgery, fractures, or disc injuries. Physical therapists increasingly incorporate yoga-derived movements into rehab — a useful bridge back to independent practice.
For most healthy adults, starting with a beginner Hatha or gentle class two to three times per week produces measurable results within 8 to 12 weeks. That's the timeframe most research uses, and it matches clinical experience. Shorter, consistent sessions outperform occasional intensive practice in essentially every outcome studied.

Style selection also matters for what you're trying to achieve. For stress reduction and mental health, slower styles with breathing emphasis (Hatha, Yin, restorative) are better studied. For cardiovascular effects and calorie expenditure, more vigorous styles (Vinyasa, Ashtanga, power yoga) are more appropriate. For chronic pain and rehabilitation, Iyengar yoga's emphasis on supported alignment and props has the most clinical trial data behind it specifically.
Frequently Asked Questions
How many times per week do you need to practice yoga to see health benefits?
Most clinical trials used two to four sessions per week, each 45 to 90 minutes, over 8 to 12 weeks. Two sessions per week appears sufficient for measurable cortisol reduction and flexibility improvements. Daily practice isn't necessary and may increase injury risk in beginners who haven't yet developed body awareness.
Is yoga effective for weight loss?
Yoga burns calories but isn't high-expenditure compared to running or resistance training — roughly 180-350 calories per hour for a moderate Hatha session. Its weight management benefit is mostly indirect: stress reduction (cortisol drives abdominal fat accumulation), improved mindful eating, and better sleep. The NIH positions yoga as a weight management support tool, not a primary weight loss intervention.
Can yoga replace conventional exercise?
Not entirely. Yoga doesn't produce the same aerobic adaptations as sustained cardio, and it doesn't build muscle mass the way progressive resistance training does. Where yoga excels — flexibility, balance, parasympathetic tone, stress response — conventional exercise largely doesn't. They're complementary, not interchangeable. Include yoga alongside other movement rather than treating it as a substitute for aerobic or strength training.
Does the research apply equally to all yoga styles?
No, and this matters when reading yoga research. Studies on Iyengar yoga can't be assumed to apply to Ashtanga — these styles share a name but differ substantially in physical demand, pacing, and mental focus. The most studied styles in clinical research are Hatha (moderate pace, accessible) and Iyengar (alignment-focused, props used — well-studied for back pain specifically). When you see a headline claiming "yoga reduces blood pressure," check which style was used. It's almost always gentle or moderate yoga, not a vigorous power class. Results are more transferable across similar-intensity styles than across very different intensity levels.
Related Articles
- Natural Blood Pressure Reduction: What the Evidence Actually Supports
- Inflammation and Chronic Disease: A Guide to Anti-Inflammatory Living
- Ashwagandha KSM-66 vs Sensoril: Cortisol, Thyroid, and What to Take
- Magnesium Types Explained: Threonate, Glycinate, Taurate — Which to Take
- Mediterranean Diet, Brain Health, and Longevity
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.


