The Wandering Nerve That Controls Your Heartbeat
There is a nerve that starts at the base of your skull, threads past your throat, wraps around your heart, and continues all the way down to your large intestine. The Romans called it "vagus" — the wanderer — and it earned that name by taking the longest, most winding path of any cranial nerve in the human body.
Your vagus nerve is actually a pair of nerves, left and right, and together they carry roughly 75 percent of all parasympathetic nerve fibers in your body. That makes them the primary communication cable between your brain and nearly every organ you own. But their relationship with the heart is especially intimate.
Every time your heart slows down after a sprint to catch the bus, every time your blood pressure eases as you fall asleep, every time your heart rhythm steadies during a calm conversation — your vagus nerve is doing that work. It acts as a biological brake pedal, counterbalancing the accelerator of your sympathetic "fight-or-flight" system. Without it, your heart would beat at roughly 105 beats per minute around the clock, which is the intrinsic firing rate of your cardiac pacemaker cells when left unchecked.
And here is where it gets interesting: the strength of that vagal connection may not just reflect how fit you are. It may determine how fast your heart ages.
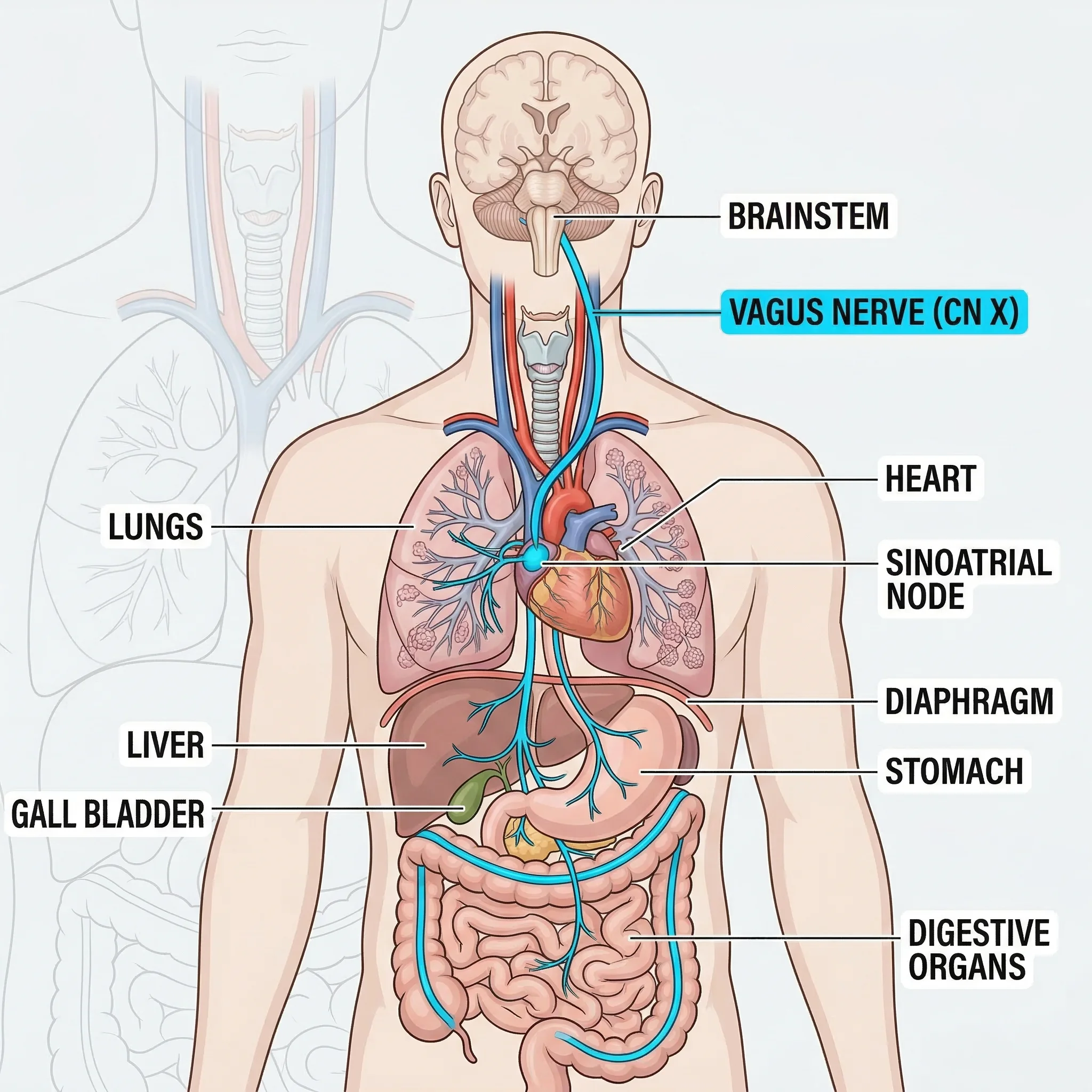
Why Doctors Are Calling Vagal Tone the New Vital Sign
Your doctor checks your blood pressure, heart rate, and temperature. But there is a measurement that an increasing number of researchers believe should join that list: vagal tone, most commonly assessed through heart rate variability.
Heart rate variability, or HRV, measures the tiny fluctuations in timing between consecutive heartbeats. A healthy heart does not beat like a metronome. Instead, the intervals between beats constantly shift — speeding up slightly when you inhale, slowing down when you exhale. This variability is driven primarily by vagal input to the sinoatrial node, your heart's natural pacemaker.
Higher HRV generally reflects stronger vagal tone and a more flexible autonomic nervous system. Lower HRV means the system has lost some of its ability to adapt. What that looks like in practice is sobering.
A 2024 narrative review published in Frontiers in Physiology compiled evidence showing that reduced HRV correlates with increased mortality risk after heart attacks, strokes, bypass operations, and in patients with heart failure or chronic obstructive pulmonary disease. The part that got my attention: people with lower HRV today have a measurably higher risk of developing hypertension within three years. Vagal tone isn't just tracking existing problems. It's forecasting future ones.
Quick Fact: Reduced heart rate variability has been shown to predict future hypertension, cardiovascular events, and even cognitive decline years before symptoms appear.
The connection extends beyond the heart entirely. A systematic review of longitudinal studies involving over 24,000 participants found that higher parasympathetic nervous system activity — the branch governed by the vagus nerve — consistently predicted better cognitive function over time. All twelve studies found the same thing: better vagal activity, better cognitive function years later. That tracks when you consider that the vagus nerve is the main physical connection in the gut-brain axis, with its fingers in inflammation, blood flow, and neural signaling all at once.
| HRV Metric | What It Measures | Clinical Significance |
|---|---|---|
| RMSSD | Beat-to-beat variation (short-term vagal activity) | Most reliable non-invasive marker of parasympathetic tone |
| SDNN | Overall variability of heart rhythm | Predicts all-cause mortality; lower values = higher risk |
| HF Power | High-frequency component (0.15-0.4 Hz) | Directly reflects vagal modulation of heart rate |
| LF/HF Ratio | Balance between sympathetic and parasympathetic | Elevated ratio suggests sympathetic dominance |
Breakthrough Research: How Losing Vagal Connection Ages Your Heart
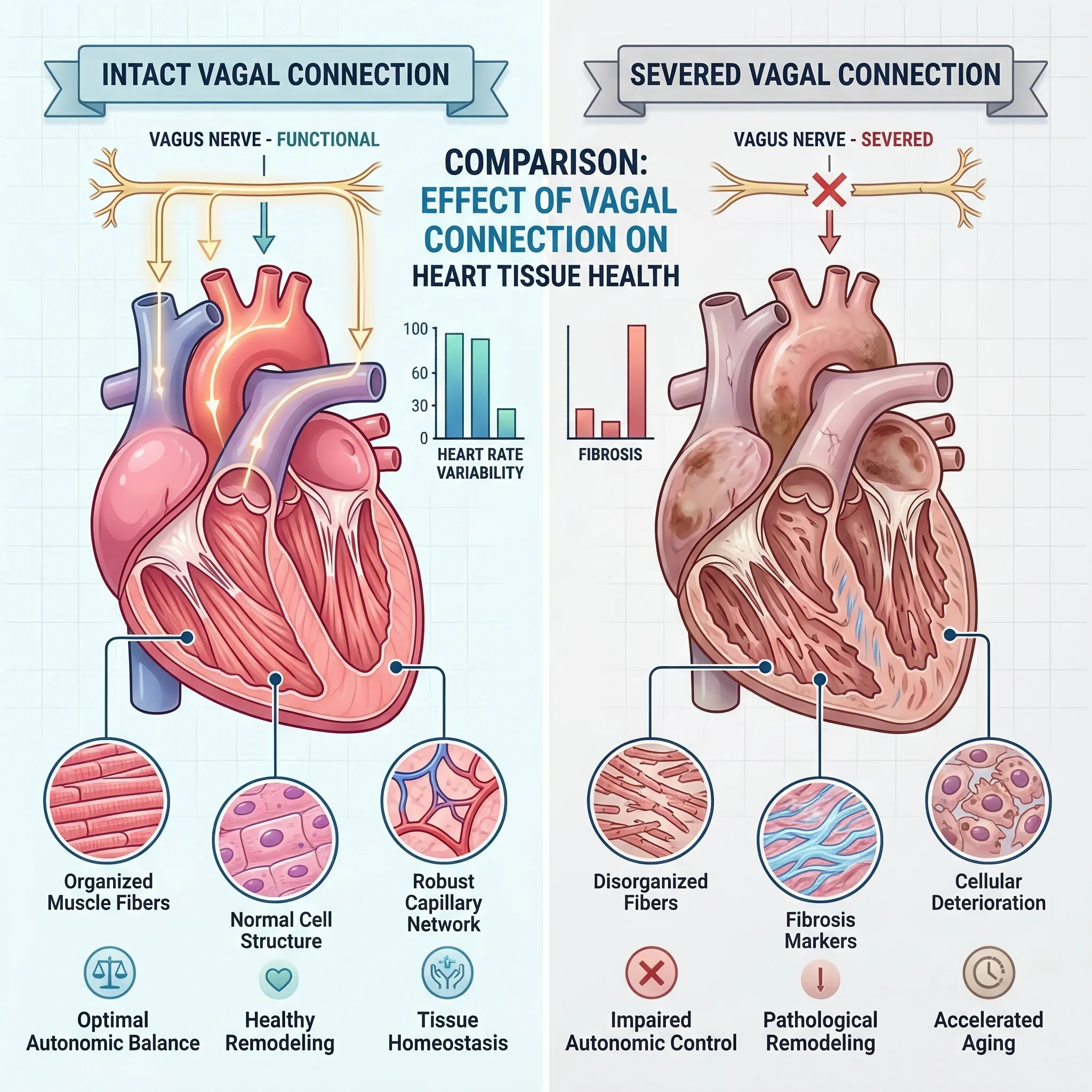
In late 2025, a team led by Professor Vincenzo Lionetti at the Sant'Anna School of Advanced Studies in Pisa published a study in Science Translational Medicine that reframed our understanding of cardiac aging. Their finding was direct: when the vagus nerve's connection to the heart is severed, the heart ages faster.
The researchers worked with a minipig model — chosen because pig cardiac anatomy closely resembles human cardiac anatomy — and surgically disconnected the right cardiac vagus nerve. The results were unambiguous. Hearts that lost their vagal connection showed accelerated cellular changes associated with aging, including deterioration of heart muscle cells and reduced pumping strength.
But the most striking part of the study was what happened when the researchers attempted to restore the connection. Using a bioabsorbable nerve conduit developed by the Biorobotics Institute at Sant'Anna, they guided the severed vagus nerve to regenerate. Even partial restoration of the nerve pathway was enough to counteract the damaging remodeling processes and preserve effective cardiac contractility.
Key Finding: "When the integrity of the connection to the vagus nerve is lost, the heart ages more rapidly," explains Professor Lionetti. Even partial reconnection reversed these aging effects.
The takeaway is blunt: the vagus nerve is not just monitoring your heart. It is actively keeping it healthy. Every moment it stays connected, it is suppressing inflammatory pathways, regulating cellular metabolism, and preserving the contractile machinery of the heart muscle. Cut that line, and the heart starts to deteriorate.
The implications extend to human medicine, particularly for cardiac and transplant surgery. During heart transplantation, the vagus nerve connections are inevitably severed, and transplant recipients universally develop a denervated heart that beats at a fixed, elevated rate. This study suggests that future surgical approaches might prioritize restoring parasympathetic innervation as a strategy for long-term heart protection — a shift from treating complications after they arise to preventing them in the first place.
Heart Rate Variability: Your Window Into Cardiac Aging
If the vagus nerve is the hardware, HRV is the diagnostic readout. And what that readout shows as we age is not encouraging — unless we do something about it.
HRV naturally declines with age. A young adult in their twenties might have an RMSSD value above 40 milliseconds, while someone in their sixties might register below 20. This decline tracks with the gradual weakening of parasympathetic tone and the relative dominance of the sympathetic nervous system that characterizes physiological aging.
But age alone does not dictate the trajectory. A 2024 review cataloged the factors that independently suppress HRV, and the list reads like a summary of modifiable risk factors: alcohol abuse, physical inactivity, chronic psychological stress, poor sleep quality, excessive body weight, and exposure to environmental stressors like chronic noise or shift work. Each of these factors independently weakens vagal tone, layering additional aging burden on top of the biological clock.
| Category | Factors That Reduce HRV | Factors That Increase HRV |
|---|---|---|
| Physical | Sedentary lifestyle, obesity, aging | Regular aerobic exercise, healthy body composition |
| Psychological | Chronic stress, anxiety, depression | Meditation, social connection, positive affect |
| Lifestyle | Alcohol abuse, poor sleep, shift work | Consistent sleep schedule, moderate alcohol, daylight exposure |
| Environmental | Chronic noise, air pollution, heat stress | Nature exposure, clean air, moderate temperatures |
| Medical | Heart failure, MI history, COPD, diabetes | Disease management, cardiac rehabilitation |
The good news: HRV responds to positive interventions, and the evidence is solid. A 2025 systematic meta-analysis of 34 randomized controlled trials involving 1,434 participants found that long-term exercise interventions significantly improved autonomic balance, reducing the LF/HF ratio — a marker of sympathetic-to-parasympathetic balance. The benefits were particularly pronounced in people who already had health conditions, and interventions lasting eight weeks or longer showed the strongest effects. Both aerobic training and resistance training delivered measurable improvements.
Bottom line: your HRV score is not fixed. It moves with how you live.
Six Evidence-Based Ways to Strengthen Your Vagal Tone
So what actually moves the needle? These six strategies have the strongest evidence behind them, from clinical trials and systematic reviews, not blog posts and Instagram reels.
1. Aerobic Exercise (The Single Most Effective Intervention)
The relationship between exercise and vagal tone is so robust that some researchers now argue causality runs in both directions — higher vagal tone enables better exercise capacity, and exercise strengthens vagal tone. A review in Physiology journal noted that elite endurance athletes display resting heart rates as low as 30 beats per minute, reflecting exceptionally strong vagal braking. But you do not need to train like an elite athlete. The 2025 meta-analysis found that structured aerobic exercise programs of eight weeks or longer significantly shifted autonomic balance toward parasympathetic dominance. Zone 2 cardio — sustained moderate-intensity exercise where you can hold a conversation — is a practical entry point.
2. Slow, Controlled Breathing
Breathing at roughly six breaths per minute — a pace called "resonance frequency breathing" — has been shown to maximize vagal stimulation through the baroreflex pathway. A 2025 review on HRV biofeedback found that this technique strengthens baroreflex sensitivity, improves autonomic balance, reduces systemic inflammation, and enhances emotional regulation. Why it works: slow exhalation activates the vagal brake on the heart, and repeated practice trains the system to hold that stronger output at rest.
3. Cold Exposure
Brief cold water exposure — whether a cold shower, cold water face immersion, or outdoor swimming — triggers a vagal reflex that acutely slows heart rate and, when practiced regularly, appears to improve baseline vagal tone. The diving reflex, triggered specifically by cold water contact with the face, activates the vagus nerve directly and is one of the strongest known vagal triggers in healthy humans.
4. Yoga and Mind-Body Practices
Yoga hits vagal tone from multiple angles at once: controlled breathing, physical postures, and meditative focus. Several of the RCTs included in the 2025 exercise meta-analysis specifically tested mind-body interventions and found significant improvements in HRV metrics. The benefit likely comes from both the respiratory side (controlled breathing) and the psychological side (lower cortisol, calmer sympathetic system).
5. Social Connection and Positive Emotion
Not what you'd expect on a heart health list, but the data is there: positive social interactions activate the ventral vagal complex, a branch of the vagal system tied to facial expression, vocalization, and social bonding. The polyvagal theory, while debated in some of its broader claims, correctly identifies a social function of the vagus nerve. People with stronger social ties tend to show higher resting vagal tone. Connection and cardiovascular resilience feed each other.
6. Gut Health and Anti-Inflammatory Nutrition
The vagus nerve is the primary neural highway between the gut and the brain, and gut inflammation sends afferent vagal signals that can suppress overall vagal tone. Conversely, an anti-inflammatory dietary pattern — rich in omega-3 fatty acids, polyphenols, fiber, and fermented foods — supports the gut microbiome and may indirectly strengthen vagal function. That's part of why anything that lowers systemic inflammation tends to improve HRV as a side effect.
| Intervention | Evidence Level | Key Mechanism | Practical Dose |
|---|---|---|---|
| Aerobic exercise | Strong (meta-analysis) | Autonomic rebalancing via baroreflex training | 150 min/week moderate intensity, 8+ weeks |
| Resonance breathing | Strong (RCTs) | Baroreflex-vagal loop amplification | 10-20 min daily at ~6 breaths/min |
| Cold exposure | Moderate (clinical studies) | Diving reflex, acute vagal activation | 30-90 seconds cold water, 3-5x/week |
| Yoga/mind-body | Strong (RCTs) | Combined respiratory and psychological pathways | 2-3 sessions/week, 45-60 min |
| Social connection | Moderate (observational) | Ventral vagal complex activation | Regular meaningful social interaction |
| Anti-inflammatory diet | Moderate (mechanistic) | Reduced gut-vagal inflammatory signaling | Mediterranean-style dietary pattern |

The Clinical Frontier: Vagus Nerve Stimulation for Heart Disease
Lifestyle changes work, but they're indirect. What if you could stimulate the vagus nerve directly with electricity? That's exactly what clinical researchers have been testing.
Vagus nerve stimulation (VNS) was originally developed in the late 1800s for epilepsy, and the FDA first approved implantable VNS devices in 1997 for treatment-resistant epilepsy. Since then, its approved uses have expanded to treatment-resistant depression and, more recently, stroke rehabilitation. But the heart applications are where things get complicated.
In animal studies, the results have been hard to ignore. VNS reduced infarct size after heart attacks, protected against ventricular fibrillation, and in one heart failure model, dropped mortality from 50 percent to 14 percent. It also normalized inflammatory markers like TNF-alpha and IL-6 that drive disease progression. The likely mechanism: the cholinergic anti-inflammatory pathway, a vagal reflex arc that tamps down excessive immune activation throughout the body.
Clinical translation, however, has been more nuanced. The largest trial to date — INOVATE-HF — enrolled 707 patients with chronic heart failure across 85 centers. The results were mixed: VNS did not reduce the composite endpoint of death or worsening heart failure compared to medical therapy alone. But it did significantly improve quality of life, NYHA functional class, and six-minute walking distance. That same pattern keeps showing up across trials: patients feel better, function better, but don't live longer.
A 2021 systematic review and meta-analysis pooling data from four RCTs and three prospective studies (1,263 total patients) confirmed this picture with high-grade evidence. VNS produced statistically significant improvements in functional class (OR 2.72), quality of life, walking capacity (+55 meters on six-minute walk), and NT-proBNP levels (a blood marker of heart failure severity), all with p-values below 0.005. Adverse effects occurred in only 11 percent of patients. Mortality? Unchanged.
Clinical Reality Check: VNS for heart failure improves how patients feel and function (high-grade evidence), but has not yet proven to extend survival. Newer trials like ANTHEM-HFrEF are testing different stimulation parameters that may change this picture.
Why the disconnect? Probably the stimulation parameters. Different trials used different devices, frequencies, and intensities, and nobody has nailed down the optimal protocol yet. The ongoing ANTHEM-HFrEF trial, using the VITARIA system at sites including the University of Arizona, is testing a more refined approach that might finally close the gap between feeling better and living longer.
There's also a less invasive option. Transcutaneous vagus nerve stimulation (tVNS), applied through the ear or neck with a handheld device, is already FDA-approved for cluster headaches and migraine. Preliminary data hints at modest cardiovascular benefits too, without the surgical commitment.
What We Used to Think vs. What Research Now Shows
| Old Understanding | Current Evidence |
|---|---|
| Vagal tone is just a marker of fitness — it reflects conditioning but doesn't drive health | Vagal tone appears to causally determine exercise capacity and directly protect cardiac tissue from aging |
| Heart rate variability declines with age and cannot be meaningfully changed | HRV responds robustly to exercise, breathing practices, and lifestyle changes at any age — 8+ weeks of intervention shows significant improvement |
| The vagus nerve's cardiac role is limited to heart rate regulation | The vagus nerve actively suppresses inflammation, prevents cellular remodeling, maintains contractile function, and protects against arrhythmias |
| Heart transplant recipients must simply adapt to a denervated heart | Bioengineered nerve conduits can promote vagal regeneration and partially restore cardiac innervation, opening new surgical possibilities |
| Electrical vagus nerve stimulation can cure heart failure | VNS reliably improves quality of life and functional capacity but has not yet demonstrated mortality benefit — stimulation parameters are still being optimized |
Frequently Asked Questions
Can you actually measure your own vagal tone at home?
Yes, through HRV tracking. Many consumer wearables — including devices from Garmin, Apple Watch, Whoop, and Oura — now measure HRV continuously or during sleep. The most common metric reported is RMSSD, which directly reflects short-term parasympathetic (vagal) activity. While these consumer measurements are less precise than clinical-grade electrocardiograms, they provide useful trend data for tracking changes over weeks and months in response to lifestyle modifications.
How quickly can lifestyle changes improve vagal tone?
The 2025 meta-analysis of exercise interventions found that statistically significant improvements in autonomic balance appear after approximately eight weeks of consistent practice. Some interventions work faster acutely — a single session of resonance frequency breathing can temporarily boost HRV within minutes — but durable improvements in resting vagal tone require sustained effort over months. Consistency matters more than intensity.
Is vagus nerve stimulation safe for people without heart failure?
Implantable VNS devices are FDA-approved exclusively for epilepsy, depression, and stroke rehabilitation — not for general cardiovascular wellness. Non-invasive transcutaneous VNS devices are approved for headache disorders and are generally considered safe, with side effects limited to mild skin irritation or tingling. However, anyone with a cardiac pacemaker, defibrillator, or known heart rhythm disorder should consult their cardiologist before using any VNS device, as electrical stimulation of the vagus nerve directly affects heart rate and rhythm.
Does the vagus nerve explain why deep breathing calms anxiety?
It's a big part of it. Slow exhalation activates the vagus nerve, which sends parasympathetic signals to the heart (slowing it), the gut (promoting digestion), and the brain (dialing down the amygdala's alarm response). That's the physiological basis of what gets called the "relaxation response." Deep breathing also lowers cortisol and activates the baroreflex, so the vagus nerve isn't the whole story, but it's doing a lot of the heavy lifting.
Should I worry if my HRV is low for my age?
Worth paying attention to, but don't panic over one bad reading. Alcohol, poor sleep, getting sick, dehydration, and stress all temporarily tank HRV. If it stays low week after week despite decent habits, bring it up with your doctor. The trend is what matters. A number that's slowly climbing or holding steady tells you more than any single snapshot.
Related Articles
- Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition — The vagus nerve is the primary neural highway connecting your gut and brain. This guide explores how the microbiome influences mental health through vagal signaling.
- The Hidden Toll of Low-Level Stress: How Chronic Tension Wrecks Your Hormones — Chronic stress suppresses vagal tone and shifts the autonomic balance toward sympathetic dominance. Learn evidence-based strategies for recovery.
- Zone 2 Cardio for Fat Burning and Longevity — Moderate-intensity aerobic exercise is the strongest evidence-based intervention for improving vagal tone and heart rate variability.
- Sauna Bathing for Heart Health: What 20 Years of Finnish Research Actually Proves — Another promising intervention for cardiovascular wellness with autonomic nervous system benefits.
- 10 Hot Health Benefits of Yoga — Yoga combines controlled breathing, physical movement, and meditation — a triple pathway to stronger vagal tone.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.