A Silent Chemical Storm Brewing in Your Digestive Tract
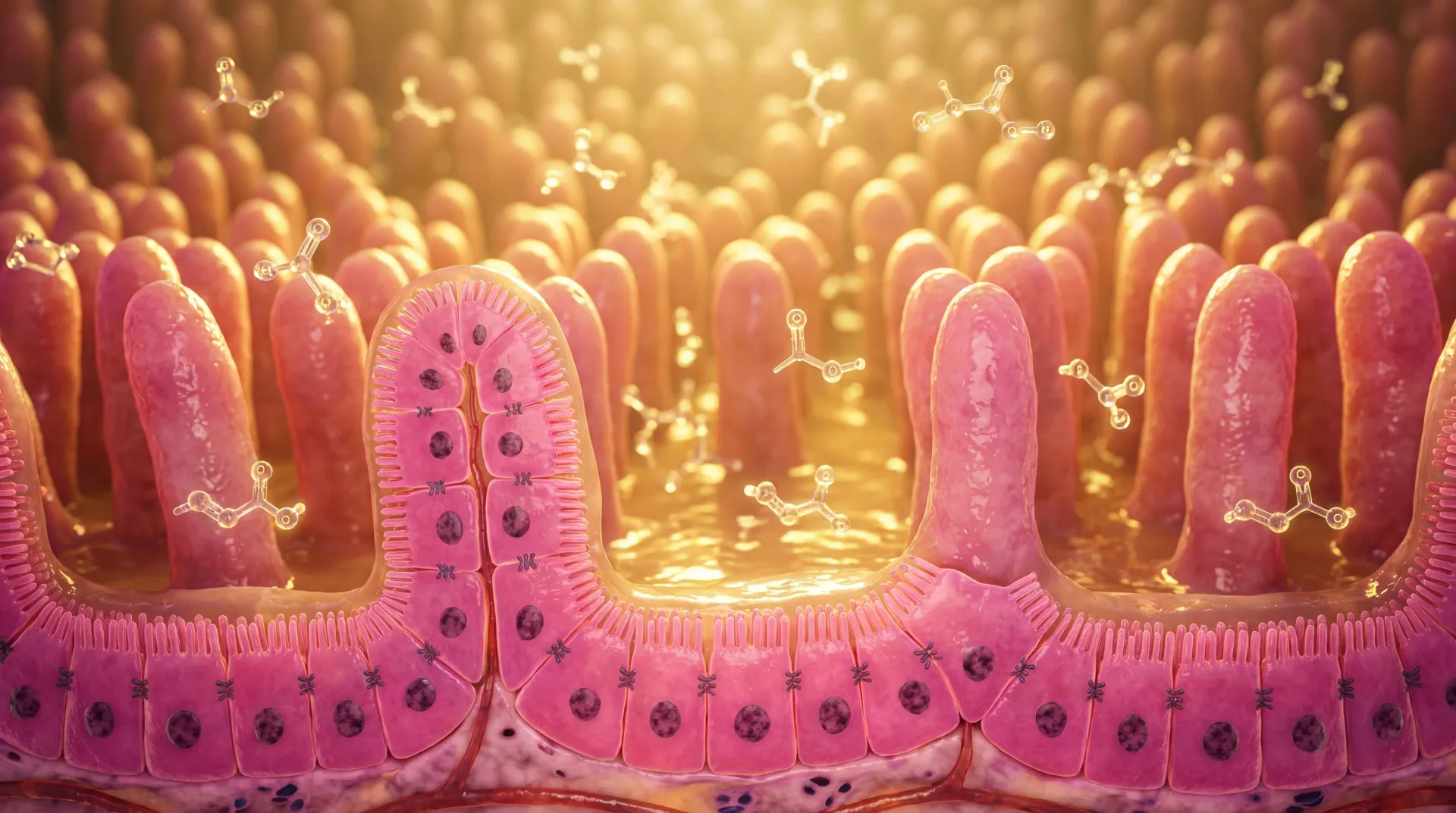
Something unsettling is happening inside you every time you eat a conventionally grown apple, drink from a plastic water bottle, or wipe down your kitchen counter with a commercial cleaner. Hundreds of synthetic chemicals are entering your gastrointestinal tract and interacting with the trillions of microorganisms that your body depends on for proper digestion, immune regulation, and even mental well-being.
For decades, researchers assumed that most industrial and agricultural chemicals passed through our bodies without meaningful consequences for our gut microbiome. That assumption began crumbling in late 2025 when a team at the University of Cambridge published findings that should give every consumer pause. Their large-scale screening in Nature Microbiology tested 1,076 chemical contaminants against 22 species of human gut bacteria and discovered that 168 of them actively inhibited bacterial growth. The majority of these chemicals were never previously suspected of having any antibacterial activity at all.
That landmark finding sits within a growing stack of evidence connecting everyday chemical exposure to measurable shifts in human gut ecology. Researchers at Penn State, the University of Chicago, and Washington State University have each contributed puzzle pieces revealing how persistent organic pollutants, food preservatives, and household chemicals reshape the microbial communities that underpin our health. What follows is a guide through the current science, the chemicals most likely to matter, and what you can realistically do about it.
168 Chemicals That Stifle Your Good Gut Bacteria
The Cambridge study, led by Dr. Indra Roux and Professor Kiran Patil, represents the most comprehensive laboratory assessment to date of how environmental chemicals interact with human gut bacteria. Rather than studying one chemical at a time, the team assembled a library spanning pesticides, pesticide metabolites, industrial chemicals, and mycotoxins, then systematically exposed each compound to carefully selected bacterial strains that are both prevalent and abundant in healthy human intestines.
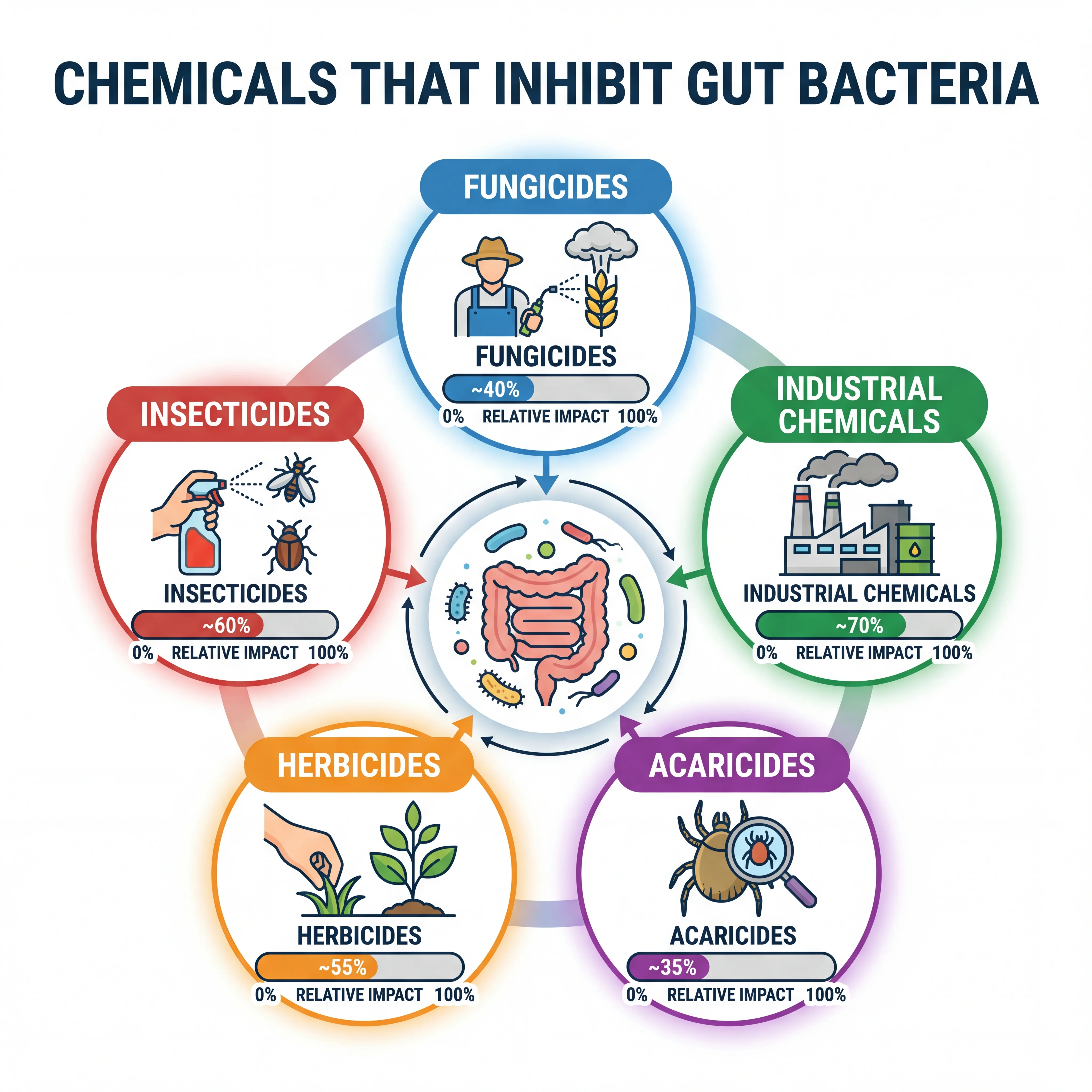
The results painted a troubling picture. Around one in six tested chemicals showed meaningful inhibitory effects. The bacteria most vulnerable to chemical assault belonged to the Bacteroidales order, particularly Parabacteroides distasonis, a species that helps regulate immune function and metabolize bile acids. Meanwhile, Escherichia coli and Akkermansia muciniphila proved more resilient, though they were not entirely unscathed.
Key finding: Twenty-four chemicals demonstrated broad-spectrum toxicity, inhibiting more than one-third of all tested bacterial species. Among the worst offenders were closantel (a livestock antiparasitic that hit 19 of 22 strains), tetrabromobisphenol A, a brominated flame retardant found in electronics (19 strains), and chlordecone, a now-banned insecticide still lingering in the environment (17 strains).
Perhaps the most alarming aspect of this research is the concentration question. The screening was conducted at 20 micromolar, a dose chosen to align with previous pharmaceutical drug screens. When the researchers cross-referenced this with real-world plasma data from a German cohort study of pregnant women, they found that hundreds of blood samples contained at least one xenobiotic compound at 10 micromolar or higher. Given that colonic concentrations tend to match or exceed plasma levels, the doses used in the lab are not far-fetched at all.
| Chemical Category | Compounds Tested | Percentage Showing Gut Bacteria Inhibition | Common Exposure Routes |
|---|---|---|---|
| Fungicides | ~150 | Over 20% | Crop residues, treated grains, wine |
| Industrial chemicals | 48 | Over 20% | Plastics, flame retardants, coatings |
| Acaricides | ~40 | Over 20% | Treated produce, honey |
| Herbicides | ~250 | ~10% | Crop residues, drinking water |
| Insecticides | ~200 | ~12% | Crop residues, household sprays |
How These Substances Actually Dismantle Beneficial Microbes
The Cambridge screening illuminated something unexpected: the way gut bacteria respond to industrial pollutants closely mirrors how they respond to pharmaceutical drugs. Bacterial strains sensitive to many pollutants were also sensitive to many pharmaceutical drugs, suggesting that gut bacteria interact with diverse chemicals through common, non-specific mechanisms. This means exposure to multiple chemicals simultaneously could compound the damage rather than each acting independently.
A comprehensive PMC review examining pollutants from heavy metals to persistent organic pollutants identified several core pathways of damage:
| Mechanism | How It Works | Downstream Consequence |
|---|---|---|
| Direct bacterial killing | Chemical compounds penetrate bacterial cell membranes or disrupt essential enzymes | Reduction in beneficial species; overgrowth of resistant, potentially harmful bacteria |
| SCFA production disruption | Chemicals reduce populations of short-chain fatty acid producers like Ruminococcaceae and Lachnospiraceae | Decreased butyrate leads to weakened intestinal barrier and increased inflammation |
| LPS/TLR4 pathway activation | Gram-negative bacteria proliferate after beneficial species decline, releasing lipopolysaccharides | Systemic inflammatory signaling, linked to metabolic syndrome and cardiovascular disease |
| AHR receptor modulation | Certain pollutants like PCB-126 activate aryl hydrocarbon receptors in intestinal cells | Altered gene expression in gut lining, impaired immune surveillance |
| Bile acid metabolism interference | Chemical disruption of bacteria responsible for bile acid deconjugation and transformation | Impaired cholesterol regulation and fat-soluble vitamin absorption |
The Cambridge team also conducted chemical-genetic screens to determine which bacterial genes modulate susceptibility to pollutants. They discovered something with significant public health implications: the genetic mechanisms bacteria use to resist chemical pollutants overlap with those that confer antibiotic resistance. When gut bacteria adapt to survive exposure to common pesticides or flame retardants, some simultaneously become resistant to clinical antibiotics like ciprofloxacin. If this process is occurring inside real human guts, it could be silently fueling the antibiotic resistance crisis.
Your Grocery Cart's Hidden Gut Disruptors
You do not need to work in a chemical plant to be exposed to gut-disrupting compounds. For most people, the primary route of exposure runs straight through the supermarket.

Consider pesticide residues alone. A UK cohort study found detectable levels of pesticides in every urine sample tested. Cypermethrin and permethrin appeared in over 96% of samples, diethylphosphate in 75%, and glyphosate in 53%. These are ordinary adults eating normal Western diets. Among pesticide categories, fungicides emerged as the worst offenders. The widely used conazole fungicides, including imazalil and prochloraz, showed potent activity against Firmicutes bacteria, inhibiting Eubacterium rectale, a key butyrate producer, at concentrations as low as 2.5 micromolar.
Food preservatives add another layer of concern. Researchers at the University of Chicago studied lantibiotics, a class of bacteriocins widely used by the food industry, and found these compounds kill beneficial commensal bacteria just as effectively as they kill targeted pathogens. Nisin, one of the most commonly used lantibiotics found in everything from beer and sausage to cheese and dipping sauces, showed potent effects against the very same gut bacteria that help protect us from harmful infections.
Worth noting: The typical French supermarket carries food products where 53.8% contain at least one food additive and 11.3% contain five or more. The United States permits over 4,000 food additives. Many of these substances were approved before the gut microbiome's importance was understood, and current safety evaluations do not assess effects on gut bacteria.
If you are working to support your gut through probiotics, prebiotics, or postbiotics, it is worth recognizing that chemical exposure through food may be undermining those efforts. Building a healthy microbiome while simultaneously feeding it compounds that kill beneficial bacteria is like trying to fill a bathtub with the drain open.
Microplastics and Forever Chemicals: The Persistent Offenders
Some of the most concerning gut disruptors simply refuse to leave. Per- and polyfluoroalkyl substances (PFAS), often called "forever chemicals," and microplastics represent exposures that are both difficult to avoid and long-lasting in their effects.
A Washington State University study of 69 toddlers and preschoolers found that children with higher PFAS blood levels showed measurable reductions in gut bacterial amount and diversity. Most striking, these children harbored dehalogenating bacteria, microorganisms normally used for bioremediation of toxic waste sites, not typically found in the human digestive system. Their guts appeared to be recruiting unusual bacteria to manage the chemical burden.
Over 95% of Americans carry detectable PFAS in their blood. The Cambridge study identified bisphenol AF, a PFAS-related plasticizer, as one of the most broadly toxic substances tested, inhibiting 12 of 22 bacterial strains.
Microplastics present a different but equally concerning problem. A comprehensive review in PMC documented how plastic particles smaller than 5 millimeters accumulate in the gastrointestinal tract, provoke inflammatory responses, and increase intestinal permeability. Humans ingest microplastics through seafood, bottled water, table salt, and even the air. Our guide on microplastic detoxification and tracking covers practical strategies.
| Persistent Chemical | Where It Hides | Known Gut Effects |
|---|---|---|
| PFOS (perfluorooctane sulfonate) | Nonstick cookware, food packaging, firefighting foam | Alters Bacteroidetes-to-Firmicutes ratio, potential sex-specific effects, decreased beta diversity in exposed infants |
| PFOA (perfluorooctanoic acid) | Stain-resistant fabrics, contaminated water | Decreases Bifidobacterium and Lactobacillus, reduces SCFA production |
| Bisphenol AF | Plastics, epoxy resins, thermal paper | Broad-spectrum inhibition of 12 out of 22 gut bacterial species tested |
| Tetrabromobisphenol A | Flame retardants in electronics, upholstery | Inhibited 19 of 22 gut bacterial strains, one of the broadest-spectrum compounds identified |
| Polyethylene microplastics | Plastic bottles, food packaging, cosmetics | Physical gut lining damage, increased intestinal permeability, dysbiosis |
What Happens When Your Microbiome Loses Its Diversity
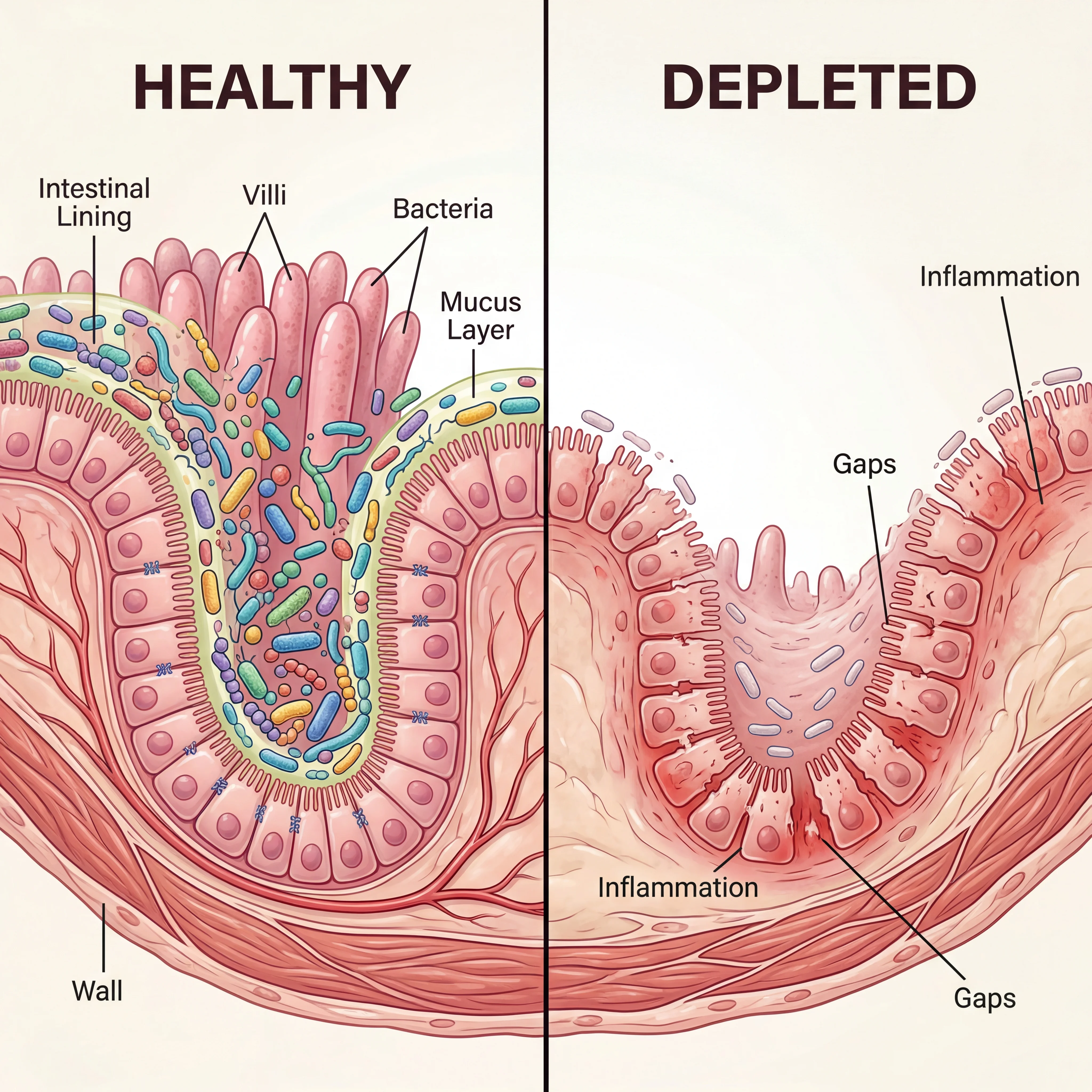
Picture your gut microbiome as a densely planted rainforest. Each bacterial species occupies a niche, performs specific tasks, and keeps its neighbors in check. When chemical pollutants selectively eliminate certain species, the ecosystem does not simply become a slightly smaller version of itself. It transforms in ways that cascade through your entire body.
Penn State researchers demonstrated this cascade vividly in a study on persistent organic pollutants. When they exposed young mice to TCDF, a widespread byproduct of waste incineration, the animals' gut microbiomes were permanently disrupted, even after the chemical was completely eliminated from their bodies. Three months later, the equivalent of a young human adult, those mice showed higher body weight and glucose intolerance. When the researchers transplanted the disrupted microbiomes into germ-free mice, the recipients developed the same metabolic problems, proving that the altered microbiome itself was driving disease.
The bacterium most affected was Akkermansia muciniphila, a species increasingly recognized as critical for metabolic health and gut barrier integrity. When the Penn State team supplemented the TCDF-exposed mice with Akkermansia as a probiotic, their microbiomes returned to normal. You can learn more about this important bacterium and its health implications in our article on Akkermansia as a probiotic for metabolic health.
The Italian "Land of Fires" study, published in Nature Communications, provided a rare human parallel. Researchers examined the gut microbiomes of 359 people living in areas of Campania, Italy with varying levels of environmental pollution from decades of illegal industrial waste dumping. People in the most polluted areas showed significantly different gut microbiome compositions compared to those in cleaner areas, even after controlling for diet, age, BMI, and antibiotic use. The microbiomes of the heavily exposed population appeared to have undergone a form of adaptive selection, enriching for bacteria capable of degrading pollutants at the expense of normal commensal species.
The consequences of lost microbial diversity are wide-reaching:
- Weakened immune regulation: Reduced SCFA production impairs the gut's ability to suppress inflammatory responses, contributing to chronic low-grade inflammation
- Metabolic disruption: Altered bile acid metabolism and reduced production of beneficial metabolites increase risk of obesity, insulin resistance, and type 2 diabetes
- Increased intestinal permeability: Loss of mucus-producing and barrier-maintaining bacteria allows bacterial toxins and food antigens into the bloodstream
- Mental health effects: Disruption of the gut-brain axis through altered neurotransmitter precursor production and increased neuroinflammation
- Heightened infection vulnerability: When beneficial bacteria are eliminated, opportunistic pathogens face less competition for resources and colonization sites
Myth vs. Fact: Chemical Exposure and Gut Health
| Myth | Fact |
|---|---|
| Chemicals in food are tested to ensure they do not harm gut bacteria | Standard chemical safety assessments do not evaluate effects on the human gut microbiome. Chemicals are tested against their intended targets only, such as insects or fungi. |
| You would need industrial-level exposure for chemicals to affect your gut | The Cambridge screening found bacterial growth inhibition at 20 micromolar, and many compounds were effective at 2.5 micromolar. Real-world human blood samples commonly show xenobiotic levels of 10 micromolar or higher. |
| Organic food completely eliminates chemical exposure risks to your gut | While organic food reduces pesticide residue exposure, you are still exposed to chemicals through water, air, food packaging, household products, and environmental pollution. Organic eating is helpful but not a complete solution. |
| Gut bacteria damaged by chemicals will bounce back once exposure stops | Penn State research showed that early-life exposure to persistent organic pollutants caused permanent microbiome disruption in mice, with metabolic consequences lasting into adulthood even after the chemical was fully eliminated. |
| Only antibiotics can cause meaningful damage to the gut microbiome | The Cambridge screening showed that the sensitivity of gut bacteria to chemical pollutants correlates with their sensitivity to pharmaceutical drugs, meaning non-antibiotic chemicals can cause antibiotic-level disruption. |
| Flame retardants and plasticizers are inert and do not affect living organisms | Tetrabromobisphenol A (a flame retardant) inhibited 19 of 22 tested gut bacterial species. Bisphenol AF (a plasticizer) inhibited 12 of 22. Both were among the most broadly toxic substances identified. |
Practical Ways to Shield Your Gut from Chemical Damage
The Cambridge researchers offered straightforward advice: wash your fruits and vegetables before eating them, and avoid using pesticides in your garden. That is a reasonable starting point, but the evidence supports a more comprehensive approach. Reducing your chemical load is not about perfection, but prudent action.
In the kitchen:
- Wash all produce thoroughly under running water. A baking soda soak (one teaspoon per two cups of water for 12-15 minutes) removes more pesticide residue than water alone
- Prioritize organic for the highest-residue items using the Environmental Working Group's "Dirty Dozen" list as a guide
- Reduce reliance on ultra-processed foods, which carry the highest burden of food additives and preservatives
- Store food in glass or stainless steel rather than plastic, especially for hot foods and acidic liquids
- Filter drinking water with a system rated for PFAS removal, such as reverse osmosis or activated carbon block filters
In your home environment:
- Replace nonstick cookware with cast iron, stainless steel, or ceramic alternatives
- Choose cleaning products with simpler ingredient lists. Vinegar, baking soda, and castile soap handle most household cleaning needs
- Ventilate your home regularly and vacuum with a HEPA filter to reduce semi-volatile organic compounds and dust-borne chemical exposure
Supporting your microbiome simultaneously:
- Eat a diverse range of fiber-rich whole foods. Dietary diversity is one of the strongest predictors of microbiome diversity
- Include fermented foods like yogurt, kefir, sauerkraut, and kimchi to introduce beneficial bacteria and maintain microbial resilience
- Consider targeted probiotics, particularly strains like Akkermansia muciniphila that research shows can be depleted by chemical exposure and restored through supplementation
- Support detoxification through adequate hydration, regular physical activity, and sufficient sleep. Maintaining proper electrolyte balance supports these processes
Frequently Asked Questions
Which everyday chemicals are most dangerous to gut bacteria?
Based on the 2025 Cambridge screening of over 1,000 compounds, the most broadly harmful chemicals include the flame retardant tetrabromobisphenol A (TBBPA), which inhibited 19 of 22 bacterial strains, and the plasticizer bisphenol AF (BPAF), which inhibited 12 strains. Among pesticides, fungicides showed the highest rate of gut bacteria inhibition, with conazole fungicides like imazalil and prochloraz being especially potent against beneficial Firmicutes species.
Can probiotics undo the damage that chemicals cause to the gut microbiome?
There is encouraging evidence. Penn State researchers showed that supplementing with Akkermansia muciniphila restored normal microbiome function in mice whose gut bacteria had been permanently disrupted by persistent organic pollutants. However, probiotics are unlikely to fully compensate if chemical exposure continues. The most effective approach combines reducing exposure with actively supporting beneficial bacteria through diet and targeted supplementation.
Does cooking or processing food remove the chemicals that harm gut bacteria?
Cooking can reduce some pesticide residues, but many chemicals identified in recent research are heat-stable. PFAS are specifically engineered to resist degradation, and microplastics can actually increase through processing. Washing produce is more effective for surface residue removal than cooking, and choosing less-processed foods reduces exposure to additives and packaging-derived contaminants.
Are children more vulnerable to chemical-induced gut microbiome damage than adults?
Evidence suggests yes. Washington State University found that children with higher blood levels of PFAS and phthalates showed measurable gut microbiome disruption. Penn State demonstrated that early-life chemical exposure caused permanent microbiome disruption with metabolic consequences lasting into adulthood. Children face higher relative exposure due to smaller body weight, tendency to mouth objects, and proximity to contaminated dust.
Should I get my gut microbiome tested if I am concerned about chemical exposure?
Commercial microbiome testing can provide a snapshot of your bacterial composition, but interpreting results in the context of chemical exposure is still an emerging science. These tests can identify reduced diversity or shifts in major bacterial groups, which may prompt useful dietary or lifestyle changes. For a deeper look at what current testing can and cannot tell you, see our guide on gut health personalization and microbiome testing.
Related Articles
- Akkermansia: The Gut Bacterium Reshaping Metabolic Health — Explore how this key bacterial species, often depleted by chemical exposure, plays a central role in metabolic regulation.
- Postbiotics vs. Probiotics vs. Prebiotics: What Your Gut Actually Needs — Understand the different approaches to supporting your microbiome and which one delivers the most benefit.
- Microplastic Detoxification and Tracking — A practical guide to monitoring and reducing your microplastic exposure, one of the persistent gut disruptors discussed in this article.
- Artificial Sweeteners: Dangers and Benefits — Another category of food chemicals with documented effects on gut bacteria that deserves your attention.
- Gut Health Personalization and Microbiome Testing — Learn what current testing reveals about your microbial health and how to use that information effectively.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.