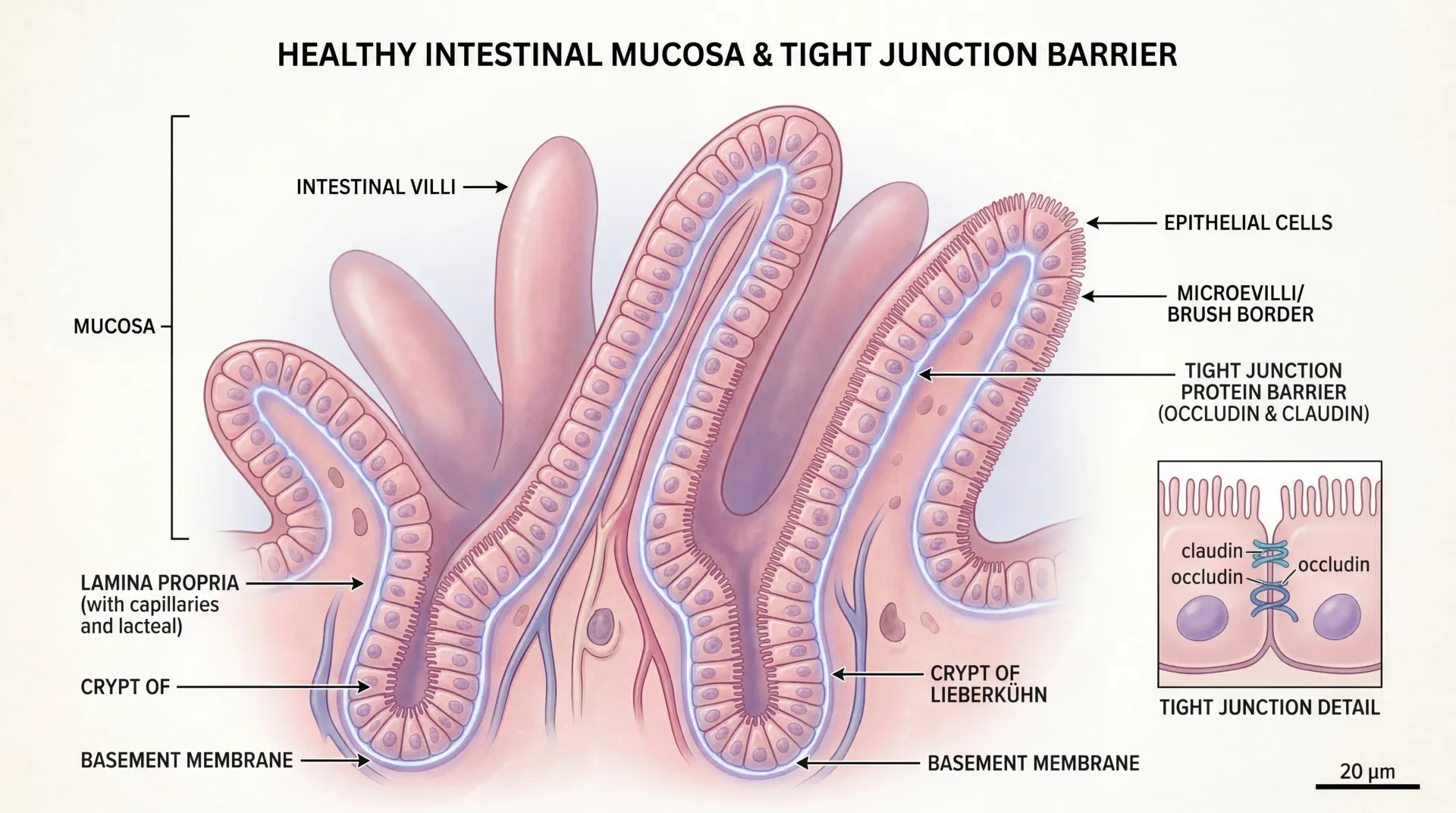
Most dietary advice tells you what to eat. Resistant starch flips the script by changing how you prepare what you already eat. Cook a pot of rice, refrigerate it overnight, and something remarkable happens at the molecular level: a portion of the starch rearranges itself into a structure your small intestine can no longer break down. That leftover rice now feeds your gut bacteria instead of spiking your blood sugar. No special supplements, no exotic ingredients, no subscription required.
The scale of the opportunity is worth paying attention to. Americans consume roughly 5 grams of resistant starch per day, barely a third of what researchers consider the minimum effective dose. Meanwhile, populations in parts of Africa consuming 20 to 30 grams daily show markedly different metabolic profiles. The gap between where most people are and where the science suggests they should be represents one of the cheapest nutritional upgrades available.
Why Your Leftovers Might Be Healthier Than the Original Meal
When you cook potatoes, rice, or pasta, heat causes starch granules to absorb water and swell in a process called gelatinization. The orderly crystalline structure breaks apart, making the starch highly accessible to your digestive enzymes. This is why freshly cooked white rice spikes blood sugar faster than you might expect from a seemingly bland food.
But cooling those same foods triggers a second transformation. As the temperature drops, the starch molecules -- particularly the linear chains called amylose -- begin reassembling into tight double-helix structures. Food scientists call this retrogradation, and it creates a form of starch that resists enzymatic breakdown. According to researchers at Ohio State University, refrigerating pasta, rice, or potatoes for at least 24 hours measurably increases their resistant starch content.
The truly surprising part: even reheating these foods does not fully reverse the process. The retrograded starch retains much of its resistance, which means your Tuesday leftovers are a different nutritional product than the same meal served fresh on Monday. Gram for gram, resistant starch delivers roughly 2.5 calories versus 4 calories for regular starch -- a meaningful reduction that accumulates over weeks and months of consistent eating.
Five Types of Resistant Starch and Where to Find Them
Resistant starch is not a single compound. It is a family of starches that all share one trait: they pass through the small intestine without being digested. Scientists currently recognize five distinct types, each with a different reason for resisting your enzymes.
| Type | Why It Resists Digestion | Common Food Sources |
|---|---|---|
| RS1 | Physically trapped inside intact cell walls | Whole grains, seeds, legumes, coarsely ground kernels |
| RS2 | Tightly packed crystalline granules block enzyme access | Raw potatoes, green bananas, high-amylose corn starch |
| RS3 | Retrograded starch formed during cooling | Cooked-and-cooled rice, pasta, potatoes, bread |
| RS4 | Chemical cross-linking engineered to resist digestion | Modified food starches used in processed products |
| RS5 | Amylose-lipid complexes shield starch from enzymes | Foods with starch-fat interactions (some baked goods) |
Understanding these categories matters because different types behave differently in your gut. RS1 and RS2 are the forms most studied for blood sugar management, while RS3 is the type you can create at home by simply refrigerating cooked starchy foods. RS4 is primarily an industrial ingredient, and RS5 is the newest category, recently expanded to include starch complexes formed with amino acids, peptides, and polyphenols.
Quick fact: The amylose-to-amylopectin ratio in a food determines how much resistant starch it can form. Higher amylose content means more potential for resistant starch -- which is why high-amylose corn varieties were specifically bred for this property.
Most real-world meals contain a mix of types. A bowl of lentil soup, for instance, delivers RS1 from intact legume cell walls. Refrigerate and reheat it the next day, and you have added RS3 to the mix. The practical takeaway is that variety and preparation method both influence your daily resistant starch intake.
| Food Category | Average RS Content (g per 100g) | Best Preparation for Maximum RS |
|---|---|---|
| Legumes (lentils, chickpeas, beans) | 4 - 10 | Cook then cool overnight |
| Grains (barley, oats, whole wheat) | 3 - 7 | Minimally processed, cooked and cooled |
| Tubers (potatoes, yams) | 2 - 5 | Boil, refrigerate 24 hours, serve cold or reheat |
| Green bananas | 8 - 12 | Eaten raw or in smoothies (ripening reduces RS) |
| Raw potato starch (supplement) | ~63 | Mixed into cold liquids (heating destroys RS2) |
What Happens When Resistant Starch Reaches Your Colon
While your small intestine ignores resistant starch, the trillions of bacteria in your large intestine treat it as a feast. This is where things get interesting, because the metabolic byproducts of that bacterial fermentation have effects that reach well beyond your gut.
When colonic bacteria break down resistant starch, they produce short-chain fatty acids (SCFAs) -- primarily butyrate, acetate, and propionate. Each plays a distinct role. Butyrate is the preferred energy source for colonocytes (the cells lining your colon), and it helps maintain the integrity of the gut barrier that prevents bacterial toxins from leaking into your bloodstream. Acetate enters the bloodstream and influences fat metabolism. Propionate travels to the liver and appears to regulate glucose production and cholesterol synthesis.
Beyond SCFAs, resistant starch fermentation reshapes the composition of your microbial community. Research has shown that RS consumption increases populations of Roseburia, Faecalibacterium, Akkermansia, and Bifidobacteria -- bacterial genera that have been consistently associated with better metabolic health. Faecalibacterium prausnitzii in particular has attracted attention because it is found at lower levels in people with inflammatory bowel disease, irritable bowel syndrome, and colorectal cancer. If you have been hearing about Akkermansia as a next-generation probiotic, it is worth knowing that resistant starch is one of the dietary strategies shown to naturally support its growth.
There is also a hormonal dimension to this bacterial activity. SCFAs stimulate specialized cells in the gut lining to release GLP-1 (glucagon-like peptide 1) and PYY (peptide YY). GLP-1 is the same hormone targeted by blockbuster diabetes and weight-loss drugs like semaglutide. The amounts produced from resistant starch fermentation are far more modest than pharmaceutical doses, but the mechanism is the same: GLP-1 stimulates insulin secretion and slows gastric emptying, keeping you satisfied longer after a meal. If you are interested in dietary strategies that work through this pathway, our guide to foods that naturally increase GLP-1 production covers additional approaches.
The Blood Sugar Connection: What 36 Clinical Trials Revealed
The most robust evidence for resistant starch's metabolic benefits comes from a systematic review and meta-analysis published in Frontiers in Nutrition that pooled data from 36 randomized controlled trials involving 982 participants with type 2 diabetes or prediabetes. The findings paint a clear picture of which types of resistant starch matter most and where the benefits are strongest.
| Outcome Measured | RS Type 1 Effect | RS Type 2 Effect |
|---|---|---|
| Acute postprandial glucose | Significant reduction (SMD -0.54) | Significant reduction (SMD -0.96) |
| Acute postprandial insulin | Not significant | Significant reduction (SMD -0.71) |
| Chronic postprandial glucose | Significant reduction (SMD -0.38) | Significant reduction (SMD -0.29) |
| Chronic fasting glucose | Not significant | Significant reduction (SMD -0.39) |
| Chronic fasting insulin | Not significant | Significant reduction (SMD -0.40) |
Two patterns stand out. First, both RS1 (from intact plant structures like whole grains and legumes) and RS2 (from raw starches like green banana and high-amylose corn) lower blood glucose after meals. But only RS2 appears to improve fasting glucose and insulin levels -- suggesting the two types work through partially different biological mechanisms.
The researchers proposed that RS1 primarily works by physically slowing starch digestion (the cell walls act as barriers), while RS2 exerts its effects through colonic fermentation and the downstream metabolic signals from SCFAs. This distinction has practical implications: if you want to blunt the blood sugar spike from a specific meal, eating intact whole grains with that meal (RS1) may help. If you want to improve your baseline metabolic markers over time, regularly consuming high-amylose starches or cooled starchy foods (RS2 and RS3) appears more effective.
A separate review in the Journal of Diabetes Investigation reached similar conclusions, noting that resistant starch can lower postprandial glucose levels comparably to a low-glycemic-index diet. The authors emphasized that RS is particularly promising because it does not require people to eliminate carbohydrates -- it changes how existing carbohydrates behave in the body.
Key finding: The meta-analysis showed RS type 2 improved fasting insulin by a standardized mean difference of -0.40 -- a meaningful shift that, if sustained, could reduce long-term diabetes risk for people with prediabetes.
Metabolism, Weight, and the Calorie Trick Hiding in Your Fridge
Resistant starch's metabolic effects go beyond blood sugar. If you care about body composition or energy balance, three things are happening at once.
Reduced caloric extraction. Because resistant starch bypasses small intestine digestion, your body extracts fewer calories from it. As noted earlier, resistant starch yields approximately 2.5 calories per gram compared to 4 calories per gram for digestible starch. For someone eating 200 grams of starchy carbohydrates daily, shifting even 20 percent of that to resistant forms could reduce caloric intake by roughly 60 calories per day -- enough to matter over months without any conscious restriction.
Increased satiety signaling. The GLP-1 and PYY released during colonic fermentation both act as appetite-regulating hormones. GLP-1 slows gastric emptying, which means food stays in your stomach longer and you feel full for an extended period. PYY signals to the brain that you have eaten enough. This is not a dramatic appetite suppression -- it is a subtle shift in how quickly hunger returns after a meal. Cleveland Clinic registered dietitian Beth Czerwony has noted that eating foods with resistant starch can help you feel full for longer, potentially reducing how much or how often you eat.
Higher thermic effect. Your body expends more energy digesting resistant starch than rapidly digestible starch. The fermentation process in the colon is metabolically active, and the subsequent processing of SCFAs by the liver and other tissues requires additional energy expenditure. While this effect is modest compared to, say, the thermic effect of protein, it contributes to a slightly higher overall metabolic rate on days when resistant starch intake is higher.
None of these effects will transform your body overnight. But they stack. Over weeks and months of eating more resistant starch, you are extracting fewer calories, staying full longer, and burning slightly more energy during digestion. For people who have tried and abandoned strict low-carb diets, this is a different proposition: you keep eating carbohydrates, but you change how your body processes them.
Myth vs. Fact: What Resistant Starch Can and Cannot Do
Resistant starch has picked up a lot of buzz online, and predictably, some of it has outrun the evidence. Here is what holds up and what does not.
| Claim | Reality |
|---|---|
| Cooling rice makes it zero-carb | Myth. Cooling converts only a fraction of the total starch to resistant starch. The rice still contains plenty of digestible carbohydrates. |
| RS can lower blood sugar after meals | Fact. Multiple meta-analyses confirm that RS types 1 and 2 significantly reduce postprandial glucose in people with diabetes and prediabetes. |
| You need expensive supplements to get enough RS | Myth. Legumes, cooled potatoes, oats, and green bananas are affordable, widely available sources. A can of beans delivers 4-10 grams. |
| RS feeds beneficial gut bacteria | Fact. Clinical trials show RS increases Faecalibacterium, Akkermansia, Bifidobacteria, and Roseburia populations. |
| RS is a replacement for diabetes medication | Myth. RS may complement medical treatment but is not a substitute. The meta-analysis evidence supports RS as a dietary adjunct, not a standalone therapy. |
| Reheating food destroys all resistant starch | Myth. Retrograded starch (RS3) retains significant resistance to digestion even after reheating. |
| RS can improve fasting insulin levels | Fact. The 36-trial meta-analysis found RS2 significantly improved chronic fasting insulin (SMD -0.40). |
One area where the evidence is still developing involves inflammation. A narrative review examining clinical evidence from 2010 to 2023 found that RS shows beneficial effects on inflammatory markers, but the data is less consistent than the glucose and insulin findings. Effects appear strongest in people who already have metabolic dysfunction, which makes biological sense: if your inflammatory baseline is normal, there is less room for improvement.

A Practical Guide to Getting More Resistant Starch Daily
The gap between the average American intake of 5 grams per day and the recommended minimum of 6 grams per meal is wide but entirely bridgeable with straightforward kitchen habits. The goal is not perfection -- it is consistent, incremental increases using foods you probably already buy.
Batch-cook and cool your starches. This is the single highest-impact change. Cook a large pot of rice, potatoes, or pasta at the beginning of the week. Transfer it to the refrigerator and use portions throughout the week. Each overnight cooling cycle converts a portion of digestible starch into RS3. You can eat these foods cold (potato salad, cold rice bowls) or reheat them -- the resistant starch largely persists.
Make legumes a daily habit. Beans, lentils, and chickpeas are the most RS-dense common foods, delivering 4 to 10 grams of resistant starch per 100 grams. They are also among the cheapest protein sources available. A daily serving of beans or lentils -- in soups, salads, grain bowls, or simply as a side -- can single-handedly close most of the RS intake gap.
Choose less-ripe bananas. Green and slightly green bananas contain substantially more resistant starch (RS2) than their ripe yellow counterparts. As bananas ripen, enzymes convert resistant starch into sugar, which is why ripe bananas taste sweeter. Slicing a green banana into overnight oats or a smoothie is an easy way to add RS2 without changing your routine.
Consider raw potato starch as a supplement. For those who want to maximize intake, unmodified raw potato starch (available at most grocery stores for a few dollars per bag) contains approximately 63 percent resistant starch by weight. One tablespoon mixed into a cold smoothie or glass of water delivers roughly 8 grams of RS2. The critical rule: do not heat it, or you will destroy the crystalline structure that makes it resistant.
Increase intake gradually. Resistant starch is fermented by gut bacteria, and ramping up too quickly can cause bloating, gas, and discomfort. Start with one additional serving of legumes or cooled starches per day for a week before adding more. Ohio State University researchers emphasize that drinking more water as you increase RS intake helps manage these transition symptoms. Most people find that their gut adapts within two to four weeks.
The connection between resistant starch and the gut-brain axis is worth noting here as well. Because RS fermentation produces butyrate and other SCFAs that influence neurotransmitter production and vagal nerve signaling, improving your gut microbiome composition through RS may have benefits that extend to mood and cognitive function -- though this research is still in earlier stages.
Budget comparison: A 24-ounce bag of raw potato starch costs roughly $3-4 and contains about 45 servings of RS2. A month's supply of a branded resistant starch supplement can cost $30-50. The starch in a bag of dried lentils ($1-2) provides RS at a fraction of any supplement's price.
Frequently Asked Questions
How long does it take for resistant starch to improve gut health?
Most people notice digestive changes (including initial gas and bloating that then subsides) within the first two weeks of increasing RS intake. Changes to gut bacteria populations can be detected within one to three weeks of consistent consumption. However, benefits to insulin sensitivity and blood sugar control may take four weeks or longer to become measurable, according to clinical trial data.
Can you get enough resistant starch from diet alone without supplements?
Absolutely. Populations in parts of Africa and China consume 15 to 30 grams of resistant starch daily from ordinary foods like legumes, whole grains, and tubers. A diet that includes daily beans or lentils, batch-cooked and cooled rice or potatoes, and whole grains can easily exceed the recommended minimum of 6 grams per meal without any supplements.
Does resistant starch help people who are already on diabetes medication?
Clinical evidence suggests that RS can complement diabetes management as a dietary adjunct. The meta-analysis of 36 trials found meaningful improvements in both fasting and postprandial glucose among participants with type 2 diabetes, many of whom were on medication. However, RS should not replace prescribed treatments, and anyone on blood sugar-lowering medication should consult their healthcare provider before significantly increasing RS intake, as it could enhance the glucose-lowering effect.
Is cooled-and-reheated rice safe to eat?
Yes, with proper food safety practices. The concern with reheated rice is Bacillus cereus, a bacterium that can multiply if cooked rice is left at room temperature for extended periods. The solution is straightforward: cool cooked rice quickly (within one hour), store it in the refrigerator promptly, and reheat it thoroughly to at least 165 degrees Fahrenheit before eating. Following these steps makes cooled rice both safe and higher in resistant starch.
Are there any people who should avoid increasing resistant starch intake?
People with SIBO (small intestinal bacterial overgrowth), active inflammatory bowel disease flares, or other conditions where fermentable carbohydrates cause significant symptoms should approach resistant starch cautiously and ideally under guidance from a gastroenterologist. For most healthy adults and those with well-managed digestive conditions, a gradual increase in RS is safe and beneficial.
Related Articles
- Butyrate: The Gut Metabolite That Heals Your Colon and Protects Your Brain -- A deeper look at the primary short-chain fatty acid produced when resistant starch is fermented in the colon.
- Akkermansia: The Next-Generation Probiotic for Metabolic Health -- How resistant starch naturally supports the growth of this beneficial gut bacterium linked to improved metabolic markers.
- Foods That Naturally Increase GLP-1 Hormone Production -- Additional dietary strategies that stimulate the same appetite and blood sugar-regulating hormone boosted by resistant starch fermentation.
- Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition -- The broader story of how gut bacteria and their metabolites influence brain function, including the SCFA pathways activated by resistant starch.
- Inflammation and Chronic Disease: A Complete Guide to Anti-Inflammatory Living -- How the anti-inflammatory effects of butyrate and other SCFAs from resistant starch fit into a comprehensive strategy for reducing chronic inflammation.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.