What Happens When Your Body Can't Clear Histamine Fast Enough?
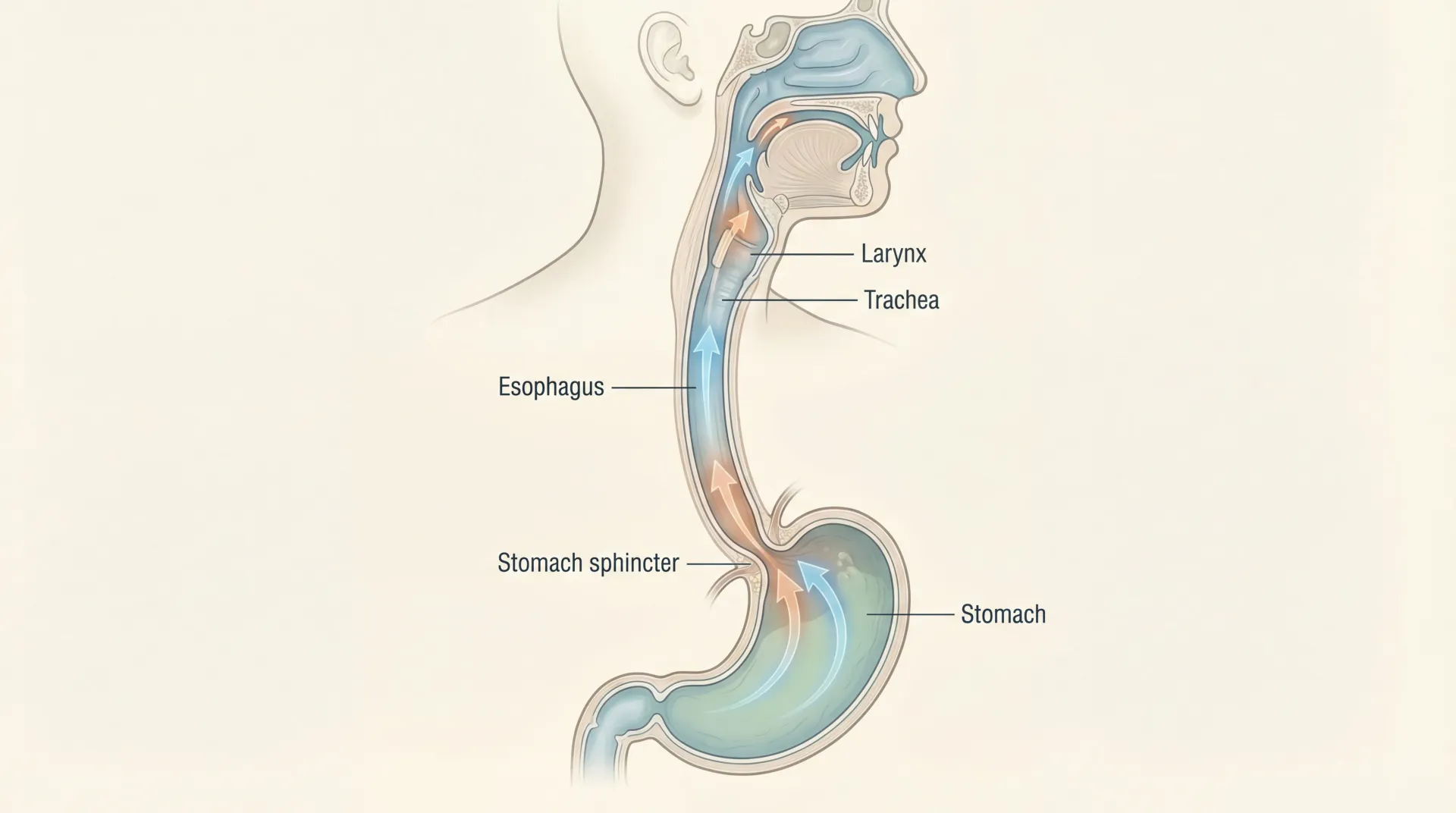
Histamine is one of those molecules your body genuinely needs. It regulates stomach acid, helps you stay alert, and coordinates your immune response to infections and allergens. Problems start when histamine builds up faster than your body can break it down. The symptoms that follow are all over the map, which is part of why so few people get the right diagnosis.
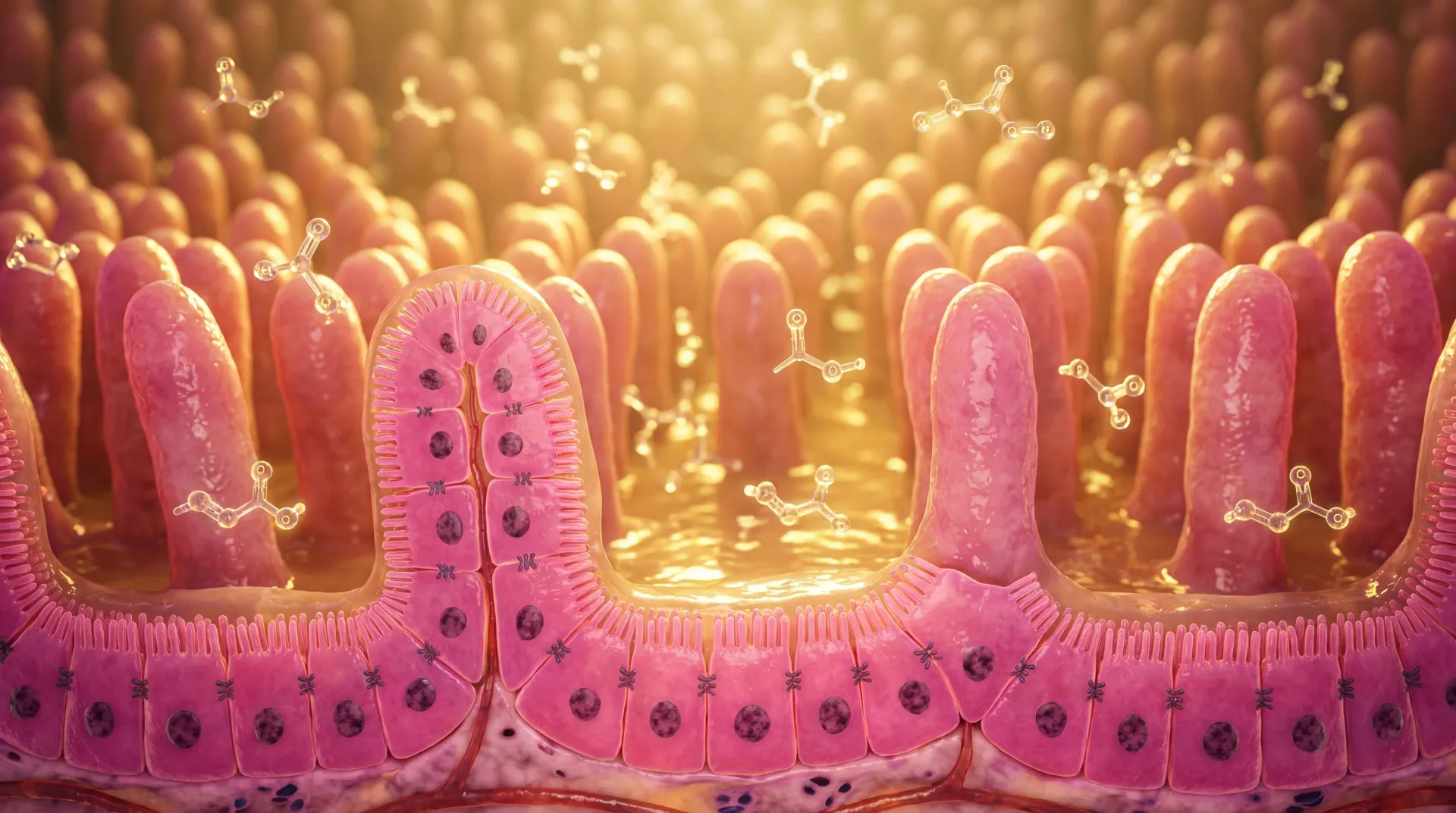
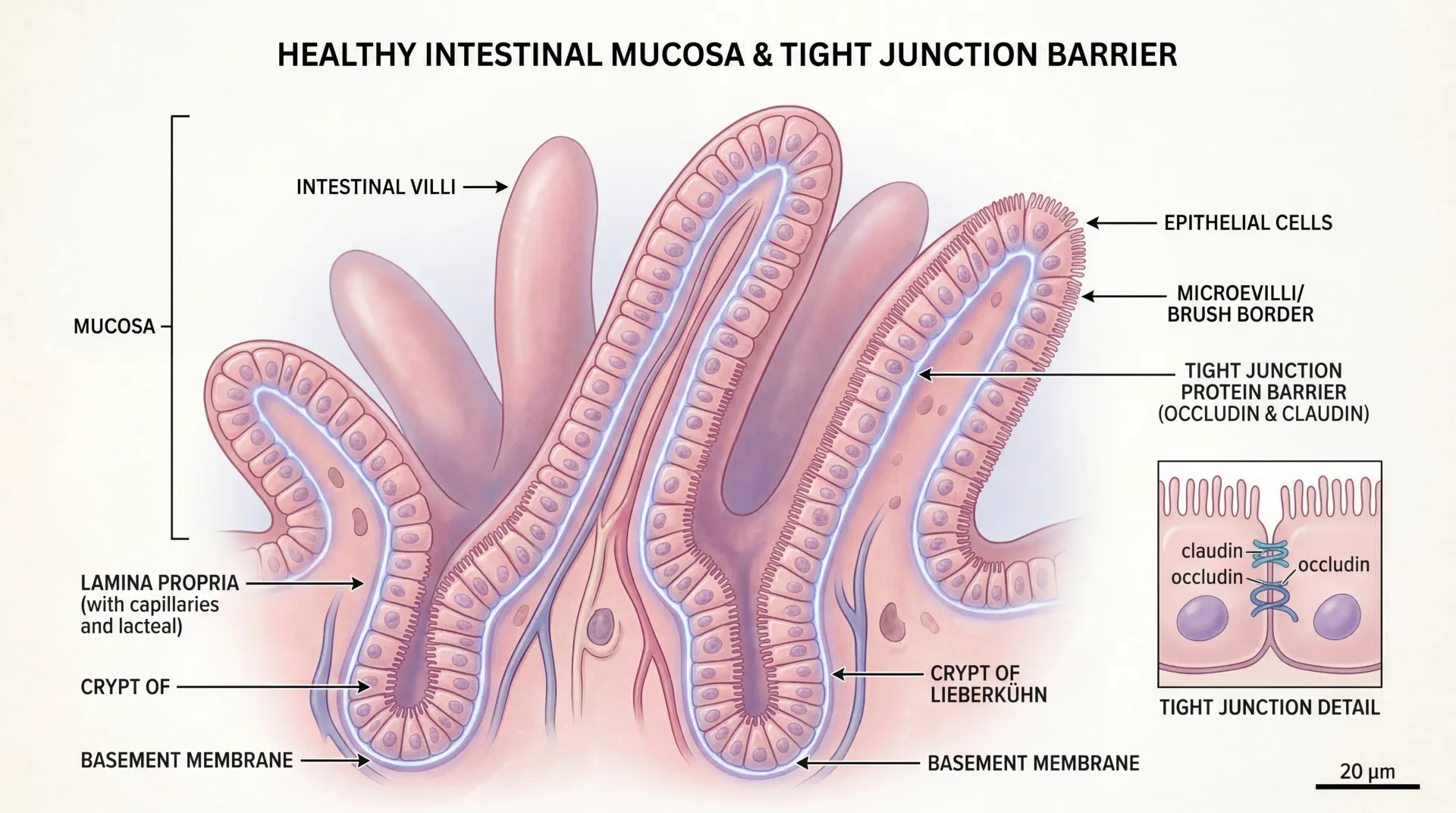
Histamine intolerance (HIT) occurs when there's a mismatch between the histamine entering your system (from food, gut bacteria, or your own immune cells) and your body's capacity to degrade it. The primary enzyme responsible for clearing dietary histamine in your intestines is diamine oxidase, or DAO. When DAO activity drops, whether because of genetics, gut damage, or certain medications, histamine spills past the intestinal barrier and triggers reactions throughout your body.
This isn't an allergy. In a true food allergy, your immune system reacts to a specific protein through IgE-mediated pathways. Histamine intolerance is a capacity problem: your enzymatic clearance system is overwhelmed. Think of it less like a lock-and-key reaction and more like a drain that's partially clogged. Everything works fine until too much water comes through at once.
Estimates suggest histamine intolerance affects roughly 1% of the population, with about 80% of those affected being middle-aged adults. But these numbers likely undercount the real prevalence — the condition is chronically underdiagnosed. Its symptoms mimic everything from small intestinal bacterial overgrowth (SIBO) to irritable bowel syndrome to seasonal allergies.
Quick Take: Histamine intolerance isn't about being allergic to histamine. It's about not being able to break it down efficiently, usually because of reduced DAO enzyme activity in your gut.
Three Reasons Your Histamine Clearance System Fails
DAO isn't a static quantity you're born with and stuck with forever. Your enzyme activity fluctuates based on genetics, gut health, and even what medications you take. Understanding why DAO drops matters because it determines what kind of intervention actually helps.
Genetic predisposition
Your DAO enzyme is encoded by the AOC1 gene, and researchers have identified over 50 single-nucleotide polymorphisms (SNPs) that can alter how efficiently it works. Three variants in particular — rs10156191, rs1049742, and rs1049793 — appear most frequently in people with histamine-related symptoms. A 2024 editorial in the Journal of Clinical Medicine reported that roughly 80% of patients with DAO-related conditions carried at least one defective allele. However, 72% of healthy individuals also carried these variants, meaning genetics loads the gun but doesn't always pull the trigger.
Gut lining damage and dysbiosis
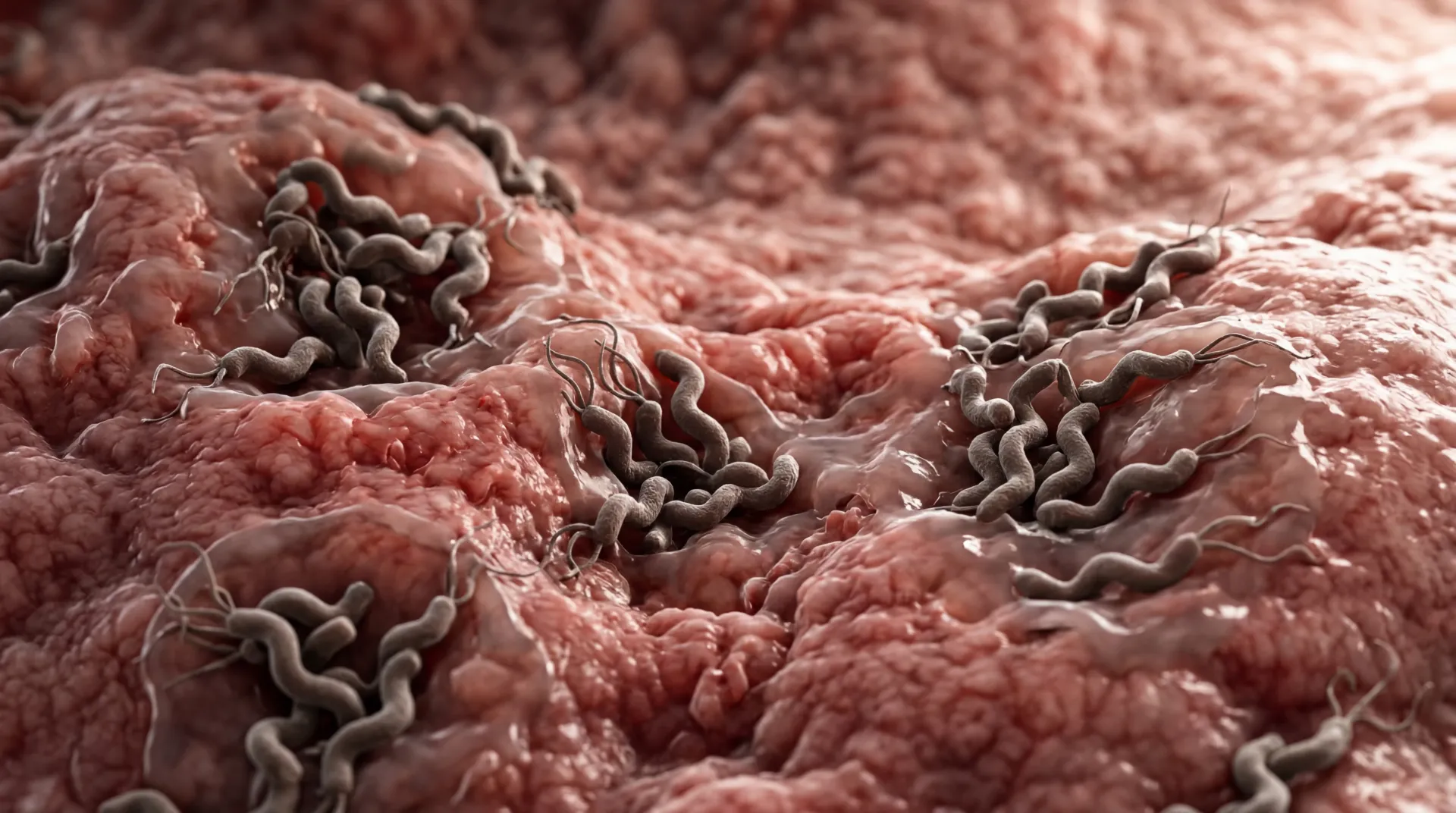
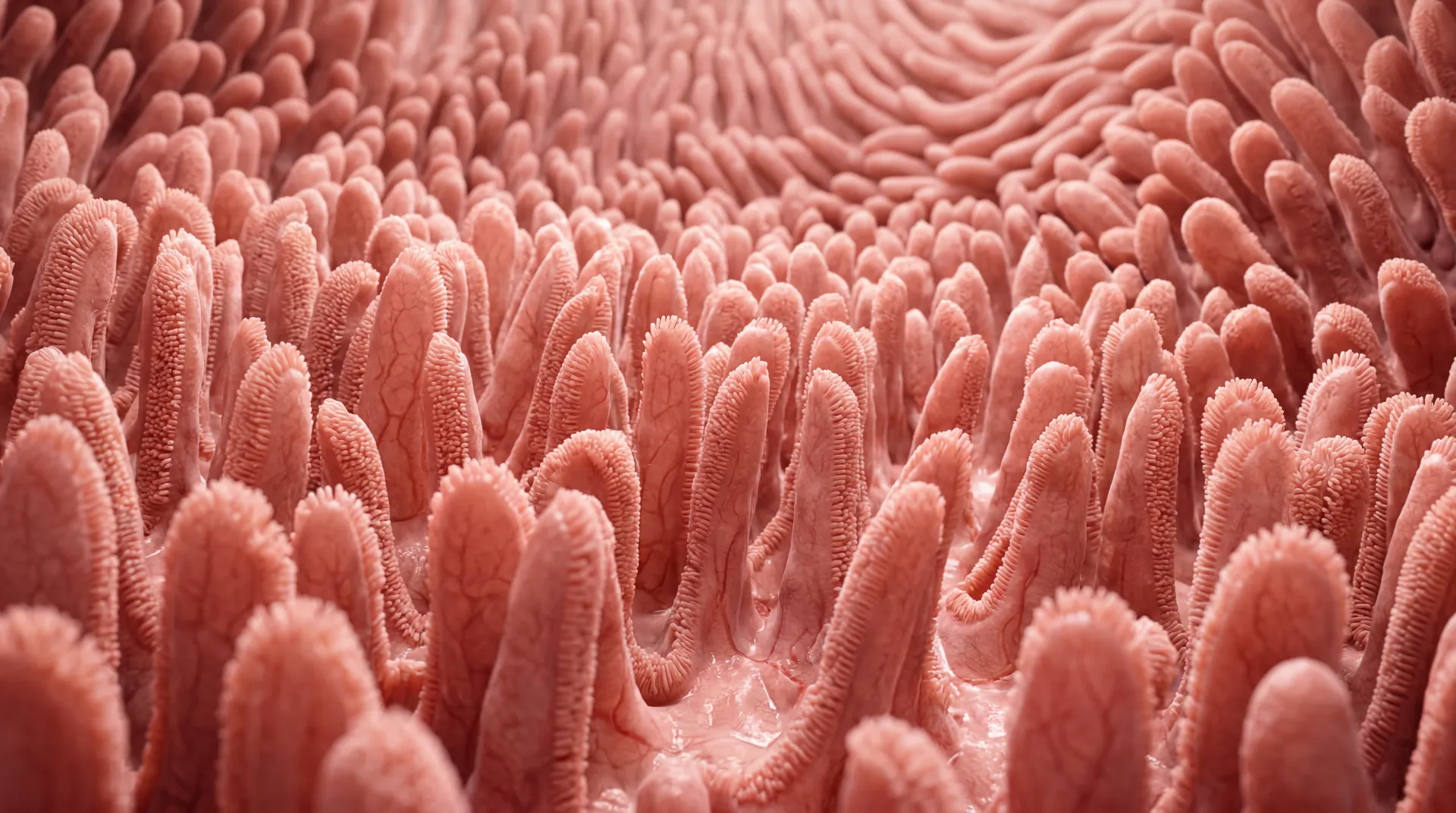
DAO is produced by mature enterocytes — the cells lining your upper small intestine. Anything that damages those cells reduces your DAO output. Conditions like leaky gut syndrome, celiac disease, inflammatory bowel disease, and chronic infections (particularly H. pylori) can all suppress DAO production. Schnedl and Enko's 2021 review in Nutrients found that histamine intolerance appeared in 55% of celiac patients who weren't responding to a gluten-free diet — which points to unresolved gut damage keeping their DAO suppressed even after removing gluten.
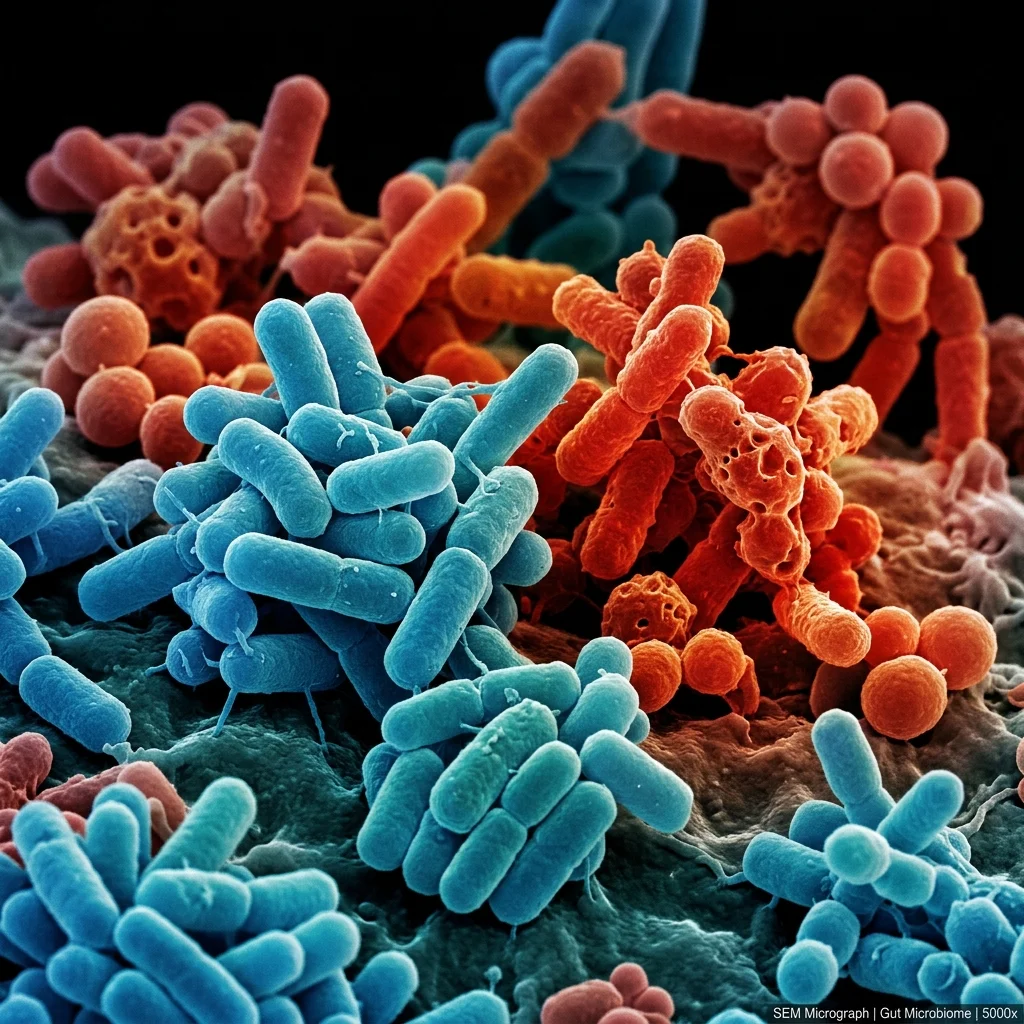
Gut bacteria add another layer. A 2022 study by Sánchez-Pérez and colleagues compared the intestinal microbiota of 12 histamine-intolerant patients against 14 healthy controls. The HIT group showed dramatically elevated levels of histamine-producing bacteria — Staphylococcus was 7-fold higher, Proteus 1.8-fold higher . Meanwhile, protective species like Faecalibacterium prausnitzii (a major butyrate producer that maintains intestinal barrier integrity) were significantly depleted.
Medications that block DAO
This is the cause people miss most often. Approximately 20% of Europeans regularly use medications that inhibit DAO activity. The list includes common painkillers (aspirin, ibuprofen), certain antibiotics, antidepressants, antihypertensives, and antifungals. The blood pressure medication verapamil is one of the most potent DAO inhibitors identified. If you're taking any of these drugs and experiencing unexplained symptoms after eating, the medication itself may be part of the problem.
| DAO Suppression Cause | Mechanism | Reversible? |
|---|---|---|
| Genetic SNPs (AOC1 gene) | Enzyme produced with reduced activity | No, but manageable with diet and supplementation |
| Gut lining damage | Fewer enterocytes producing DAO | Yes, with gut healing interventions |
| Intestinal dysbiosis | Excess histamine-producing bacteria + mucosal inflammation | Yes, with dietary and microbiome restoration |
| DAO-inhibiting medications | Drug compounds directly block enzyme function | Yes, if medication can be adjusted |
| Nutrient deficiencies (vitamin C, copper, B6) | Missing cofactors required for DAO function | Yes, with targeted supplementation |
92% of Patients Report This as Their Top Symptom
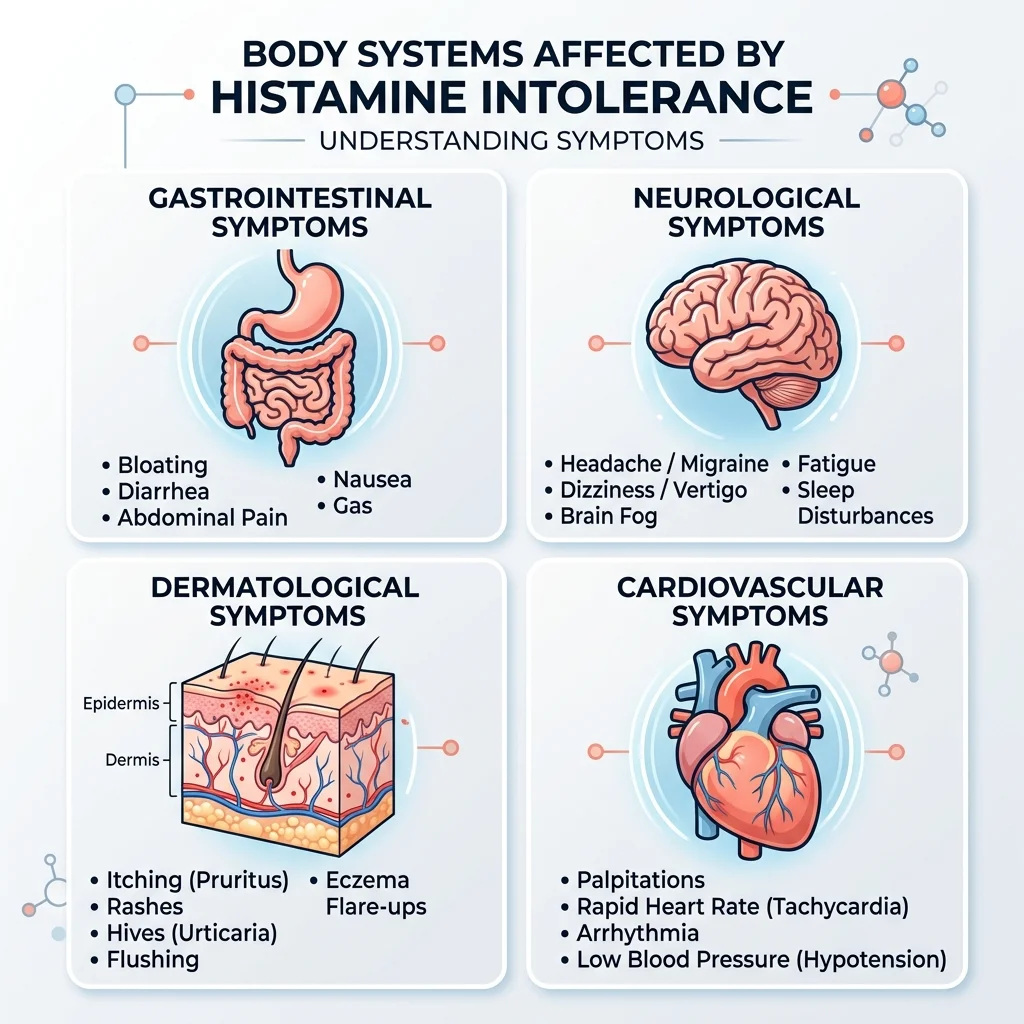
Histamine intolerance is frustrating to diagnose partly because it hits nearly every organ system. The same molecule that makes your nose run during allergy season also regulates your gut motility, blood pressure, and brain function. When it accumulates, the symptom list can look chaotic.
A 2024 review of 133 patients published in Nutrients documented the most common presentations and their severity ratings:
| System | Symptom | Prevalence | Severity (0-5) |
|---|---|---|---|
| Gastrointestinal | Bloating | 92% | 4/5 |
| Gastrointestinal | Postprandial fullness | 73% | 3/5 |
| Gastrointestinal | Diarrhea | 71% | 3/5 |
| Gastrointestinal | Abdominal pain | 68% | 3/5 |
| Neurological | Dizziness | 66% | 3/5 |
| Neurological | Headache/migraine | 65% | 3/5 |
| Gastrointestinal | Constipation | 55% | 2/5 |
| Dermatological | Itching (pruritus) | 48% | 2/5 |
| Cardiovascular | Palpitations | 47% | 2/5 |
Bloating dominates. At 92% prevalence with a severity rating of 4 out of 5, it's the hallmark complaint. But notice how the symptoms span the gut, brain, skin, and heart — which is exactly why HIT gets missed so often. People end up visiting a gastroenterologist for the bloating, a neurologist for the migraines, and a dermatologist for the rashes, never connecting the dots.
The overlap with other conditions is significant. Research from Schnedl and Enko found that 80% of IBS patients identified food and histamine as triggers for their symptoms. The migraine connection is even more pronounced: one analysis found DAO deficiency in roughly 90% of migraine patients. And 63% of HIT patients reported the combination of bloating and headache together, a pairing that should raise clinical suspicion.
There's a hormonal angle here as well. DAO levels fluctuate across the menstrual cycle, with higher activity during the luteal phase and lower activity during the follicular phase. This helps explain why some women experience worsening symptoms at certain points in their cycle — and why histamine intolerance is diagnosed more frequently in women.
Foods That Drive Histamine Up — and Safer Swaps
Histamine in food isn't static. It accumulates over time as bacteria convert the amino acid histidine into histamine through fermentation, aging, and improper storage. One fact that shapes everything about a low-histamine diet: once histamine forms in food, it cannot be removed. Not by cooking, not by freezing, not by any processing method. Prevention is the only strategy.
This means freshness matters more than almost any other dietary variable. The same piece of fish that's perfectly safe when eaten fresh from the market could trigger symptoms after sitting in your fridge for two days. Grilling produces more histamine than steaming or braising, and restaurant meals are inherently riskier because you can't control how long ingredients have been stored or at what temperature.
| Category | High Histamine (Avoid or Limit) | Low Histamine (Generally Safe) |
|---|---|---|
| Proteins | Aged cheese, cured meats, canned fish, smoked salmon, shellfish | Fresh-cooked chicken, fresh-caught fish (eaten same day), eggs, fresh unprocessed meat |
| Vegetables | Tomatoes, spinach, eggplant, fermented vegetables (sauerkraut, kimchi) | Zucchini, broccoli, carrots, sweet potatoes, leafy greens (excluding spinach) |
| Fruits | Citrus fruits, strawberries, bananas, pineapple, papaya | Blueberries, apples, pears, mangoes, melons |
| Beverages | Red wine, beer, champagne, coffee, energy drinks | Water, herbal tea, fresh fruit juices |
| Other | Chocolate, vinegar, soy sauce, nuts, leftover foods | Fresh bread, rice, honey, olive oil, fresh herbs |
The Cleveland Clinic notes that beyond high-histamine foods, two other categories cause problems: histamine liberators (foods that trigger your body's own mast cells to release stored histamine, like citrus fruits and egg whites) and DAO inhibitors (foods that interfere with your enzyme's function, including alcohol, coffee, and chocolate). Managing all three categories simultaneously is what makes a low-histamine diet so restrictive.
Storage tip: Freeze leftovers immediately after cooking rather than refrigerating them. Bacterial histamine production is minimal at freezer temperatures but continues slowly in the fridge. When thawing, cook the food right away — don't let it sit at room temperature.
The standard clinical protocol follows a phased approach. Jackson and colleagues (2025) describe a four-phase dietary framework: start with four weeks of strict histamine avoidance to establish a symptom baseline, then progress through controlled reintroduction of small portions, larger portions, and finally histamine-releasing and DAO-inhibiting foods. The goal isn't permanent restriction. It's identifying your individual threshold so you can eat as broadly as possible without triggering symptoms.
This diet requires professional supervision. Because of its restrictiveness, it carries real risks of nutritional deficiency and is explicitly contraindicated for anyone with a history of eating disorders. Work with a registered dietitian who understands histamine intolerance, not a generic elimination diet template from the internet.
Rebuilding the Gut Environment That Keeps Histamine in Check
If histamine intolerance originates in the gut — and the evidence increasingly supports this — then long-term management has to go beyond avoiding trigger foods. The real work is repairing the intestinal environment where DAO gets produced and where histamine-generating bacteria live.
What the microbiome research shows
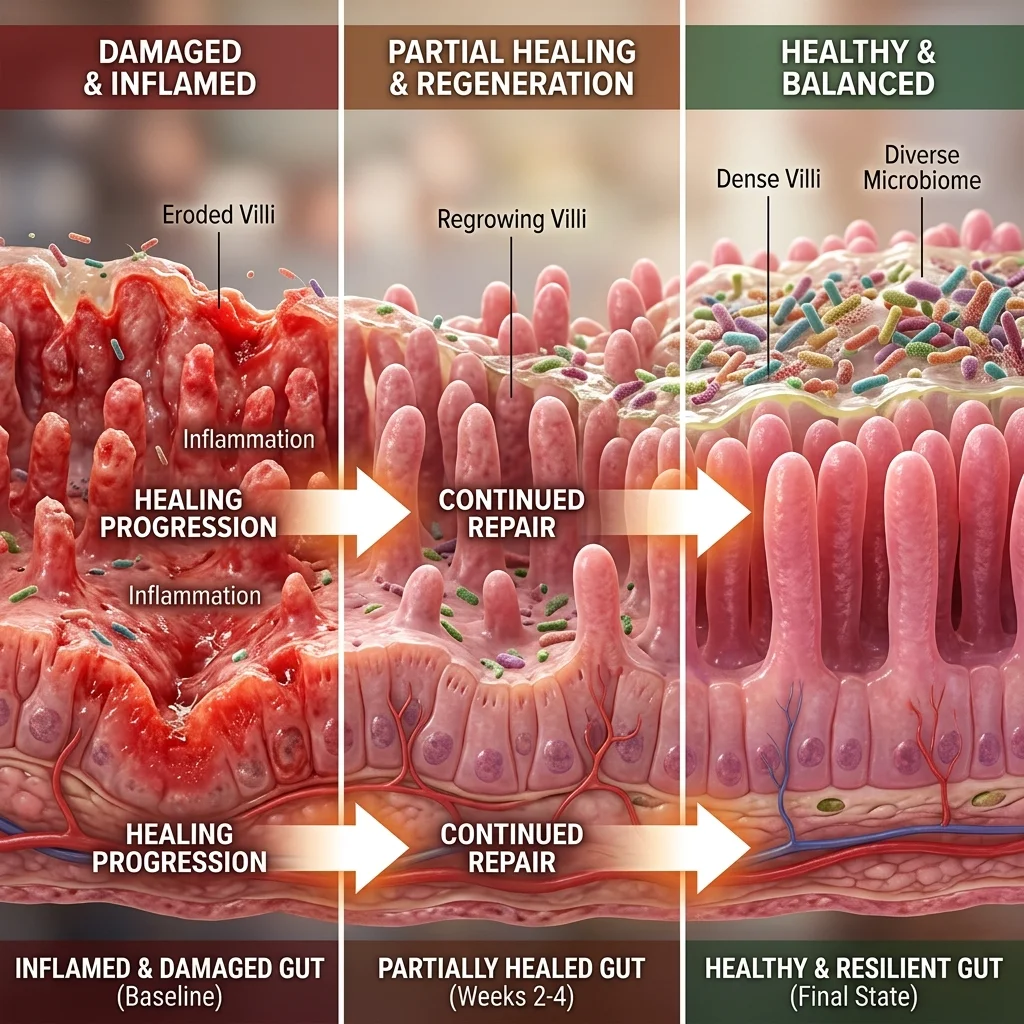
A 2022 pilot study at the University of Barcelona offers some of the clearest evidence for gut-level recovery. Sánchez-Pérez and colleagues tracked five women with confirmed HIT through nine months of low-histamine diet plus DAO supplementation, sequencing their gut bacteria at baseline, 2 months, 6 months, and 9 months. What they found: histamine-producing bacteria like Proteus and Morganellaceae were completely eliminated by month 6, while beneficial Roseburia species — which produce short-chain fatty acids that maintain intestinal barrier integrity — increased steadily throughout treatment.
Gastrointestinal symptoms predominantly resolved by month 2, and by month 9, three of the five patients showed microbiota compositions that resembled healthy controls. That matters because it tells us gut dysbiosis isn't necessarily a permanent state. With the right dietary intervention sustained over months, the bacterial ecosystem can shift back toward something closer to normal.
DAO supplementation: what the trials say
When dietary changes alone aren't enough, exogenous DAO supplementation offers additional support. The enzyme works locally in the intestine, it is not absorbed into the bloodstream, and directly degrades histamine before it can cross the intestinal wall.
Schnedl and colleagues ran a controlled trial with 28 HIT patients receiving DAO capsules (derived from porcine kidney extract) three times daily before meals for four weeks. All 22 measured symptoms improved significantly (p<0.0001). Abdominal pain prevalence dropped from 68% to 25%. When supplementation stopped, symptoms returned but didn't reach their original severity, suggesting some intestinal mucosal recovery had occurred during the treatment period.
A separate study by Manzotti and colleagues found that 13 of 14 patients (93%) reported symptomatic improvement with DAO supplementation, and that combining dietary modification with supplementation produced better quality-of-life outcomes than diet alone.
Newer formulations combining DAO with vitamin C appear more effective. Research published in the International Journal of Molecular Sciences found that DAO supplements formulated with vitamin C showed greater histamine-degrading capacity than DAO alone, because vitamin C helps break down the hydrogen peroxide generated as a byproduct of histamine degradation.
Supporting DAO with the right nutrients
DAO doesn't work in isolation. It requires specific cofactors to function optimally, and deficiencies in any of them can mimic or worsen histamine intolerance even if your underlying DAO genetics are fine. Vitamin C, copper, zinc, and vitamin B6 all serve as DAO cofactors. If you're investigating histamine intolerance, checking your levels of these micronutrients is a practical first step that's often overlooked.
The connection between gut health and chronic inflammation also matters here. Mucosal inflammation from any source (dysbiosis, food sensitivities, ongoing infections) damages the enterocytes that produce DAO. Getting at those underlying inflammatory triggers, rather than just managing the histamine coming in, is the difference between temporary relief and actual progress.
Myth vs. Fact: What Gets Misunderstood About Histamine Intolerance
| Myth | Fact |
|---|---|
| A low DAO blood test confirms histamine intolerance | A 2023 population study of 1,051 adults found that 44% of healthy people had DAO below the standard 10 U/mL cutoff with no symptoms. Blood DAO levels don't reliably correlate with intestinal DAO activity. The test can support a diagnosis but can't confirm one alone. |
| Histamine intolerance is just a food allergy | HIT is a non-immunological, non-IgE-mediated reaction. It's an enzyme capacity problem, not an immune response to a specific protein. Allergy tests will come back negative. |
| You need to avoid high-histamine foods forever | The goal of a low-histamine diet is to identify your personal threshold, not to eliminate foods permanently. The phased reintroduction protocol exists precisely because many people can tolerate moderate histamine once their gut has healed and their DAO function has improved. |
| Only fermented foods cause problems | Histamine liberators (citrus, egg whites, chocolate) and DAO inhibitors (alcohol, coffee) also contribute. The total histamine load from all three categories is what matters, not just the histamine content of a single food. |
| Antihistamines are the best treatment | H1 and H2 blockers can help with acute symptoms, but some antihistamines (notably cimetidine) actually inhibit DAO activity — potentially making the underlying problem worse. Dietary management and DAO supplementation address the root mechanism more directly. |
| Histamine intolerance is an officially recognized diagnosis | The American Academy of Allergy and Immunology does not currently recognize HIT as an official diagnosis. Diagnostic criteria are not standardized, and no single validated biomarker test exists. Diagnosis relies on clinical history plus response to dietary intervention. |
Frequently Asked Questions
How do I know if I have histamine intolerance or a food allergy?
Food allergies involve an IgE-mediated immune reaction to a specific protein and can be confirmed through skin prick tests or blood tests. Histamine intolerance produces negative allergy test results because the mechanism is different — it's an enzyme deficiency, not an immune response. If you're reacting to a wide variety of unrelated foods (aged cheese, wine, tomatoes, canned fish) rather than one specific food group, and your allergy tests are negative, histamine intolerance is worth investigating with your doctor. A four-week elimination diet followed by controlled reintroduction is the current diagnostic standard.
Can histamine intolerance be cured, or is it permanent?
It depends on the underlying cause. If your DAO deficiency stems from genetic SNPs, you'll likely need ongoing dietary management and potentially lifelong supplementation. But if the cause is gut dysbiosis, medication side effects, or a treatable condition like H. pylori infection or celiac disease, restoring gut health can substantially improve or resolve your symptoms. The Barcelona pilot study showed that nine months of dietary treatment normalized microbiota composition in 3 of 5 patients, suggesting meaningful recovery is possible when the root cause is addressed.
Is DAO supplementation safe, and does it actually work?
Multiple clinical trials, including a double-blind placebo-controlled study of 39 patients, have demonstrated significant symptom reduction with oral DAO supplements. The enzyme works locally in the intestine and is not absorbed into the bloodstream, which limits systemic side effects. Most formulations derive from porcine kidney extract and are taken 15-20 minutes before meals. However, quality and potency vary between brands, and the evidence base still consists mostly of small trials. Talk to your healthcare provider before starting supplementation.
Why do my symptoms get worse around my period?
DAO activity is influenced by estrogen levels and fluctuates across the menstrual cycle. Research shows DAO levels are higher during the luteal phase (after ovulation) and lower during the follicular phase (leading up to and during menstruation). At the same time, estrogen increases mast cell reactivity, which can boost endogenous histamine release. That combination of less clearance capacity and more histamine production explains why many women with HIT notice symptom flares around menstruation.
What should I eat on a low-histamine diet?
Focus on fresh, unprocessed foods eaten as close to preparation time as possible. Safe staples include freshly cooked chicken and meat, same-day-caught fish, rice, bread, eggs, most fresh vegetables (except tomatoes, spinach, and eggplant), blueberries, apples, pears, olive oil, fresh herbs, and herbal teas. The principle is freshness — the longer food sits, the more histamine bacteria produce. Freeze leftovers immediately rather than refrigerating them, and favor steaming or braising over grilling. A registered dietitian can help you build a balanced, individualized meal plan that avoids unnecessary restriction.
Related Articles
- Leaky Gut Syndrome: Symptoms, Causes, and Evidence-Based Healing — Intestinal permeability is a key factor in both DAO production and histamine absorption from the gut.
- SIBO: Symptoms, Testing, and Treatment — Small intestinal bacterial overgrowth shares significant symptom overlap with histamine intolerance and may contribute to gut-derived histamine production.
- The Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition — Understanding the microbiome's role in brain function helps explain the neurological symptoms of histamine overload.
- Inflammation, Chronic Disease, and Anti-Inflammatory Living — Chronic gut inflammation suppresses DAO production and drives the cycle of histamine intolerance.
- H. Pylori: Symptoms, Natural Eradication, and Recovery — H. pylori infection can directly contribute to histamine dysregulation through its effects on gastric histamine signaling.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.