The Three "Biotics" Your Gut Depends On
Walk into any health food store and you will see shelves of supplements stamped with "probiotic," "prebiotic," or the newer buzzword, "postbiotic." The labels blur together, and the marketing does not help. Yet these three categories do genuinely different things inside your body, and understanding the distinction matters more than picking whichever bottle has the highest billion-count number on the front.
The simplest way to sort them out: probiotics are live microorganisms you swallow. Prebiotics are what those microorganisms eat once they arrive. And postbiotics are the beneficial compounds those microorganisms produce after they have finished eating. All three operate on the same roughly 25 feet of intestinal real estate we casually call "the gut," but they each pull a different lever.
The International Scientific Association for Probiotics and Prebiotics (ISAPP) has published formal definitions for all three, and researchers are still refining where one category ends and another begins. This guide breaks down how each one works, what the clinical evidence supports, and how to use all three without spending half your paycheck on supplements.
Your Gut Ecosystem: 100 Trillion Reasons to Pay Attention
To make sense of any biotic, you first need to know the neighborhood. Your gastrointestinal tract hosts more than 100 trillion microorganisms spanning over 1,000 bacterial species, plus viruses, fungi, and other microbial residents. About 90 percent of those bacteria belong to two major phyla: Firmicutes and Bacteroidetes. Together, they form a living ecosystem that scientists now refer to as the gut microbiome.
This ecosystem is not just along for the ride. Gut bacteria synthesize vitamins your cells cannot make on their own, ferment dietary fibers into short-chain fatty acids that fuel your colon lining, train your immune system to distinguish friend from foe, and communicate with your brain through what researchers call the gut-brain axis. When that ecosystem falls out of balance, a state called dysbiosis, the consequences can range from digestive discomfort to systemic inflammation linked to cardiovascular disease, obesity, type 2 diabetes, and even mood disorders.
Quick fact: Your gut microbiome contains more microbial cells than your entire body has human cells, and the collective genetic material of those microbes outnumbers your own genome by roughly 150 to 1.
The bottom line: the composition and diversity of your gut bacteria matters far more than any single supplement. Probiotics, prebiotics, and postbiotics give you three different ways to shift that composition, each through its own mechanism.
Probiotics: The Living Reinforcements
Probiotics are defined by the ISAPP as "live microorganisms that, when administered in adequate amounts, confer a health benefit on the host." The key word is live. For a product to count as a true probiotic, the organisms inside it must survive the journey through stomach acid and bile, arrive in the colon still viable, and then exert a measurable positive effect.
The most commonly used probiotic genera are Lactobacillus (recently reclassified into several new genera in 2020), Bifidobacterium, and the yeast Saccharomyces boulardii. But here is a detail that supplement marketing often glosses over: different strains within the same species can have completely different effects. A specific strain of Lactobacillus rhamnosus might reduce the risk of atopic dermatitis in infants, while a different strain of the same species does nothing at all for that condition.
What the Clinical Evidence Shows
Probiotic research has produced a mosaic of results, partly because studies use different strains, doses, and patient populations. Still, certain findings have emerged with reasonable consistency:
| Condition | Evidence Strength | Key Findings |
|---|---|---|
| Antibiotic-associated diarrhea | Strong | Multiple meta-analyses show reduced risk, particularly with Saccharomyces boulardii and Lactobacillus rhamnosus GG |
| Atopic dermatitis prevention | Moderate | A meta-analysis of 27 RCTs (6,907 infants) found probiotic exposure reduced risk from 34.7% to 28.5% |
| Irritable bowel syndrome | Moderate | Symptom improvement reported with specific multi-strain formulations |
| Acute infectious diarrhea (pediatric) | Moderate | Some strains reduce duration by approximately 1 day |
| Inflammatory bowel disease | Mixed | More promise in ulcerative colitis maintenance than Crohn's disease |
An important safety note: the FDA has warned that cases of severe or fatal infections have been reported in premature infants given probiotics. For most healthy adults, side effects are rare and typically limited to mild gas or bloating, but anyone with a compromised immune system should consult a physician before starting supplementation.
Food Sources vs. Supplements
You do not need a capsule to get probiotics. Fermented foods like yogurt (with live active cultures), kefir, sauerkraut, kimchi, and traditionally fermented foods deliver probiotics alongside other nutrients. However, not all fermented foods qualify as probiotic. Sourdough bread, commercial pickles, and most shelf-stable sauerkraut are processed after fermentation and no longer contain live cultures when you eat them.
Supplement dosages typically range from 1 to 50 billion colony-forming units (CFU) per dose. Contrary to what label comparisons suggest, higher CFU counts are not necessarily more effective than lower ones. What matters more is matching the specific strain to the health outcome you are targeting and ensuring viability at the time of consumption, not just at the time of manufacture.
Prebiotics: Feeding the Good Guys
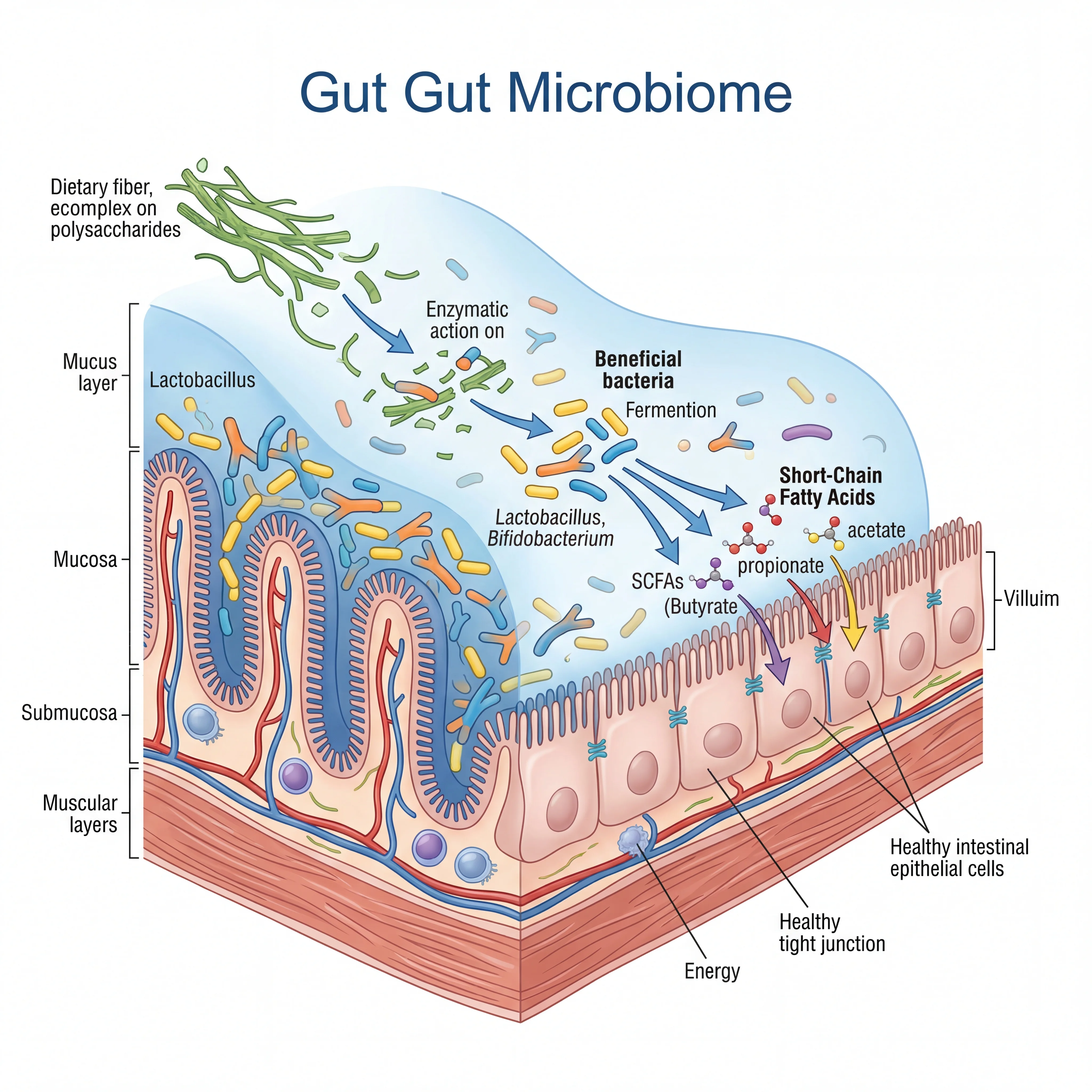
If probiotics are the seeds you plant in a garden, prebiotics are the fertilizer. Prebiotics are non-digestible food components, most often certain types of dietary fiber, that selectively stimulate the growth and activity of beneficial bacteria already living in your colon. Your own digestive enzymes cannot break them down, so they pass through the stomach and small intestine intact and arrive in the large intestine ready to be fermented by your resident microbes.
That fermentation process generates short-chain fatty acids (SCFAs), chiefly butyrate, acetate, and propionate. These molecules do far more than you might expect from simple bacterial waste products. Research published in Biomolecules documented that SCFAs accelerate healing and regeneration of the intestinal lining, increase mucus production, maintain healthy colonic pH to suppress pathogen growth, and even improve the absorption of minerals like calcium, iron, and magnesium.

The Three Main Types of Prebiotics
| Prebiotic Type | How It Works | Top Food Sources |
|---|---|---|
| Resistant starches | Resist digestion and reach the colon intact, where fermentation produces primarily butyrate | Boiled and cooled potatoes, green bananas, oats, barley, beans, legumes |
| Inulin | A soluble fiber fermented by Bifidobacteria; promotes satiety, supports regularity, and may lower LDL cholesterol | Chicory root, garlic, Jerusalem artichokes, leeks, onions, asparagus, dandelion greens |
| Pectin | A gel-like polysaccharide with antioxidant properties; strengthens intestinal lining cells and broadens microbial diversity | Apples (especially raw with pulp), apricots, carrots, raspberries, tomatoes |
Prebiotics occur naturally in over 36,000 plant-based foods, which means a varied diet rich in fruits, vegetables, and whole grains will deliver meaningful amounts without supplementation. However, the average American falls well short of the 25 to 35 grams of daily fiber that gut bacteria need to thrive, which is one reason prebiotic supplements have gained traction.
Practical Tips for Adding Prebiotics
Introducing prebiotics too aggressively can backfire. As your gut microbes ramp up fermentation, gas production increases, potentially causing bloating and discomfort. Start gradually: add one or two new prebiotic-rich foods per week. Your gut microorganisms are also more metabolically active during daylight hours, so eating fiber-rich meals earlier in the day can improve tolerance. If you have IBS, stone fruits like peaches and mangoes may be harder to handle, so focus on root vegetables, oats, and legumes instead.
Postbiotics: The Finished Products Your Body Actually Uses
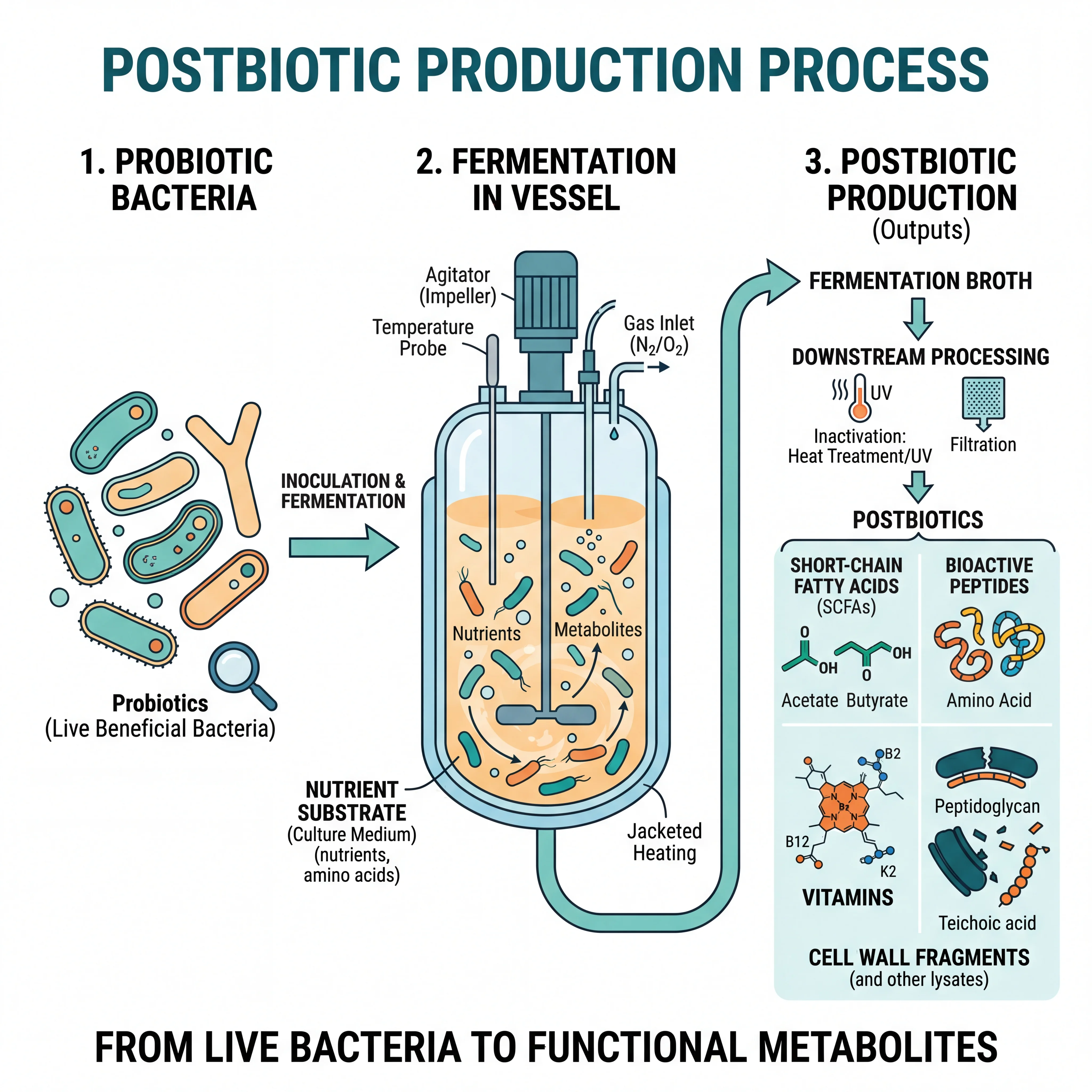
Postbiotics are the newest member of the biotics family, and their formal definition was only established by ISAPP in 2021. The consensus panel defined postbiotics as "preparations of inanimate microorganisms and/or their components that confer a health benefit on the host." That definition is broader than many people expect. It includes not just metabolic byproducts but also dead bacterial cells, cell wall fragments, and enzymes, as long as they deliver a measurable health benefit.
Think of it this way: when you eat yogurt, the live bacteria (probiotics) feed on the lactose and fiber you have consumed (prebiotics acting as fuel) and produce lactic acid, SCFAs, vitamins, and other bioactive compounds. Those end products are the postbiotics. Your body was benefiting from postbiotics long before anyone coined the term.
Key distinction: Probiotics must be alive to work. Postbiotics, by definition, do not contain live microorganisms. This makes them inherently more shelf-stable, easier to standardize, and potentially safer for vulnerable populations like immunocompromised patients or premature infants.
What Postbiotics Include
| Postbiotic Category | Examples | Known or Emerging Benefits |
|---|---|---|
| Short-chain fatty acids | Butyrate, acetate, propionate | Fuel colon cells, regulate inflammation, strengthen gut barrier, improve mineral absorption |
| Bioactive peptides | ACE-inhibitory peptides from L. helveticus | Blood pressure reduction, lipid metabolism modulation |
| Exopolysaccharides | Complex sugars secreted by bacteria | Immune modulation, anti-inflammatory effects |
| Bacterial lysates | Broken-down bacterial cell components | Immune stimulation, used in some respiratory infection therapies |
| Enzymes | Bacterial enzymes surviving fermentation | Improved digestion, nutrient bioavailability |
| Vitamins | B12, B2, B6, folate, vitamin K | Metabolic support, coagulation, energy production |
| Cell-free supernatants | Liquid fraction after removing bacterial cells | Antimicrobial activity, gut barrier reinforcement |
Why Researchers Are Excited About Postbiotics
What makes postbiotics interesting is that their effects go well beyond the gut. A 2020 review in Nutrients catalogued their range: they can modulate immune cell balance (specifically the Th1/Th2 ratio), reduce inflammation, act as antioxidants, and in some lab settings show anti-cancer activity. A separate 2025 study in Frontiers in Microbiomes reported something unexpected: postbiotic metabolites can boost how well your body absorbs certain drugs. One finding showed a 4.3-fold increase in lurasidone bioavailability and a 269.9 percent bump for omeprazole.
In clinical settings, postbiotic preparations have shown promise for strengthening the gut barrier, managing IBS symptoms, reducing eczema severity, and easing infant colic. One study found that adults with IBS who followed a postbiotic regimen experienced significant improvements in bowel movement frequency, bloating, and pain after just four weeks.
There is a practical angle too. Postbiotics do not need to be kept alive, which sidesteps the cold-chain logistics and expiration headaches that make probiotic manufacturing so tricky. You can standardize them to exact concentrations, dose them precisely, and they carry essentially no infection risk. That last point matters given the FDA warnings about probiotic use in premature infants and immunocompromised patients.
Head-to-Head: How All Three Compare
Most of the confusion comes from the fact that these three are deeply connected. Prebiotics feed probiotics. Probiotics generate postbiotics. They are different chapters of the same process, but each one has practical quirks worth knowing about.
| Feature | Probiotics | Prebiotics | Postbiotics |
|---|---|---|---|
| What they are | Live microorganisms | Non-digestible food components (fiber) | Inactivated microbes and/or their metabolites |
| Must be alive? | Yes | N/A (not organisms) | No |
| Primary mechanism | Colonize gut, produce metabolites, compete with pathogens | Selectively feed beneficial bacteria | Directly deliver bioactive compounds |
| Shelf stability | Low to moderate (some need refrigeration) | High (stable fibers) | High (no live organisms) |
| Safety profile | Generally safe; caution in immunocompromised | Very safe; gradual introduction advised | Very safe; no infection risk |
| Best food sources | Yogurt, kefir, kimchi, sauerkraut, kombucha | Garlic, onions, bananas, oats, chicory root | Fermented foods (byproducts of fermentation) |
| Supplement form | Capsules, powders (CFU-based) | Fiber powders (inulin, FOS, GOS) | Emerging; some butyrate and lysate supplements |
| Research maturity | Decades of studies; well-established | Well-established for fiber; growing for specific types | Newest field; rapidly expanding since 2021 |
Common Myths and Realities
One persistent myth is that you need to choose between these three. In reality, they form a cooperative system. Eating a high-fiber meal (prebiotics) while consuming yogurt (probiotics) leads to greater SCFA production (postbiotics) than either intervention alone. This is the principle behind synbiotics, products that intentionally combine probiotics with their preferred prebiotic fuel source.
Another myth is that more CFUs always mean a better probiotic. The NIH Office of Dietary Supplements is explicit on this point: products with 50 billion CFU are not inherently superior to those with 5 billion. The strain, the condition you are targeting, and whether the organisms are still viable when you take them matter far more than raw numbers.
A third misconception holds that postbiotics are just "dead probiotics" and therefore inferior. The ISAPP definition makes clear that the health benefit must be demonstrated for the postbiotic preparation itself. A dead bacterium with no measurable effect is not a postbiotic; it is simply a dead bacterium. When the right inactivated strains or metabolites are used, postbiotics can deliver effects that rival or complement their living counterparts.
Putting It All Together: Building a Biotic-Rich Routine
No single supplement is going to transform your gut. The better approach is layering all three biotics through the food you already eat and, when there is a clear reason, adding targeted supplements. Below is a practical framework.
Step 1: Build a Prebiotic Foundation Through Food
Start with your plate. Aim for 25 to 35 grams of fiber daily from a variety of sources: whole grains, legumes, vegetables, and fruits. The more diverse your fiber intake, the more diverse your gut microbiome becomes. Specific targets include garlic and onions (inulin), oats and cooled potatoes (resistant starch), and apples and berries (pectin). This alone will naturally increase postbiotic production in your gut.
Step 2: Add Probiotic-Rich Foods Regularly
Incorporate fermented foods that still contain live cultures: yogurt with documented strains, fresh sauerkraut from the refrigerated section, kefir, kimchi, or kombucha. Research from Stanford University has shown that a diet high in fermented foods increases microbial diversity and reduces markers of systemic inflammation more effectively than a high-fiber diet alone.
Step 3: Consider Targeted Supplementation When Needed
Supplements fill gaps that food cannot always cover. If you are taking antibiotics, Saccharomyces boulardii or Lactobacillus rhamnosus GG have the strongest evidence for preventing associated diarrhea. If you want a postbiotic specifically, butyrate supplements (often sold as tributyrin) can deliver this SCFA directly to the colon. Spore-forming probiotics like Bacillus coagulans survive shelf storage and stomach transit better than many conventional strains.
Step 4: Mind the Timing and Transitions
Your gut microbes follow circadian patterns, with higher metabolic activity during daylight hours. Eating your highest-fiber meals earlier in the day can improve tolerance and SCFA production. When increasing fiber or starting a new probiotic, give your system two to three weeks to adjust before judging whether the intervention is working.
Frequently Asked Questions
Can you take probiotics and prebiotics at the same time?
Yes, and doing so may be more effective than taking either one alone. When a probiotic is paired with its preferred prebiotic fuel source, the probiotic is more likely to survive transit and colonize the gut successfully. Products that combine both are called synbiotics. You can also achieve this naturally by eating yogurt (probiotic) with oats or bananas (prebiotic) in the same meal.
Are postbiotics safer than probiotics?
For most healthy adults, both are considered safe. However, postbiotics carry an inherently lower risk because they do not contain live microorganisms. This makes them a potentially better option for people with weakened immune systems, critical illness, or premature infants, groups for whom live probiotics have occasionally caused serious infections. If you fall into a higher-risk category, discuss options with your physician.
Do I need supplements, or can I get enough from food?
For many people, a varied diet rich in fiber (25 to 35 grams daily) and fermented foods provides adequate prebiotics and probiotics without supplementation. The challenge is that most Americans consume only about 15 grams of fiber per day, well below the recommended range. If your diet consistently falls short, or if you are managing a specific condition like IBS or antibiotic-associated diarrhea, targeted supplements can help fill the gap.
How long does it take for probiotics or prebiotics to work?
Effects vary by individual and condition. Some people notice digestive improvements within a few days, but most clinical trials assess outcomes after four to eight weeks of consistent use. It takes time for new bacterial populations to establish themselves and for SCFA production to reach levels that meaningfully influence gut barrier function and immune signaling.
What foods contain all three biotics at once?
Fermented foods made from high-fiber ingredients come closest. Kimchi, for example, delivers live Lactobacillus strains (probiotics), fiber from the vegetables (prebiotics), and organic acids and other metabolites produced during fermentation (postbiotics). Kefir made with whole grains and yogurt topped with fruit and oats similarly provide overlapping biotic benefits in a single serving.
Related Articles
- Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition — Explores the communication pathways between gut bacteria and your central nervous system.
- Butyrate: The Gut Metabolite That Heals Your Colon and Protects Your Brain — A deep dive into the most studied postbiotic and its wide-ranging health effects.
- Leaky Gut Syndrome: Symptoms, Causes, and Evidence-Based Healing — How intestinal permeability connects to the biotic ecosystem discussed in this guide.
- Akkermansia: The Next-Generation Probiotic for Metabolic Health — Covers one of the most promising individual probiotic strains for metabolic wellness.
- Inflammation and Chronic Disease: A Complete Guide to Anti-Inflammatory Living — The systemic inflammation context that makes gut health interventions so important.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.