A $32.69 Billion Market You're Already Part Of
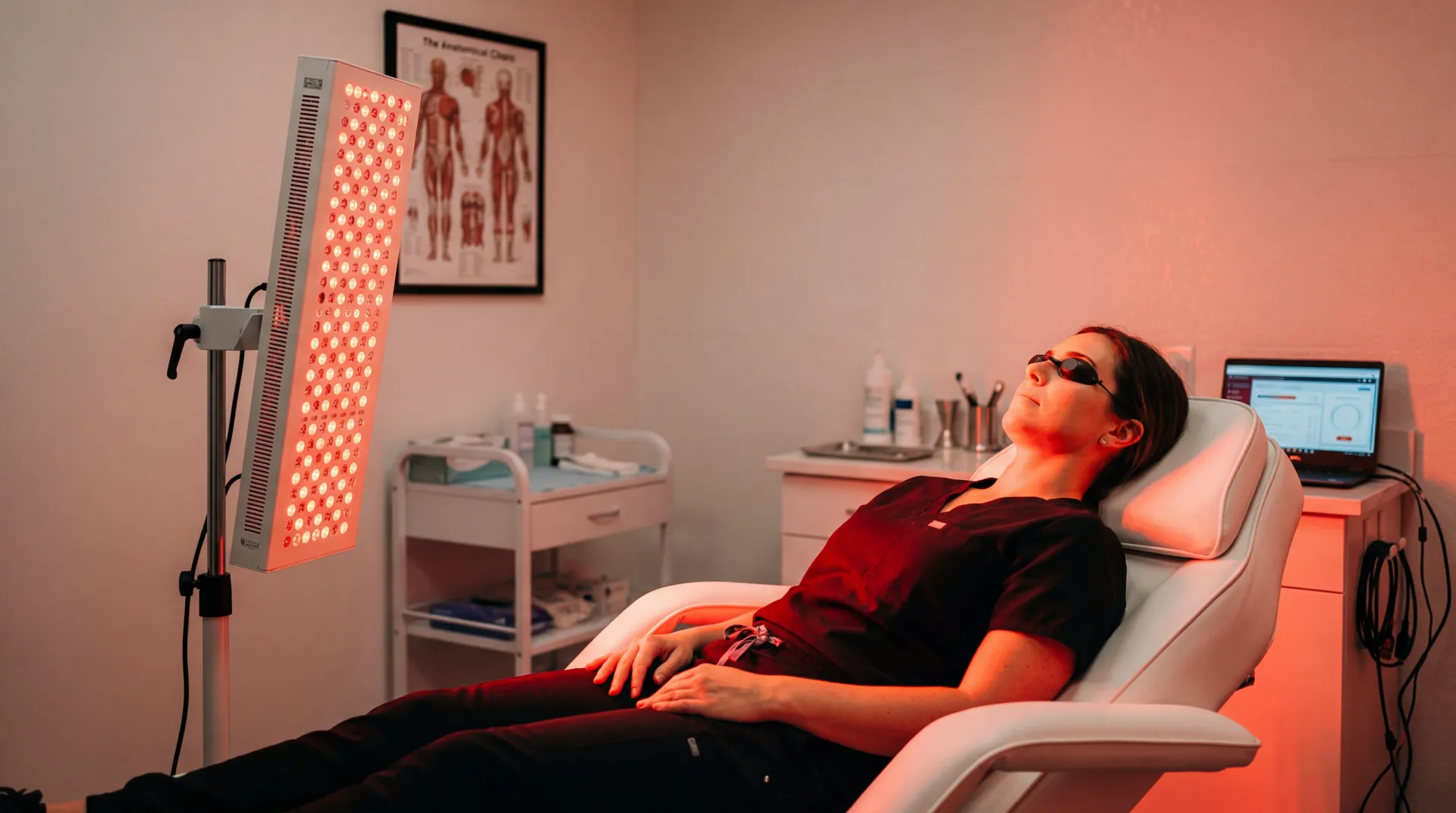
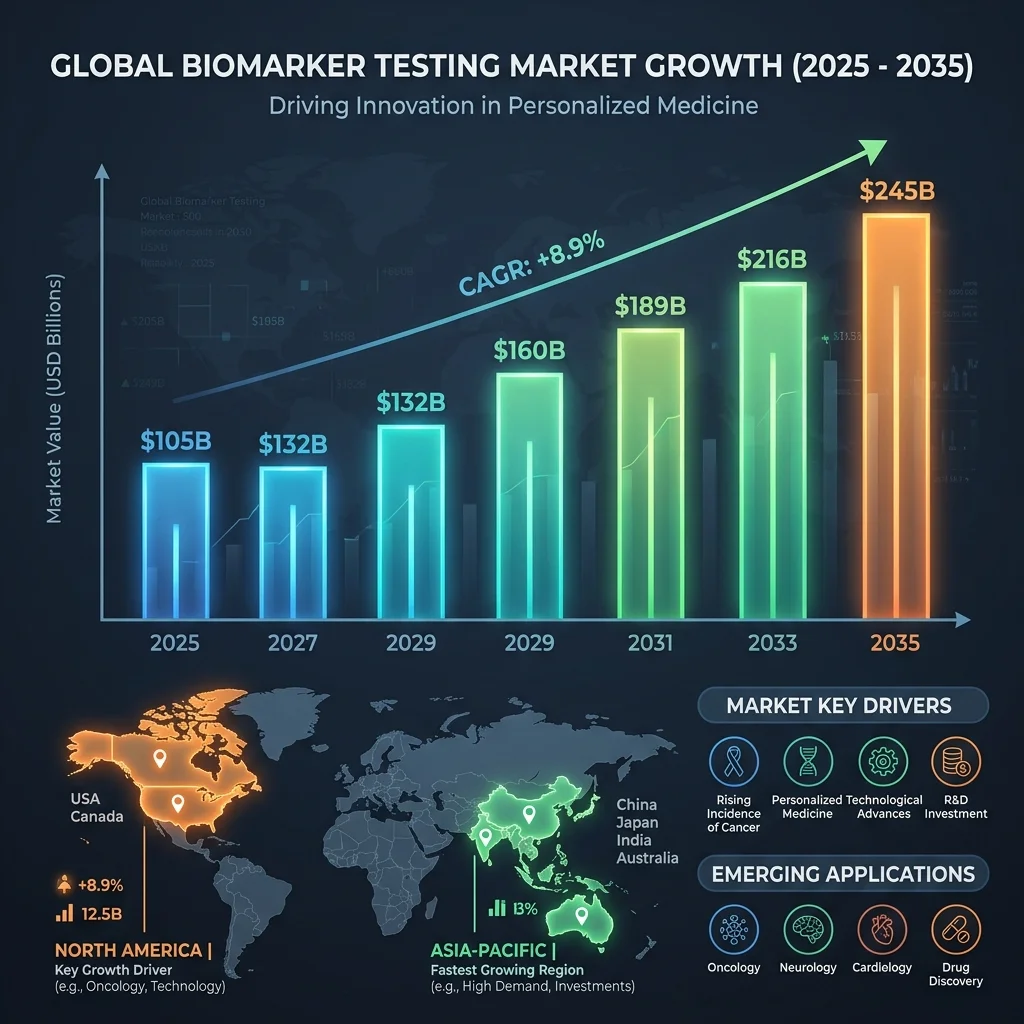
The global biomarker testing market hit $32.69 billion in 2025, and analysts project it will climb to $50.76 billion by 2035. That 4.51% annual growth rate is fueled by millions of people who got tired of waiting for symptoms to tell them something was wrong.
The biomarker testing services segment alone grew from $648.8 million in 2024 to a projected $1.06 billion by 2030, expanding at 8.59% per year. North America commands roughly 42-46% of this market, though Asia-Pacific is sprinting ahead at a 9.60% compound annual growth rate. The fastest-growing applications sit outside oncology (which still holds about 45% of the market): cardiovascular and neurological disorder testing are picking up speed as consumers and clinicians alike recognize that blood-based biomarkers can flag problems years before they become diagnoses.
Multiple demand signals are converging. One in four American adults carries high LDL cholesterol levels, according to the latest ACC/AHA data. The direct-to-consumer wellness testing wave, which exploded during COVID-19, trained an entire generation to see self-testing as normal rather than niche. And the longevity medicine movement has reframed blood work from a reactive diagnostic tool into a proactive optimization strategy.
During the 20th century, lifespan in high-income countries increased by about 30 years. Researchers at Nature Aging now argue that dramatic further gains are unlikely in the 21st century. The new frontier is health span: years spent in good health, not just years spent alive.
That reframing from lifespan to health span is what's driving biomarker testing into mainstream adoption. The real decisions now are which markers to track, how often, and through which platform.
The Seven Blood Markers That Predict Your Future Health
A 2026 study published in Nature Medicine by researchers at the Karolinska Institutet followed more than 2,200 adults over 60 in Stockholm for 15 years. They analyzed 54 blood biomarkers and found that just seven predicted which participants would develop multiple chronic diseases and how quickly those diseases accumulated.
The seven markers: GDF-15, HbA1c, Cystatin C, leptin, insulin, gamma-glutamyl transferase (GGT), and albumin. Five of those (GDF-15, HbA1c, Cystatin C, leptin, and insulin) correlated with every measure of multimorbidity the researchers examined. The remaining two, GGT and albumin, specifically tracked the speed of disease progression over time.
"Our study suggests that disturbances in metabolism, stress responses, and energy regulation are among the main drivers of multimorbidity in older people," said principal investigator Davide Liborio Vetrano, associate professor at Karolinska Institutet. The team validated their results in an independent cohort of 522 participants in the United States.
That finding aligns with earlier work. Toshiko Tanaka and colleagues at the National Institute on Aging analyzed 1,301 plasma proteins in 997 individuals aged 21 to 102 and found that 651 proteins shifted with age. Of those, 33.5% were tied to mortality and 45.3% to multimorbidity. They built a 76-protein proteomic age signature that predicted both chronic disease accumulation and all-cause mortality. GDF-15 appeared in both studies as a key marker, belonging to a family of senescence-associated secretory proteins (SASP) that aging cells release into the bloodstream.
Think of SASP factors like exhaust from a car engine. A young, efficient engine runs clean. As the engine ages, it throws off more byproducts. GDF-15, IL-6, and TIMP1 are the biological equivalent of that exhaust, and measuring them gives you a reading on how hard your cells are working just to maintain normal function.
A separate team developed a 7-biomarker clinical aging clock from 59,741 healthy samples, then validated it across both the NHANES and UK Biobank cohorts. Using only routine blood chemistry markers, this clock predicted the five most common chronic diseases: lipidemias, hypertension, type 2 diabetes, chronic ischemic heart disease, and chronic kidney disease. The clock proved robust even during acute infections, meaning a temporary cold wouldn't throw off your biological age estimate.
For longevity-focused testing, experts group biomarkers into six categories. Michael Doney, M.D., executive medical director at Biograph, and Matt Kaeberlein, Ph.D., CEO of Optispan, told Forbes that cardiovascular markers (lipid panels, ApoB), metabolic markers (fasting glucose, HbA1c, insulin), inflammatory markers (hs-CRP, homocysteine), aerobic capacity (VO2 max), body composition (DEXA scans), and hormonal markers (testosterone, estrogen, DHEA) form the foundation of any serious longevity protocol. Jim LaValle, chief science officer at Life Time, added that the neutrophil-to-lymphocyte ratio (NLR) from a standard complete blood count is emerging as one of the most accessible indicators of "inflammaging," the chronic, low-grade inflammation that accelerates biological aging.
You don't need 1,301 proteins measured to get useful information. Seven to ten well-chosen markers, tracked over time, tell you more about your health trajectory than a single comprehensive panel ever could.

What Your Standard Blood Panel Misses
Most annual physicals include a basic metabolic panel (BMP) or comprehensive metabolic panel (CMP) alongside a lipid panel and complete blood count (CBC). That covers electrolytes, kidney function, blood sugar, liver enzymes, cholesterol fractions, and blood cell counts. For decades, physicians treated this as the standard snapshot of health.
The problem is what it leaves out. The 2026 ACC/AHA Guideline on the Management of Dyslipidemia, published in March in the Journal of the American College of Cardiology, now recommends testing for lipoprotein(a) and apolipoprotein B (ApoB) in addition to standard cholesterol. Harmony R. Reynolds, M.D., director of NYU Langone's Cardiovascular Clinical Research Center, who served on the guideline writing committee, put it plainly: "Cholesterol care isn't one-size-fits-all. These additional tools give us a clearer picture of each patient."
ApoB counts the actual number of atherogenic particles in your blood, which turns out to be a better predictor of arterial plaque than LDL cholesterol alone. Two people can have identical LDL numbers but very different ApoB counts, and the person with more particles faces higher risk. Lp(a) is trickier because it's genetically determined and barely budges with diet or exercise changes. If yours is elevated, you can't lifestyle your way out of it, but knowing early lets you and your physician adjust the overall cardiovascular strategy.
The guideline also introduced a new risk calculator called PREVENT (Predicting Risk of Cardiovascular Disease EVENTs), which estimates both 10-year and 30-year risk for adults ages 30 to 79. That's a departure from previous tools that only looked a decade ahead. "We're shifting from focusing only on 10-year risk to also looking at 30-year risk, recognizing that cardiovascular disease develops over a lifetime," said Dr. Reynolds.
| Test Category | Standard Panel | Advanced Panel | What It Catches |
|---|---|---|---|
| Cardiovascular | Total cholesterol, LDL, HDL, triglycerides | ApoB, Lp(a), coronary calcium score | Hidden particle-level risk, genetic cardiovascular risk |
| Metabolic | Fasting glucose | HbA1c, fasting insulin, HOMA-IR | Insulin resistance years before diabetes diagnosis |
| Inflammatory | Often not included | hs-CRP, homocysteine, NLR | Chronic low-grade inflammation driving aging |
| Hormonal | TSH (sometimes) | Free T3, free T4, testosterone, estradiol, DHEA-S | Subclinical thyroid issues, hormonal aging |
| Nutritional | Rarely included | Vitamin D, B12, folate, ferritin, magnesium, omega-3 index | Deficiencies affecting energy, immunity, cognition |
| Kidney/Liver | Creatinine, BUN, ALT, AST | Cystatin C, GGT, albumin | Earlier kidney decline detection, liver stress beyond enzymes |
The "standard panel" column represents what most insurance-covered annual physicals include. The "advanced panel" is what longevity-focused platforms and precision medicine practitioners now recommend. That gap is where undetected risk sits for years.
HbA1c and fasting insulin together, for example, can reveal insulin resistance years before fasting glucose alone moves out of range. A person with a "normal" fasting glucose of 95 mg/dL could already have significantly elevated insulin, meaning their pancreas is working overtime to maintain that glucose level. By the time glucose itself rises, the underlying metabolic dysfunction has been progressing for years.
One important caveat from Dr. Richard Mayeux at Columbia University: biomarker panels are more useful than single markers because no single measurement captures the full picture. The value is in combining markers across categories and watching trends over time rather than reacting to any individual number in isolation.
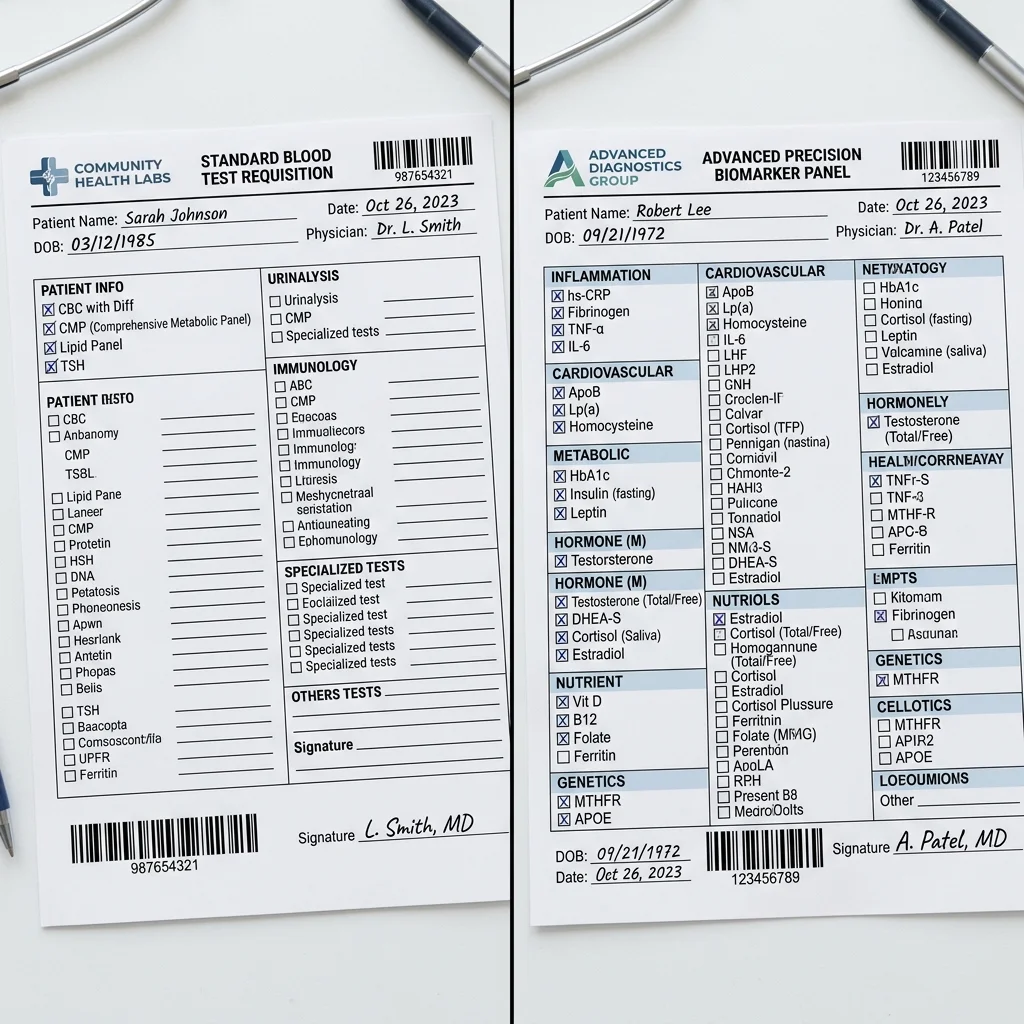
Function Health vs InsideTracker: Where Your Money Goes
The two platforms most often compared in the direct-to-consumer biomarker space are Function Health and InsideTracker. Both use Quest Diagnostics for blood draws and accept HSA/FSA payments. Beyond that, they diverge in nearly every dimension that matters.
Function Health charges $365 per year for two comprehensive draws covering more than 100 biomarkers each. That includes clinician-reviewed notes, a biological age calculation, an AI health coach, and access to add-ons like the Galleri multi-cancer screening test and ApoE genotyping. The cost per biomarker works out to roughly $2.81.
InsideTracker takes a different approach. The $149 annual membership grants platform access, but blood tests are purchased separately. The Ultimate panel runs $589 and covers up to 54 biomarkers. Two tests per year (matching Function Health's cadence) totals $1,327. Add the InnerAge biological age calculation at $99 per assessment and optional DNA testing at $249, and first-year costs can exceed $1,500. The cost per biomarker on the Ultimate panel is approximately $10.89.
| Feature | Function Health | InsideTracker |
|---|---|---|
| Annual cost (2 tests/year) | $365 | $1,327 |
| Biomarkers per test | 100+ | Up to 54 |
| Cost per biomarker | ~$2.81 | ~$10.89 |
| Biological age | Included | $99 add-on per calculation |
| DNA testing | ApoE only (add-on) | 261 genetic variants ($249) |
| Clinician review | Yes, included | No (AI-driven recommendations) |
| Wearable integration | Oura, Garmin, Fitbit, Polar, Coros, Suunto, + 4 more | Oura, Apple Health, Fitbit, Garmin |
| Upload existing bloodwork | No | Yes ($149/year) |
Function Health's depth advantage is substantial. Cheryl McColgan, who completed four rounds of Function Health testing starting in August 2024, reported that the comprehensive panel caught a hemoglobin drop to 8.6 g/dL after competition prep, a neutrophil count of 760 cells per microliter (below range), and an ALT spike that turned out to be exercise-induced. None of those findings would have appeared on a 54-biomarker panel unless those specific markers happened to be included.
InsideTracker's edge lies in flexibility. The platform lets you upload bloodwork from any provider for $149 per year, giving you access to their analysis algorithms and Action Plan system without paying for new draws. If your physician already orders comprehensive labs, this upload feature makes InsideTracker the cheaper option. The DNA testing covers 261 health-related genetic variants that Function Health doesn't offer (aside from ApoE). And the modular approach lets you retest specific categories (inflammation, heart health, cognition) for $99 to $149 each without repeating a full panel.
One finding worth noting about biological age calculations: McColgan tested on three platforms at roughly the same time. Function Health reported a biological age of 37.3 against her calendar age of 52, Hundred Health showed 38.0, and Superpower returned 45.2. That 8-year spread between platforms for the same person at the same time underscores that biological age is an algorithm-dependent estimate, not an objective measurement. It's useful for tracking your own trend on a single platform over time. Comparing across platforms tells you more about the algorithm differences than about your actual aging.
Function Health delivers more data per dollar, and the clinician review adds a human check that AI-only systems miss. InsideTracker wins on flexibility, genetic testing, and the ability to leverage existing bloodwork. Some users run both: Function Health for the deep panel and clinician notes, InsideTracker for the goal-tracking system and wearable integration at $149 per year using uploaded results.
The At-Home Testing Trap Nobody Talks About
A research team at the University of Birmingham, led by Jonathan J. Deeks, professor of biostatistics, purchased 30 direct-to-consumer self-test devices from UK high street shops and evaluated them against evidence-based clinical guidance. The results, published in the BMJ in 2025, are not encouraging.
Of the 30 self-tests reviewed, only 27% indicated who should use the test and when to use it. Only 23% provided information about what to do after getting a result. A third offered numerical performance data (sensitivity and specificity). Most alarming: 58% of the tests were judged contrary to evidence-based guidance in at least one dimension, whether that was the intended population, testing frequency, threshold used, or the type of investigation actually needed for the condition.
"The current market for self-tests does not support consumer informed decisions about their use, interpretation of test results, and subsequent actions," the researchers concluded. They called for improved regulatory oversight to protect both the public and healthcare systems from misuse.
The overdiagnosis problem runs deeper than bad packaging. A separate BMJ analysis of overdetection in healthcare found that more testing doesn't automatically mean better health outcomes. South Korea's experience with thyroid cancer screening illustrates the risk: between 1999 and 2008, thyroid cancer incidence increased 6.4-fold after widespread screening was introduced. But 95% of detected cancers were small (under 20mm), and mortality from thyroid cancer remained essentially unchanged. The screening found real cancers, but they were overwhelmingly cancers that would never have caused symptoms or death.
The same paper noted a relationship between how many PSA tests general practitioners ordered and how many prostate cancer diagnoses appeared on their patient lists. Mortality rates, however, stayed constant regardless of testing volume. More tests produced more diagnoses without producing more cures.
None of this means at-home testing is worthless. The value depends on what you're testing, whether the test meets clinical-grade standards, and whether you have a framework for interpreting results. Tests processed through CLIA-certified, CAP-accredited laboratories (the standard used by platforms like Function Health and InsideTracker) are fundamentally different from a lateral flow test purchased at a pharmacy.
The distinction matters because pre-analytic factors significantly affect biomarker results. Posture during blood draw, time of day, recent food intake, exercise within the previous 24 hours, and hydration status can all shift values enough to create misleading readings. A finger-prick sample collected at home after coffee and a morning run produces different numbers than a fasting venous draw performed at 8 AM in a seated position. Both are "blood tests," but they're not measuring the same thing.
"Obsessing over a biomarker that is slightly high or low without any symptoms is more likely to tax your mental health than to make a significant positive impact on your physical health." — Levels Health clinical guidance
At-home collection kits from reputable platforms that route samples to certified labs sit between pharmacy self-tests and full clinical draws. They work for tracking trends in markers where finger-prick accuracy is acceptable: certain hormones, vitamin D, basic metabolic markers. For markers where precision matters and small differences carry clinical weight (lipid particles, insulin, inflammatory markers), venous blood draws through a certified lab remain the standard.

Your Personal Testing Calendar: When and How Often
Testing frequency should match your age, health status, and goals. But general principles hold across all three.
For most healthy adults, testing every six to twelve months covers the basics: CBC, comprehensive metabolic panel, thyroid function, lipid panel, and inflammatory markers. Someone in their 20s with no symptoms or family history might stretch to every two to three years. By 40, annual testing becomes genuinely useful because metabolic and hormonal shifts accelerate. By 50, catching trends early becomes the difference between prevention and treatment.
The 2026 ACC/AHA guideline introduced a new wrinkle: the PREVENT risk calculator now recommends cardiovascular risk assessment starting at age 30, evaluating both 10-year and 30-year risk. The guideline also recommends cholesterol screening for children between ages 9 and 11, a recognition that plaque buildup can begin far earlier than most people assume. Dr. Reynolds noted that "half of people with high LDL cholesterol don't have a family history of heart disease."
| Biomarker Category | Baseline | Healthy Adults | Active Monitoring | Notes |
|---|---|---|---|---|
| Metabolic (glucose, HbA1c, insulin) | Age 20-30 | Annually | Every 3 months | HbA1c every 3 months for diabetics during therapy changes |
| Cardiovascular (lipids, ApoB, Lp(a)) | Age 20 (lipids); 30 (ApoB, Lp(a)) | Annually | Every 6 months | Lp(a) is genetic — one test may suffice unless on treatment |
| Inflammatory (hs-CRP, homocysteine) | Age 30 | Annually | Every 3-6 months | Retest after lifestyle interventions to confirm improvement |
| Thyroid (TSH, free T3/T4) | Age 30 | Annually | Every 3-6 months | More frequent during medication adjustments or pregnancy |
| Hormonal (testosterone, estradiol, DHEA) | Age 30-35 | Annually | Every 3-4 months | Cycle-dependent for women; after TRT initiation for men |
| Nutritional (D, B12, iron, magnesium) | Age 20-30 | Annually | Every 3-6 months | Retest after supplementation to confirm absorption |
| Kidney/Liver (Cystatin C, GGT, albumin) | Age 40 | Annually | Every 6 months | GGT and albumin track disease progression speed per Karolinska study |
Two principles matter more than any specific schedule. First, consistency beats frequency. Testing under the same conditions (fasting, same time of day, same lab) produces comparable data points. A quarterly test done after coffee, a run, and minimal sleep will look different from the same markers drawn in a controlled fasting state, not because your health changed, but because pre-analytic variability shifted the numbers.
Second, your individual trend line matters more than any single value. Population reference ranges are derived from broad averages. A "normal" result might be perfectly healthy for one person and an early warning signal for another. Individualized reference ranges built from your own serial measurements reveal meaningful shifts that population norms would miss. This is where testing platforms with longitudinal tracking (Function Health, InsideTracker) offer genuine value over one-off lab orders: they build your personal baseline and flag deviations from it.
The question of when to test immediately rather than waiting for your next scheduled draw is straightforward. Persistent new symptoms, including unexplained fatigue, mood changes, hair loss, skin changes, or menstrual irregularities, warrant blood work regardless of when you last tested. These symptoms often map to thyroid, hormonal, nutritional, or inflammatory markers that can be quickly assessed through targeted panels.

Frequently Asked Questions
What is the difference between a standard blood panel and biomarker testing?
A standard blood panel (CBC, basic metabolic panel, lipid panel) covers about 20-30 markers and is designed to flag existing disease or acute abnormalities. Biomarker testing expands this to 50-130+ markers across categories like advanced cardiovascular (ApoB, Lp(a)), inflammatory (hs-CRP, homocysteine), hormonal, and nutritional markers. The goal shifts from "is something already wrong" to "where is your health trajectory heading." Platforms like Function Health test over 100 biomarkers per draw, while InsideTracker's most comprehensive panel covers up to 54.
Are at-home blood tests as accurate as lab draws?
It depends on the test and the lab processing the sample. At-home kits that route finger-prick samples to CLIA-certified, CAP-accredited laboratories can produce reliable results for many markers. However, a 2025 BMJ study found that 58% of direct-to-consumer self-tests sold in UK shops were contrary to evidence-based guidance. Pre-analytic factors like posture, food intake, and exercise affect results significantly. For markers requiring high precision (lipid particles, insulin), a fasting venous draw at a certified lab remains the standard.
How much does comprehensive biomarker testing cost?
Costs range widely. Function Health charges $365 per year for two comprehensive draws covering 100+ biomarkers. InsideTracker's comparable coverage (two Ultimate panels per year) runs approximately $1,327. Individual panels through your physician vary by insurance coverage. Most direct-to-consumer platforms accept HSA and FSA payments, which can reduce effective cost by 25-35% depending on your tax bracket.
Which biomarkers should I test first if I've never done advanced testing?
Start with a comprehensive metabolic panel, full lipid panel (including ApoB if available), HbA1c, fasting insulin, hs-CRP, thyroid panel (TSH, free T4), vitamin D, and a CBC with differential. This covers metabolic, cardiovascular, inflammatory, thyroid, nutritional, and blood health in one draw. If you have family history of heart disease, add Lp(a), which only needs to be tested once since it's genetically determined. This baseline costs significantly less than a full longevity panel and captures the markers most likely to reveal actionable findings.
Can biological age tests actually tell you how fast you're aging?
Biological age clocks built from blood biomarkers provide an estimate of your cellular health relative to your chronological age. A 2025 study validated a 7-biomarker aging clock in 59,741 samples across multiple ethnic cohorts. However, these estimates are algorithm-dependent. One tester reported biological ages of 37.3, 38.0, and 45.2 from three different platforms at the same time. The number itself is less meaningful than your trend on a single platform over repeat measurements. If your biological age drops after lifestyle changes, that's a genuinely useful signal regardless of which specific number the algorithm produces.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.