What Happens Inside Your Body During Dehydration
Your body is about 60% water by weight. Every cell depends on that fluid to function, so when you lose more than you take in, the effects go well past feeling thirsty.
Water is the medium for nearly every biochemical reaction in your body. It regulates temperature, cushions joints, carries nutrients through the bloodstream, and flushes waste through the kidneys. When fluid levels drop, blood volume shrinks. Your heart has to work harder to push thicker, more concentrated blood through your vessels. Meanwhile, the kidneys start conserving water by producing less urine, which concentrates waste products that can irritate the bladder and urinary tract.
At the cellular level, water moves across membranes through osmosis to balance electrolyte concentrations. Dehydration disrupts that balance, causing cells to shrink and impairing their signaling. The brain is especially vulnerable because it sits in a fluid-filled cavity, and even small hydration shifts affect how neurons communicate. A 2018 meta-analysis in Medicine & Science in Sports & Exercise found measurable impairments in attention, executive function, and motor coordination starting at just 2% body mass loss.
Quick fact: Losing 1-2% of your body weight in water (roughly 1.5 to 3 pounds for a 150-pound person) is enough to trigger headaches, fatigue, and trouble concentrating.
How Much Water Do You Actually Need Each Day?
The answer depends on who you are, where you live, and what you do. The National Academies of Sciences, Engineering, and Medicine established Adequate Intake levels for total daily water from all sources (beverages and food combined):
| Group | Total Daily Water (All Sources) | From Beverages Alone |
|---|---|---|
| Men (19+) | 3.7 L (125 oz) | ~3.0 L (about 13 cups) |
| Women (19+) | 2.7 L (91 oz) | ~2.2 L (about 9 cups) |
| Pregnant women | 3.0 L (101 oz) | ~2.4 L (about 10 cups) |
| Breastfeeding women | 3.8 L (128 oz) | ~3.1 L (about 13 cups) |
About 20% of your daily water comes from food, especially fruits and vegetables. Watermelon, cucumbers, oranges, and strawberries are all more than 90% water by weight. If you eat a lot of produce, you don't need to drink as much. For more on how water supports your body, see our guide on the health benefits of drinking water.
These numbers go up with physical activity, hot climates, high altitude, and illness. Endurance athletes can lose more than 2 liters of sweat per hour in the heat, according to the American College of Sports Medicine.
Early Warning Signs Most People Miss
Thirst is the obvious one, but it is far from the first signal. Your body sends several subtler warnings before you ever feel like reaching for a glass of water.
Headaches. One of the earliest symptoms, and one people rarely connect to hydration. Even 1-2% body mass loss can trigger headaches because reduced blood volume affects oxygen delivery to the brain.
Bad breath. This one surprises people. Saliva has antibacterial properties, and when dehydration cuts saliva production, oral bacteria multiply fast. The result is halitosis that brushing won't fix.
Sugar cravings. Your liver needs water to release stored glycogen (glucose) into the bloodstream for energy. When fluid levels drop, your body struggles to access these reserves, triggering sudden cravings for sweets and simple carbohydrates.
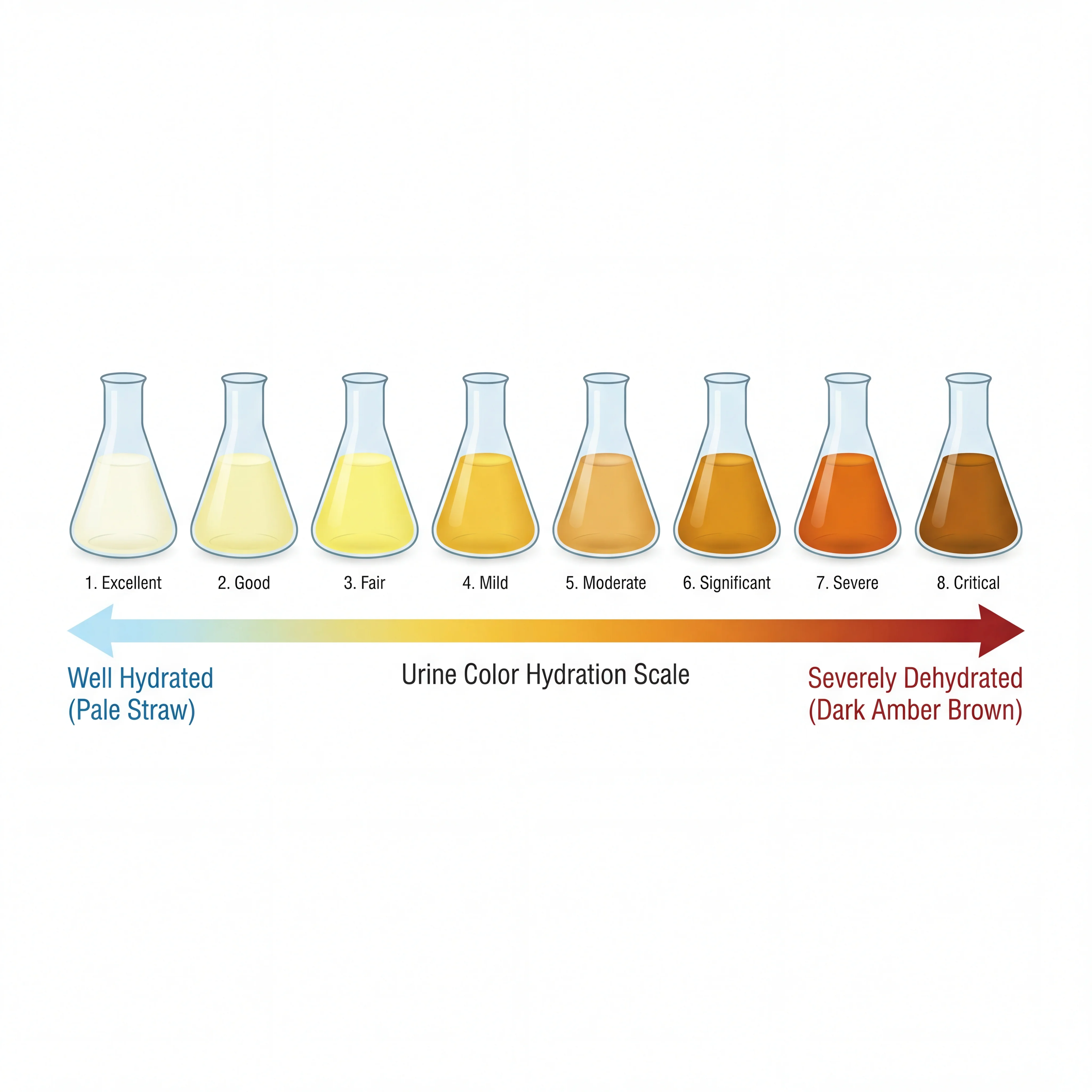
Dark urine. Healthy, well-hydrated urine is pale straw to light yellow. As dehydration progresses, kidneys conserve water by concentrating urine, turning it dark yellow or amber.
Dry skin that tents. Try this: pinch the skin on the back of your hand and let go. If you're well hydrated, it snaps back. Dehydrated skin "tents," staying raised for 2 or more seconds before slowly flattening.
Muscle cramps. Fluid loss concentrates electrolytes and impairs muscle function. Cramps can appear even at mild dehydration levels, especially during or after exercise.
Fatigue and brain fog. When blood volume drops, your heart pumps harder to move oxygen around. A study in the British Journal of Nutrition found that at just 1.59% body mass loss, participants made more errors on cognitive tasks. At 1.36% loss, fatigue, tension, and anxiety all went up.
Dry eyes. Tear production slows down early in dehydration. Many people blame screen time or allergies when the real issue is not drinking enough.
When Dehydration Becomes a Medical Emergency
Most dehydration is mild and fixes itself once you start drinking. Severe dehydration is different. It can cause organ damage, seizures, and death if untreated.
| Severity | Body Weight Loss | Key Signs | Action Required |
|---|---|---|---|
| Mild | 1-3% | Thirst, slightly dark urine, dry mouth | Increase oral fluids |
| Moderate | 3-6% | Very dry mouth, reduced urination, dizziness, rapid heartbeat | Oral rehydration solution; monitor closely |
| Severe | 6-10% | Confusion, no urination, sunken eyes, rapid breathing | Emergency room — likely IV fluids |
| Life-threatening | >10% | Unconsciousness, seizures, organ failure | Call 911 immediately |
Go to the emergency room if you or someone else experiences: confusion or altered mental state, no urination for 12 or more hours, fainting or loss of consciousness, seizures, rapid or weak pulse, fever above 103°F (39.4°C), inability to keep any fluids down, or bloody or black stool.
The complications at this stage are serious. The Mayo Clinic warns about brain swelling (cerebral edema) when fluids rush back after rehydration, seizures from electrolyte imbalances, hypovolemic shock from dangerously low blood volume, and kidney failure from prolonged reduced blood flow.

Who Faces the Greatest Risk?
Anyone can get dehydrated, but some groups are hit harder and faster than others.
Older adults (65+). Aging dulls the thirst signal, so older adults often don't feel thirsty even when their bodies need fluid. Kidney concentrating ability declines too. By age 80, the kidneys can only concentrate urine to about half the level of younger kidneys. Add common medications like diuretics and laxatives, and fluid loss gets worse. A 2023 review in Nutrients found that between 50% and 92% of nursing home residents with inadequate fluid intake are dehydrated.
Infants and young children. Kids have a higher surface-area-to-volume ratio, so they lose more water through the skin proportionally. They also have faster metabolisms and can't get water for themselves. Stomach bugs (acute gastroenteritis) remain the leading cause of pediatric dehydration worldwide.
Athletes and outdoor workers. Sweat losses can exceed 2 liters per hour during intense exercise in hot conditions. The American College of Sports Medicine notes that losing more than 2% of body mass impairs endurance performance, and a 5% loss reduces work capacity by approximately 30%. Core body temperature rises 0.12-0.25°C for every 1% of body mass lost through sweat.
People with chronic illness. Diabetes causes the kidneys to excrete excess glucose along with large volumes of water. Chronic kidney disease makes it harder to concentrate urine. Heart failure is tricky because both dehydration and overhydration are dangerous. If you deal with chronic fatigue, dehydration may be making your symptoms worse. Our article on chronic fatigue syndrome looks at this overlap.
Pregnant women. Blood volume expands during pregnancy, and amniotic fluid requires water too. Dehydration during pregnancy can cause oligohydramnios (low amniotic fluid) and is a known trigger for preterm contractions.
How Doctors Diagnose Dehydration
No single test can confirm dehydration on its own. Doctors rely on a mix of clinical signs, urine tests, and blood work.
Clinical examination. Your doctor checks skin turgor (the pinch test), looks for dry mucous membranes, presses your fingernail to measure capillary refill time (color should return in under 2 seconds), and takes orthostatic vital signs, checking whether your blood pressure drops or pulse rises when you stand up.
Urine tests. Urine specific gravity above 1.020 points to dehydration. Urine osmolality above 800 mOsm/kg is another red flag. Urine color gives a quick visual clue (pale straw is ideal, dark amber means concentrated), though diet and supplements can throw the results off.
Blood tests. Serum osmolality is the most reliable single marker. Normal range is 275-295 mOsm/kg; values above 300 indicate dehydration. A BUN-to-creatinine ratio above 20:1 suggests the kidneys are not receiving adequate blood flow, a hallmark of dehydration.
Important: A Cochrane review found that no single physical sign or laboratory test reliably diagnoses dehydration in older adults when used alone. Combination assessment is always recommended.
Evidence-Based Remedies That Actually Work
For mild to moderate dehydration, oral rehydration is the go-to treatment. Decades of evidence show it works as well as IV fluids for most cases.
The WHO Oral Rehydration Solution. This formula, first developed in the 1970s, has saved an estimated 70 million lives. The current version (adopted by WHO in 2003) balances glucose and sodium to activate a co-transport mechanism in the intestinal lining. That mechanism pulls water into the bloodstream even when the gut is inflamed, which is why it works during diarrheal illness.
| Component | Amount per Liter | What It Provides |
|---|---|---|
| Sodium chloride (table salt) | 2.6 g | 75 mEq/L sodium |
| Potassium chloride | 1.5 g | 20 mEq/L potassium |
| Trisodium citrate | 2.9 g | 10 mEq/L citrate |
| Glucose (sugar) | 13.5 g | 75 mmol/L glucose |
A simplified home version: dissolve 6 level teaspoons of sugar and half a teaspoon of salt in 1 liter of clean water. This approximation is endorsed by the WHO for emergency use when commercial ORS packets are unavailable. A 2024 systematic review confirmed that low-osmolarity ORS remains effective for acute and persistent diarrhea in children, producing 36% lower stool output than the original formula.
Hydrating foods. Water-rich fruits and vegetables give you both fluid and electrolytes. Watermelon is about 92% water and also delivers potassium, magnesium, and vitamins A and C. Cucumbers, strawberries, oranges, and soups all count toward your daily fluid intake.
When you need IV fluids. If you cannot keep liquids down, are showing signs of severe dehydration (confusion, no urine output, rapid pulse), or have lost more than 6% of body weight, emergency IV rehydration is necessary. Hospitals typically administer isotonic saline (0.9% sodium chloride) or lactated Ringer's solution.

Hydration Myths vs. Medical Facts
There is a lot of bad hydration advice floating around. Here is what the research actually says.
| Myth | Medical Fact | Source |
|---|---|---|
| "Drink 8 glasses of water a day" | No scientific evidence supports this specific number. A 2002 Dartmouth review found the claim likely originated from a misread 1945 recommendation that included water from food. | Valtin, Am J Physiol, 2002 |
| "Coffee dehydrates you" | A 2014 randomized crossover trial of 50 men found no evidence that moderate coffee intake (up to 4 cups/day) causes dehydration. Coffee counts toward daily fluid intake. | Killer et al., PLoS ONE, 2014 |
| "Clear urine means you're hydrated" | Completely clear urine may indicate overhydration and risk of hyponatremia (dangerously low sodium). Pale straw is the ideal color. | Shirreffs, BMJ Open Sport Exerc Med, 2018 |
| "If you're thirsty, you're already dehydrated" | Thirst begins at 1-2% body mass loss — mild and easily corrected. For healthy adults, drinking when thirsty is a reliable strategy. This warning applies mainly to older adults with blunted thirst. | University of Rochester Medical Center |
| "You can't drink too much water" | Water intoxication (hyponatremia) is real and potentially fatal. Drinking 3-4 liters in 1-2 hours can overwhelm the kidneys, causing seizures, brain swelling, and death. | Cleveland Clinic |
Children and Dehydration: A Parent's Quick Reference
Dehydration moves faster in children than in adults. They have higher metabolic rates and proportionally more skin surface area relative to their body mass, so they lose water quicker.
Causes. Gastroenteritis (vomiting and diarrhea) is the leading cause worldwide. Fever, refusal to drink, hot weather, and vigorous play also contribute. If your child has been ill with vomiting or diarrhea, dehydration risk climbs rapidly.
Warning signs in infants: no tears when crying, no wet diapers for 3 or more hours, sunken fontanelle (the soft spot on top of the head), excessive sleepiness or fussiness, and sunken eyes.
Warning signs in older children: dry mouth and tongue, reduced urination (fewer than 6-8 wet diapers in 24 hours for toddlers), dark urine, listlessness, and cool or mottled skin on the extremities.
What to do. Give small, frequent sips of pediatric oral rehydration solution (like Pedialyte) rather than large amounts at once, which can trigger more vomiting. Skip fruit juice, soda, and sports drinks because their sugar content can worsen diarrhea. Breastfed infants should keep breastfeeding with ORS offered between feedings. If your child can't keep fluids down or shows signs of moderate or severe dehydration, get medical help.
The Role of Electrolytes in Staying Hydrated
Drinking water is not enough on its own. Electrolytes (electrically charged minerals dissolved in your body fluids) control how water moves between cells and the bloodstream. Without them, drinking more water can actually dilute your blood to dangerous levels.
Sodium drives fluid balance outside your cells. It determines how much water your body holds onto and how fluid gets distributed between compartments. You lose anywhere from 0.5 to 2 grams of sodium per liter of sweat, depending on your fitness level and how acclimatized you are to heat.
Potassium handles fluid balance inside your cells and works alongside sodium through the sodium-potassium pump (Na+/K+-ATPase) in every cell membrane. Most adults don't get enough; the recommendation is 2,600-3,400 mg per day. Bananas, potatoes, spinach, and beans are good sources. Chia seeds provide potassium too, plus fiber that helps with hydration retention.
Magnesium is involved in over 300 enzymatic reactions, including muscle relaxation and nerve function. About 40% of adults don't get enough magnesium from their diet, and deficiency makes muscle cramping and fatigue worse. Those are two symptoms people often blame on dehydration alone when magnesium may be part of the problem.
This is why chugging plain water after heavy sweating or a bout of illness can backfire. If you've lost a lot of fluid, you need electrolytes with it. Commercial electrolyte drinks, coconut water, or a homemade ORS all work. During the hot summer months, anyone spending time outdoors should be thinking about electrolyte balance, not just water.
Frequently Asked Questions
How long does it take to recover from dehydration?
Mild cases usually resolve in 1-2 hours once you start drinking steadily. Moderate dehydration may take 6-12 hours of oral rehydration. Severe cases needing IV fluids can take 24-48 hours to fully recover, depending on the cause and whether any organs were affected.
Can chronic dehydration cause long-term health problems?
It can. Not drinking enough over time is linked to higher rates of kidney stones, urinary tract infections, constipation, and declining kidney function. A 2024 study in Nutrition Bulletin flagged habitual low water intake as a possible contributor to chronic disease risk, though researchers say more long-term studies are needed to prove direct causation.
Is sparkling water as hydrating as still water?
It is. The carbon dioxide that makes the bubbles doesn't affect water absorption or hydration status. If you prefer sparkling water and find you drink more of it, that's a fine approach.
Do older adults need more water than younger people?
The baseline fluid requirements are about the same. The problem is that older adults have a weaker thirst signal and less efficient kidneys. They don't necessarily need more water; they need to be more intentional about it. Drinking on a schedule and watching urine color are more reliable than waiting until you feel thirsty.
What is the fastest way to rehydrate?
An oral rehydration solution with glucose and sodium gets absorbed faster than plain water because it activates the sodium-glucose co-transport pathway in the intestines. In practical terms, sipping an ORS or a balanced electrolyte drink over 15-30 minutes rehydrates you faster than gulping water, which the kidneys may just flush out as dilute urine.
Related Articles
- Top 10 Health Benefits of Drinking Water — Why staying hydrated does more for your body than most people realize.
- Watermelon Health Benefits: Ultimate Guide — At 92% water with natural electrolytes, it's one of the best hydrating foods out there.
- Running: Health Benefits and Side Effects — What runners need to know about fluid loss and performance.
- Summer Skin Protection Ultimate Guide — Hydration plays a bigger role in skin protection than most sunscreen ads suggest.
- Chronic Fatigue Syndrome: Causes, Symptoms, and Treatment — Chronic dehydration and fatigue share several overlapping symptoms.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.