Your Body Already Makes a Version of Ozempic
Before semaglutide and tirzepatide became household names, your intestines were already producing the hormone they mimic. Glucagon-like peptide-1, or GLP-1, is manufactured by specialized enteroendocrine L-cells scattered along the lining of your gut, with the highest concentrations in the lower small intestine and colon. Every time you eat, these cells detect incoming nutrients and release GLP-1 into your bloodstream within about 15 minutes of your first bite.
From there, GLP-1 acts on multiple organs at once. GLP-1 signals your pancreas to release insulin in response to rising blood sugar, a process researchers call the "incretin effect." This single mechanism accounts for roughly half of all postprandial insulin secretion in healthy people. Simultaneously, GLP-1 tells your pancreatic alpha cells to dial back glucagon production, which prevents your liver from dumping extra glucose into the bloodstream when you have already eaten.
GLP-1 also works directly on your brain. It activates appetite-suppressing POMC/CART neurons in the hypothalamus while quieting the hunger-promoting NPY/AgRP pathways. Appetite drops and fullness lingers well past the meal. GLP-1 also slows gastric emptying, keeping food in your stomach longer so nutrients are absorbed gradually rather than flooding your system all at once.
Key point: GLP-1 levels in your blood typically sit between 5 and 15 pmol/L when fasting, then climb two to four times higher after eating. But the hormone is fragile. An enzyme called DPP-IV chews through it so quickly that only 10-15% of newly secreted GLP-1 ever reaches your systemic circulation. That short half-life, just one to two minutes, is exactly why the foods and habits that stimulate frequent, robust GLP-1 release matter so much.
How Food Triggers GLP-1 Release From Your Gut
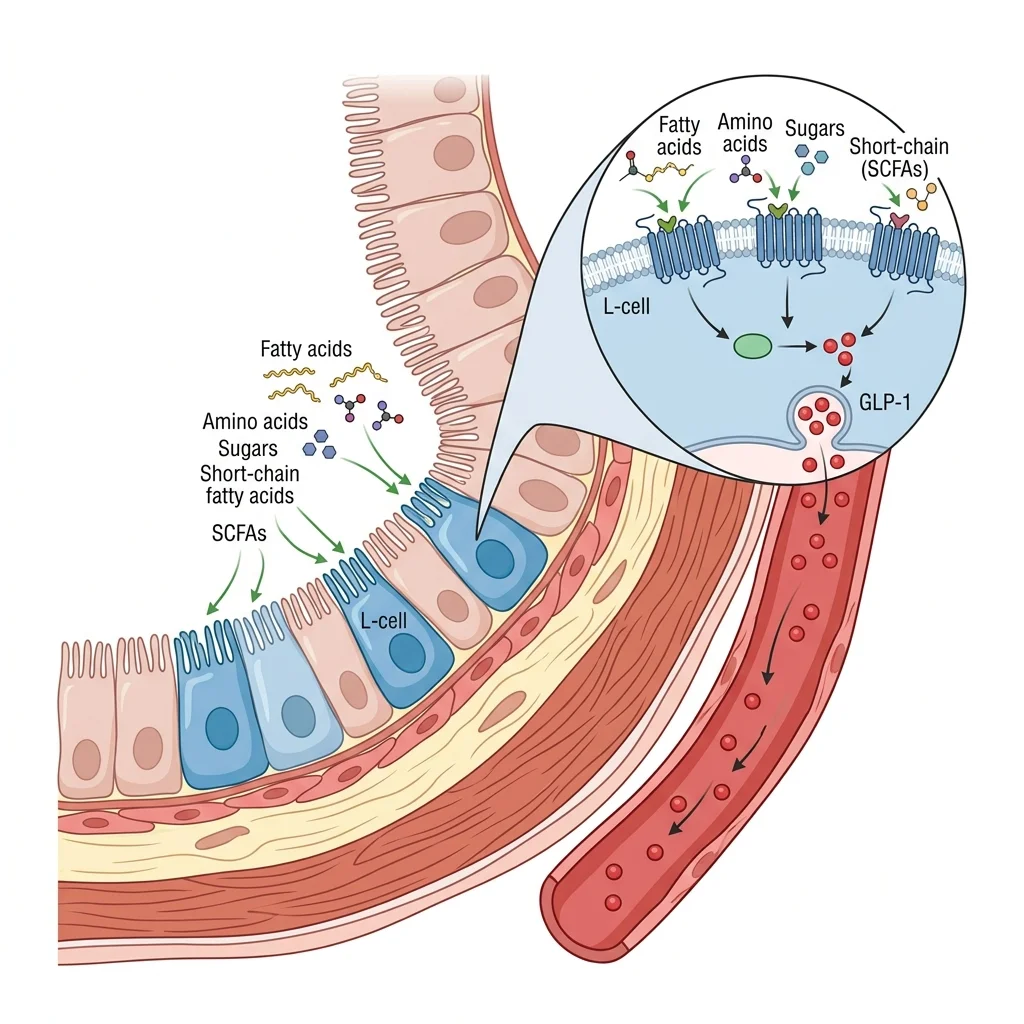
Understanding how food talks to your L-cells helps explain why certain meals leave you satisfied for hours while others send you reaching for snacks within ninety minutes. L-cells are equipped with an array of G-protein coupled receptors (GPCRs) on their surface, each tuned to detect specific nutrient molecules as they pass through the intestinal lumen.
Different macronutrients activate different receptor pathways. Long-chain fatty acids with more than 12 carbon atoms, like those in olive oil and salmon, bind to the FFAR1 (GPR40) and FFAR4 (GPR120) receptors. Amino acids and small peptides from digested protein activate the calcium-sensing receptor (CaSR) and peptide transporter PepT1. Simple sugars use sodium-dependent glucose transporter-1 (SGLT1) to enter L-cells, where their metabolism triggers calcium influx and hormone exocytosis. And short-chain fatty acids produced by gut bacteria in your colon activate FFAR2 (GPR43) and FFAR3 (GPR41), providing a sustained, second-wave GLP-1 signal long after you have finished eating.
This is why a diverse, nutrient-dense meal outperforms a single-macronutrient load for GLP-1 stimulation. When you eat a plate containing protein, healthy fats, and fiber together, you are activating multiple receptor systems simultaneously, producing a stronger and more sustained GLP-1 response than any one nutrient could achieve alone. Your gut bacteria add a delayed bonus: as they ferment fiber into short-chain fatty acids hours later, they keep your colonic L-cells producing GLP-1 well into the afternoon or evening.
| Nutrient | Receptor/Transporter | GLP-1 Timing | Top Food Sources |
|---|---|---|---|
| Long-chain fatty acids | FFAR1 (GPR40), FFAR4 (GPR120) | 30-60 min post-meal | Olive oil, avocado, salmon, nuts |
| Amino acids/peptides | CaSR, PepT1 | 15-90 min post-meal | Eggs, whey, fish, legumes |
| Glucose/monosaccharides | SGLT1, sweet taste receptor | 15-30 min post-meal | Whole fruits, starchy vegetables |
| Short-chain fatty acids | FFAR2 (GPR43), FFAR3 (GPR41) | 2-8 hours post-meal | Produced from fiber by gut bacteria |
The Best Foods That Boost GLP-1 Naturally
With the receptor biology in mind, here are the food categories that research has consistently linked to increased GLP-1 secretion, organized from strongest evidence to emerging evidence.
Protein-Rich Foods
Protein is the most reliable dietary trigger for GLP-1 release. In a controlled crossover study published in Obesity, a breakfast deriving 60% of its calories from protein produced significantly higher GLP-1 levels than isocaloric high-fat or high-carbohydrate meals, with elevated concentrations persisting for at least four hours. Among protein sources, whey stands out. Researchers use it as the positive control in GLP-1 studies because it consistently produces rapid, robust hormone spikes. Whey floods the small intestine with fast-absorbing amino acids that activate multiple L-cell receptors almost immediately.
But whey is not the only option worth considering. Eggs, codfish, and casein have all demonstrated GLP-1-stimulating activity in enteroendocrine cell models. Casein, the "slow" protein in milk, produces a more gradual but prolonged GLP-1 elevation compared to whey, making the two complementary rather than competing choices. A glass of whole milk or a bowl of Greek yogurt gives you both.
There is also a synergy between protein and calcium worth knowing about. Research published in Advances in Nutrition found that co-ingesting protein with calcium triggered some of the highest GLP-1 concentrations ever recorded following physiological food intake. The mechanism appears to involve the calcium-sensing receptor (CaSR) on L-cells, which responds to both amino acids and calcium ions simultaneously.
| Protein Source | GLP-1 Effect | Speed of Action | Additional Benefits |
|---|---|---|---|
| Whey protein | Strong, rapid spike | Fast (15-30 min) | Also inhibits DPP-IV enzyme |
| Eggs | Moderate-strong | Moderate (30-60 min) | Complete amino acid profile |
| Casein (milk, yogurt) | Moderate, sustained | Slow (60-180 min) | Prolonged satiety |
| Fish/seafood | Moderate-strong | Moderate | Omega-3s provide additional receptor activation |
| Legumes (beans, lentils) | Moderate + fiber bonus | Moderate-slow | Dual protein + fiber GLP-1 stimulation |
Extra Virgin Olive Oil and Monounsaturated Fats
The Mediterranean diet's centerpiece earns its reputation through GLP-1 biology. Human studies have shown that olive oil-rich meals produce higher GLP-1 responses than butter-rich meals, even when total fat and calorie content are matched. Unsaturated fatty acids, particularly the oleic acid abundant in olive oil, appear to be stronger GLP-1 stimulators than saturated fats. Extra virgin olive oil also appears to inhibit the DPP-IV enzyme that breaks GLP-1 down. So beyond triggering GLP-1 release through FFAR1 and FFAR4 receptors, it may extend the hormone's short lifespan in your bloodstream.
Avocados, walnuts, almonds, chia seeds, and flaxseeds deliver similar monounsaturated and polyunsaturated fatty acid profiles. Fatty fish like salmon, mackerel, and sardines add omega-3 fatty acids to the mix, which activate the same FFAR4 receptor on L-cells. Including these polyphenol-rich foods in your daily eating pattern creates a consistent base of GLP-1 stimulation throughout the day.

High-Fiber Foods
Fiber works through a different mechanism than protein or fat, and its effects unfold over a longer timeline. When soluble and fermentable fibers reach your colon undigested, your gut bacteria break them down into short-chain fatty acids, primarily acetate, propionate, and butyrate. These SCFAs then activate FFAR2 and FFAR3 receptors on colonic L-cells, triggering a delayed but meaningful wave of GLP-1 secretion. Studies using knockout mice that lack these receptors show impaired SCFA-triggered GLP-1 secretion and worsened glucose tolerance, confirming the pathway is not just theoretical.
Your colon can sustain SCFA concentrations above 100 mmol/L under healthy conditions, creating a persistent stimulatory environment for L-cells. The best fiber sources for this purpose include oats, barley, legumes (beans, lentils, chickpeas), artichokes, asparagus, and apples. Resistant starch, found in cooled potatoes, green bananas, and cooked-then-cooled rice, is another potent SCFA precursor. This is one of the reasons why butyrate production from dietary fiber is so valuable beyond its direct GLP-1 effects.
Fermented Foods and Probiotics
The gut bacteria that produce those GLP-1-stimulating SCFAs need to be healthy and diverse. Fermented foods, including yogurt, kefir, sauerkraut, kimchi, miso, and tempeh, supply live bacterial cultures that contribute to a thriving microbiome. Research on specific probiotic strains like Akkermansia muciniphila has shown direct links between certain gut bacterial populations and improved metabolic hormone signaling, including GLP-1.
Polyphenol-Rich Foods: Dark Chocolate, Berries, and Quercetin
Emerging research points to plant polyphenols as another GLP-1 lever. Quercetin, a flavonoid concentrated in onions, apples, berries, and capers, has been shown to directly stimulate GLP-1 secretion from enteroendocrine cell models. Dark chocolate containing at least 70% cacao solids provides flavanols that may support GLP-1 activity, though the evidence here is still developing. A one-ounce serving provides a meaningful dose of flavanols without excessive sugar intake.
The Fiber-to-GLP-1 Pipeline: Short-Chain Fatty Acids and Your Microbiome
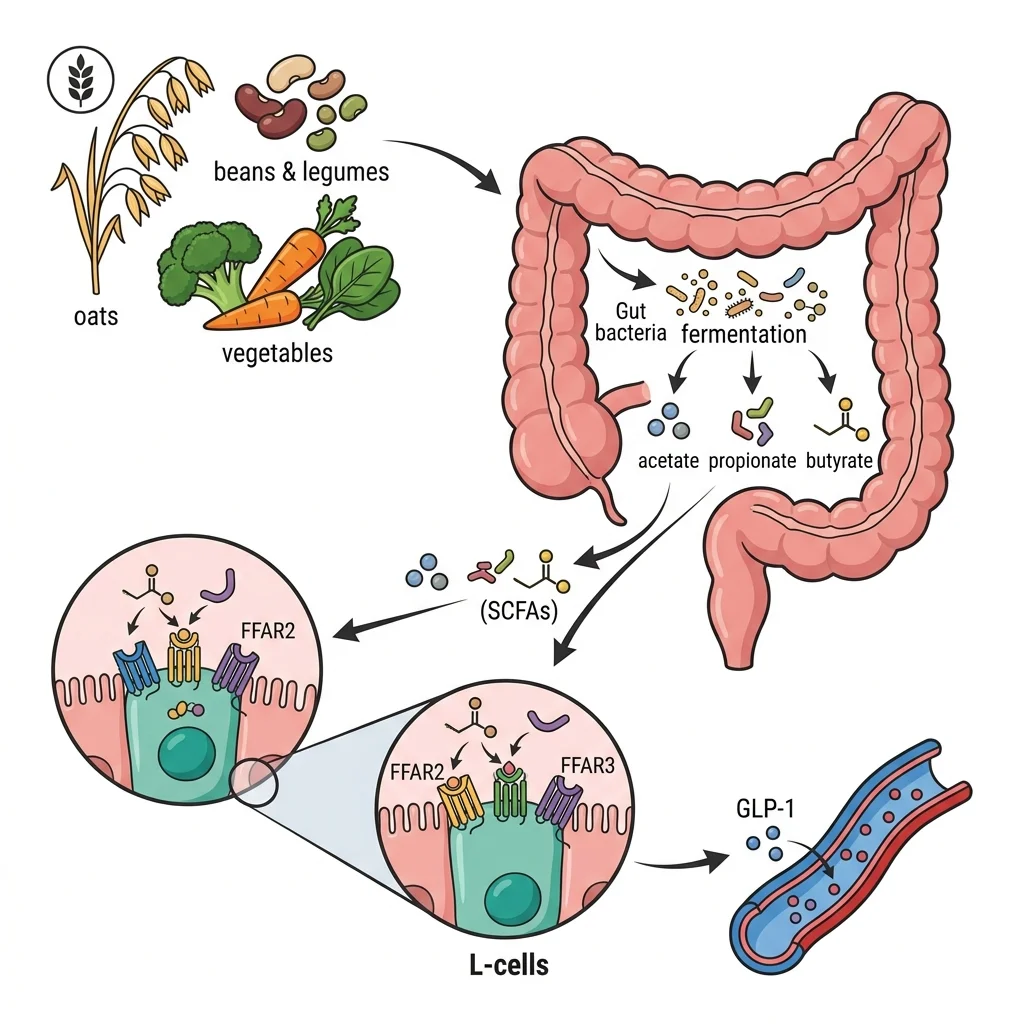
Most discussions of GLP-1-boosting foods stop at protein and fat. The fiber-to-SCFA pathway is the overlooked piece. While protein and fat produce immediate GLP-1 spikes that fade within a couple of hours, fiber-derived SCFAs create a sustained, low-level GLP-1 signal that continues working for you long after the meal has left your stomach.
Fermentable fiber arrives in your colon essentially unchanged. Your colonic bacteria, particularly species from the Firmicutes and Bacteroidetes phyla, ferment this fiber into three primary SCFAs: acetate (making up roughly 60% of the total), propionate (about 25%), and butyrate (around 15%). Each of these fatty acids activates L-cell receptors. Acetate and propionate preferentially bind FFAR2, while propionate and butyrate favor FFAR3. The receptor activation raises intracellular calcium levels in the L-cell, which triggers exocytosis of GLP-1-containing secretory granules.
If you only focus on protein and fat for GLP-1 stimulation, you are neglecting the entire colonic arm of the system. Adding 25-35 grams of fiber daily, with an emphasis on fermentable sources, recruits the densest population of L-cells in your entire digestive tract. The colonic L-cells actually outnumber those in the small intestine, but they only fire when SCFAs are available. For many people eating a standard Western diet low in fiber, these cells sit largely dormant.
Supporting a diverse gut microbiome through varied fiber intake is the key to maximizing this pathway. Different bacterial species prefer different fiber substrates, so eating a wide range of vegetables, fruits, legumes, and whole grains ensures you are feeding the full ecosystem rather than favoring a single strain.
| Fiber Source | Primary SCFA Produced | GLP-1 Receptor Activated | Serving Ideas |
|---|---|---|---|
| Oats (beta-glucan) | Propionate, butyrate | FFAR2, FFAR3 | Overnight oats, oatmeal |
| Beans and lentils | Acetate, propionate | FFAR2 | Soups, salads, hummus |
| Green bananas, cooled potatoes (resistant starch) | Butyrate | FFAR3 | Potato salad, banana smoothie |
| Asparagus, artichokes (inulin) | Acetate, butyrate | FFAR2, FFAR3 | Roasted, steamed |
| Apples, pears (pectin) | Acetate, propionate | FFAR2 | Whole fruit with skin |
Eating Habits That Amplify Your GLP-1 Response
What you eat matters, but how and when you eat shapes the GLP-1 response just as profoundly. These behavioral strategies come from controlled human trials, not theoretical speculation.
Meal Sequencing: Protein and Vegetables First
The order you eat your food in changes your GLP-1 response. Eating protein and fat together with fiber before carbohydrates produces a stronger GLP-1 surge than eating carbohydrates first. This works because protein and fat arriving in the small intestine ahead of glucose gives L-cells a head start on receptor activation, so that by the time carbohydrates hit the bloodstream, the insulin response is already primed and amplified. Practically, this means starting a meal with your salad and protein, and saving bread or starchy sides for the end.
Eating Speed and Chewing
Slower eating produces more pronounced GLP-1 levels, greater satiety, and lower total food intake. Taking smaller bites and chewing more thoroughly increases the surface area of food exposed to digestive enzymes, which means more nutrient fragments reach L-cells in the small intestine. Research suggests aiming for meals that take 20-30 minutes rather than being consumed in five.
Meal Timing and Circadian Rhythm
GLP-1 secretion follows your body's circadian clock, with higher responsiveness during daylight hours and reduced signaling overnight. Eating your largest meals earlier in the day, when L-cell sensitivity peaks, may produce a stronger incretin response than consuming the same food late at night. This aligns with research on intermittent fasting patterns that emphasize earlier eating windows.
GLP-1 Myths vs. Research-Backed Facts
| Myth | Research-Backed Fact |
|---|---|
| You need GLP-1 drugs to get meaningful GLP-1 effects | Your body produces GLP-1 naturally with every meal. While drug doses are pharmacologically higher, nutritional GLP-1 stimulation through diet provides meaningful metabolic benefits without side effects, and the natural rise-and-fall pattern may help preserve receptor sensitivity. |
| All fats increase GLP-1 equally | Unsaturated fats (olive oil, avocado, nuts) produce significantly higher GLP-1 responses than saturated fats (butter, lard) at matched calorie levels, based on controlled human feeding studies. |
| Only high-dose protein (40+ grams) triggers GLP-1 | Research shows that even 8 grams of whey protein produced a statistically significant GLP-1 increase at 90 minutes when combined with glucomannan fiber. |
| Eating more sugar boosts GLP-1 because glucose stimulates L-cells | While glucose does trigger GLP-1, the spike is short-lived and leads to rapid blood sugar swings. Protein, fat, and fiber produce more sustained GLP-1 responses with better metabolic outcomes. |
| Fiber only matters for digestive regularity | Fiber's conversion to SCFAs by gut bacteria triggers a second wave of GLP-1 secretion from colonic L-cells, hours after the original meal. This sustained signal is absent when fiber intake is low. |
A Sample Day of GLP-1-Supporting Meals
This sample day applies every principle covered above: protein at each meal, healthy fats from unsaturated sources, fermentable fiber for the SCFA pipeline, polyphenol-rich foods, and calcium-protein synergy. It also incorporates meal sequencing by suggesting you eat protein and vegetables before starches.
Breakfast (7:00-8:00 AM)
Overnight oats made with Greek yogurt (whey + casein + calcium), topped with fresh berries (polyphenols, pectin fiber), ground flaxseed (omega-3, soluble fiber), and a drizzle of extra virgin olive oil. Two scrambled or poached eggs on the side.
Lunch (12:00-1:00 PM)
Large salad with mixed greens, chickpeas, walnuts, and sliced avocado dressed in olive oil and lemon. Grilled salmon or sardines. A serving of artichoke hearts for inulin fiber. Eat the salad and protein before any bread.
Afternoon Snack (3:00-4:00 PM)
One ounce of dark chocolate (70%+ cacao) with a small handful of almonds. An apple with skin for pectin fiber.
Dinner (6:00-7:00 PM)
Lentil soup with asparagus and onions (inulin, quercetin, resistant starch). A side of cooled potato salad dressed in olive oil. Steamed broccoli. A glass of kefir.
Practical tip: You do not need to eat perfectly at every meal to see benefits. Even adding one GLP-1-boosting food to each meal, whether that is a handful of walnuts, an extra drizzle of olive oil, or a serving of fermented vegetables, shifts the balance in your favor. Consistency over weeks and months matters more than perfection on any single day.

Frequently Asked Questions
Can food really boost GLP-1 as much as medications like Ozempic?
No, dietary GLP-1 stimulation produces lower circulating hormone levels than pharmacological GLP-1 receptor agonists, which are engineered to resist DPP-IV breakdown and persist in the body for days or weeks. Natural GLP-1 from food has a half-life of just one to two minutes. That said, the natural rise-and-fall pattern of food-stimulated GLP-1 provides meaningful metabolic benefits, may help preserve receptor sensitivity over time, and activates vagal nerve pathways that drug agonists may not fully engage.
How quickly will I notice changes from eating more GLP-1-boosting foods?
GLP-1 release happens immediately with each meal, within 15 minutes of eating. You may notice improved satiety and fewer between-meal cravings within the first week of consistently prioritizing protein, healthy fats, and fiber. Longer-term metabolic improvements, including better fasting blood sugar and sustained appetite control, typically take several weeks as your gut microbiome adapts to higher fiber intake and SCFA production ramps up.
Is there a specific amount of fiber needed to activate the SCFA-GLP-1 pathway?
Most adults in Western countries consume only 15 grams of fiber per day, well below the 25-35 grams recommended for general health. Research on SCFA production and GLP-1 stimulation suggests that reaching at least 25 grams daily from diverse fermentable sources is needed to meaningfully activate colonic L-cells. Increasing fiber gradually over two to three weeks helps avoid digestive discomfort as your gut bacteria adjust.
Does the time of day I eat affect my GLP-1 response?
Yes. GLP-1 secretion follows a circadian rhythm, with stronger responses during daylight hours. Eating your largest, most nutrient-dense meals earlier in the day, when L-cell sensitivity is highest, tends to produce a more robust GLP-1 and insulin response than consuming the same food late at night. This is one reason many researchers advocate for front-loading calories toward breakfast and lunch.
Are there foods that suppress GLP-1 production?
Ultra-processed foods high in refined carbohydrates and low in fiber, protein, and healthy fats produce weak, short-lived GLP-1 spikes followed by rapid crashes. Chronic high-sugar diets may also impair L-cell function over time. Chronic stress and poor sleep quality further blunt GLP-1 responsiveness by disrupting cortisol and circadian signaling. A diet built around whole, minimally processed foods is the most reliable way to support consistent GLP-1 output.
Related Articles
- Butyrate: The Gut Metabolite That Heals Your Colon and Protects Your Brain - Learn how this key short-chain fatty acid supports gut health and GLP-1 production.
- Berberine for Blood Sugar and Weight Management - Explore another natural compound with incretin-enhancing properties.
- Akkermansia: The Probiotic for Metabolic Health - Discover how specific gut bacteria influence metabolic hormone signaling.
- The Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition - Understand the broader connections between gut health and hormonal regulation.
- Polyphenol-Rich Foods for Heart Health - Many of the same flavonoids that boost GLP-1 also protect your cardiovascular system.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.












