Your Brain Runs on a Fat You Have Probably Never Heard Of
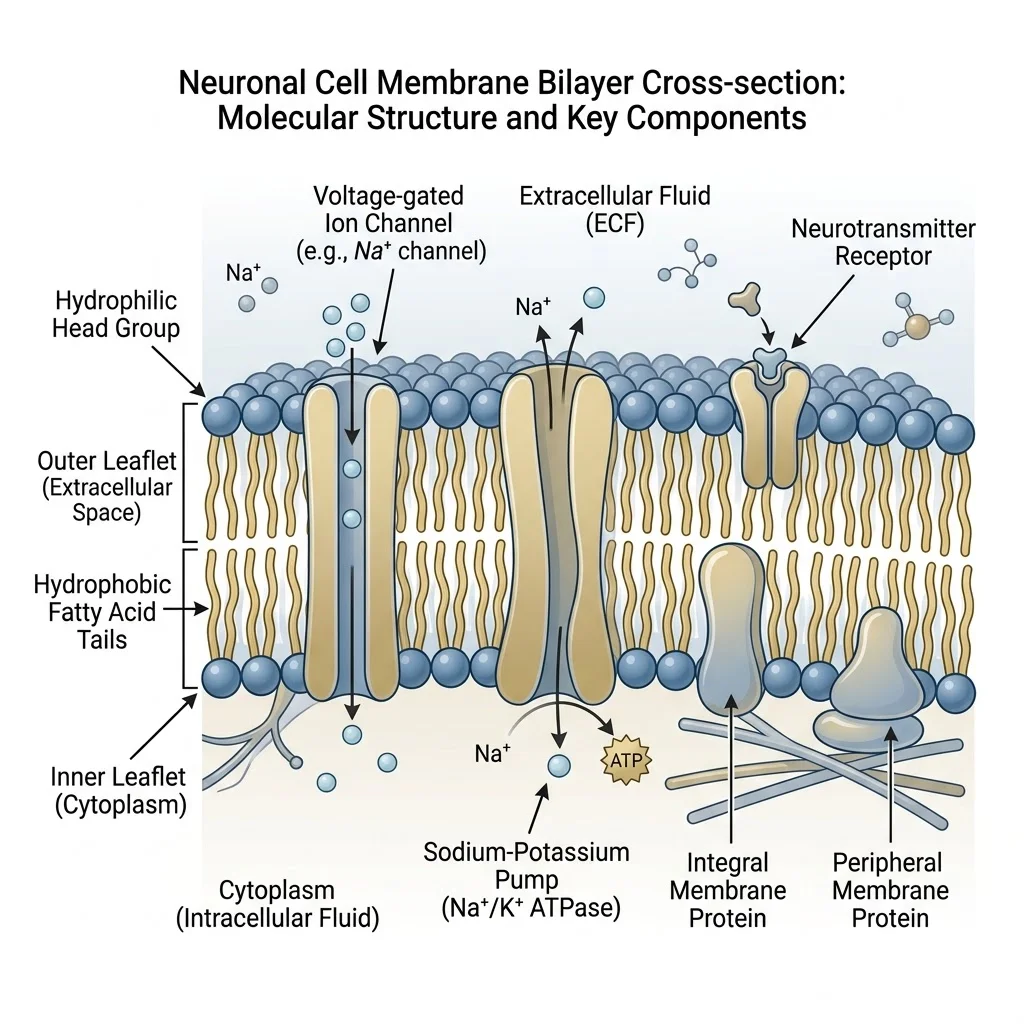
Every neuron in your brain is wrapped in a double-layered membrane, and phosphatidylserine (PS) is one of the most abundant phospholipids holding that structure together. It makes up roughly 11 to 21 percent of all brain phospholipids, concentrated on the inner leaflet of nerve cell membranes where it does much more than fill space.
PS acts as a docking platform. When proteins like protein kinase C, the PI3K/Akt pathway, or the Raf/Ras cascade need to activate, they rely on the negative charge of PS headgroups to anchor into position. Researchers at the National Institutes of Health have described this mechanism as distinct from typical second-messenger signaling — PS does not get broken down to produce its effects. It stays put and physically recruits the proteins that keep neurons alive, growing, and firing.
The body manufactures PS through two enzyme systems (PSS1 and PSS2) in the endoplasmic reticulum. PSS1 preferentially uses phosphatidylcholine enriched with docosahexaenoic acid (DHA), the omega-3 fatty acid concentrated in brain tissue. This is why DHA status and PS levels are linked — when DHA drops, PS production follows. Ethanol exposure has been shown to disrupt this DHA-to-PS conversion in neurons, which may partly explain alcohol's documented effects on cognition.
At the synapse level, PS participates in neurotransmitter release by facilitating the calcium-sensing activity of synaptotagmin and supporting SNARE-complex-mediated vesicle fusion. In plain terms, it helps nerve cells package chemical signals and send them across the gap to the next neuron. It also modulates how sensitive AMPA glutamate receptors are to incoming signals, directly influencing how efficiently your brain processes information.
Quick fact: PS crosses the blood-brain barrier after oral supplementation. This is unusual for a molecule of its size and makes it one of the few supplemental phospholipids that can directly reach brain tissue.
Unlike minerals or vitamins that serve as isolated cofactors, PS is woven into the physical architecture of every nerve cell. When brain PS content drops — as it naturally does with aging — it does not just mean one pathway slows down. The entire scaffolding that supports neural signaling, mood regulation, and cognitive processing becomes less stable.
A Six-Month Trial Changed What We Know About PS and Recall
The strongest human evidence for PS and memory comes from a double-blind randomized controlled trial published in the Journal of Clinical Biochemistry and Nutrition. Researchers enrolled 78 elderly Japanese adults (ages 50 to 69) who reported memory complaints and assigned them to receive a placebo, 100 mg of soy-derived PS daily, or 300 mg daily for six months, followed by three months of observation without supplementation.
The results split along an interesting line. When the researchers looked at the entire group, all three arms improved on general memory tests — likely a practice effect. The real finding emerged when they stratified by baseline cognitive performance. Among participants who started with lower scores, both PS groups significantly outperformed placebo on delayed word recall (p < 0.05 for 300 mg), and the MMSE delayed word recall subtest also showed significant improvements at both doses.
Here is what caught the researchers off guard: the benefits became more pronounced three months after supplementation stopped. The placebo group's scores drifted back toward baseline, while both PS groups held their gains. This pattern suggests PS may trigger structural or lasting metabolic changes in neurons rather than temporarily boosting a chemical signal that fades when you stop taking it.
| Measure | Placebo | PS 100 mg | PS 300 mg |
|---|---|---|---|
| Delayed Word Recall (low-baseline group) | No significant change | Trend toward improvement (p = 0.09) | Significant improvement (p < 0.05) |
| MMSE Delayed Recall | No significant change | Significant vs. placebo (p < 0.05) | Significant vs. placebo (p < 0.05) |
| Post-treatment maintenance | Returned to baseline | Maintained gains | Maintained gains |
A separate open-label extension study with 122 non-demented elderly participants found that 100 mg of PS combined with DHA daily improved sustained attention and memory recognition, while participants who continued from an earlier treatment phase maintained their cognitive status. This PS-DHA combination echoes the biological logic — DHA is PS's preferred fatty acid partner in brain membranes.
A literature review examining 127 published studies confirmed that exogenous PS at 300 to 800 mg daily can cross the blood-brain barrier and safely slow, halt, or reverse biochemical alterations associated with brain aging, supporting functions from short-term memory formation to language processing and reaction speed.
Not every trial has been positive, though. A 2001 study of 120 elderly participants at Maastricht University found no significant cognitive differences between groups receiving 300 mg, 600 mg, or placebo over 12 weeks. The shorter duration is worth noting — the positive Japanese trial ran for six months before benefits became clear, and the strongest effects appeared three months after that. PS may simply need more time to produce measurable changes in memory performance.
600 Milligrams Reduced Cortisol by 39 Percent in Ten Days
The relationship between PS and the stress hormone cortisol has been studied since the early 1990s, and the findings have been remarkably consistent across research groups and study designs.
The foundational study came in 1992 when Italian researchers gave nine healthy men 800 mg of PS daily for 10 days. They then measured hormonal responses during physical exercise stress. ACTH responses dropped significantly (p = 0.003) and cortisol followed (p = 0.03), while growth hormone and prolactin remained unchanged. This selectivity was important — PS was not broadly suppressing the endocrine system. It was specifically dampening the hypothalamic-pituitary-adrenal (HPA) axis response to stress.
Sixteen years later, a double-blind crossover study at the University of Mississippi confirmed these effects at a lower dose. Ten healthy males took 600 mg of soy-derived PS daily for 10 days, then exercised at 65 to 85 percent of their VO2 max. Peak cortisol concentrations dropped by 39 percent compared to placebo, and the total cortisol output (measured as area under the curve) fell by 35 percent. At the same time, the testosterone-to-cortisol ratio improved by 184 percent — a marker athletes use to gauge recovery state versus overtraining risk.
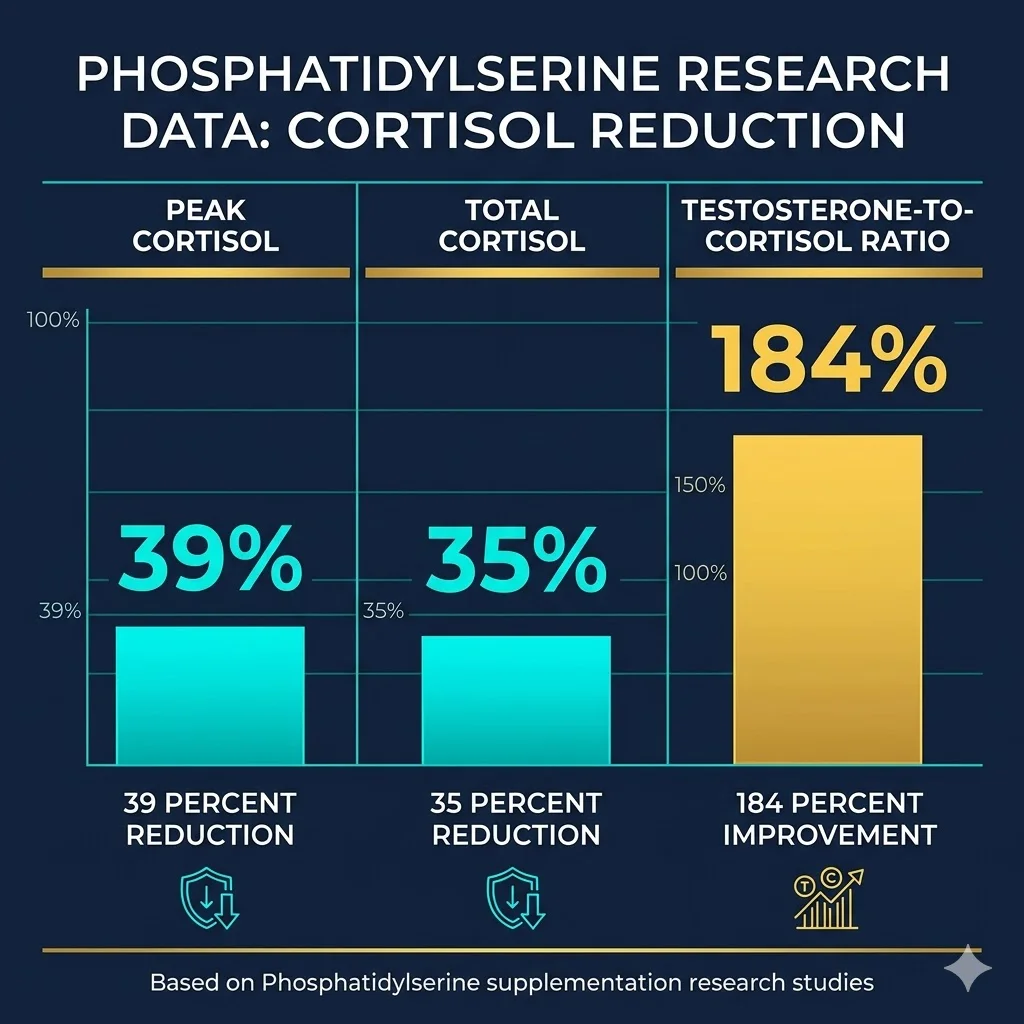
The mechanism appears to involve PS modulating corticotropin-releasing factor (CRF) receptor interactions in the hypothalamus, potentially inhibiting vasopressin (AVP) release, which in turn reduces ACTH secretion and the downstream cortisol cascade. The researchers described this as "rate-limited" — PS seems most effective at moderating cortisol during moderate stress rather than eliminating it during extreme exertion.
Perhaps the most nuanced finding came from a 2014 randomized controlled trial with 75 healthy men. Participants took either placebo, 200 mg, or 400 mg of a PS/phosphatidic acid complex daily for 42 days, then underwent the Trier Social Stress Test (a standardized psychological stressor involving a mock job interview and mental arithmetic under observation). In chronically stressed subjects, the 400 mg dose normalized ACTH (p = 0.010), salivary cortisol (p = 0.043), and serum cortisol (p = 0.035). In subjects with low baseline stress, the supplement had no measurable effect.
| Study | Dose | Duration | Cortisol Result |
|---|---|---|---|
| Monteleone et al., 1992 | 800 mg/day | 10 days | ACTH reduced (p = 0.003), cortisol reduced (p = 0.03) |
| Starks et al., 2008 | 600 mg/day | 10 days | Peak cortisol reduced 39%, AUC reduced 35% |
| Hellhammer et al., 2014 | 400 mg PS+PA/day | 42 days | Normalized cortisol in chronically stressed (p = 0.035) |
This distinction matters. PS does not just blunt cortisol universally — it appears to normalize an overactive stress response. The Hellhammer team described this as a "normalization of stress responsivity" rather than pharmacological suppression, which aligns with what you would want from a supplement rather than a drug. People whose HPA axis is already functioning normally do not see their cortisol pushed artificially low.
PS Recovers Dendritic Spines That Aging Strips Away
Beyond memory formation and stress regulation, PS plays roles in brain health that extend into territory typically reserved for pharmaceutical interventions — reducing neuroinflammation, supporting neuronal structure, and potentially modifying the course of neurodegenerative conditions.
Animal research has shown that chronic PS administration recovers dendritic spine density in the aged hippocampus. Dendritic spines are the tiny protrusions on neurons where most synaptic connections form. As we age, these spines thin out, and the connections they support grow weaker. PS appears to physically rebuild this infrastructure, which aligns with the observation from the Japanese memory trial that benefits persisted after supplementation stopped — you do not lose structural improvements the way you lose a chemical boost.
At the molecular level, a 2022 review in Frontiers in Aging Neuroscience documented that PS reduces pro-inflammatory cytokines TNF-alpha and IL-1beta while increasing anti-inflammatory factors TGF-beta and PGE2. It achieves this through PS receptor signaling (Mer, CD36, PSR) that inhibits the NFkB pathway — the same inflammatory master switch targeted by many prescription anti-inflammatory drugs. For a naturally occurring phospholipid with FDA GRAS status, this is a notable anti-inflammatory profile.
PS also maintains levels of key neurotransmitters that decline with age. Research has documented that it prevents the loss of acetylcholine-producing neurons, recovers dopamine discharge, and improves glutamic acid neurotransmission. This is not the same as flooding the brain with extra neurotransmitters the way a stimulant might — PS supports the neurons that produce these chemicals, keeping the machinery intact rather than temporarily amplifying its output.
| Neuroprotective Action | Mechanism | Evidence Level |
|---|---|---|
| Anti-inflammatory | Reduces TNF-alpha, IL-1beta; inhibits NFkB | Multiple preclinical + clinical studies |
| Structural repair | Recovers dendritic spine density | Preclinical (aged animal models) |
| Neurotransmitter support | Maintains ACh neurons, recovers dopamine | Preclinical + mechanistic studies |
| Cortisol normalization | Restores HPA axis function, circadian rhythm | Multiple RCTs |
| Synaptic signaling | Activates PI3K/Akt, PKC, Raf/Ras | Mechanistic studies (NIH) |
In clinical settings, PS supplementation at 100 mg three times daily for 12 weeks significantly improved cognitive impairment in Alzheimer's patients, with the most pronounced effects in early-stage disease. Parkinson's patients receiving PS showed improvements in motivation, anxiety, and emotional affect, though elevated PS in PD brains has also been linked to alpha-synuclein aggregation — a complexity that underscores why PS is better described as a modulator than a simple "brain booster."
A study in elderly patients with treatment-resistant major depression found that PS combined with omega-3 fatty acids normalized salivary cortisol levels and restored the normal morning cortisol peak in responders, while simultaneously improving depression scores from severe (HAM-D17 21.1) to near-remission levels (8.6) over 12 weeks. The biological normalization — not just symptom improvement — distinguished responders from non-responders, suggesting PS works through measurable hormonal pathways rather than placebo mechanisms.
Children with ADHD have also shown benefits. Two separate clinical studies found that PS at 200 to 250 mg daily significantly improved ADHD symptoms over treatment periods of two to seven months. While these represent preliminary evidence rather than definitive proof, they point to PS having relevance across the lifespan, not just in aging populations.
What to Eat, What to Supplement, and How Much
Your body produces some PS on its own, and you get additional amounts from food. The richest dietary sources include organ meats (particularly liver and kidney), fish, soybeans, eggs, and white beans. However, the typical Western diet provides only about 130 mg of PS per day — well below the 300 to 800 mg range used in clinical trials showing cognitive benefits.
| Food Source | PS Content (approximate) | Notes |
|---|---|---|
| Bovine brain | 713 mg per 100 g | Historical source; rarely consumed today |
| Atlantic mackerel | 480 mg per 100 g | Also provides DHA for PS synthesis |
| Chicken heart | 414 mg per 100 g | Organ meat category |
| Atlantic herring | 360 mg per 100 g | Fatty fish source |
| Soy lecithin | Up to 200 mg per 100 g | Most common supplement source |
| White beans | 56 mg per 100 g | Plant source |
| Egg yolk | 45 mg per 100 g | Moderate source |
Modern PS supplements come primarily from soy, sunflower, or marine (fish) sources. The original research used bovine cortex-derived PS, which is no longer commercially available due to concerns about transmissible diseases. Soy-derived PS has a somewhat different molecular profile — the fatty acid tails differ from bovine PS — but clinical trials with soy-PS have still demonstrated measurable cognitive and cortisol-modulating effects.
The Cleveland Clinic notes that adults typically take 100 to 200 mg daily, though clinical trials have used doses ranging from 100 mg to 800 mg. The Alzheimer's Drug Discovery Foundation reports a range of 80 to 500 mg across studies. Based on the available evidence, a reasonable breakdown looks like this:
- General cognitive support: 100 to 300 mg daily, taken with meals containing fat for better absorption
- Stress and cortisol management: 400 to 600 mg daily, based on the exercise and psychological stress trials
- Cognitive decline concerns: 300 mg daily (100 mg three times per day), matching the Alzheimer's trial protocols
PS supplements enriched with DHA or omega-3 fatty acids may offer an edge over plain PS. This makes biological sense — the brain's dominant PS species incorporates DHA in its fatty acid tail, and DHA availability directly drives PS synthesis. Supplementing both together supplies the raw material and the finished product simultaneously. The open-label extension study using PS-DHA showed cognitive benefits at just 100 mg daily, compared to 300 mg needed with PS alone.
The FDA classifies PS derived from soy lecithin, fish, and sunflower as "generally recognized as safe" (GRAS). Common side effects at standard doses include mild digestive discomfort, gas, and occasional insomnia. Higher doses carry proportionally greater risk of these effects. PS may increase bleeding risk and could interact with anticholinergic medications by opposing their mechanism — something worth discussing with a healthcare provider if you take any prescription drugs affecting brain chemistry or neurological function.
What PS Can Deliver and What It Cannot
PS occupies an unusual position in the supplement world — there is genuine research behind it, but the marketing often stretches well past what that research supports. Here is where the line actually falls.
| Claim | Reality |
|---|---|
| Myth: PS will noticeably sharpen your memory within days | Fact: The positive Japanese trial required six months before significant memory improvements emerged, and benefits became clearest three months after stopping. This is not a rapid-onset supplement. |
| Myth: PS works for everyone's memory | Fact: Benefits appeared primarily in people with existing memory complaints or lower baseline cognitive scores. Those with normal cognition showed ceiling effects on tests — there was no room to improve. A 2001 trial with 120 elderly participants found zero cognitive benefit at any dose over 12 weeks. |
| Myth: PS suppresses cortisol to dangerously low levels | Fact: The 2014 Hellhammer study showed PS normalizes cortisol in chronically stressed individuals but has no effect on people with healthy stress responses. It buffers overactivation rather than suppressing normal function. |
| Myth: All PS supplements are equivalent | Fact: The ADDF notes that different sources of PS have different chemical makeups, making direct trial comparisons difficult. Soy-derived, sunflower-derived, and marine-derived PS contain different fatty acid profiles. |
| Myth: PS is a proven treatment for Alzheimer's disease | Fact: Early trials showed benefits in AD patients, particularly in early-stage disease, but improvements were described as "short-lived or detectable only in severely impaired patients." No major health authority recommends PS as an Alzheimer's treatment. |
The honest summary: PS has real, replicated effects on cortisol regulation and emerging evidence for memory support in populations already experiencing decline. It is well-tolerated, has FDA GRAS status, and works through identified biological mechanisms rather than vague "brain support" claims. It is not a cognitive enhancer for people who already think well, and it takes months, not days, to show memory-related benefits. For stress and hormonal balance, the timeline is shorter — cortisol effects appeared within 10 to 42 days across studies.
Frequently Asked Questions
How long does it take for phosphatidylserine to work?
It depends on the target effect. Cortisol reduction has been measured within 10 days of supplementation at 600 to 800 mg daily. Memory improvements take considerably longer — the strongest positive trial required six months of daily supplementation, with benefits becoming most apparent three months after the treatment ended. If you do not notice changes after six months, PS may not be the right fit for your specific cognitive needs.
Can phosphatidylserine help with anxiety?
PS lowers cortisol, and chronically elevated cortisol is linked to anxiety symptoms. The 2014 Hellhammer study showed cortisol normalization in chronically stressed men, and the depression trial showed PS combined with omega-3s restored healthy cortisol circadian rhythms. However, PS is not FDA-approved for anxiety treatment, and the research on subjective anxiety relief (as opposed to hormonal changes) has been mixed, with most studies showing no significant changes in psychological stress ratings.
Is phosphatidylserine safe to take every day?
Clinical trials lasting up to six months have reported no serious adverse events at doses up to 800 mg daily. The FDA recognizes soy-derived, fish-derived, and sunflower-derived PS as GRAS. Common minor side effects include digestive discomfort and occasional insomnia. PS may increase bleeding risk, so discuss it with your doctor if you take blood thinners or have a bleeding disorder. Research on use during pregnancy and breastfeeding is insufficient, so most manufacturers recommend avoiding it during those periods.
Should I take phosphatidylserine with food?
Yes. PS is a fat-soluble phospholipid, and taking it with a meal that contains dietary fat improves absorption. Some research suggests that pairing PS with omega-3-rich foods (fatty fish, walnuts, flaxseed) may enhance its effectiveness, since DHA directly supports PS synthesis in the brain.
What is the difference between soy-derived and sunflower-derived PS?
Both are plant-based and contain phosphatidylserine, but they carry different fatty acid profiles in their molecular tails. Most clinical research has used soy-derived PS, which has the larger evidence base. Sunflower-derived PS is marketed as a soy-free alternative for people with allergies, but fewer clinical trials have directly tested it. The core PS headgroup is identical regardless of source — the difference lies in the attached fatty acids, and it remains unclear whether those differences affect brain outcomes.
Related Articles
- Gut-Brain Axis: How Your Microbiome Affects Mood and Cognition — Explores the biological pathways connecting digestive health to brain function and mental clarity.
- Adrenal Fatigue and HPA Axis Dysfunction — A deeper look at the stress response system that PS helps regulate, including signs of chronic HPA axis overactivation.
- NAD+ and NMN Supplements for Aging and Cellular Repair — Covers another class of supplements targeting brain aging and neuroprotection through cellular energy pathways.
- Inflammation, Chronic Disease, and Anti-Inflammatory Living — How chronic low-grade inflammation drives cognitive decline and what dietary strategies address it.
- Inositol for PCOS, Anxiety, and Hormonal Balance — Another phospholipid-adjacent supplement with evidence for mood, hormonal regulation, and cognitive support.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.