The $6.8 trillion wellness industry just named its next frontier
On January 27, 2026, the Global Wellness Summit released its annual trends report and put one word at the center: neurowellness. The concept is straightforward. Regulate the nervous system to support whole-body health, resilience, and recovery, rather than chasing individual symptoms like poor sleep or chronic inflammation after they've already taken hold.
Your nervous system governs sleep quality, immune function, digestion, hormonal balance, and emotional regulation. When it gets stuck in low-grade fight-or-flight from nonstop notifications, artificial light, and work that never ends, everything downstream suffers. Neurowellness targets the root: the stuck switch itself.
What makes this different from generic "stress management" advice is the emphasis on measurable physiology. Wearables like Oura and WHOOP turned a private struggle into a daily number -- your sleep score, your heart rate variability, your recovery readiness. When those numbers stay low for weeks, the message becomes hard to ignore. Something in the body's regulatory system has gone wrong, and telling yourself to relax will not fix it.
The Global Wellness Institute's press release framed the trend within a $6.8 trillion wellness economy that has been "rewritten by high-tech, medical, hyper-optimizing approaches" over the past two years. Neurowellness sits at the tension between that tech-driven optimization and a growing counter-movement demanding something more body-centered. Both sides converge on the same target: the autonomic nervous system.
Your autonomic nervous system: the operating system you never learned to use
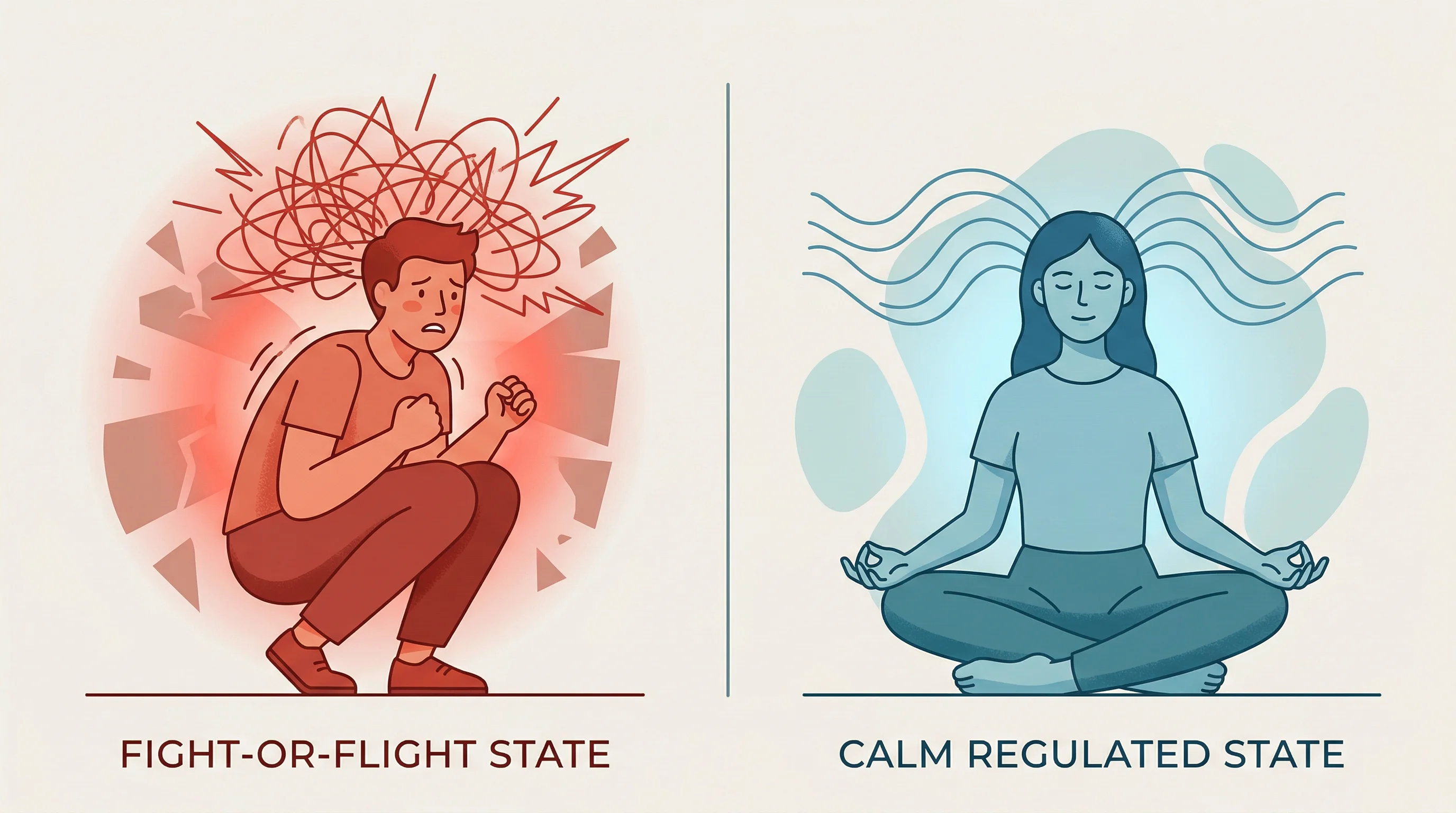
Your autonomic nervous system works like the operating system running beneath every app on your phone. You never interact with it directly, but when it crashes, nothing works. The ANS runs digestion, heart rate, breathing, immune response, and hormonal cycles without conscious input. It has two primary modes.
The sympathetic branch accelerates things: heart rate rises, pupils dilate, blood diverts to muscles, digestion pauses. This is the fight-or-flight response, evolved to save your life in acute danger. The parasympathetic branch, driven primarily by the vagus nerve, does the opposite. It slows heart rate, promotes digestion, tamps down inflammation, and signals the body that it is safe to recover. In a healthy person, these two systems trade dominance dozens of times per hour.
A meta-analysis in Psychiatry Investigation reviewing 37 studies on stress and heart rate variability illustrates the problem. Researchers Hye-Geum Kim and Bon-Hoon Koo at Yeungnam University found that stressed individuals most frequently showed reduced activity in the high-frequency HRV band, the direct marker of vagal (parasympathetic) function. Chronic psychological stress keeps the sympathetic branch activated while suppressing parasympathetic function. The accelerator stays pressed. The brake releases.
Agorastos Agorastos and colleagues described this in a Biomedicines review as "decreased dynamic adaptability" leading to "increased morbidity and mortality." When the operating system loses the ability to switch between modes, every organ it manages pays the price. Resting heart rate stays elevated. The immune system either overreacts or underperforms. Sleep stays shallow because the body never fully enters recovery mode.
Stephen Porges complicated this picture with Polyvagal Theory. Porges proposed that the vagus nerve operates through two circuits, not one. The newer "ventral vagal" circuit supports social engagement, calm communication, and a felt sense of safety. The older "dorsal vagal" circuit triggers shutdown and immobilization when threat becomes overwhelming. A 2025 review in Frontiers in Psychology documented how this framework has moved from controversial theory into clinical application across trauma therapy, cardiac rehabilitation, and developmental neuroscience. Your body does not just toggle between stressed and relaxed. It has a hierarchy of responses, and neurowellness aims to keep you in the ventral vagal state where social connection, clear thinking, and recovery are possible.
The vagus nerve is your body's longest cranial nerve. It travels from the brainstem through the neck and into the chest and abdomen, connecting to the heart, lungs, liver, and digestive tract. Roughly 80% of its fibers are afferent, meaning they carry information from the body to the brain rather than the other way around. Your brain is listening to your body far more than it is talking to it.
Vagal tone: the biomarker that predicts stress resilience
If neurowellness has a single measurable target, it is vagal tone. The proxy we use to track it is heart rate variability. HRV measures the variation in time between consecutive heartbeats. A healthy heart does not beat like a metronome. It speeds up slightly when you inhale and slows down when you exhale -- a phenomenon called respiratory sinus arrhythmia, controlled by the vagus nerve.
Higher HRV means stronger vagal tone: the parasympathetic brake works well, and the body can shift between activation and recovery efficiently. Lower HRV signals a nervous system stuck in one gear, usually sympathetic overdrive.
Asaf Gitler and colleagues at the University of Haifa reported in a 2025 narrative review that HRV correlates with vagal nerve activity at r=0.88, making it one of the most reliable non-invasive proxies for autonomic function. The same review documented that reduced HRV is associated with cardiovascular disease, hypertension, systemic inflammation, and mental health disorders. People with higher resting HRV show better emotional regulation, greater cognitive flexibility, and faster recovery from acute stress.
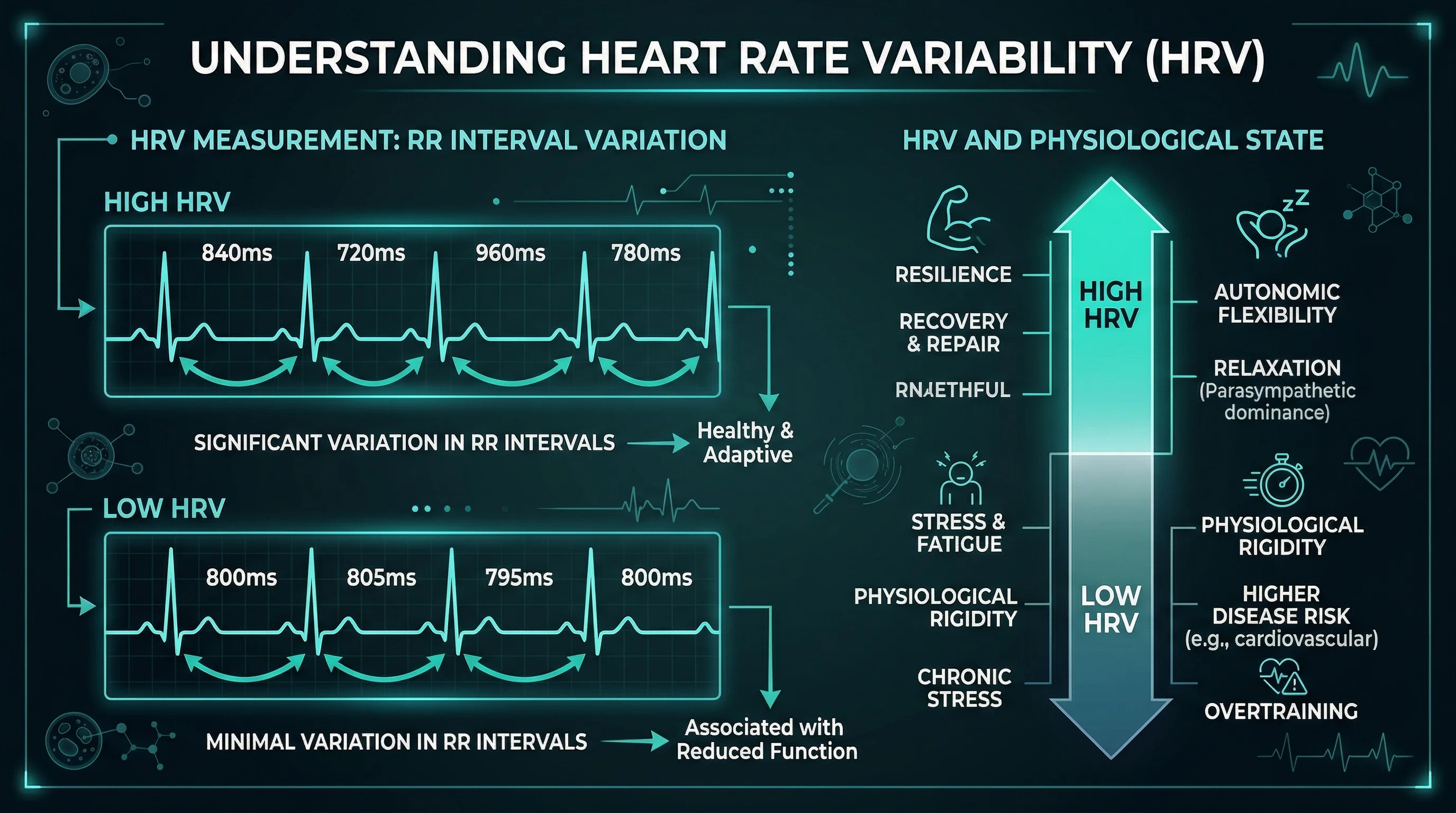
The Kim et al. meta-analysis established that SDNN, the standard deviation of normal-to-normal heartbeat intervals, functions as "an index of physiological resilience against stress." When HRV is large and irregular (in the healthy sense), the SDNN value increases, reflecting a nervous system with room to respond to challenges. When it drops, the system has lost flexibility.
HRV responds to intervention, which is what makes it clinically useful. Unlike cortisol, which requires blood draws or saliva tests and fluctuates with time of day, HRV can be measured continuously through consumer wearables. The specific HRV components -- particularly RMSSD (root mean square of successive differences) and high-frequency power -- are reliable indicators of parasympathetic activity even from recordings as brief as one minute.
You can watch your vagal tone change in response to a breathing exercise, a cold shower, or a terrible night of sleep. That feedback loop separates vagal tone from vague wellness concepts like "stress levels" or "energy." Intervention leads to measurable change. That measurability is driving the neurowellness trend.
| HRV metric | What it measures | What it tells you |
|---|---|---|
| SDNN | Standard deviation of beat-to-beat intervals | Overall autonomic flexibility and stress resilience |
| RMSSD | Beat-to-beat variation (short-term) | Parasympathetic (vagal) activity, even from 1-minute recordings |
| HF power | High-frequency oscillations (0.15-0.4 Hz) | Direct vagal nerve influence on the heart |
| LF power | Low-frequency oscillations (0.04-0.15 Hz) | Mixed sympathetic and parasympathetic influence, baroreflex activity |
| LF/HF ratio | Balance between frequency bands | Sympathovagal balance (higher ratio = more sympathetic dominance) |
Tech-assisted nervous system regulation: what works and what's marketing
The Global Wellness Summit report splits the neurowellness device market into "hard-care" and "soft-care." Hard-care means technology that directly stimulates or monitors the nervous system: vagus nerve stimulation devices, EEG headbands, neurofeedback platforms. Soft-care covers practice-based interventions -- breathwork, movement, touch therapy -- that achieve similar physiological effects without electronics. Both have research behind them. But the evidence base varies wildly across products, and that unevenness matters when people are spending real money.
Vagus nerve stimulation has the deepest clinical history. The technology dates to the 1980s, when Jacob Zabara and colleagues developed the first modern implantable VNS device for treatment-resistant epilepsy. Since then, implanted VNS has gained FDA approval for epilepsy, treatment-resistant depression, obesity, migraine and cluster headache, and post-stroke motor rehabilitation, according to a 2024 review by Christopher Austelle and Bashar Badran in Bioelectronic Medicine. The mechanisms are well-documented: VNS modulates norepinephrine and serotonin levels, decreases inflammatory cytokines through the cholinergic anti-inflammatory pathway, and increases brain-derived neurotrophic factor in the hippocampus.
The consumer VNS market is a different animal. Devices like Pulsetto, Sensate, Neuvana, and Nurosym use transcutaneous (through-the-skin) stimulation rather than implanted electrodes. Two approaches exist: transcutaneous cervical VNS (tcVNS) targets the vagus nerve through the neck, and transcutaneous auricular VNS (taVNS) stimulates the auricular branch through the ear. The Cleveland Clinic and Mayo Clinic both note that FDA-approved VNS remains limited to specific medical conditions with implanted devices, while the consumer transcutaneous market operates in a different regulatory space.

The safety data for transcutaneous approaches is generally favorable, with a caveat. A systematic review and meta-analysis in Scientific Reports evaluated 177 taVNS studies covering 6,322 subjects and found an overall adverse events incidence of 12.84 per 100,000 person-minutes-days. The most common complaints were ear pain, headache, and tingling -- all mild and transient. No causal relationship between taVNS and severe adverse events was established. But 55.37% of the studies did not even mention whether adverse events occurred. Absence of reporting is not absence of risk.
Denise Bellinger, associate research professor at Loma Linda University, offered a more cautious take in an interview with BrainFacts.org. She noted that external VNS devices face a basic precision problem: "A fully external VNS device can't be implanted right on the nerve." The targeting is less precise, which means both efficacy and side effect profiles differ from clinical-grade devices. Bellinger warned that commercial VNS devices carry potential risks including cardiac complications due to the vagus nerve's direct connection to the heart, and recommended physician oversight for any VNS use.
HRV biofeedback has stronger evidence behind it. Instead of delivering electrical stimulation, it trains you to regulate your own autonomic function through paced breathing. A systematic review in Applied Psychophysiology and Biofeedback established guidelines for HRV biofeedback methods. The Gitler et al. review documented research supporting its efficacy in improving cardiovascular outcomes, managing hypertension, and reducing depressive and anxiety symptoms. No documented serious adverse effects. Measurable changes in vagal tone that persist beyond the training session. And the cost barrier is low: several smartphone apps do this adequately.
| Approach | Mechanism | Evidence level | Accessibility |
|---|---|---|---|
| Implanted VNS | Direct electrical stimulation of vagus nerve | FDA-approved for 5 conditions; decades of clinical trials | Requires surgery; prescription only |
| Transcutaneous VNS (consumer) | Electrical stimulation through skin at neck or ear | Meta-analysis shows safety; efficacy evidence growing but uneven | Over-the-counter; $200-500 |
| HRV biofeedback | Paced breathing with real-time HRV monitoring | Systematic reviews support efficacy for hypertension, anxiety, depression | Apps and wearables; low cost |
| Neurofeedback (EEG) | Real-time brain wave monitoring and training | Established for ADHD; emerging for stress/sleep | Clinical sessions or home devices ($200-800) |
A practical daily neurowellness protocol
A handful of interventions have consistent evidence for improving vagal tone and autonomic balance. None require expensive devices. They all work through the same mechanism: activating the parasympathetic branch to counterbalance chronic sympathetic overdrive.
Resonance frequency breathing. This is the single best-supported non-pharmacological intervention for improving vagal tone. The technique involves breathing at approximately 5.5 to 6 breaths per minute, far slower than most people breathe at rest (typically 12-20 breaths per minute). At this frequency, breathing synchronizes with the body's baroreflex cycle, creating a resonance effect that amplifies heart rate variability. The systematic review of HRV biofeedback methods confirmed that this frequency range, individually calibrated through biofeedback, produces the strongest improvements in baroreflex sensitivity and autonomic balance. In practice: inhale for about 5.5 seconds, exhale for 5.5 seconds, repeat for 10 to 20 minutes.
Extended exhalation. If resonance breathing feels too structured, a simpler approach works through the same vagal pathway. Respiratory sinus arrhythmia -- the natural acceleration of heart rate during inhalation and deceleration during exhalation -- means that longer exhales directly increase parasympathetic activation. A pattern like inhaling for 4 seconds and exhaling for 6-8 seconds shifts autonomic balance toward recovery without requiring precise frequency calibration.
Cold exposure. Brief cold exposure (cold shower, face immersion in cold water, or cold water applied to the neck) triggers the diving reflex, a vagal activation response. The mechanism is direct: cold receptors in the face and neck stimulate the vagus nerve, producing an immediate drop in heart rate and shift toward parasympathetic dominance. This is not about ice bath endurance culture. Even 30 seconds of cold water at the end of a warm shower produces a measurable vagal response.

Humming and singing. The vagus nerve runs past the vocal cords, and vocal vibration directly stimulates vagal fibers. The Gitler et al. review noted that the Safe and Sound Protocol (SSP), an auditory-based intervention grounded in Polyvagal Theory, targets the ventral vagal complex through filtered music to promote social engagement, emotional regulation, and parasympathetic activation. You do not need the SSP protocol to activate this pathway. Humming during exhales, singing, or even gargling vigorously produces measurable vagal stimulation.
Movement that stays out of fight-or-flight. High-intensity interval training and competitive exercise activate the sympathetic branch. For nervous system regulation, the better choices are walking (especially outdoors), yoga, tai chi, and swimming. These activities maintain enough physical demand to produce cardiovascular benefit while keeping the nervous system in a parasympathetic-friendly zone. The goal is not more intensity but more time in recovery-compatible states.
| Practice | Mechanism | Minimum effective dose | When to do it |
|---|---|---|---|
| Resonance breathing (5.5 breaths/min) | Baroreflex synchronization, vagal amplification | 10 minutes, once daily | Morning or before a stressful event |
| Extended exhalation (4 in / 6-8 out) | Respiratory sinus arrhythmia, parasympathetic shift | 5 minutes, as needed | Anytime you feel activated |
| Cold exposure (face/neck) | Diving reflex, direct vagal stimulation | 30-90 seconds | Morning, after exercise |
| Humming/singing | Vocal cord vibration stimulates vagal fibers | 5 minutes | During breathing practice or casually |
| Gentle movement (walking, yoga) | Parasympathetic-compatible cardiovascular benefit | 20-30 minutes | Daily |
When neurowellness becomes medical: knowing the line
Breathing exercises and cold showers are safe for almost everyone. The device end of neurowellness gets more complicated, and the boundary between self-care and medical intervention matters more than the marketing implies.
Implanted VNS is surgery. The Cleveland Clinic lists contraindications including pregnancy, breathing disorders (asthma, COPD, sleep apnea), active peptic ulcer disease, heart arrhythmias, and a history of schizophrenia or rapid-cycling bipolar disorder. Side effects include voice changes, hoarseness, throat pain, headache, shortness of breath, and trouble swallowing. These are not minor inconveniences, and they illustrate why implanted VNS remains a last-resort treatment for specific medical conditions.
Consumer transcutaneous devices occupy a gray zone. The Scientific Reports meta-analysis found that taVNS adverse events, when they occurred, were mild: ear pain at the stimulation site, headache, and skin tingling. The overall incidence was low at 12.84 per 100,000 person-minutes-days. But Austelle and Badran noted that cardiac events from implanted VNS, specifically bradycardia and asystole, occur in approximately 1 per 1,000 cases. While transcutaneous devices avoid surgical risks, the vagus nerve's direct connection to cardiac function means that any form of vagal stimulation carries at least theoretical cardiovascular risk, particularly for people with existing heart conditions.
Bellinger's point about targeting precision bears repeating. An external device stimulating through the skin of the ear or neck works with less control than a surgically implanted electrode wrapped around the nerve. The research is promising but incomplete. Using a consumer VNS device for stress relief is a different risk proposition than using it as an unmonitored treatment for a diagnosed condition.
Several signals suggest nervous system dysregulation has crossed from a lifestyle concern into a medical one:
- Persistent sleep disruption that does not respond to sleep hygiene improvements
- Resting heart rate that stays elevated (above 80-85 bpm) for weeks without explanation
- HRV that trends consistently below age-adjusted norms on your wearable
- Panic attacks, dissociation, or emotional shutdown episodes
- Digestive symptoms (IBS, chronic nausea) that coincide with stress patterns
- Post-viral autonomic dysfunction (common after COVID-19, where reduced HRV has been observed in recovering patients)
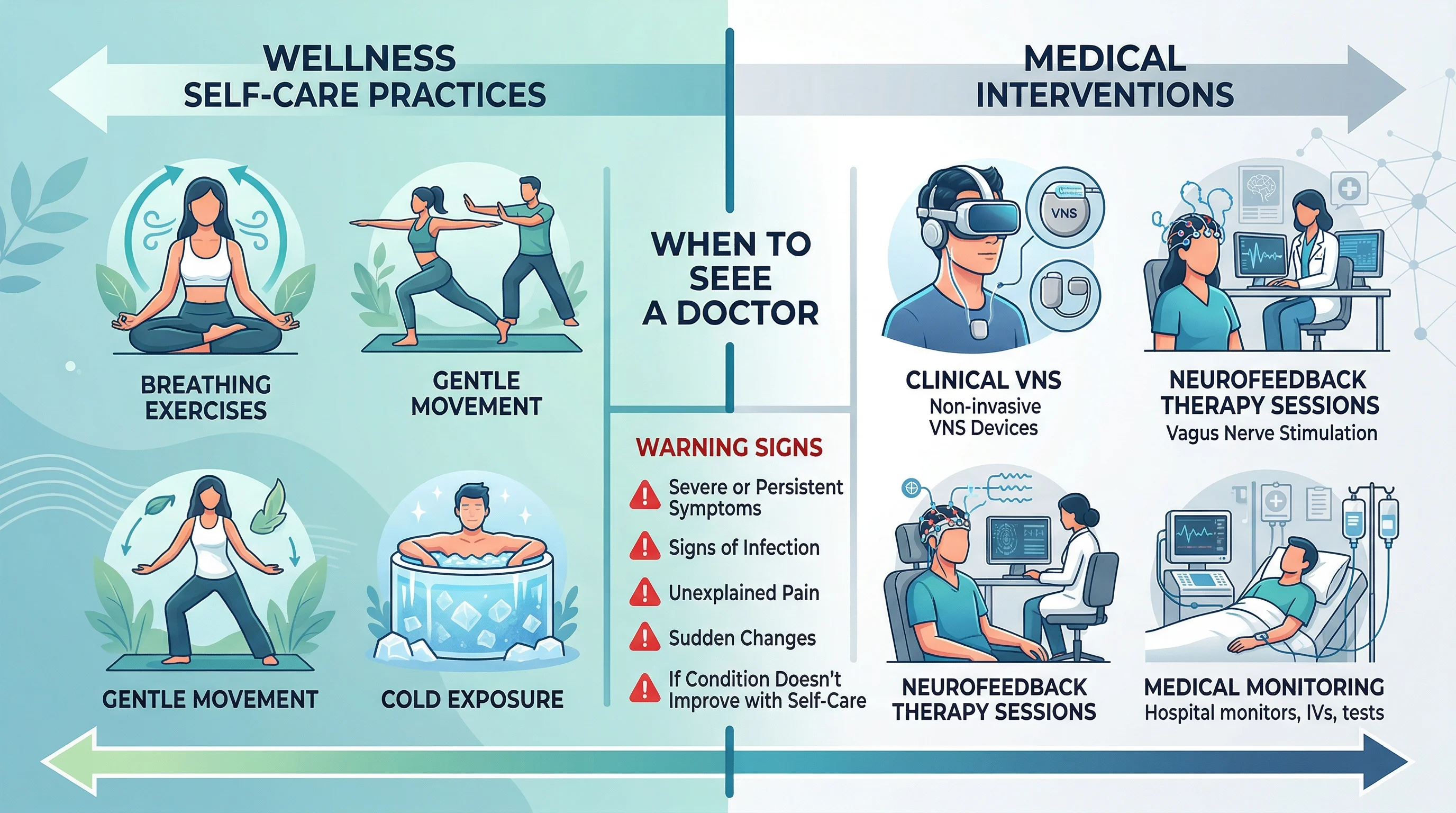
Any of those patterns warrant evaluation by a clinician familiar with autonomic function, not a consumer device or a breathing app. Neurowellness practices work as daily maintenance for people whose nervous systems function within normal range but spend too much time in sympathetic activation. When autonomic systems are genuinely dysregulated from trauma, illness, or structural causes, the interventions need to be supervised, targeted, and often medical.
Frequently Asked Questions
Can you measure vagal tone at home?
Yes. Heart rate variability, the primary proxy for vagal tone, can be tracked through consumer wearables like Oura Ring, Apple Watch, WHOOP, and Garmin devices. The most useful metrics are RMSSD (for real-time parasympathetic activity) and SDNN (for overall autonomic flexibility). Morning resting measurements tend to be the most consistent and informative. For clinical-grade accuracy, a chest strap monitor produces better data than wrist-based optical sensors, but wrist devices are reliable enough for tracking trends over time.
How quickly does HRV respond to breathing exercises?
Within minutes. A single session of resonance frequency breathing at 5.5 to 6 breaths per minute produces measurable changes in HRV during the session itself. Lasting improvements in baseline resting HRV typically require consistent daily practice over 2 to 4 weeks. The effect compounds: regular practice trains the baroreflex arc to become more responsive, producing higher resting vagal tone even outside of breathing sessions.
Are consumer vagus nerve stimulation devices safe?
For most healthy adults, transcutaneous VNS devices appear to carry a low risk of adverse effects. The most common side effects are mild: ear discomfort, headache, and skin tingling at the electrode site. The evidence base is still developing, and people with heart conditions, implanted cardiac devices, or autonomic disorders should consult a physician before use. These are not regulated as medical devices for most of their marketed purposes, which means oversight of safety and efficacy claims is limited.
Is polyvagal theory scientifically accepted?
Polyvagal theory remains debated. Its core claim -- that the autonomic nervous system operates through a hierarchy of three response states rather than a simple two-branch toggle -- has gained clinical traction and influenced trauma therapy approaches. A 2025 review described its movement from theory into clinical application across multiple fields. Some neuroscientists have critiqued specific physiological claims, particularly about the evolutionary timeline of vagal circuits. The practical interventions derived from the theory (breathing techniques, social engagement exercises, auditory stimulation) have independent evidence supporting their effects on vagal tone, regardless of whether the full theoretical framework holds up.
What is the difference between neurowellness and mental health treatment?
Neurowellness focuses on the physiological regulation of the nervous system. Mental health treatment addresses emotional, psychological, and behavioral symptoms. As the Global Wellness Summit's report put it, neurowellness "focuses on physiology, how the nervous system actually shifts between activation and recovery." It is not a replacement for therapy, medication, or psychiatric care. Instead, it addresses the body's regulatory infrastructure that underlies mental health. Many clinicians are integrating both approaches, using neurowellness techniques as adjuncts to traditional treatment.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.