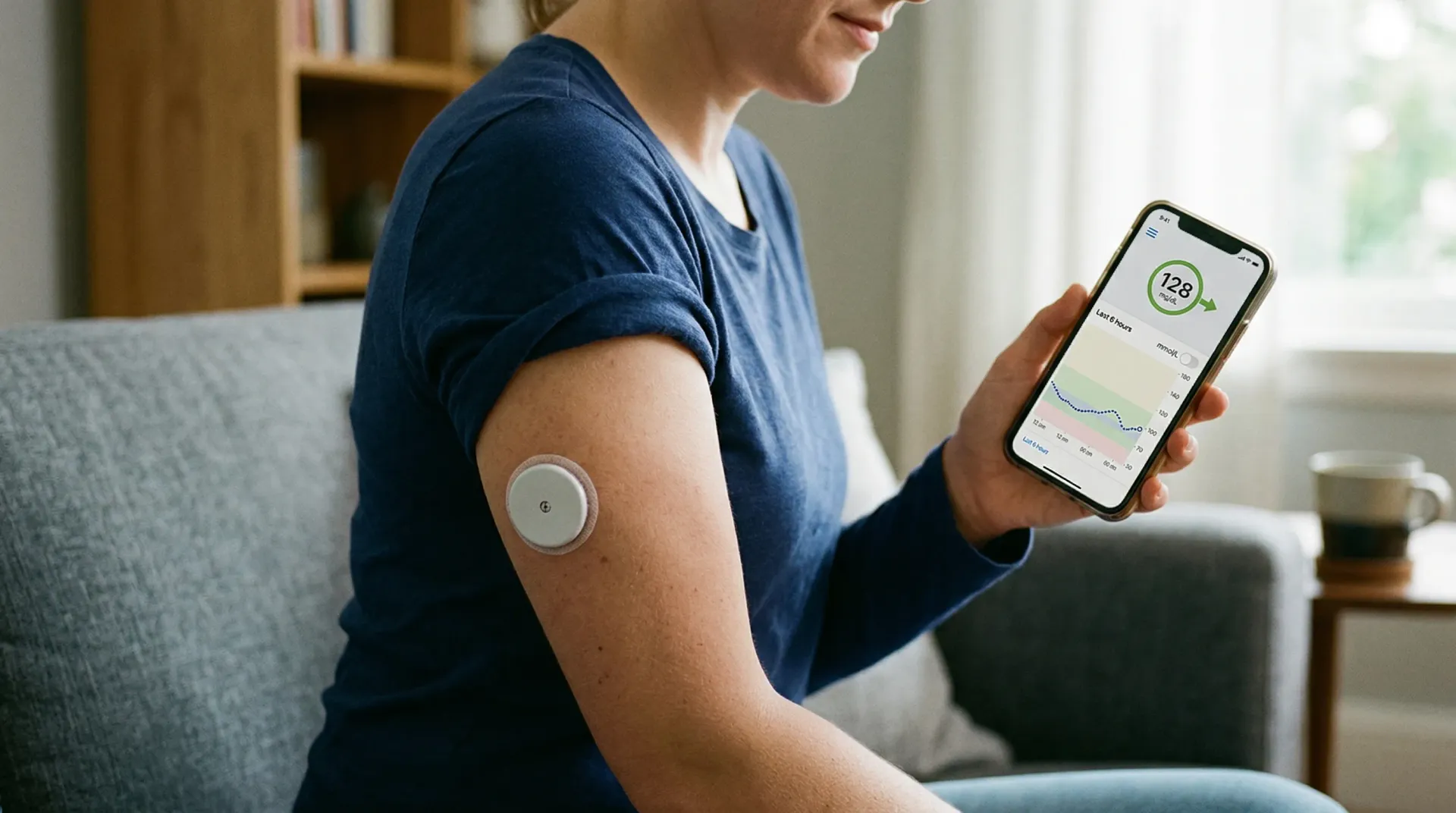
A $63 billion market that used to ignore half its customers
For most of the wearable tech era, "women's health" meant a period tracker bolted onto a fitness app. You logged your cycle start date, maybe got a push notification about your predicted fertile window, and that was it. The underlying assumption was that female biology was a footnote to the real business of counting steps and measuring VO2 max.
That assumption is collapsing. The global FemTech market hit $63.14 billion in 2025, with projections reaching $266.99 billion by 2035 at a compound annual growth rate of 15.51%. The fastest-growing segment is not fertility. It is menopause.

The money followed. According to market research from Astute Analytica, roughly 75% of women seeking midlife care were previously ignored by traditional healthcare systems. That is a massive underserved population with spending power and unmet needs.
The demand is also coming from women themselves. A survey by menstrual tracking app Clue of more than 26,000 users found that 70% of respondents were not sure what perimenopause actually was. Fewer than half of participants over age 51 had heard about perimenopause from a healthcare provider. When women cannot get answers from their doctors, they start looking for tools that will give them data they can interpret on their own.
This is already reshaping product strategy at companies that used to focus exclusively on fertility. Mira CEO Sylvia Kang told The Verge that 40% of Mira's users are not trying to conceive — they want to understand menopause, PCOS, and hormonal symptoms. Researchers at Northumbria University found in a 2025 study of 29 peri- and post-menopausal women that menopause tracking apps helped women combat what the researchers called "epistemic injustice" in healthcare settings — being dismissed or disbelieved when describing their symptoms. Women showed up to appointments with app-generated data visualizations, and their doctors took them more seriously.
Hormone tracking tech is growing because women have been asking questions their healthcare system was not equipped to answer. The technology is filling a gap that should not have existed.
Your hormones are not declining — they are becoming unpredictable
The popular image of perimenopause as a slow, gradual decline in estrogen is wrong. What actually happens is more like a radio signal losing its lock — hormones spike, crash, double-peak, and flatline in patterns that change month to month. That unpredictability is what makes perimenopause so hard to track with standard wearables designed for regular, repeating cycles.
The Staging of Reproductive Aging Workshop (STRAW) criteria, the clinical standard for classifying where a woman falls in the menopause transition, define the variable stage of perimenopause as cycles that differ by 7 or more days within a 10-month period. In a retrospective analysis of 42 women aged 40 to 50, Dr. Maria Meyers and colleagues at Marquette University found no women in regular cycles past age 47. But the transition itself started as early as age 41.
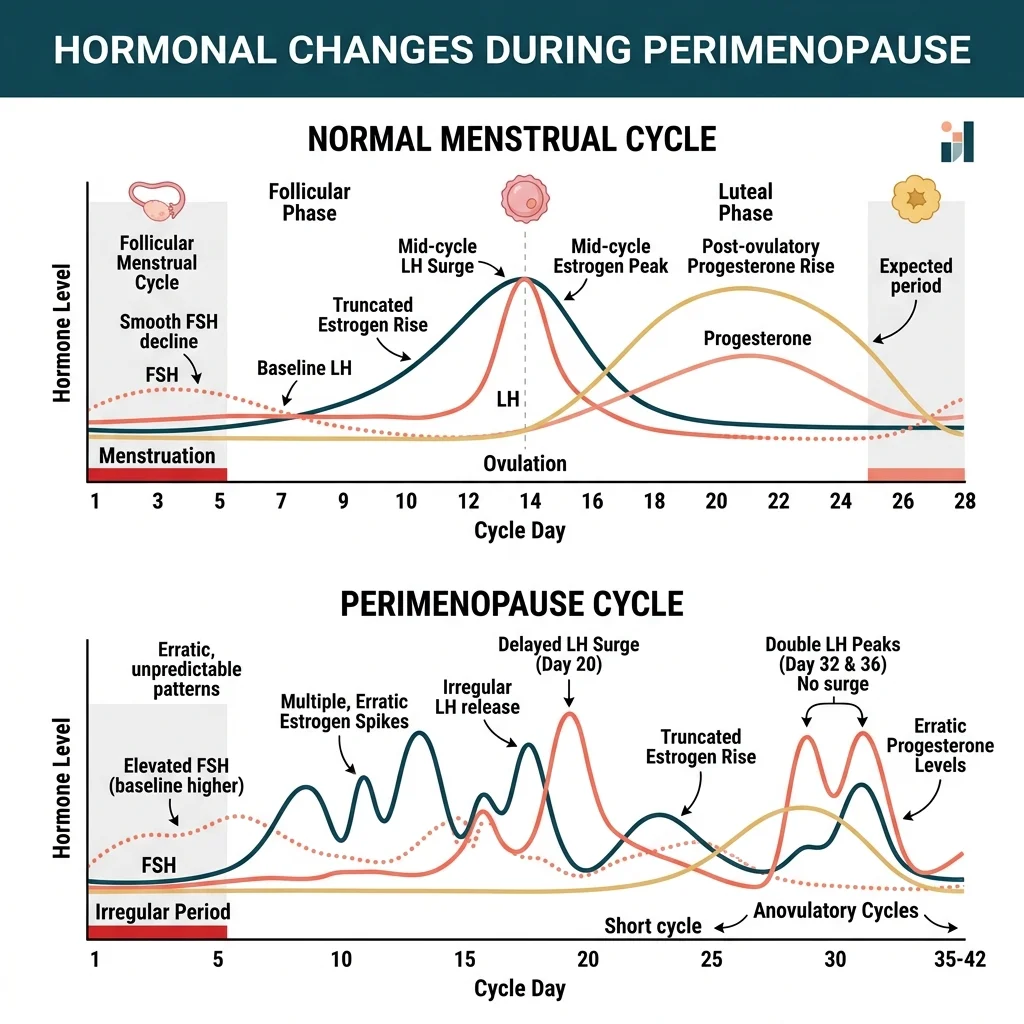
What the Marquette researchers found with quantitative hormone monitoring was that perimenopause produces a distinct set of hormonal signatures: delayed luteinizing hormone surges that throw off ovulation timing, truncated estrogen rises that give little warning before the LH peak, double LH surges in a single cycle, and stretches of continuously elevated estrogen and LH with no clear ovulatory pattern. Think of it like a conductor who keeps changing tempo mid-symphony — the musicians (your organs) are still playing, but nobody is quite sure what beat they are on.
This chaos affects more than just fertility. Oura Ring data shows an overwhelming increase in members over 40 tagging symptoms like insomnia, night sweats, hot flashes, anger, and migraines. Heart rate variability — a measure of your nervous system's flexibility — tends to drop during hot flash episodes, and that drop correlates with fatigue, anxiety, and disrupted sleep. One in ten women will leave the workforce earlier than they planned because of unmanaged menopause symptoms.
Standard fitness trackers were not built to make sense of any of this. They assume a roughly predictable cycle and generate alerts based on averages. When your hormones stop following the average, those alerts become noise. Almost 50% of women in the Clue survey did not know it was still possible to get pregnant during perimenopause — a gap in understanding that generic cycle tracking does nothing to close.
CES 2026 turned bodily fluids into a product category
At CES 2026 in January, the health tech floor looked different. As Verge senior reviewer Victoria Song put it, the show was "awash in bodily fluids." Urine, blood, sweat, saliva — all of it was being analyzed by devices that a year ago would have sounded like science fiction. The shift was not just about what the devices measured, but who they were measuring it for. Women's hormonal health was, for the first time, a major product category at the world's biggest consumer electronics show.

The standouts fell into three categories: hormone analyzers, symptom trackers, and metabolic sensors.
Mira Ultra4 ($249) was the most talked-about hormone device. The system pairs an egg-shaped analyzer with disposable test wands that measure four reproductive hormones simultaneously — follicle-stimulating hormone (FSH), luteinizing hormone (LH), estrone-3-glucuronide (E3G, a urinary metabolite of estrogen), and pregnanediol glucuronide (PdG, a progesterone metabolite). You collect a urine sample, insert the wand into the analyzer, and get quantitative results in about 16 minutes. The device is FDA-listed as a Class I device, which means low regulatory risk but also means it is classified as wellness, not diagnostic.
Peri ($449) took a different approach. Winner of PCMag's Best Wellness Tech award at CES, Peri is an adhesive patch worn on the torso that uses accelerometry, electrodermal activity (EDA), optical heart rate (PPG), and temperature sensors to detect perimenopause symptoms in real time. Co-founder Donal O'Gorman told PCMag that the company developed its own algorithms to create a "digital biomarker of a hot flash" by combining signals from all sensors simultaneously. The companion app tracks symptoms over time with no subscription fee. The 3M-developed adhesive needs changing every 10 to 14 days. One limitation O'Gorman acknowledged: the device cannot detect brain fog.
Abbott Lingo ($49–$249) represents the metabolic angle. This over-the-counter continuous glucose monitor, FDA-cleared in June 2024, streams real-time glucose data from a biosensor worn on the back of the arm for up to 14 days. Built on the same FreeStyle Libre sensor technology used by over 6 million people with diabetes, Lingo is designed for people without diabetes who want to understand how food, exercise, and stress affect their blood sugar. For perimenopausal women, this matters because hormonal shifts directly influence insulin sensitivity and glucose metabolism.
Other notable devices at CES included Vivoo's FlowPad, a menstrual pad that analyzes period blood for ovarian health, fertility, and hormone markers, and OhmBody, an earpiece using neurostimulation to reduce period pain by engaging the trigeminal and vagus nerves.
| Device | Type | Price | What it tracks | Subscription |
|---|---|---|---|---|
| Mira Ultra4 | Hormone analyzer | $249 | FSH, LH, E3G, PdG (urine) | None (wands ~$99/pack) |
| Peri | Symptom tracker | $449 | Hot flashes, night sweats, sleep, anxiety | None |
| Abbott Lingo | Glucose monitor | $49–$249 | Continuous glucose | None |
| FlowPad | Menstrual analysis | TBD | Ovarian health, fertility, hormones (period blood) | TBD |
| OhmBody | Pain management | TBD | Menstrual cramp relief (neurostimulation) | TBD |
Fluorescence assays vs. temperature proxies: two different philosophies
At-home hormone tracking splits into two camps. One measures hormones directly from body fluids. The other infers hormonal changes from proxy signals like skin temperature and heart rate variability. The distinction matters because each approach answers a different question.
Direct measurement devices like the Mira monitor use a technique called immunochromatography with fluorescence labeling. In plain terms: you provide a urine sample on a test wand. The wand contains antibodies that bind to specific hormone metabolites in your urine. When a hormone is present, it triggers a fluorescent reaction whose intensity corresponds to the hormone's concentration. A reader device measures that fluorescence and converts it to a quantitative number — not just "high" or "low," but an actual measurement in nanograms per milliliter.
This is meaningfully different from older qualitative monitors like the ClearBlue Fertility Monitor, which uses optical intensity measurement and reports results as threshold categories: Low, High, or Peak. As a 2025 validation study from the University of Calgary explained, the ClearBlue system tells you whether a hormone crossed a preset line. Mira tells you how far it went. During perimenopause, when hormone levels are erratic and the "line" may not mean what it did at age 30, that distinction becomes the difference between useful data and guesswork.
Four quantitative at-home monitors are now on the market — Mira, Proov, Inito, and Oova — each using disposable test wands with the same basic immunoassay chemistry but different companion apps and algorithmic interpretations.
Proxy-based tracking works differently. Devices like the Oura Ring, Apple Watch, and Garmin smartwatches measure skin temperature continuously and use the data to infer where you are in your cycle. A 2024 study by researchers at SRI International analyzed data from 120 women wearing Oura Rings and found that menstrual skin temperature variation is better described as a smooth oscillation (a cosinor curve) than as the traditional biphasic "low follicular / high luteal" model taught in textbooks. When temperature data did not oscillate, it consistently indicated anovulatory cycles — cycles without ovulation.
Direct hormone testing gives you specific numbers about what your reproductive hormones are doing right now. Proxy tracking gives you pattern recognition over weeks and months. Are your cycles still oscillating? Is ovulation happening? Both have clinical value.
The accuracy question: promising data, honest gaps
The research is encouraging but unfinished. No consumer hormone tracking tool has been validated against the gold standard (serum blood draws combined with transvaginal ultrasound) in large perimenopause-specific populations. What exists is a growing set of smaller studies that point in a consistent direction.
The strongest validation data comes from Dr. Thomas Bouchard's team at the University of Calgary, who compared the Mira monitor against the ClearBlue Fertility Monitor in 16 women, including 8 in perimenopause across 35 cycles. The LH surge detection between the two devices was highly correlated: R = 0.83 in perimenopause cycles and R = 0.94 in postpartum cycles, both statistically significant at p < 0.001. An earlier pilot study of the same comparison in regular cycles found an even stronger correlation of R = 0.98.
The perimenopause correlation being lower than the regular-cycle number is expected and honest. Perimenopause hormones are more erratic, so any measuring tool will show more variance. An R of 0.83 is still strong, but it means roughly 1 in 6 readings may not line up perfectly between devices.
For wearable temperature tracking, the SRI International study of 120 women using Oura Rings found high agreement between their skin temperature rhythm method and LH surge detection for identifying ovulatory cycles. But the researchers were careful to note that their r² threshold of 0.4 for reliable rhythm metrics was specific to their dataset and device. Transferability to other populations remains to be assessed.
One complication that cuts across all methods: nearly 47% of regularly menstruating individuals experience at least one premature LH surge — a temporary spike that looks like ovulation on a test but does not actually trigger egg release. During perimenopause, these false signals become more common. LH home test kits have been shown to achieve up to 97% accuracy compared to ultrasound in identifying ovulatory cycles, but that number comes from younger populations with regular cycles. Perimenopause-specific accuracy data is still thin.
The current generation of home hormone monitors and wearable trackers produces data that correlates well with clinical tools, but they are not diagnostic devices. Use them to spot trends, build a hormonal baseline, and have more informed conversations with your doctor. They do not replace clinical testing.
Researchers at Northumbria University documented an additional concern: even when women bring app-generated data to appointments, clinician distrust of patient-generated health data remains a barrier in some healthcare settings. The technology is only as useful as the conversation it enables.
Matching the device to what you actually need to know
The right tracker depends on what question you are trying to answer. A woman at 42 whose cycles just started getting irregular has different needs from a woman at 51 who has not had a period in eight months. Here is how the current options map to different hormonal stages and goals.
If you want to know your actual hormone levels: The Mira Ultra4 is the most data-rich consumer option. It gives you quantitative readings of four hormones, which is useful for women in early perimenopause who want to understand whether they are still ovulating and what their FSH levels look like over time. The $249 starter kit plus ongoing wand costs (~$99 per pack) make it the most expensive option per data point, but it is also the only one producing lab-comparable numbers at home. Mira recommends testing for five consecutive days across two cycles to build a perimenopause baseline. The other quantitative monitors — Proov, Inito, and Oova — use similar chemistry with different app ecosystems and price points.
If you want to track perimenopause symptoms: Peri is purpose-built for this. Its multi-sensor approach — combining accelerometry, EDA, PPG, and temperature — is specifically designed to detect and log hot flashes, night sweats, sleep disturbances, and anxiety patterns. At $449 with no subscription, it is a significant investment, but it eliminates the unreliability of self-reported symptom logging. The trade-off is the adhesive form factor, which some women may find uncomfortable for continuous wear.
If you want metabolic insights alongside hormonal changes: Abbott Lingo tracks glucose continuously for up to 14 days per sensor, starting at $49 for a two-week trial. For perimenopausal women, glucose data can reveal how hormonal shifts are affecting insulin sensitivity and energy levels — connections that blood work done twice a year would miss entirely.
If you want general cycle and wellness tracking: Garmin smartwatches offer what Tom's Guide calls the most detailed women's health tracking available in a mainstream wearable, including menopause and perimenopause symptom logging. Through the MetLuma partnership, Garmin's HRV, sleep, and Body Battery data feeds into a clinical menopause management platform — a model where wearable data informs actual medical care. Dr. Nicole Avard, MetLuma's medical director, noted that patients reported being able to "join the dots between symptoms, how they're feeling, and real-time data from their wearables."
The Oura Ring takes a research-first approach: its collaboration with Clue and UC Berkeley uses ring-collected biometric data (skin temperature, HRV, heart rate, sleep stages) combined with self-reported symptoms to study perimenopause patterns at scale. Apple Watch offers temperature-based ovulation detection, but Tom's Guide notes that this data is retrospective rather than predictive — it tells you ovulation already happened, not that it is about to.
| Device | Best for | Cost | Data type | Perimenopause-specific? |
|---|---|---|---|---|
| Mira Ultra4 | Quantitative hormone levels | $249 + ~$99 wands | Direct (urine hormones) | Yes — validated in perimenopause |
| Peri | Symptom detection and logging | $449 | Proxy (multi-sensor) | Yes — built specifically for it |
| Abbott Lingo | Metabolic and glucose patterns | $49–$249 | Direct (continuous glucose) | Indirect — relevant to hormonal metabolic shifts |
| Garmin + MetLuma | Clinical menopause management | $250–$800 (watch) + MetLuma | Proxy (HRV, sleep, temp) | Yes — through MetLuma platform |
| Oura Ring | Research-backed cycle tracking | ~$299+ | Proxy (temp, HRV, sleep) | Partially — research ongoing |
| Apple Watch | General cycle awareness | ~$399+ | Proxy (temperature) | Limited — retrospective only |
No single device covers everything. The women getting the most useful data are often combining approaches — using a wrist or ring wearable for continuous passive monitoring alongside periodic urine hormone tests to anchor the pattern data with actual numbers. That combination gives you both the "what" (hormone levels) and the "how" (how those levels manifest as symptoms, sleep changes, and metabolic shifts in daily life).
Frequently Asked Questions
Can a wearable actually detect perimenopause?
Wearable devices can detect patterns associated with perimenopause — irregular temperature rhythms, changes in HRV, disrupted sleep architecture — but they cannot diagnose it. A 2024 study of 120 women using Oura Ring data showed that wearable skin temperature tracking reliably distinguishes ovulatory from anovulatory cycles, which is one marker of perimenopausal transition. For a formal assessment, you still need a conversation with a healthcare provider, ideally armed with several months of tracking data.
How accurate are at-home hormone tests during perimenopause?
The best validation data comes from a University of Calgary study comparing the Mira monitor against the ClearBlue Fertility Monitor in perimenopause cycles, which found LH surge detection correlated at R = 0.83 (p < 0.001). That is strong but lower than the R = 0.98 seen in regular cycles, reflecting the natural hormonal volatility of perimenopause. These devices produce clinically useful trend data, but they are not a substitute for serum blood tests when a diagnosis is needed.
Do I need a hormone tracker or a symptom tracker?
It depends on your stage and goals. If you are in early perimenopause and want to understand whether you are still ovulating regularly, a direct hormone monitor like Mira provides the most specific data. If you are further along and dealing with hot flashes, sleep disruption, and mood changes, a symptom tracker like Peri or a general wearable with HRV and temperature tracking may be more useful for day-to-day management and conversations with your doctor.
Are these devices covered by insurance?
Most consumer hormone trackers and health wearables are classified as wellness devices, not medical devices, which means they are typically not covered by insurance. The Mira Ultra4 is FDA-listed as a Class I device, and Abbott Lingo is FDA-cleared, but neither classification currently triggers insurance reimbursement for most plans. Some HSA and FSA accounts may cover these purchases — check with your specific plan.
What should I bring to my doctor from my tracking data?
Researchers recommend bringing at least two to three months of data showing hormone level trends, cycle length variability, and symptom patterns. The Northumbria University study found that women who arrived at appointments with app-generated data visualizations were more successful at having their menopause symptoms taken seriously by healthcare providers. Focus on trends and patterns rather than individual data points.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.