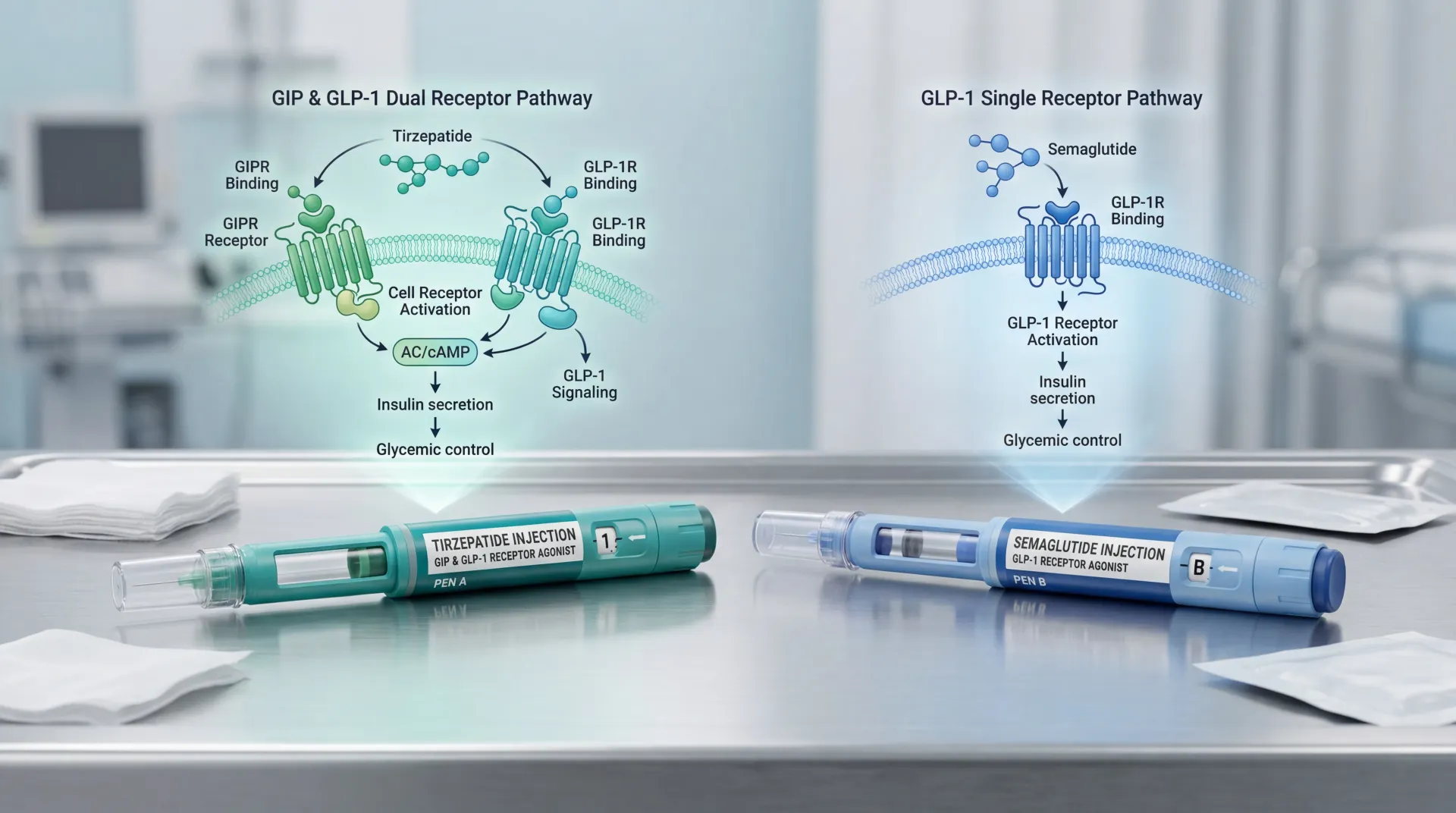
Roughly 12 percent of American adults have now used an incretin-based medication for weight loss, and that number continues climbing. Semaglutide, tirzepatide, and other GLP-1 receptor agonists deliver weight reductions that were once achievable only through surgery. But the speed and magnitude of that fat loss has revealed a complication that clinical trials were not designed to prevent: significant losses of lean body mass, including skeletal muscle.
If you are taking one of these medications, this tension between losing fat and keeping muscle is not a minor footnote. Muscle is metabolically active tissue that governs your resting energy expenditure, regulates blood sugar, protects your joints from injury, and determines how well you function in daily life. Losing too much of it can slow your metabolism, make weight regain more likely after stopping the drug, and accelerate the frailty process by decades. But a growing body of research now shows that specific lifestyle strategies can tip the scales back toward fat loss while holding onto, or even adding, lean tissue.
Up to 40 Percent of the Weight You Lose Could Be Muscle
The clinical trial numbers are hard to ignore. In the STEP-1 trial for semaglutide, participants in the DXA body composition subset lost an average of 6.92 kilograms of lean mass over 68 weeks. That represented roughly 40 percent of the total weight they shed, and approximately 13 percent of their baseline lean mass. Put another way, that single year of treatment compressed about 20 years of normal age-related muscle decline into one concentrated period.
The SURMOUNT-1 trial for tirzepatide told a similar story. Pooled across all dosage groups, about 26 percent of weight loss came from lean soft tissue, with participants losing an average of 5.6 kilograms of lean mass over 72 weeks. A systematic review examining tirzepatide's muscle effects concluded that while relative lean mass proportions were preserved across different age and sex subgroups, the absolute losses were still clinically meaningful.
Key takeaway: Without deliberate intervention, somewhere between a quarter and nearly half of the weight lost on GLP-1 medications can come from lean tissue rather than fat. The clinical trials enrolled participants who were not given structured exercise or nutrition programs, meaning those numbers represent the outcome when medication alone drives weight loss.
| Clinical Trial | Drug | Duration | Mean Weight Loss | Lean Mass as % of Weight Lost |
|---|---|---|---|---|
| STEP-1 | Semaglutide 2.4 mg | 68 weeks | -17.3 kg (~15%) | ~40% |
| SURMOUNT-1 | Tirzepatide (pooled) | 72 weeks | -20.9 kg (~21%) | ~26% |
| SEMALEAN | Semaglutide 2.4 mg | 52 weeks | -13% | Lean mass stabilized after month 7 |
The Mechanism Is Not the Drug Itself
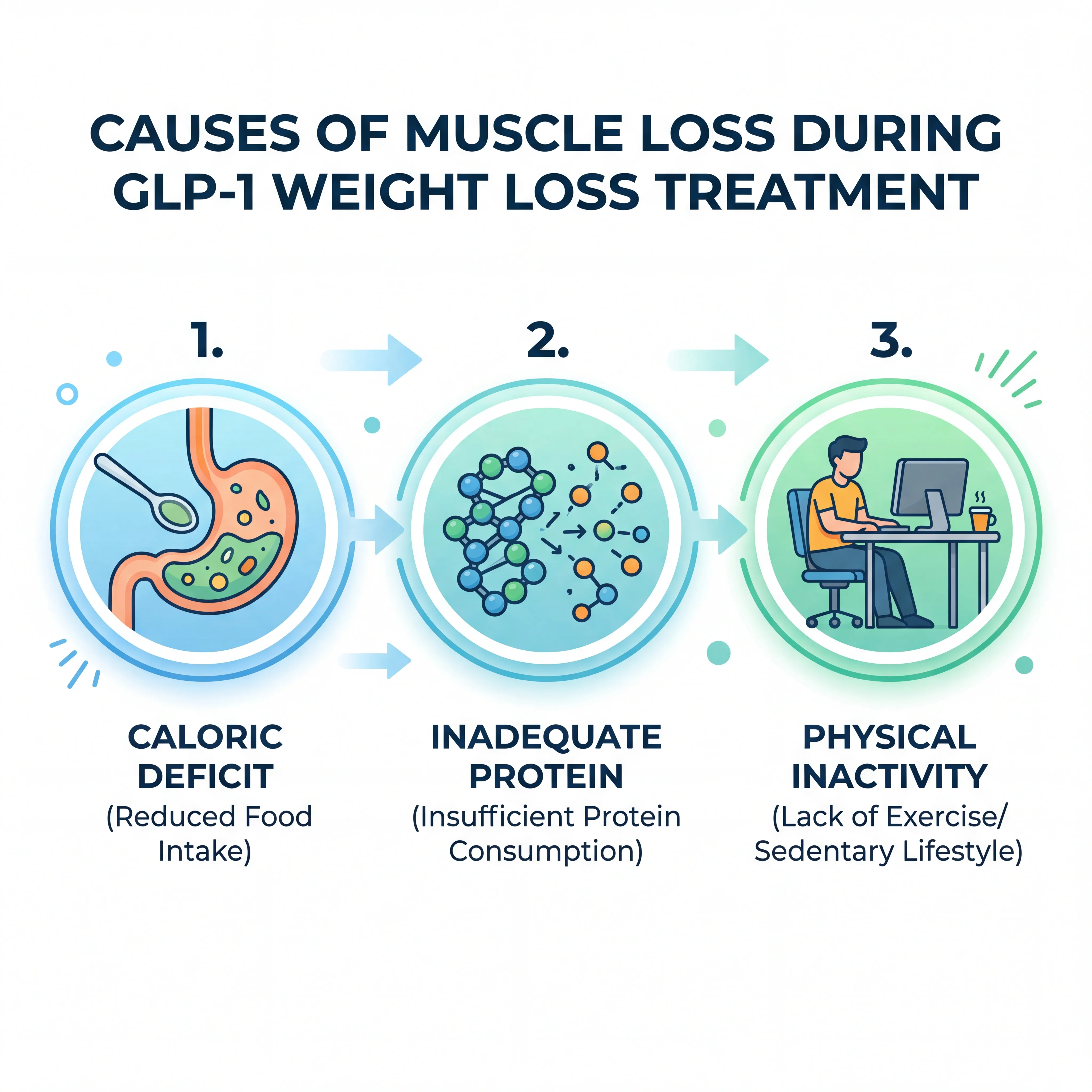
A common misconception is that semaglutide or tirzepatide directly attack muscle tissue. They do not. As obesity medicine specialist Dr. W. Scott Butsch of the Cleveland Clinic explains, muscle loss on these medications is driven by the weight loss process itself, not the pharmacology of the drug. When your body faces a substantial and sustained caloric deficit, it does not exclusively tap fat reserves for energy. It also breaks down protein from muscle, organs, and other lean tissues to meet its metabolic needs.
Several compounding factors make this worse during GLP-1 therapy. The appetite suppression these medications produce can be profound, sometimes reducing daily caloric intake by 30 percent or more. Many people living with obesity already have inadequate protein and micronutrient intake before starting treatment, and the reduced appetite, food aversions, and nausea that accompany dose escalation can deepen those deficits. When protein intake drops below what the body needs to maintain muscle protein synthesis, lean tissue breakdown accelerates.
There is also the issue of disuse. Muscle responds to a straightforward biological rule: use it or lose it. If you are eating less, feeling fatigued, and not deliberately loading your muscles against resistance, your body interprets the reduced demand as a signal that maintaining all that metabolically expensive tissue is no longer necessary. It starts cannibalizing what it perceives as surplus.
The Single Most Important Thing You Can Do in a Gym
If you take away one actionable lesson from this entire guide, let it be this: resistance training is the single most effective countermeasure against muscle loss during GLP-1 therapy. This is not a theoretical suggestion. A compelling case series published in 2025 tracked three patients who combined semaglutide or tirzepatide with structured resistance training and intentional protein intake. Their body composition outcomes looked nothing like the clinical trial averages.
One woman lost 33 percent of her body weight on tirzepatide over 115 weeks while training three to five days per week. A full 91 percent of her weight loss came from fat, with only 6.9 percent from lean tissue. A second patient, who trained five days per week and consumed 1.2 to 1.7 grams of protein per kilogram of body weight daily, actually gained lean soft tissue while losing 26.8 percent of her body weight. Her fat mass dropped by 61.6 percent, while lean mass increased by 2.5 percent. A third patient similarly gained 5.8 percent lean mass while losing 13.2 percent body weight.
Compare these outcomes to the STEP-1 trial participants who had no structured exercise program: 40 percent of their weight loss was lean tissue. The difference is not subtle. It is the difference between emerging from treatment with a stronger, more functional body and emerging with a depleted one that is primed for weight regain.
| Strategy | Frequency | Key Details |
|---|---|---|
| Compound lifts (squats, deadlifts, rows, presses) | 3-5 days per week | Target all major muscle groups; progressive overload |
| Session duration | 30-45 minutes per session | Quality and intensity matter more than duration |
| Intensity | Moderate to high (RPE 7-8/10) | Muscles must be challenged to trigger adaptation |
| Aerobic complement | 150-300 min/week moderate intensity | Zone 2 cardio supports fat loss without undermining muscle |
The Physical Activity Guidelines for Americans recommend muscle-strengthening activities targeting all major muscle groups, including legs, hips, back, abdomen, chest, shoulders, and arms, on at least two days per week. For someone on a GLP-1 medication facing accelerated lean tissue loss, three to five sessions is a more appropriate starting target. If you are new to resistance training, working with a qualified trainer to establish proper form is a worthwhile investment that reduces injury risk during a period when your body is already under metabolic stress.
Getting Enough Protein When Your Appetite Has Disappeared
Resistance training provides the stimulus for muscle preservation, but protein provides the raw material. Without adequate amino acid availability, the anabolic signal from lifting weights cannot translate into maintained or new muscle tissue. This creates a particular challenge on GLP-1 medications, because the very appetite suppression that drives fat loss also makes eating enough protein difficult.
General population guidelines recommend 0.8 grams of protein per kilogram of body weight daily, but that floor was established for sedentary adults maintaining their weight. For someone actively losing weight on a GLP-1 agonist while resistance training, the evidence supports substantially higher targets. The Joslin Diabetes Center recommends 1.0 to 1.5 grams per kilogram of adjusted body weight for obesity management, while bariatric surgery guidelines suggest at least 60 grams daily and up to 1.5 grams per kilogram of ideal body weight.
The case series of patients who preserved or gained lean tissue on GLP-1 medications reported typical intakes of 0.7 to 1.7 grams per kilogram of actual body weight, or 1.6 to 2.3 grams per kilogram of fat-free mass. For a 90-kilogram person, the higher end of that range translates to roughly 120 to 150 grams of protein daily.

Practical tip: When appetite is severely reduced during dose escalation, liquid protein sources like whey protein shakes or bone broth can be easier to tolerate than solid food. A high-protein approach also increases satiety and thermogenesis, which can actually support rather than hinder your weight loss goals.
| Population | Protein Target (g/kg/day) | Source |
|---|---|---|
| General population (sedentary) | 0.8 | Institute of Medicine RDA |
| Adults over 65 | 1.2-1.5 | Geriatric nutrition guidelines |
| Weight loss with resistance training | 1.2-1.7 (body weight) | Case series, GLP-1 patients |
| Joslin Diabetes Center (obesity) | 1.0-1.5 (adjusted weight) | Clinical nutrition guidelines |
| Post-bariatric surgery | 60 g minimum; up to 1.5 (ideal weight) | Bariatric surgery guidelines |
Protein Timing and Quality
Beyond total daily intake, distributing protein across multiple meals matters for muscle protein synthesis. Three to four protein-containing meals spread throughout the day maintain a steadier flow of amino acids to muscle tissue than loading everything into one sitting. Protein quality also plays a role. Complete proteins containing all essential amino acids, particularly leucine-rich sources like whey, eggs, poultry, fish, and dairy, have a stronger effect on stimulating muscle protein synthesis than incomplete plant sources. This does not mean plant proteins are useless, but it does mean that someone relying primarily on plant-based sources needs to eat a greater total volume and combine complementary protein sources.
Supplements, Hydration, and the Pace of Weight Loss
Creatine Monohydrate
One of the patients in the landmark case series who preserved lean mass while losing over 33 percent of her body weight supplemented daily with creatine monohydrate. That tracks with what the research shows. Creatine is among the most well-researched sports supplements, with decades of evidence supporting its role in increasing strength, power output, and lean mass, particularly when combined with resistance training. A standard dose of 3 to 5 grams daily is sufficient for most adults.
Micronutrient Adequacy
An analysis of NHANES data cited in the scientific roundtable on GLP-1 muscle loss found that more than 40 percent of American adults already have inadequate micronutrient intake before any caloric restriction. GLP-1 therapy further reduces food volume, potentially deepening deficiencies in magnesium, vitamin D, iron, B vitamins, and other nutrients essential for muscle metabolism and energy production. A high-quality multivitamin or targeted electrolyte supplementation becomes more important during active treatment than at any other time.
Hydration
Dehydration impairs muscle function, accelerates fatigue, and worsens the cramping many people experience on GLP-1 medications. The Academy of Nutrition and Dietetics recommends approximately 100 ounces (3.1 liters) of fluid daily for men and 73 ounces (2.1 liters) for women, though individual needs vary with activity level, climate, and body size.
Dose Titration: The Case for Patience
Slower dose escalation gives your body more time to adapt to the caloric deficit and allows you to establish nutrition and exercise habits before the appetite suppression becomes most intense. This is not just about tolerating side effects. A more gradual weight loss trajectory gives muscle tissue a better chance to adapt rather than being rapidly catabolized. Discuss pacing with your prescribing physician, particularly if you are over 60 or have risk factors for sarcopenia.
Myth Versus Reality: What the Science Actually Shows

| Myth | Reality |
|---|---|
| GLP-1 drugs directly destroy muscle tissue | Muscle loss is driven by the caloric deficit and physical inactivity, not the drug's mechanism. Preclinical evidence suggests GLP-1 receptor activation may actually enhance muscle fiber formation and reduce fatty infiltration. |
| All lean mass lost is skeletal muscle | Lean mass measured by DXA includes organs, water, bone, and connective tissue. Actual skeletal muscle likely accounts for about half of measured lean mass changes. MRI studies from SURPASS-3 show fat-free muscle volume losses were small and within expected ranges. |
| Muscle loss on GLP-1 drugs is worse than other forms of weight loss | A review in Diabetes, Obesity and Metabolism found that lean mass changes with GLP-1 treatments appear adaptive and proportional to the degree of weight loss achieved, similar to caloric restriction or bariatric surgery. |
| You cannot build muscle while losing weight on these drugs | The case series showed two patients actually gained lean tissue while losing 13-27% of body weight, through consistent resistance training and adequate protein intake. |
| Muscle function always declines with lean mass loss | The SEMALEAN study found that handgrip strength improved by 4.5 kg over 12 months on semaglutide, and the prevalence of sarcopenic obesity decreased from 49% to 33%. |
When to Talk to Your Doctor
Not everyone on a GLP-1 medication will experience problematic muscle loss, but certain populations face elevated risk. People over 65, those with type 2 diabetes (which independently accelerates muscle decline), individuals with a history of weight cycling, and anyone who was sedentary before starting treatment should be particularly vigilant.
Watch for these signals that your muscle loss may be outpacing what your body can afford:
- Progressive weakness: Difficulty with tasks that used to be manageable, such as climbing stairs, carrying groceries, or standing from a seated position without using your hands
- Declining grip strength: Trouble opening jars or holding objects that previously posed no challenge
- Rapid weight loss without exercise: Losing more than 1 to 2 percent of body weight per week, especially if you are not resistance training
- Visible muscle wasting: Noticeable thinning in your thighs, arms, or buttocks (sometimes called "Ozempic butt" or "Ozempic face")
- Persistent fatigue: Exhaustion that does not improve with rest and interferes with your ability to exercise
- Frequent falls or balance problems: Especially concerning in older adults
If you notice several of these signs, request body composition testing. DXA scans provide the most accurate assessment of lean mass changes. Your physician can also check simple functional measures like grip strength and the timed chair stand test to objectively track muscle function over time.
Research is also advancing on pharmacological solutions. Several companies are developing drugs designed to prevent muscle atrophy in combination with GLP-1 therapy, with early results from the COURAGE trial showing preservation of muscle mass alongside continued fat loss. These treatments target pathways like myostatin, activin, and other negative regulators of muscle growth, and may eventually become standard companion therapies.
Frequently Asked Questions
Does semaglutide directly cause muscle wasting?
No. Semaglutide does not directly attack or degrade muscle tissue. The muscle loss observed in clinical trials results from the substantial caloric deficit the drug produces, combined with insufficient protein intake and lack of resistance exercise. When patients pair semaglutide with structured strength training and adequate protein, lean mass can be largely preserved or even increased, as demonstrated in published case reports.
How much protein should I eat daily while on a GLP-1 medication?
Most clinical guidelines for people actively losing weight recommend 1.0 to 1.5 grams of protein per kilogram of body weight daily, distributed across three to four meals. If you are also resistance training, aiming toward the higher end of that range is advisable. For context, a 90-kilogram individual would target roughly 90 to 135 grams of protein per day. Working with a registered dietitian can help you find the right target for your specific situation.
Is cardio or resistance training more important for preserving muscle?
Resistance training is far more effective for preserving muscle mass during weight loss than aerobic exercise alone. Cardio supports cardiovascular health and additional calorie expenditure, but it does not provide the mechanical loading stimulus that signals the body to maintain or build muscle. Ideally, combine both: resistance training three to five days per week with 150 to 300 minutes of moderate aerobic activity.
Can I still lose fat effectively if I focus on preserving muscle?
Yes, and the results can actually be better. In the published case series, patients who prioritized resistance training and protein saw 53 to 62 percent of their total weight loss come from fat, compared to lower proportions in the clinical trials. Preserving metabolically active muscle tissue also maintains a higher resting metabolic rate, which supports ongoing fat loss and reduces the likelihood of weight regain.
Should I be worried about bone loss alongside muscle loss?
Bone density can decrease during rapid weight loss from any cause, with research showing a 10 percent body weight reduction is associated with approximately a 2.2 percent decrease in hip bone mineral density. However, resistance training and adequate nutrition, the same strategies that protect muscle, also help preserve bone. Some preclinical research suggests GLP-1 receptor activation may even promote bone-forming osteoblast activity, though more human studies are needed.
Related Articles
- Best Supplements for Muscle Growth -- Evidence-based supplements that support lean mass development alongside your training program.
- Resistance Training for Women Over 40 -- A practical guide to starting or advancing a strength training routine for bone and muscle health.
- High-Protein Diet for Women: How Much You Need -- Detailed breakdown of protein targets for active women pursuing body composition goals.
- Creatine Benefits Beyond the Gym -- How creatine monohydrate supports muscle, brain, and bone health at every age.
- Collagen Supplements for Skin, Joints, and Gut -- Understanding the role of collagen protein in connective tissue support during weight loss.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.