Walk into a wellness clinic in 2026 and ask about peptides for fat loss, and there is a fair chance someone will mention AOD-9604. The pitch is seductive: a tiny piece of human growth hormone, targets fat cells directly, and unlike Ozempic or Wegovy, doesn't kill your appetite. You eat normally. You just lose fat.
What nobody at that clinic will tell you is that the drug's own developer abandoned it as an obesity treatment nearly two decades ago, after a 24-week trial in 536 people came back negative. That single fact reshapes the entire conversation around AOD-9604, and it is almost completely missing from the marketing materials.
Editorial note: AOD-9604 is not FDA-approved for weight loss or any other indication. This article is educational, not medical advice. Discuss any peptide therapy with a licensed clinician who knows your full medical history.
What AOD-9604 actually is
AOD-9604 stands for "Anti-Obesity Drug 9604" — a 16-amino-acid synthetic peptide that mimics a small slice of human growth hormone, specifically residues 177 through 191 at hGH's C-terminus, with a tyrosine added to the front to improve stability. The full hormone has 191 amino acids, so AOD-9604 is about 8% of growth hormone in size. Wikipedia and a 2015 anti-doping paper by Cox and colleagues describe the structure consistently.
The design rationale was straightforward. Growth hormone mobilizes fat, but it also raises IGF-1, drives blood sugar up in some patients, and at high doses causes the tissue overgrowth seen in acromegaly. The hope was that the C-terminal fragment would carry the lipolytic activity without the metabolic mischief. Mark Heffernan and colleagues at Monash University showed in 2001 that, in obese mice, 14 days of injections reduced body weight and adipose mass while pushing β3-adrenergic receptor RNA back toward normal levels. That 2001 Endocrinology study is the foundational mechanistic citation — and a reminder of the gulf between mice and people. The mice were ob/ob obese mice with a defective leptin gene: instructive, but not interchangeable with a sedentary middle-aged human.
The "no hunger" promise
One claim in AOD-9604 marketing happens to be substantially correct. The drug does not work on appetite. Unlike GLP-1 agonists such as semaglutide or tirzepatide, it does not slow gastric emptying, does not act on the brain's satiety circuits, and has no hunger-suppression mechanism in the molecule. Patients on AOD-9604 typically report eating about the same as before.
The pooled human safety data line up with this story. Heike Stier, Evert Vos, and David Kenley reviewed six placebo-controlled trials covering roughly 900 adults and reported that AOD-9604 had no measurable effect on serum IGF-1 and no negative effect on carbohydrate metabolism in oral glucose tolerance tests, per their 2013 report in the Journal of Endocrinology and Metabolism. No anti-AOD antibodies were detected. The safety profile, as the authors put it, was "indistinguishable from placebo." The marketing line — "fat loss without hunger or blood sugar effects" — tracks with the published data.
Here is the inconvenient question. Is "no hunger suppression" a feature or a bug? GLP-1 drugs do not suppress appetite as a side effect. They suppress appetite as the mechanism. When semaglutide produces 14.9% body weight reduction at 68 weeks, it does so largely by reducing how much patients eat. A drug that leaves your appetite alone has to be doing something else compelling at the level of fat metabolism. The trial data tell us how much that "something else" actually amounts to.
The trial record nobody mentions
There were essentially two human obesity trials worth knowing about. The first looked promising. The second was the one that mattered.
The first, completed by Metabolic Pharmaceuticals around 2004, was a 12-week study in 300 obese adults across five Australian sites. As reported in contemporary coverage from News-Medical, the 1 mg dose group lost an average of 2.8 kg, compared with 0.8 kg for placebo. A later peer-reviewed obesity pharmacotherapy review reported the figure as 2.6 kg vs. 0.8 kg. Either way, the net advantage was roughly 1.8 kg — modest but statistically real in a short trial. This is the result cited everywhere, the basis for nearly every "AOD-9604 has been clinically shown to" claim on a peptide vendor's homepage.
What rarely gets mentioned is the OPTIONS Study — the Phase 2b trial that was supposed to confirm the finding. The design was rigorous: 536 obese subjects randomized to placebo or 0.25, 0.5, or 1 mg AOD-9604 once daily, with 24 weeks of treatment plus 8 weeks observation, per BioSpace's 2006 report. Double-blind, placebo-controlled, properly powered. The result, per the PMC review: "Development of this drug was terminated in 2007 as the drug failed to induce significant weight loss in a 24-week trial of 536 subjects." Later studies "failed to demonstrate a sufficient lipolytic effect," and development for obesity was halted, per the Wikipedia summary.
The failed trial was not small — 536 subjects is a respectable Phase 2b cohort. The failure was not at one dose; the OPTIONS Study tested three, and none cleared the bar. And this was the company's own trial. Metabolic Pharmaceuticals had every commercial incentive to find a positive result. They didn't. When a peptide clinic says AOD-9604 is "clinically proven" for weight loss, the trial they are pointing at is the 12-week one — not the 24-week trial designed to confirm it.
Why Metabolic Pharmaceuticals walked away

The story after 2007 follows a familiar pharma pattern. When a Phase 2b trial fails, the company stops funding development and someone reframes the value proposition. For AOD-9604, that meant a quiet pivot from "potential prescription obesity drug" to "novel nutraceutical ingredient." The 2014 paper by Margret Moré and David Kenley in the Journal of Endocrinology and Metabolism — titled, tellingly, Safety and Metabolism of AOD9604, a Novel Nutraceutical Ingredient for Improved Metabolic Health — is the most visible artifact of this repositioning. AOD-9604 does appear safe in animals at doses far above what any human would take (6-month rat oral NOAEL ≥100 mg/kg/day; 9-month monkey NOAEL 50 mg/kg/day). But once a compound is positioned as a nutraceutical rather than a drug, the bar drops sharply. You no longer need to demonstrate efficacy in adequate-and-well-controlled trials.
Outside formal regulatory pathways, AOD-9604 found a home in two adjacent markets: Australian compounding clinics, where it gained notoriety after the 2013 AFL supplements scandal involving Essendon Football Club players, per a 2025 Guardian investigation; and the U.S. compounding and "research peptide" market. A drug retired by its developer for failing a confirmatory trial does not normally reappear a decade later as a frontline weight-loss therapy. When you see AOD-9604 marketed in 2026, you are looking at the second life of a discontinued asset, not a cutting-edge breakthrough.
The osteoarthritis pivot
While the obesity narrative was dying, a different research thread quietly opened up. In 2015, Dong Rak Kwon and Gi Young Park published a study in the Annals of Clinical and Laboratory Science testing intra-articular AOD-9604 in a rabbit model of knee osteoarthritis. Thirty-two New Zealand white rabbits had cartilage damage induced by collagenase, then were randomized into four groups: saline control, hyaluronic acid alone, AOD-9604 alone, and AOD-9604 plus hyaluronic acid. The combination group recovered from lameness in 11±4 days vs. 25±2 days for saline controls (p<0.05), and histopathological scores of cartilage integrity were significantly better in the combination group than in either monotherapy group.
It is one rabbit study. The dose used (0.25 mg per injection into a single joint) is wildly different from systemic dosing for fat loss, and the comparison group received saline rather than current standard-of-care therapies. None of that makes the result wrong; it just means it is preliminary. A more recent 2026 review of therapeutic peptides in orthopaedics by Rahman, Lee, and Seeds places AOD-9604 in context: described as used "in some regenerative protocols for osteoarthritis, often in combination with HA or platelet-rich plasma," but with "limited RCTs" in human musculoskeletal applications. If AOD-9604 turns out to have a real clinical role, this — not weight loss — is the likeliest place.
The compounded peptide market
AOD-9604 in the United States is dispensed through three overlapping channels: 503A compounding pharmacies, telehealth wellness clinics that work with those pharmacies, and an online "research peptide" grey market shipping vials labeled "for research purposes only." All three operate in regulatory territory that is uncertain and shifting fast.
The FDA's current position is unambiguous. On its page on bulk drug substances for compounding, AOD-9604 appears under "Bulk drug substances nominated but withdrawn." The agency's exact language: "Compounded drugs containing AOD-9604 may pose significant risk for immunogenicity for certain routes of administration ... FDA has identified no, or only limited, safety-related information. Therefore, the agency lacks sufficient information to know whether the drug would cause harm when administered to humans. FDA has also identified serious adverse events that may be associated with AOD-9604, though causality is not clear." Compounding it for human use is, per analysis from healthcare regulatory attorneys at DJ Holt Law, "strictly prohibited."
The political picture in early 2026 is more complicated. As PBS NewsHour reported, the FDA's Pharmacy Compounding Advisory Committee is scheduled for a July 2026 meeting to reconsider compounding access for several peptides, with HHS leadership publicly advocating looser restrictions. Dr. Peter Lurie, a former FDA official, called the trajectory "the Wild West about to become wilder." Dr. Eric Topol of Scripps Research told PBS the situation amounts to "a disaster in the works," noting that "these peptides have no data to support their safety and efficacy." FDA has separately warned about unapproved fat-dissolving injections causing permanent scarring, infections, and skin necrosis. The only FDA-approved fat-dissolving injectable is Kybella, and it is approved only for under-chin fat.
Side effects and unknowns
The trial data are reassuring within their narrow scope. Stier and colleagues' 2013 pooled safety analysis across roughly 900 adults found no withdrawals or serious adverse events tied to AOD-9604 across six placebo-controlled trials. The most common AEs were mild headaches and GI symptoms, indistinguishable from placebo. No IGF-1 elevation, no impaired glucose tolerance, no detectable anti-AOD antibodies. That last point matters: a peptide drug that triggers antibody formation can lose effectiveness, cause hypersensitivity reactions, or both.
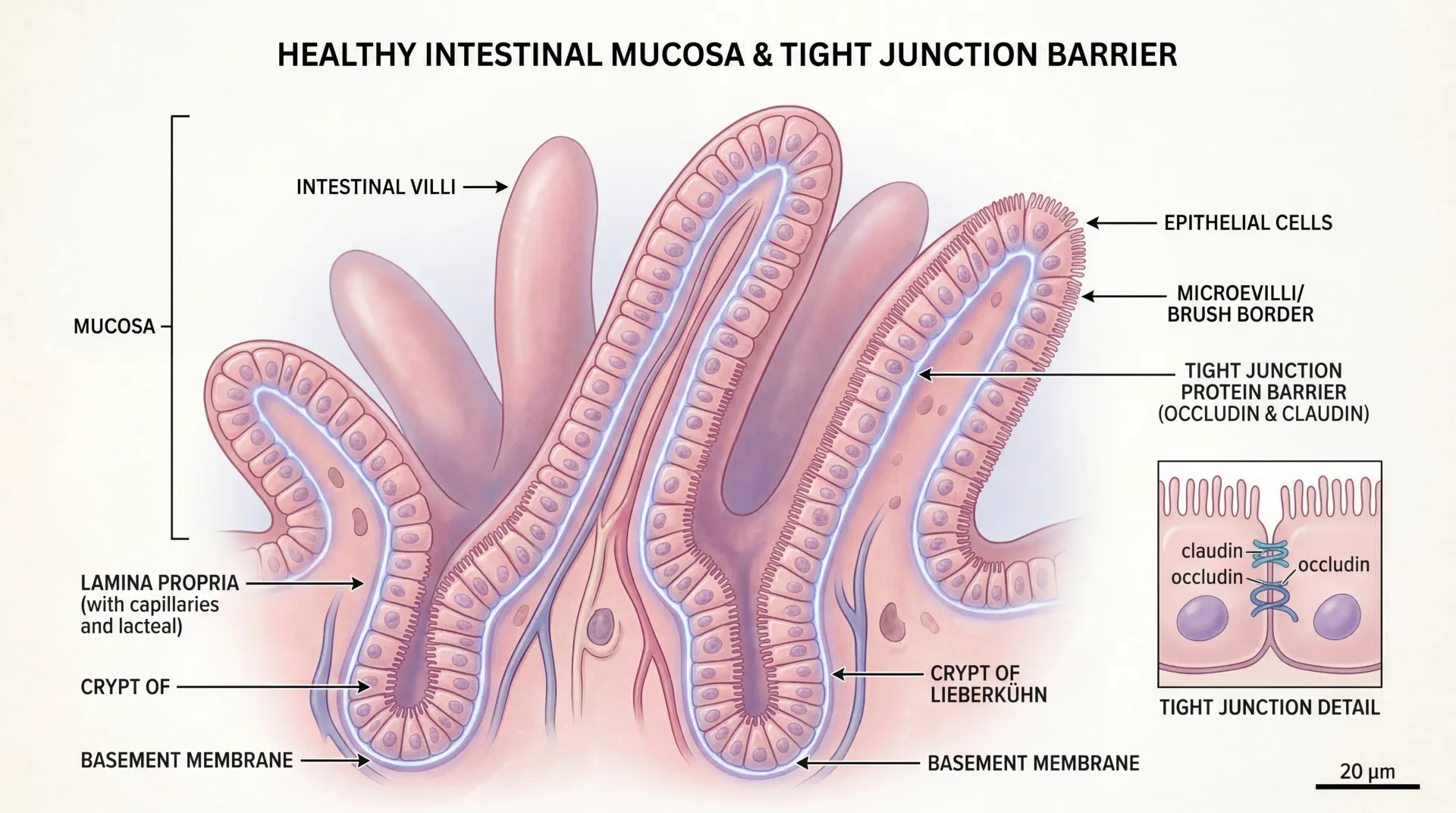
The regulatory caution exists because the trial data don't tell us everything. Most of those 900 trial subjects took AOD-9604 orally, not by subcutaneous injection. The popular compounded version is injected, which raises immunogenicity concerns the oral data cannot rule out — peptides delivered subcutaneously interact with the immune system differently than those broken down in the gut. AARP reported in early 2026 on a Las Vegas incident in which two women were hospitalized with swollen tongues, breathing difficulties, and elevated heart rates after receiving peptide injections; the specific peptide was not identified, but the incident illustrates how poorly characterized this market's adverse-event landscape really is.
Dr. Ian Musgrave, a molecular pharmacologist at the University of Adelaide, told the Guardian: "Every time you inject yourself with a substance, there is a potential for harm. If you're injecting peptides then you have a risk of having an immune response to those peptides … which may be dangerous." The other unknown is long-term safety. Pooled human data cover trials of up to 24 weeks; real-world use can stretch on for months or years. In trial conditions AOD-9604 appears unusually well-tolerated. Outside trial conditions, with manufacturing chains that include overseas vendors and routes of administration the trials never tested, the risk profile is harder to characterize.
AOD-9604 vs. GLP-1 agonists
To understand AOD-9604's place in 2026, compare it directly with what is actually working for weight loss. The comparison does not flatter AOD-9604.
AOD-9604's best-case 12-week result was about 2.6 kg vs. 0.8 kg for placebo, per the PMC obesity pharmacotherapy review — roughly 3.3% of body weight for an 80 kg adult. The 24-week confirmatory trial in 536 people produced no statistically significant separation from placebo at all.
Compare with the STEP-1 trial of semaglutide, published by John Wilding and colleagues in The New England Journal of Medicine in 2021, which enrolled 1,961 adults. Mean body weight reduction was 14.9% at 68 weeks for semaglutide 2.4 mg weekly versus 2.4% for placebo — in absolute terms, 15.3 kg vs. 2.6 kg. SURMOUNT-1, the tirzepatide trial published by Ania Jastreboff and Louis Aronne in NEJM in 2022, enrolled 2,539 adults; at 72 weeks, the 15 mg dose group lost 20.9% of body weight versus 3.1% for placebo. Tirzepatide at 5 mg weekly produced 15.0% weight loss — five times the magnitude of AOD-9604's best result, in a trial seven times as large.
The order-of-magnitude difference is what matters. AOD-9604 at its absolute best produced roughly the same weight loss as the placebo arm of SURMOUNT-1. The counter-argument from advocates usually goes: "GLP-1s come with nausea, GI side effects, and muscle loss; AOD-9604 is gentler." Partly true. They also cause real, measured weight loss at a magnitude AOD-9604 never demonstrated in a properly powered confirmatory trial. A drug with no efficacy is, by definition, gentler than a drug with efficacy. That isn't a value proposition; it's tautology.
Questions to ask before someone injects you
If a clinic is recommending AOD-9604, the following questions reliably distinguish a defensible clinical recommendation from a sales pitch:
- Where is the AOD-9604 sourced from, and what's the certificate of analysis? Compounding pharmacies should provide third-party purity testing for each batch.
- What's the indication, and what's the comparator? If the answer is weight loss, ask why AOD-9604 over an FDA-approved obesity medication. "I cannot tolerate GLP-1s" is a defensible answer. "It's gentler" is not.
- What's the protocol if I have an immune response or injection-site reaction? Any clinician dispensing an injectable peptide should have a clear adverse-event protocol — not just "stop using it."
- How are you monitoring me? Reasonable monitoring includes baseline and follow-up metabolic panel, IGF-1, fasting glucose, and inflammatory markers.
- What does this cost vs. FDA-approved alternatives? A 12-week course of compounded AOD-9604 can run $400-$1,200. Brand-name Wegovy and Zepbound are increasingly covered by insurance for qualifying patients.
Peptide-marketing clinics tend to answer one or two of these well and deflect on the rest. A clinician who treats all five as fair questions is the one worth working with.
Frequently Asked Questions
Is AOD-9604 FDA-approved?
No. AOD-9604 is not FDA-approved for weight loss, osteoarthritis, or any other indication. It appears on FDA's list of bulk drug substances nominated but withdrawn from compounding eligibility, with the agency citing immunogenicity risk and limited safety data. The only FDA-approved fat-dissolving injection is Kybella (deoxycholic acid), approved only for under-chin fat.
Did AOD-9604 ever pass a Phase 2b trial for obesity?
No. The OPTIONS Study — a 24-week, 536-subject Phase 2b trial run by Metabolic Pharmaceuticals — failed to show statistically significant weight loss at the prespecified endpoint. The company terminated obesity development in 2007. The often-cited "2.6 kg vs. 0.8 kg placebo" figure comes from the earlier 12-week trial that did not survive replication.
Why doesn't AOD-9604 cause hunger like GLP-1 drugs?
AOD-9604 acts on fat-cell metabolism through β3-adrenergic pathways and lipolysis, not on appetite circuits. GLP-1 drugs slow gastric emptying and suppress appetite signaling in the hypothalamus, which is why they cause nausea and reduced food intake. AOD-9604 does neither.
Does AOD-9604 work for joint pain?
The strongest evidence is preclinical: Kwon and Park's 2015 rabbit study found that intra-articular AOD-9604 combined with hyaluronic acid produced faster recovery and better cartilage histology than saline or HA alone. Subsequent orthopaedic peptide reviews describe a plausible role in regenerative protocols, but with limited human RCTs. More defensible than weight loss, but still experimental.
What are the safety risks of compounded AOD-9604?
Trial-condition safety data from ~900 patients looked clean — no serious adverse events, no antibody formation, no metabolic disruption. Real-world risks come from the supply chain: peptides from research-only vendors may have purity issues or variable potency. Injectable use raises immunogenicity concerns the oral trial data cannot fully address. FDA has flagged "serious adverse events that may be associated with AOD-9604, though causality is not clear."
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.