What Athletes Mean by the "Wolverine Stack"
The phrase "Wolverine stack" is not a medical term. It is a recovery-culture nickname for combining BPC-157 with TB-500, usually with the promise of faster repair in muscles, tendons, ligaments, and other soft tissue according to commercial peptide guides. The name borrows from the comic-book character who heals almost instantly, which tells you a lot about the psychology of the trend before you ever get to the biology.
The pitch is simple: BPC-157 is framed as the local repair peptide, while TB-500 is framed as the broader systemic recovery peptide in stack marketing copy. If your shoulder has been angry for months or your hamstring keeps barking every time you sprint, that story lands hard. The stack sounds less like a drug experiment and more like a secret shortcut other athletes already found.
That shortcut story has spread beyond niche forums. The Guardian reported on April 4, 2026 that influencers, athletes, and high-profile figures were discussing experimental peptides for injury repair, and it specifically noted that Joe Rogan had alleged BPC-157 plus TB-500, known as the Wolverine stack, helped with injury recovery.
So the question is not whether athletes are curious. They are. The better question is whether the stack is a training tool, a banned experiment, or a very persuasive story built from rodent data, clinic copy, and fear of losing fitness.

Why the Combo Sounds So Plausible
BPC-157 has enough biology behind it to make the hype feel rational. A 2025 scoping review by Flynn P. McGuire, Riley Martinez, Annika Lenz, Lee Skinner, and Daniel M. Cushman described BPC-157 as a synthetic pentadecapeptide originally isolated from gastric juice, with preclinical evidence touching VEGFR2, nitric oxide signaling through Akt-eNOS, ERK1/2 signaling, endothelial repair, muscle repair, fibroblast activity, angiogenesis, anti-inflammatory effects, and neuromuscular stabilization in musculoskeletal healing research.
That list reads like a repair crew arriving at a damaged building: blood supply, scaffolding, cleanup, and communication all matter. Tendons and ligaments are slow healers partly because they do not have the generous blood supply of muscle. Anything that appears to improve blood-vessel signaling or fibroblast behavior is going to attract athletes who live in the gap between "not injured enough for surgery" and "not healthy enough to train."
TB-500 gets its plausibility from thymosin beta-4 biology. D. Philp, A. L. Goldstein, and H. K. Kleinman's PubMed abstract reported that thymosin beta-4 promoted angiogenesis and wound repair in normal and aged rodents, acting through angiogenesis and cell migration in a 2004 Mechanisms of Ageing and Development paper. Yuka Tokura and colleagues later reported that muscle injury increased local thymosin beta-4 production in mice and promoted myoblast migration in a 2011 Journal of Biochemistry study.
The analogy is a road repair project. BPC-157 is sold as the crew working at the damaged intersection; TB-500 is sold as the traffic coordinator helping repair cells move through the area. That is a tidy story. It is also exactly where careful readers should slow down, because a tidy mechanism is not the same as a proven human recovery outcome.
| Peptide | What marketing says | What stronger evidence supports |
|---|---|---|
| BPC-157 | Local tendon, ligament, muscle, and joint recovery support | Preclinical musculoskeletal signals and very limited human pilot evidence summarized in 2025 |
| TB-500 | Systemic recovery and tissue-regeneration support | Thymosin beta-4 cell-migration, angiogenesis, wound, and mouse muscle-regeneration biology reported in 2004 and reported in 2011 |
What BPC-157 Evidence Actually Shows
The strongest BPC-157 recovery claims usually trace back to animal work. In a 2003 Journal of Orthopaedic Research study, M. Staresinic and colleagues used BPC-157 after transecting rat Achilles tendons, with daily intraperitoneal doses of 10 microg, 10 ng, or 10 pg per kg in the rat tendon model. The treated rats showed better load of failure, load of failure per area, Young's modulus, Achilles functional index values, fibroblast formation, reticulin, collagen, and tendon-defect closure in that same PubMed abstract.
That is not nothing. If you are a sports-medicine researcher, it is interesting. If you are a lifter with a cranky patellar tendon, it is tempting. The problem is the translation jump. A rat Achilles tendon study is a clue, not a treatment protocol for a human ACL sprain, rotator cuff tear, or hamstring strain.
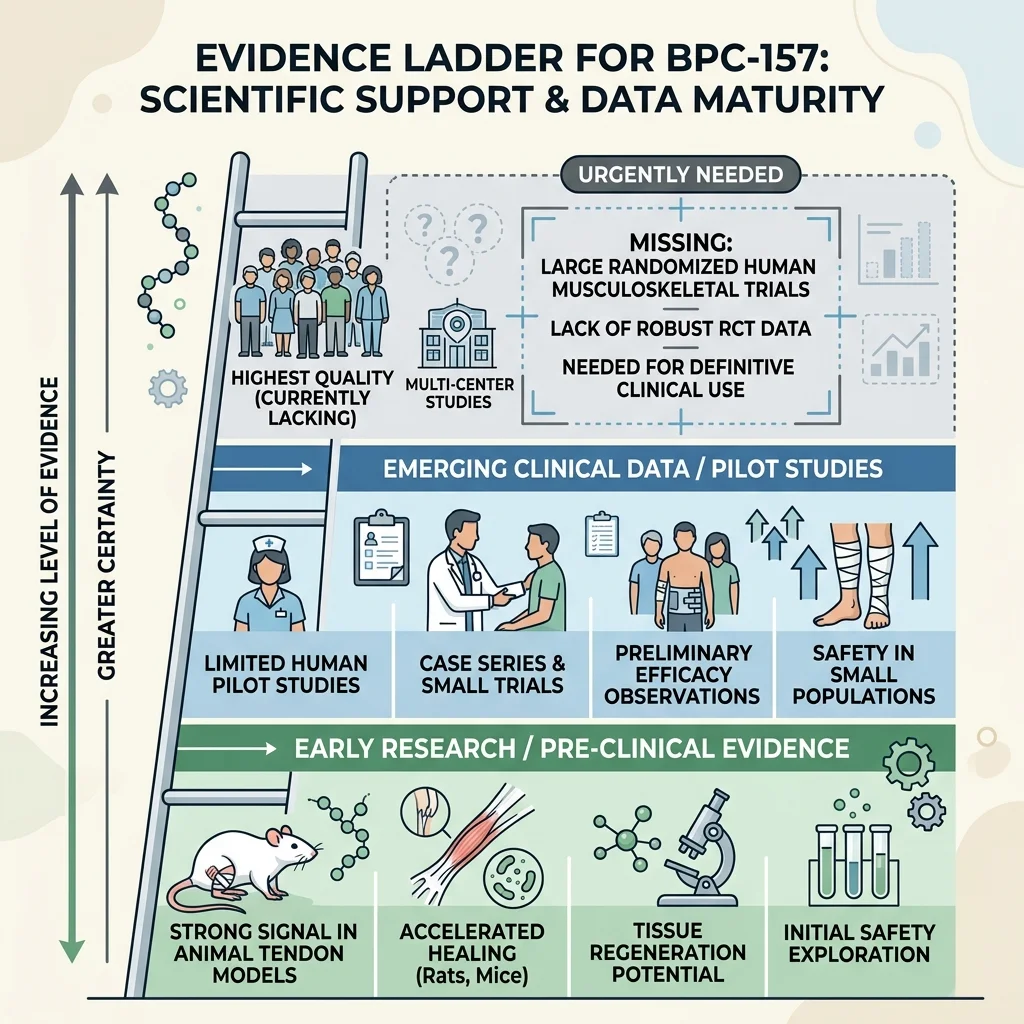
The 2025 BPC-157 review is the better anchor for readers because it zooms out. McGuire and colleagues found broad preclinical support but only three pilot human studies, including intra-articular knee pain, interstitial cystitis, and intravenous safety/pharmacokinetics in their review. They also stated that rigorous, large-scale human trials are lacking and that BPC-157 should be considered investigational until better clinical trials test safety, efficacy, and clinical utility for musculoskeletal medicine.
Practically, BPC-157 has a signal. It does not have the kind of human evidence that should make an athlete casually inject it because someone in a locker room says it worked.
What TB-500 Evidence Actually Shows
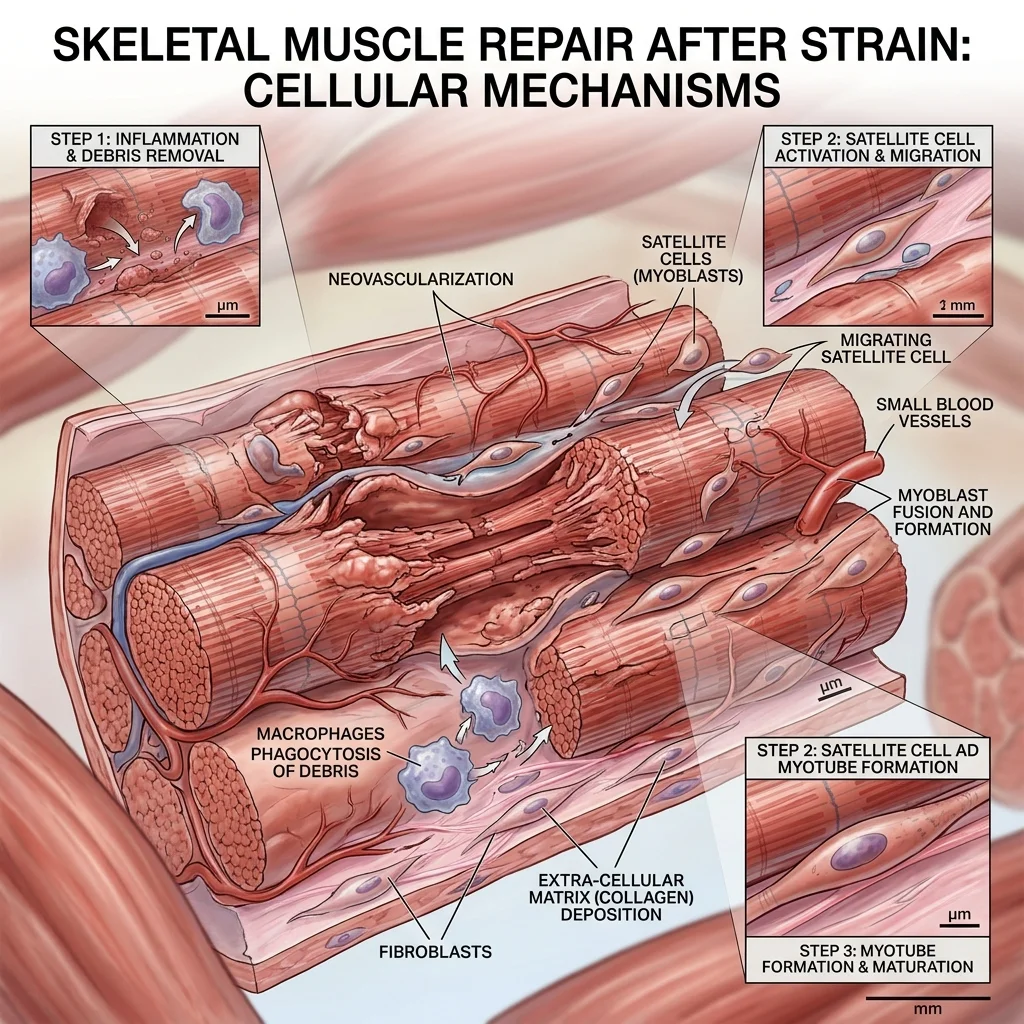
TB-500 is even harder to pin down because much of the human-facing marketing borrows credibility from thymosin beta-4 research. Philp, Goldstein, and Kleinman's 2004 abstract supports the idea that thymosin beta-4 can influence angiogenesis, wound repair, and cell migration in rodents in preclinical wound biology. Tokura and colleagues' 2011 study supports a muscle-regeneration mechanism in mice by showing thymosin beta-4 up-regulation after injury and myoblast chemoattraction in skeletal muscle regeneration research.
Mechanistically, that is the right neighborhood for recovery. Repair cells need to move, new vessels help deliver resources, and damaged muscle needs satellite-cell activity. But you can live in the right neighborhood and still have the wrong address. TB-500 products sold to athletes are not the same thing as a validated human therapy for tendon, ligament, or muscle injuries.
The Guardian summarized the evidence gap bluntly: experts reviewing BPC-157, TB-4, and TB-500 found animal and cell signals, but human data for musculoskeletal conditions were lacking, and there had been no TB-500 studies in human participants in its 2026 peptide explainer. That is the line athletes need to remember. TB-500's story is biologically plausible, not clinically proven for return-to-play decisions.
If BPC-157 is a promising draft of a recovery idea, TB-500 is more like a mechanism sketch. Interesting, maybe useful someday, but not enough to replace diagnosis, load management, imaging when needed, or progressive rehab.
Why Athletes Keep Using It Anyway
The stack survives because injuries create desperation. The Guardian reported that peptide interest began as a niche in the 2010s among powerlifters and bodybuilders before spreading into a broader health, fitness, athlete, and influencer conversation through social media and online vendors. Athletes are especially vulnerable to this pitch because time away from training feels like identity loss, not just inconvenience.
Commercial pages make the timeline sound manageable. One stack guide describes anecdotal expectations of 1-2 weeks for reduced pain and inflammation, 2-4 weeks for improved mobility, and 4-8 weeks for tissue regeneration or functional recovery while still noting limited human trials. The same kind of guide describes anecdotal dosing patterns of 200-500 mcg of BPC-157 daily and 2-5 mg of TB-500 weekly, while also acknowledging that there is no FDA-approved dosing for either peptide for injury recovery.
Those ranges can make the stack feel standardized. It is not. A dosing chart on a clinic blog is not the same thing as a labeled medication with indication, contraindications, pharmacokinetics, manufacturing controls, adverse-event reporting, and trial-defined outcomes.
There is also a social proof problem. A teammate says his elbow calmed down. A podcaster says he recovered faster. A clinic page says the stack supports physical therapy, rest, nutrition, and rehabilitation rather than replacing them in its recovery framing. That sounds moderate enough to lower the reader's guard.
The useful takeaway is not "athletes are foolish." It is that recovery pain makes weak evidence feel stronger than it is. When your next race, fight, meet, or season depends on a tendon behaving, the brain starts shopping for certainty.
That is why the stack's best marketing does not sound reckless. It sounds disciplined. It borrows the language of protocols, cycles, local injections, systemic support, tissue resilience, and return-to-function. For an injured athlete, those words feel like structure. They turn waiting into action.
A safer way to read those pages is to separate the emotional promise from the clinical proof. The emotional promise is control: do something, inject something, stack something, and stop feeling passive. The clinical proof would be boring but decisive: diagnosed injuries, matched comparison groups, defined dosing, measured return-to-play outcomes, adverse-event tracking, and enough follow-up to know whether the short-term win created a long-term cost. The Wolverine stack has far more of the first than the second.
| Claim athletes hear | More careful translation |
|---|---|
| "It speeds tendon healing." | BPC-157 has animal tendon data, including a rat Achilles model published in 2003, but human injury-recovery proof is sparse. |
| "TB-500 moves repair cells." | Thymosin beta-4 biology supports cell migration and muscle-regeneration mechanisms in mice and cells, not a proven athlete protocol. |
| "The stack is common in sport." | Discussion is common; clean clinical evidence and eligibility safety are different questions according to current reporting. |

The Doping and Safety Problem Most Stack Guides Skip
The anti-doping issue comes before the wellness issue for tested athletes. The 2025 WADA Prohibited List became effective on January 1, 2025, and its S0 category prohibits at all times any pharmacological substance with no current approval by a governmental regulatory health authority for human therapeutic use under the World Anti-Doping Code. The Guardian also reported that BPC-157, TB-4, and TB-500 are banned substances in sport on WADA's list in its peptide overview.
USADA's athlete-facing warning is direct: it describes BPC-157 as experimental, not approved for human clinical use, potentially harmful, and risky for athletes on its BPC-157 page. That matters even if an athlete never competes internationally. College programs, pro leagues, federations, and event organizers can have their own enforcement systems, but WADA categories shape the risk conversation.
The FDA picture is also unsettled. FDA's bulk-substance update says BPC-157 was removed from Category 2 because nominations were withdrawn, while FDA announced a July 23, 2026 PCAC consultation for BPC-157 acetate and BPC-157 free base on the 503A bulks list in its compounding update. That is not a green light for athletes. It is a regulatory process about whether certain bulk substances may be considered for compounding, not proof that the stack works for sports injuries.
Safety is not just about the peptide molecule. Prof. Adam Taylor told the Guardian that animal or cell benefits do not necessarily translate to human benefit, and he warned that increasing peptide pathways could throw body systems out of balance, including theoretical concerns around cancer biology in the context of unregulated peptide use. Lynda Scammell of the MHRA also told the Guardian that "research purposes" labels do not avoid scrutiny when products are effectively unauthorized medicines for human use under UK regulatory analysis.
Think of the stack like an unlabeled performance part installed in a race car. It might fit. It might fail. It might disqualify the car before the race even starts. For competitive athletes, the eligibility risk alone is enough to make casual use a bad bet.

How to Think About Recovery Without Buying the Myth
The most honest answer is not that the Wolverine stack is fake. It is that the evidence is uneven. BPC-157 has interesting preclinical musculoskeletal data and a small human evidence base. TB-500 has thymosin beta-4 mechanism signals in wound and muscle biology. Neither has the kind of human sports-injury evidence that should make the stack routine.
For BPC-157, McGuire and colleagues' 2025 review gives the cleanest summary: promising preclinical biology, only three pilot human studies, and a recommendation not to use it clinically for musculoskeletal medicine until well-designed human trials are published in Current Reviews in Musculoskeletal Medicine. For TB-500, the Guardian's review of the evidence gap is just as important: animal and cell signals exist, but human musculoskeletal data are lacking and no TB-500 human participant studies were identified in current reporting.
A practical recovery decision starts with diagnosis. Tendinopathy, a partial tear, a full rupture, joint instability, nerve irritation, and referred pain are different problems. Peptides cannot make a wrong diagnosis right. They also cannot replace progressive loading, enough calories, protein, sleep, mobility work, and the patience to let tissue adapt.
If you are not drug-tested and are still considering the stack, the minimum bar should be higher than "a clinic sells it." Ask what diagnosis is being treated, what outcome is being measured, what product-quality documentation exists, what adverse-event plan is in place, and what evidence would make you stop. If you are drug-tested, the decision is simpler: treat the stack as an eligibility problem before treating it as a recovery experiment given USADA's warning and WADA's prohibited-at-all-times language.
The boring plan is still the stronger plan: get the injury assessed, load the tissue gradually, track pain and function, use imaging when the diagnosis is unclear, and be wary of anything sold as a way to skip the work. The stack's name promises superhero healing. Real recovery usually looks more like a spreadsheet, a coach, and several disciplined weeks.

| Decision point | Conservative interpretation | Best next step |
|---|---|---|
| Untested athlete | Evidence is biologically interesting but not definitive | Discuss risks with a qualified clinician before considering any experimental therapy |
| Drug-tested athlete | Eligibility risk is immediate | Check WADA, USADA, and sport-specific rules before using any peptide |
| Acute or worsening injury | Peptide talk can delay proper diagnosis | Prioritize examination, imaging when indicated, and structured rehab |
Frequently Asked Questions
Is the BPC-157 and TB-500 Wolverine stack proven to heal sports injuries?
No. BPC-157 has preclinical tendon and musculoskeletal signals, including the 2003 rat Achilles tendon study and a 2025 review noting only three pilot human studies in animal tendon research and in the BPC-157 review. TB-500 has thymosin beta-4 mechanism evidence, but current reporting notes no TB-500 human participant studies for musculoskeletal conditions in reviewed evidence.
Why do athletes say they recover faster on it?
The stack has a persuasive mechanism story, commercial pages describe anecdotal recovery timelines, and injury frustration makes shortcuts attractive in stack marketing. But anecdote cannot separate true drug effect from natural healing, rehab, rest, placebo response, or a less severe injury than first feared.
Is the stack allowed in tested sport?
A tested athlete should assume serious risk. WADA's S0 category prohibits at all times substances without current approval by a governmental regulatory health authority for human therapeutic use, and current reporting identifies BPC-157, TB-4, and TB-500 as banned sport substances under the WADA list and in the Guardian's explainer.
What is the biggest safety concern?
The biggest concern is uncertainty: limited human evidence, unclear product quality, injection risk, and possible pathway effects that have not been monitored in long-term human studies. Prof. Adam Taylor specifically warned that increasing peptide pathways could disturb body systems and raise theoretical concerns around cancer biology in the Guardian's reporting.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.












