The "I tried it for 90 days" headline is its own genre — one person, one scale, one triumphant photo. That frame hides almost everything that matters. Instead of one anecdote, this guide assembles what randomized trials, real-world cohorts, and dermatology and endocrinology reviews actually show happens in the first 90 days on semaglutide — the brand versions sold as Wegovy and Ozempic, plus the compounded versions still moving through specialty pharmacies in early 2026. The results are more interesting than the marketing, and a lot less tidy.
This article is not medical advice. Semaglutide is a prescription drug with serious warnings, and peptide regulation has shifted considerably after the FDA declared the shortage resolved in February 2025. Talk to a clinician before starting, stopping, or switching any GLP-1 therapy.
What 90 days of semaglutide actually changes
Day 90 is a strange place in a semaglutide protocol. According to the Mayo Clinic dosing summary for Wegovy, the standard escalation is 0.25 milligrams once weekly for four weeks, then a dose bump every four weeks through 0.5, 1.0, and 1.7 milligrams, with patients hitting the 2.4-milligram maintenance dose around week 17. At day 90, most people are still climbing — typically on 1.0 to 1.7 milligrams, not the headline-making full dose.
The big-banner number — a mean 14.9 percent body weight reduction — comes from the STEP-1 trial in the New England Journal of Medicine, which followed 1,961 adults with overweight or obesity on 2.4 milligrams versus placebo for 68 weeks. That figure is week 68, not week 12. Clinic syntheses from AFC Urgent Care and a primary-care 90-day overview both put the realistic 12-week range at 5 to 10 percent of starting body weight — about 10 to 20 pounds for a 200-pound starting point.
Cardiometabolic markers move faster than the scale suggests. The STEP-4 trial in JAMA documented a mean 9.7-centimeter waist reduction, a 3.9-mm Hg drop in systolic blood pressure, and a 2.5-point gain on the SF-36 physical functioning score by week 68, with a meaningful share appearing in the first three months. At 90 days, the change in the mirror lags the change in your blood pressure cuff.
The week-by-week timeline most people experience
The first month is mostly biological negotiation. On the starter 0.25-milligram dose, patients tend to notice subtle appetite suppression rather than scale movement, which maps cleanly to AFC Urgent Care's description of weeks one through four as a body-adjustment window where significant weight change is "not immediately evident." Mild gastrointestinal symptoms — nausea, bloating, constipation, or post-meal fatigue — show up early and often intensify each time the dose climbs. The pattern is dose-step nausea: a rough few days after each titration, then a return to baseline.
By weeks five through eight, weekly loss tends to settle into the one-to-two-pound range. Patients eat noticeably smaller portions without the friction of conscious dieting. By weeks nine through twelve, many are nine to fifteen pounds down, and the appetite shift feels less like willpower and more like an internal volume control. The original NEJM authors framed the side-effect curve in their own words: the gastrointestinal events "were typically transient and mild-to-moderate in severity and subsided with time" — language that acknowledges how common the symptoms are while signaling they usually resolve.
Practically, the first 90 days are not a single experience but a series of three-to-four-week mini-cycles, each opening with a dose bump, a wave of nausea, an appetite drop, and a slow ease back to a new normal. Knowing that pattern is the difference between thinking the medication stopped working and recognizing the body is resetting before the next phase.
The honest before-and-after — what patients commonly notice
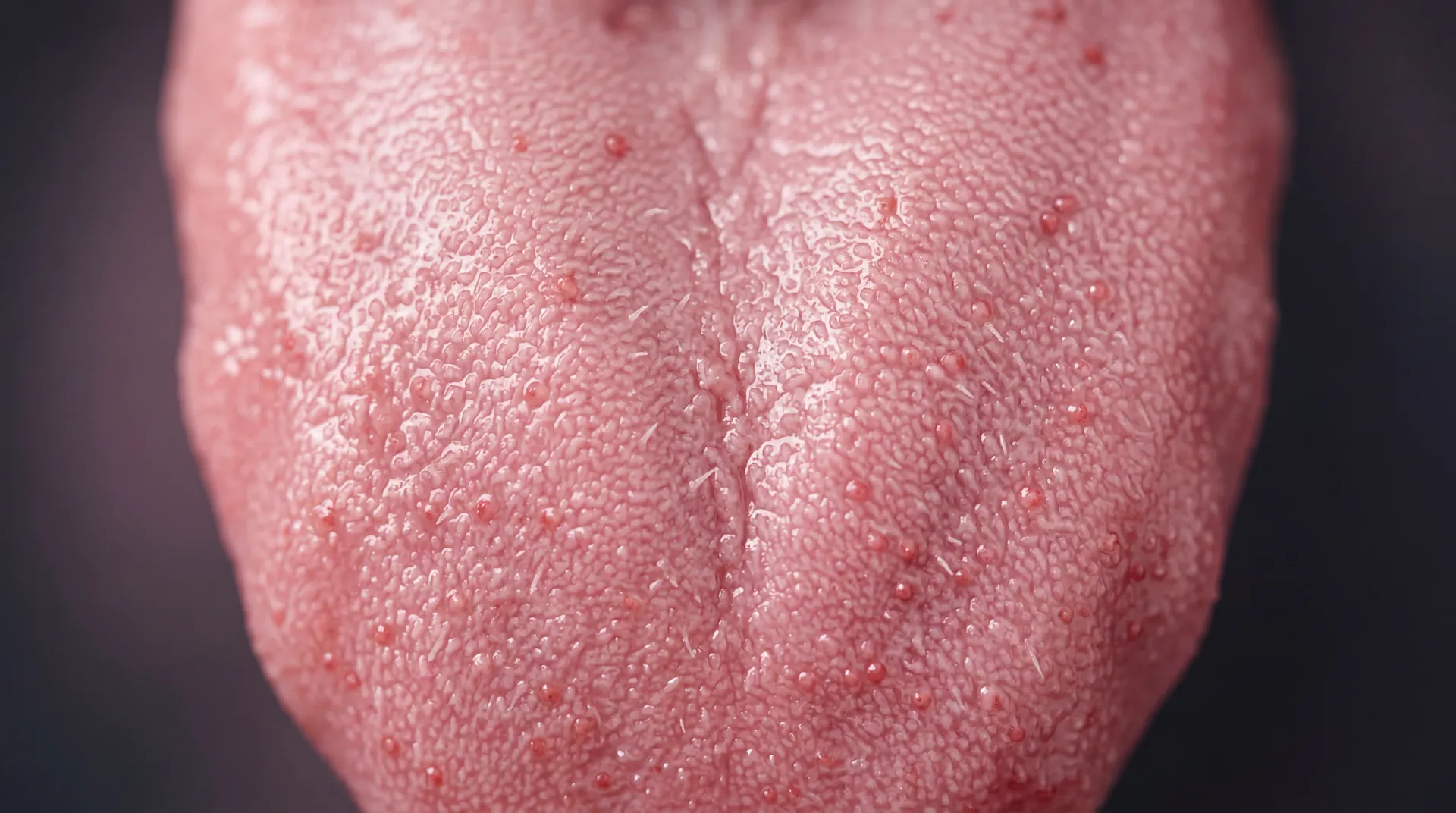
The most consistent subjective change has nothing to do with the scale. Patients describe the disappearance of "food noise" — the persistent, intrusive thoughts about what to eat next. A 2023 conceptual review in Nutrients defined it formally as "heightened and/or persistent manifestations of food cue reactivity, often leading to food-related intrusive thoughts and maladaptive eating behaviors." On semaglutide, patients report that volume drops sharply — sometimes within days.
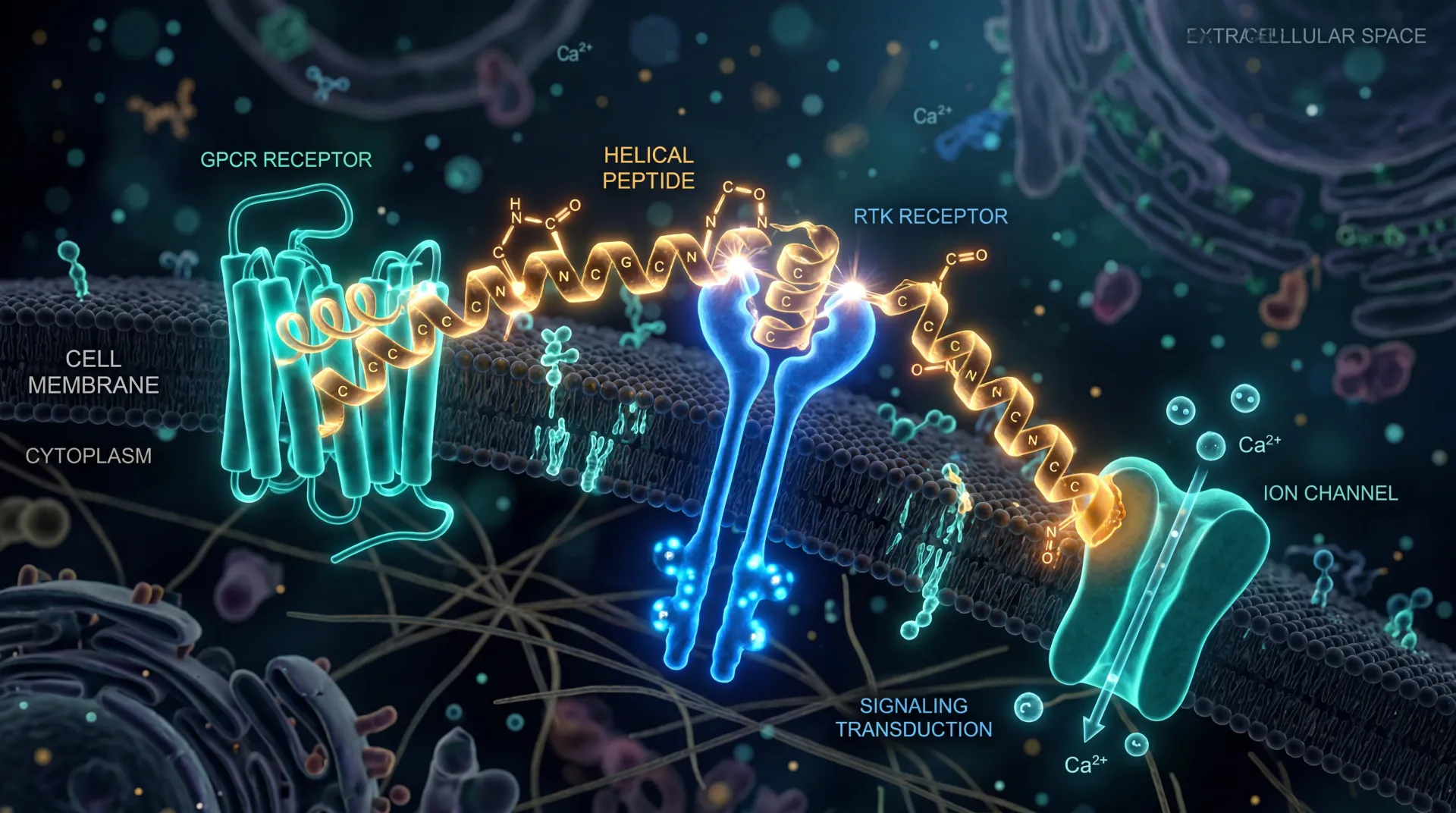
The neuroscience is catching up to the testimony. Scientific American reports that Wegovy patient Kimberly Chauche described "some part of my brain that was always there just went quiet" within 48 hours of her first dose. Researcher Matthew Hayes notes that GLP-1 receptors are present "everywhere, everywhere, throughout the brain," with concentrations in the hypothalamus, nucleus tractus solitarius, and nucleus accumbens — regions that translate gut signals into appetite, satiety, and reward. Lisa Beutler at Northwestern, in the Journal of Clinical Investigation in October 2025, mapped a "double whammy" mechanism: GLP-1 drugs activate brainstem fullness signals while silencing AgRP neurons — the cells that normally drive rebound hunger during weight loss.
Think of it like a thermostat that has been overcorrecting. The body's hunger signals defend a higher set point as calories drop. Semaglutide does not override that thermostat so much as quietly recalibrate it, which is why patients describe feeling "satisfied" rather than "deprived" — a distinction diet alone rarely produces. The same mechanism shows up elsewhere: Scientific American reports that Patricia Grigson's team observed roughly a 40 percent reduction in opioid cravings when GLP-1 agonists were paired with standard addiction treatments. The 90-day implication is that the appetite shift may extend to other reward-driven behaviors — alcohol, late-night snacking, compulsive ordering.
Response is not uniform. Roughly 18 percent of users lose less than 5 percent of their body weight while others approach 20 percent, a spread researchers attribute partly to genetic differences in GLP-1 receptor expression. The practical reality of the 90-day mark is wide. Some people will be down 18 pounds; others 4 and frustrated. Both are within the published distribution.
The side effects nobody puts in the marketing
The headline gastrointestinal numbers are well established. AARP's review of Mayo Clinic data reports nausea in 38 percent of users and diarrhea in 9 percent, with roughly half of patients experiencing some side effect — most mild enough that they continued treatment. STEP-1 itself documented a 4.5 percent discontinuation rate due to GI events, against 0.8 percent on placebo. What the marketing does not lead with is everything else.
Hair shedding is real but smaller than rumor suggests. A real-world analysis in JAAD by Jairath, Abreu, and Mann compared trial and EMR data: 3 percent of patients on the 2.4-milligram dose reported hair loss in registration trials versus 1 percent on placebo, while EMR data from the Barnes Jewish system and the TriNetX research network put telogen effluvium rates at 0.80 and 0.83 percent within six months. The authors concluded semaglutide "does not significantly increase the risk of hair loss" beyond what rapid weight loss itself produces — the same pattern seen after bariatric surgery.
Muscle and lean mass loss is the under-reported story. A Karakasis meta-analysis summarized in industry coverage suggests up to 39 percent of weight lost on semaglutide may come from lean mass. The SEMALEAN body composition study, published in 2025 with 106 completers, gives a more nuanced picture: fat mass dropped 14.3 percent at month 7 and 18.9 percent at month 12, while lean mass fell about 3 kilograms early and stabilized. Handgrip strength rose 4.1 kilograms; sarcopenic obesity prevalence dropped from 49 to 33 percent. Translation: lean mass loss is real but front-loaded and partially functional — provided patients eat enough protein and do some form of resistance work.
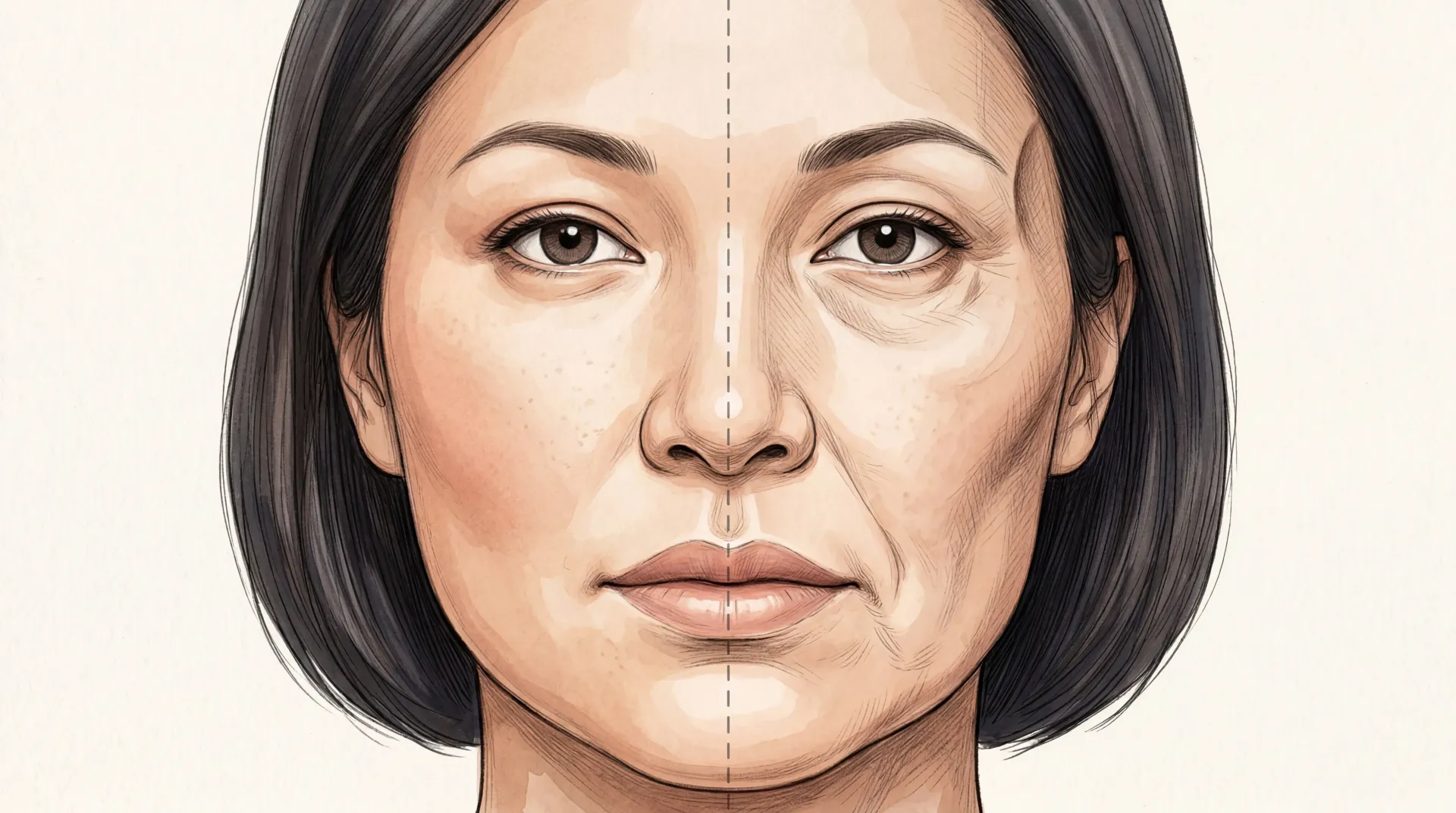
"Ozempic face" is a side effect of fast fat loss, not the drug itself. A systematic review in plastic surgery literature notes that roughly 13 percent of US adults — about 32 million people — have used a GLP-1 receptor agonist, and the facial pattern is consistent: preferential fat loss in temples, cheeks, tear troughs, jawline, and nasolabial folds. Cleveland Clinic endocrinologist Vinni Makin calls it "a very common side effect because people often maximize their dose to try to achieve target weight goals quickly." The fix is mostly slower loss, more protein, and patience — not less drug.
The rare but serious tail. A Cleveland Clinic retrospective review of 161 patients with prior pancreatitis history found a 10 percent recurrence rate on GLP-1 therapy — "likely no greater than what is observed in the general population." A summary of newer studies notes a June 2025 JAMA Ophthalmology paper finding a substantially higher risk of wet age-related macular degeneration among GLP-1 users, and a February 2026 paper in the Journal of Clinical Endocrinology & Metabolism — analyzing more than 46,000 older adults — finding GLP-1 users were 11 percent more likely to experience fragility fractures than peers on other diabetes drugs. Worth knowing: the Wegovy label includes a suicidal-ideation warning that the otherwise-identical Ozempic label does not.
Sulfur burps and other indignities. The infamous egg-smelling reflux some patients describe as their most embarrassing 90-day moment likely traces to the slowed gastric emptying that defines the GLP-1 mechanism. It tends to ease with smaller, lower-fat meals.
Plateaus, dose escalations, and what happens around day 60
Sometime in the second half of the 90-day window — roughly day 55 to 75 — many patients hit what feels like a stall. The scale stops moving; sometimes it ticks up a pound. The cause is usually a combination of a fresh dose escalation pulling water around the body, a temporary plateau in fat loss while lean mass stabilizes, and the variability of a weekly injectable whose blood levels are still climbing toward steady state.
This is where titration discipline pays off. Cleveland Clinic's pancreatitis review recommends clinicians lower the dose if weekly weight loss exceeds 1.5 kilograms — about 3.3 pounds — because rapid loss is the lever that drives gallstone risk, lean mass loss, and the facial changes. A plateau at day 60 is sometimes the body protecting you from a faster pace than your physiology can sustain. The right move is rarely a dose jump; it is usually more protein, more sleep, light resistance training, and a few weeks of patience while the next titration takes hold.

What 90 days does not do
The least-discussed fact about semaglutide: it does not durably solve obesity in a 90-day window — or even a 12-month one — unless you keep taking it. The STEP-1 extension followed participants for a year after stopping. They regained a mean of 11.6 percentage points of body weight, dropping the net loss from 17.3 percent at week 68 to 5.6 percent at week 120 — meaning two-thirds of the loss was reversed.
The withdrawal effect is even sharper in the trial designed to test it. STEP-4 enrolled patients into a 20-week run-in on semaglutide, then randomized them to continue or switch to placebo. In the JAMA paper, 82.4 percent of those switched to placebo gained weight over the next 48 weeks, against 15.2 percent of those who continued. The drug works while it is in your system; that is the whole story.
The pattern generalizes. A 2025 BMJ meta-analysis of 9,341 participants across 37 studies estimated an average regain of about 0.4 kilograms per month after stopping anti-obesity medication, with projected return to baseline at 1.7 years and cardiometabolic markers reverting within 1.4 years. The authors framed obesity as "a chronic disease that usually relapses when treatment is stopped" — medically tidy but financially bracing for anyone budgeting a 90-day course.
Lifestyle still matters in a specific way: people who hold onto more of their loss use the 90-day appetite suppression to actually rebuild eating and movement habits, rather than treating it as a temporary fix. The drug buys runway. It does not pay the rent forever.
Cost and access reality in 2026
Semaglutide pricing in 2026 is in active flux. Novo Nordisk announced in February 2026 that Wegovy's monthly list price will drop from roughly $1,350 to $675 effective January 1, 2027 — a 50 percent cut aimed at insured patients on high-deductible or coinsurance plans. Cash-paying patients can access a direct-to-consumer program ranging from $149 to $499 per month depending on dose. Medicare patients will see a separately negotiated price of $274 per month under the Inflation Reduction Act, also effective 2027.
The compounded-semaglutide channel that absorbed shortage demand from 2022 through 2024 has narrowed sharply. FDA declared the semaglutide shortage resolved on February 21, 2025, ending the emergency exception that allowed widespread compounding. Pharmacies can still produce the molecule for non-standard doses tied to a specific clinical need, but the bulk-compounding model that drove much of the telehealth boom is no longer permitted. Branded products are easier to get than at any point in the past three years — but patients who relied on $200 monthly compounded subscriptions are paying brand prices or sitting out treatment.
For a 90-day course in early 2026, the realistic out-of-pocket math depends entirely on insurance. A high-deductible patient who hasn't met their deductible can still face roughly $4,000 for three months; strong commercial coverage may bring that to $25 per month with manufacturer support; a Medicare patient is in a transitional window waiting for the negotiated price. None of those scenarios make a 90-day "trial" a casual financial decision — which makes the regain data above all the more uncomfortable.
Frequently Asked Questions
Is semaglutide safe to use without medical supervision?
No. Mayo Clinic lists contraindications including a personal or family history of medullary thyroid cancer or MEN type 2, severe gastroparesis, and Type 1 diabetes, alongside warnings for pancreatitis, gallbladder disease, kidney injury, retinopathy progression, and severe allergic reactions. Dose escalation and monitoring all require a clinician. This article is informational, not medical advice — consult your physician before starting or stopping GLP-1 therapy.
How much weight should I realistically expect to lose in 90 days?
Real-world clinic data points to 5 to 10 percent of starting body weight by week 12 — about 10 to 20 pounds for a 200-pound starting point. The 14.9 percent figure from STEP-1 is a 68-week endpoint, not a 12-week one. About 18 percent of patients lose less than 5 percent in trial settings, so falling below the average does not necessarily mean failure.
Will I gain the weight back when I stop?
Most people will. The STEP-1 extension showed participants regained a mean of 11.6 percentage points of body weight in the year after stopping, leaving only about a third of the loss intact. STEP-4 data showed 82.4 percent of patients who switched to placebo at week 20 gained weight afterward. A 2025 BMJ meta-analysis projected return to baseline at roughly 1.7 years post-discontinuation. Semaglutide is generally a long-term therapy, not a short course.
What is "Ozempic face" and is it permanent?
"Ozempic face" describes facial volume loss after rapid weight loss — sunken cheeks, prominent tear troughs, jawline laxity. The systematic review in plastic surgery literature attributes it to preferential fat loss in facial regions, not a direct drug effect on skin. It does not resolve on its own with maintained weight loss. Mitigation includes slower loss, protein intake, hydration, sun protection, and — for those wanting correction — dermal filler or fat grafting.
Are compounded versions of semaglutide still available in 2026?
Mostly no. FDA ended the broad compounding exception in February 2025. Pharmacies can still produce semaglutide when a clinician documents a specific medical need branded products cannot meet — typically a non-standard dose. The $200-per-month compounded subscription model is no longer permitted, and patients should be skeptical of any source still selling it that way.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.