A flavonoid hiding in your spice rack
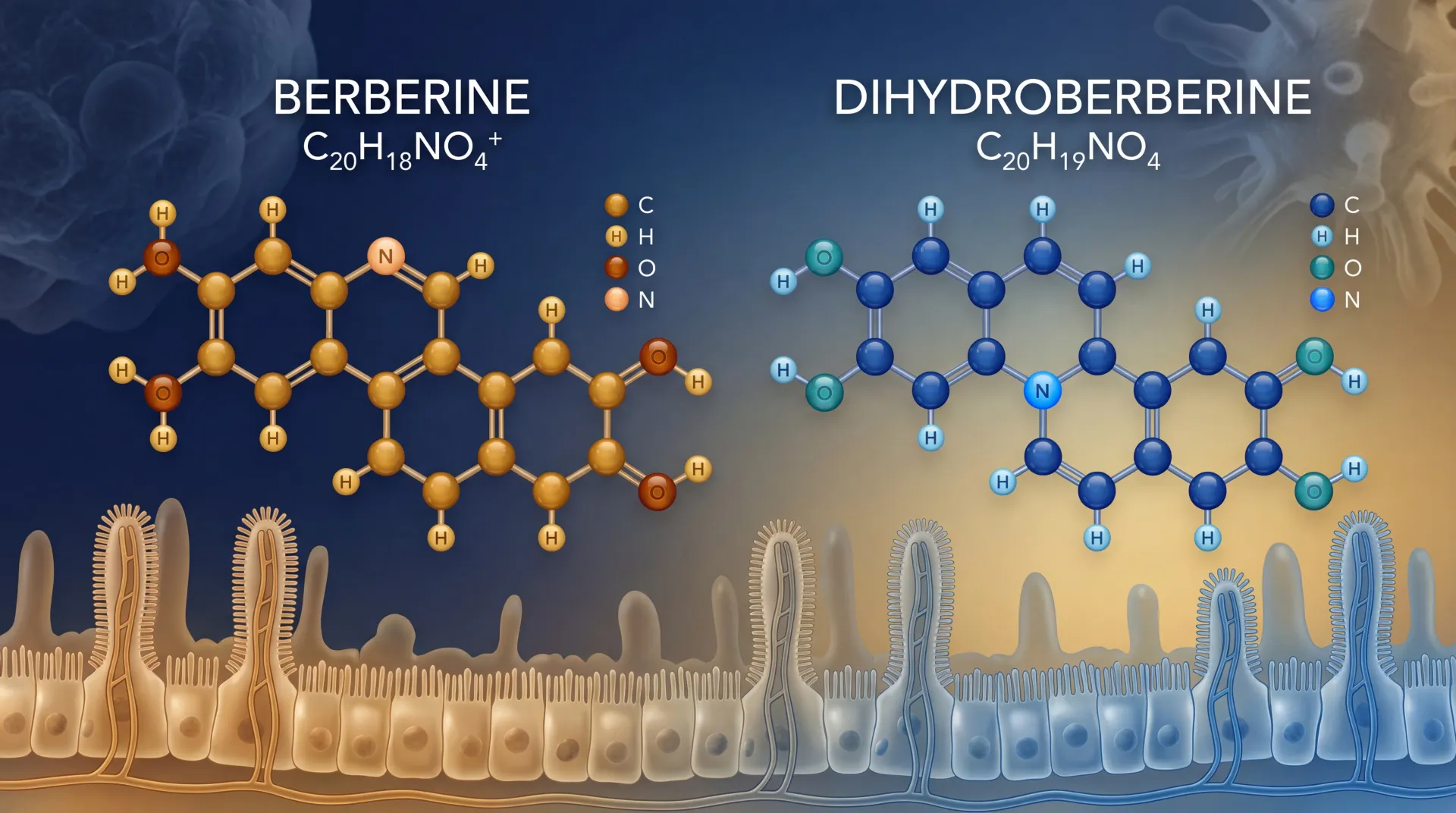
Apigenin belongs to a class of plant compounds called flavones, one branch of the broader flavonoid family. Its chemical name, 4',5,7-trihydroxyflavone, describes three hydroxyl groups attached to a 15-carbon skeleton, giving it a molecular weight of 270.24 g/mol. If that sounds abstract, picture a molecule built like a set of interlocking rings studded with oxygen atoms that love to bind things. That binding promiscuity is what makes apigenin interesting to researchers across such different fields.
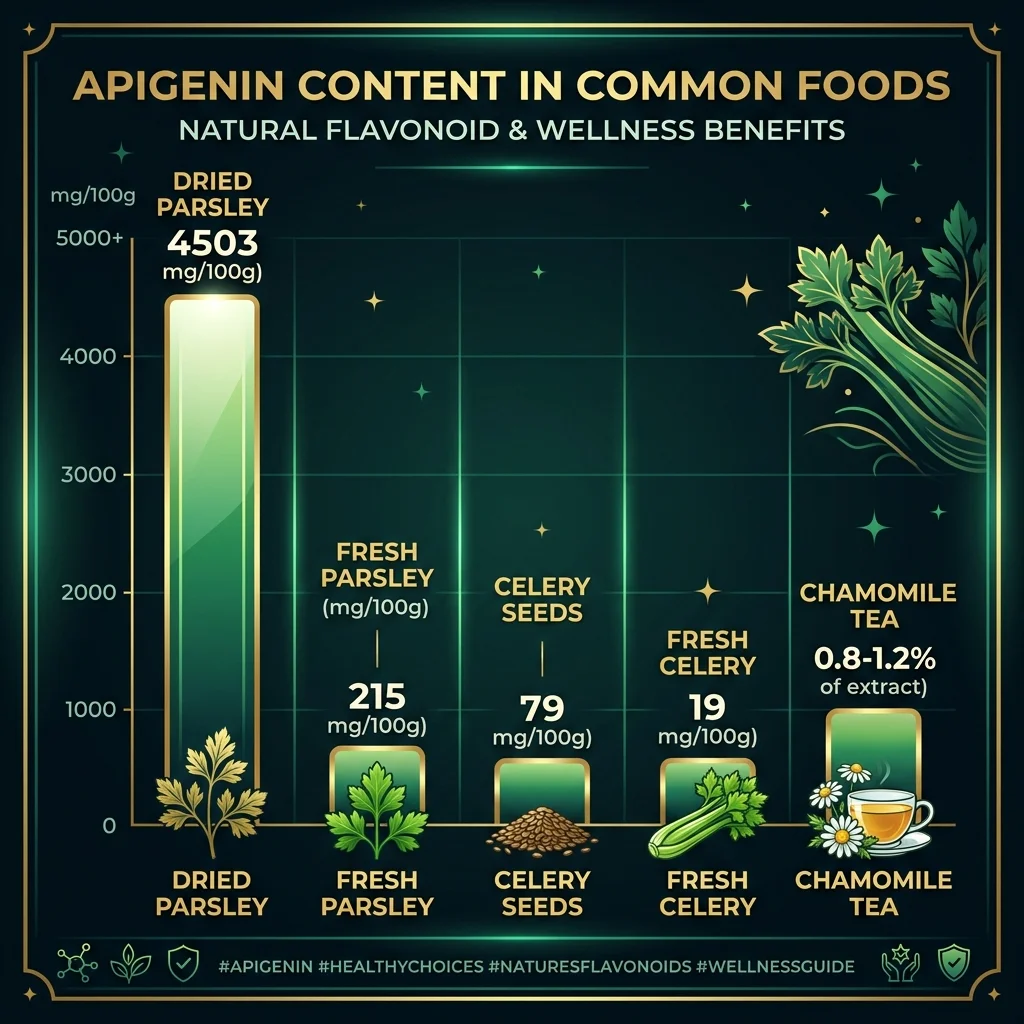
You have probably consumed apigenin today without knowing it. It is the dominant flavonoid in chamomile tea, making up 0.8 to 1.2% of chamomile extract. But the real concentration champion is parsley: dried parsley packs 4,503 mg per 100 grams, while fresh parsley delivers about 215 mg per 100g. Celery, another member of the same botanical family (Apiaceae), comes in at a more modest 19 mg per 100g fresh, though celery seeds concentrate it to about 79 mg. Beyond those, apigenin shows up in oregano, thyme, basil, tarragon, cilantro, and even red wine and beer.
Think of apigenin as a molecular Swiss Army knife. Its electron-rich structure gives it the ability to scavenge free radicals, chelate metal ions, and inhibit enzymes across unrelated biological pathways. That same promiscuity is both its promise and its problem: it does many things in a petri dish, but translating those effects to the human body is where the story gets complicated.
For practical purposes, two things matter. First, most dietary apigenin exists in glycosylated form, meaning it is attached to sugar molecules that affect how your gut processes it. Second, the average Western diet provides less than 5 mg of apigenin per day from fruits and vegetables, which is orders of magnitude below the doses used in laboratory studies. That gap between dietary intake and research doses runs through every claim you will read about this compound.
What your chamomile tea is actually doing to your brain
The sleep connection is the one most people encounter first, usually through the advice to drink chamomile tea before bed. But chamomile tea contains hundreds of compounds, so pinning the sedative effect on apigenin specifically requires careful work.
In animal studies, the evidence is reasonably clear. Mice given apigenin showed a 26 to 48% reduction in locomotor activity at doses of 30 to 100 mg/kg, consistent with mild sedation. At a much lower dose of 1.5 mg/kg, rats showed significantly reduced locomotor activity between 90 and 120 minutes after oral administration, suggesting the sedative effect kicks in with a delay rather than immediately.
The mechanism seems to involve the brain's GABA system, which is the same system targeted by benzodiazepines and alcohol. Apigenin binds to GABA-A receptors, but interestingly, this activity appears to be independent of the benzodiazepine binding site. Think of a GABA-A receptor like a building with multiple doors. Benzodiazepines enter through the front door; apigenin appears to use a side entrance. This distinction matters because it means apigenin is unlikely to carry the same dependence and tolerance risks associated with benzodiazepine drugs, though this has never been tested in humans over extended periods.
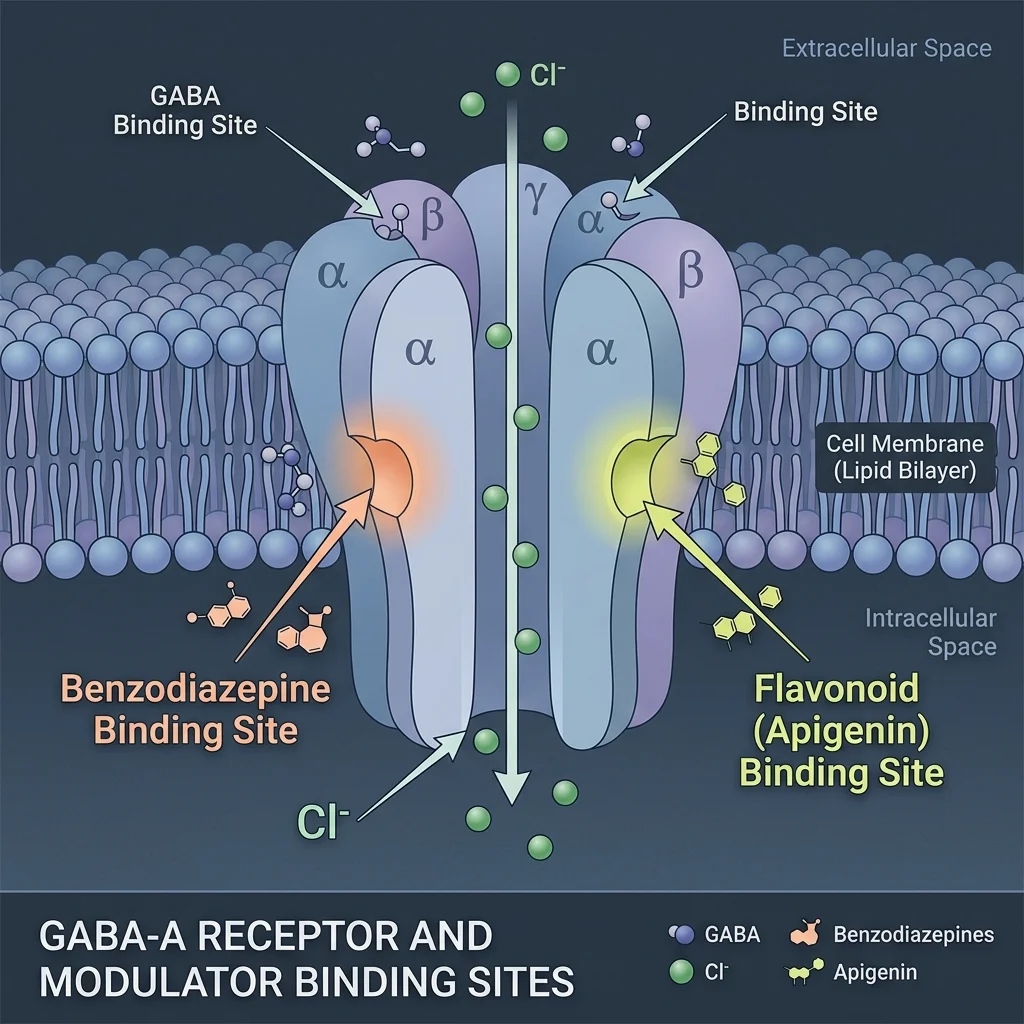
Apigenin also inhibits NMDA receptors, which are excitatory. Blocking excitation while boosting inhibition is a logical recipe for calming neural activity. Beyond receptors, rodent studies show apigenin decreased stress hormone (corticosterone) levels and increased BDNF and serotonin in the hippocampus, both of which are associated with healthy sleep.
Human evidence is where things get thin. Clinical trials have used chamomile extract, not apigenin alone. A pilot study giving insomnia patients 540 mg of chamomile extract twice daily for 28 days found only a trend toward improved daytime functioning that did not reach statistical significance. Studies on anxiety are more encouraging: 1,500 mg daily of chamomile extract for eight weeks reduced anxiety symptoms in patients with generalized anxiety disorder, and doses of 220 to 1,100 mg improved depression and mood scores. A randomized trial found that drinking chamomile tea for two weeks after childbirth significantly improved sleep efficiency and postnatal depression. And a cross-sectional study in a large adult cohort found that lower dietary apigenin intake correlated with worse sleep quality.
Key takeaway: Animal data shows apigenin has genuine sedative and anxiolytic activity through GABA modulation. Human data is limited to chamomile extract studies (not apigenin alone), showing benefits mainly for anxiety and mood rather than direct sleep improvement. The grandmother's remedy of chamomile tea before bed has some pharmacological backing, but attributing the effect to apigenin specifically remains unproven.
The testosterone connection: separating data from hype
Search for apigenin online and you will find supplement companies claiming it "boosts testosterone." The actual research behind this claim is far more nuanced, and most of it has never been tested in humans.
The primary mechanism through which apigenin might affect testosterone is indirect, running through an enzyme called CD38. This enzyme acts as a NADase, meaning it breaks down NAD+, a molecule central to cellular energy production that declines with age. In a landmark 2013 study published in Diabetes, Escande and colleagues demonstrated that apigenin inhibits CD38 activity, and in mice, this inhibition nearly doubled liver NAD+ levels while improving glucose and lipid homeostasis. A 2020 study by Ogura et al. confirmed this in diabetic rats, showing that apigenin downregulated CD38 expression, increased the NAD+/NADH ratio, and restored Sirt3 activity in kidney tissue.
Testosterone enters the picture through a secondary connection: NAD+ and the sirtuins it powers are involved in cellular processes that include steroidogenesis. Higher NAD+ levels could theoretically support testosterone production, but this is a chain of reasoning with multiple unverified links, not a demonstrated effect.
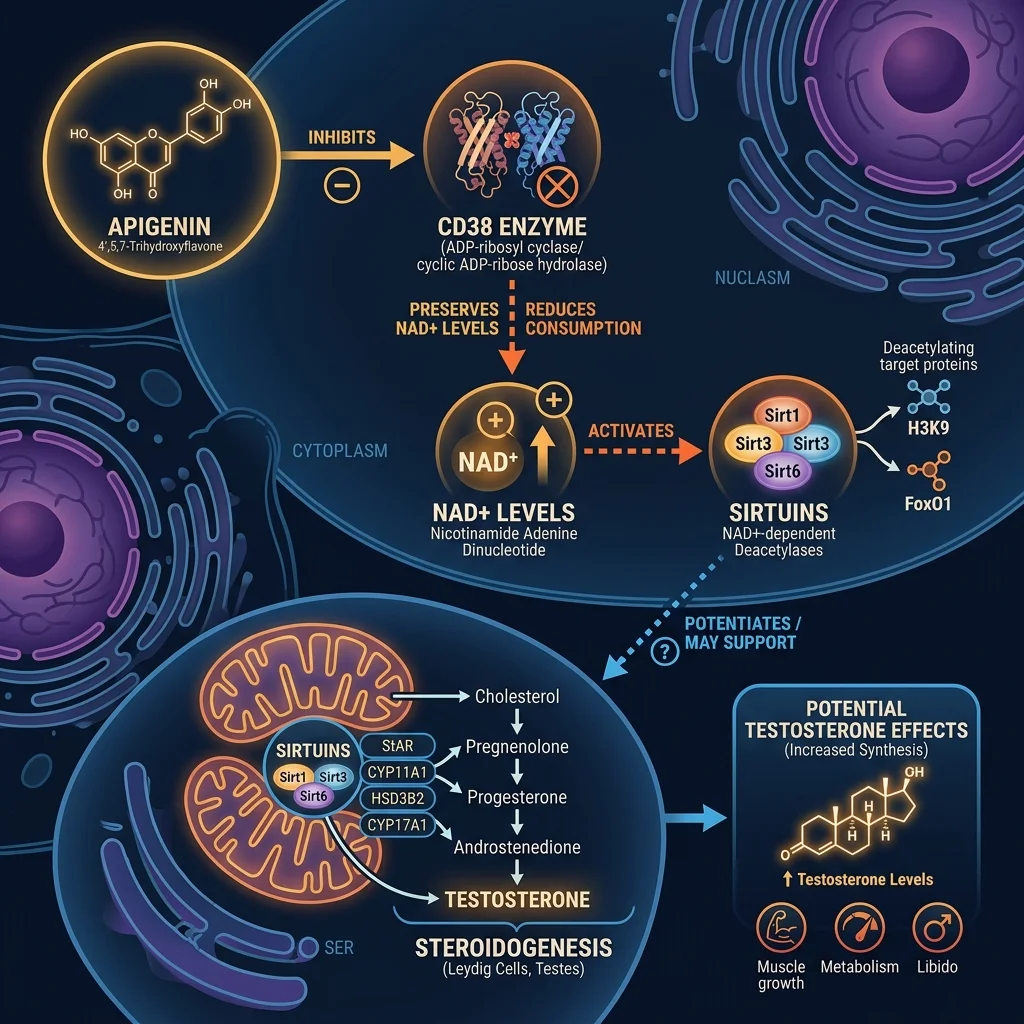
More directly, preclinical data from cell studies shows that apigenin modified steroidogenic enzyme receptors and activity at concentrations of 5 to 10 micromolar. A separate study found that apigenin inhibited aromatase activity in human ovarian cells. Aromatase converts testosterone to estrogen, so inhibiting it could theoretically preserve testosterone levels. Apigenin also reduced cortisol production by up to 47.3% in human adrenal cells in vitro at concentrations of 12.5 to 100 micromolar.
| Claim | Evidence type | Status |
|---|---|---|
| Apigenin inhibits CD38, boosting NAD+ | Mouse and rat studies | Demonstrated in animals |
| Apigenin inhibits aromatase | Cell culture (ovarian cells) | In vitro only |
| Apigenin modifies steroidogenic enzymes | Cell culture (5-10 uM) | In vitro only |
| Apigenin reduces cortisol | Cell culture (adrenal cells) | In vitro only |
| Apigenin raises testosterone in humans | None | No human data exists |
The honest assessment: no human clinical trials have tested apigenin's direct effects on testosterone. The aromatase inhibition and steroidogenic enzyme findings come from cell cultures at concentrations that may not be achievable through oral supplementation. The CD38/NAD+ pathway is real and well-documented in animals, but the leap from "more NAD+" to "more testosterone" has not been measured in people. Anyone selling apigenin supplements as a testosterone booster is running ahead of the evidence.
Anti-cancer mechanisms: what happens in the lab versus the body
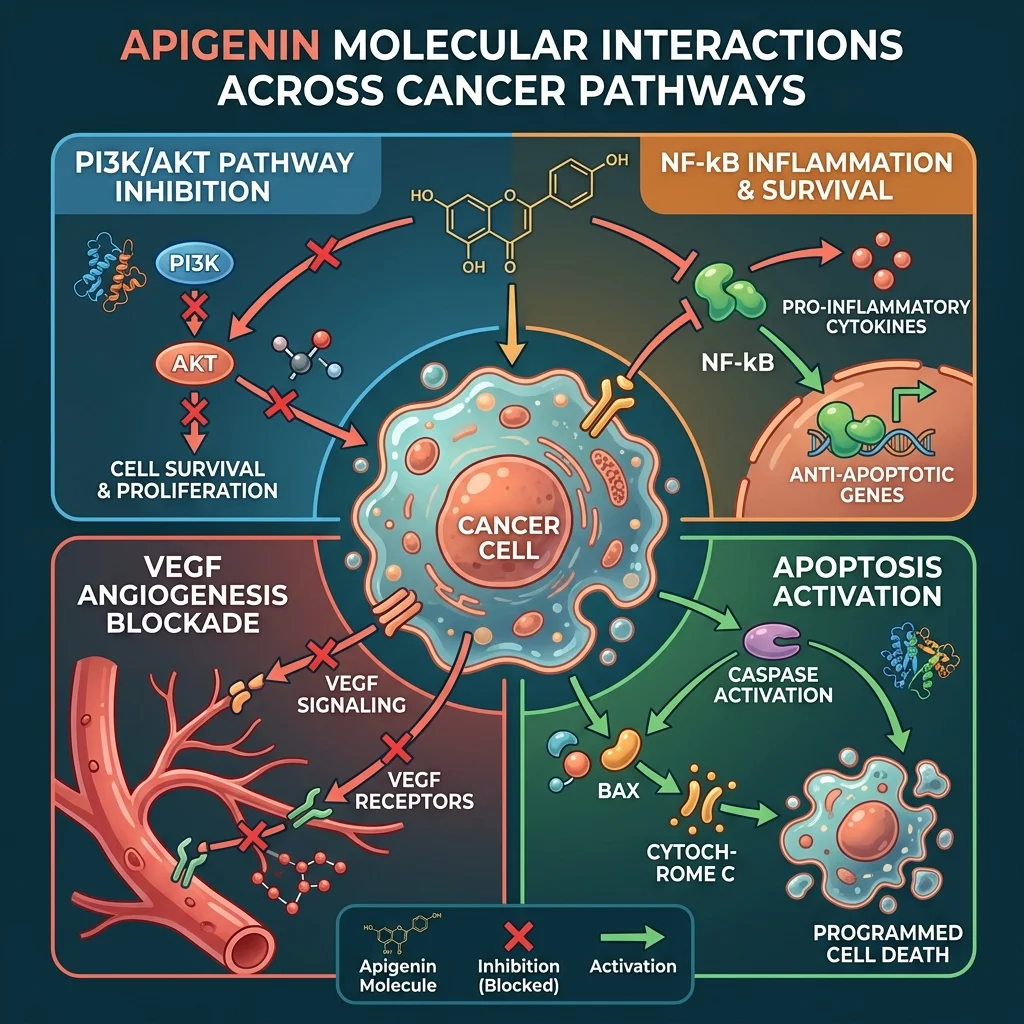
Apigenin was first proposed as an anti-carcinogenic agent in the 1980s, and since then, hundreds of lab studies have explored its effects on cancer cells. The in vitro evidence covers a lot of ground. Apigenin hits multiple cancer-related pathways simultaneously: it targets PI3K/Akt/mTOR, MAPK/ERK, JAK/STAT, NF-kB, and Wnt/beta-catenin signaling. It triggers programmed cell death through both intrinsic and extrinsic apoptotic pathways, and it inhibits HIF-1-alpha and VEGF, which tumors need to build blood supply.
In animal models, the results follow a similar pattern. Mice with prostate cancer xenografts given oral apigenin at 20 to 50 micrograms per mouse daily for eight weeks showed markedly reduced tumor growth. In a breast cancer xenograft model, daily apigenin injections increased apoptosis in tumor cells and reduced proliferation. Apigenin also sensitized colon cancer cells to the chemotherapy drug ABT-263 by inhibiting a drug-resistance protein called Mcl-1.
Human observational data tells a different story. The Women's Health Study followed 38,408 women for 11.5 years and found no significant association between flavonol or flavone-rich food intake and cancer incidence, with relative risks ranging from 1.01 to 1.15 across cancer types. The Nurses' Health Study, with 66,940 women, actually found a trend toward increased ovarian cancer incidence with higher apigenin intake (p=0.03), though the result was not statistically significant when analyzed by quintile.
One small interventional study provides a counterpoint: patients with resected colon cancer who took a combination of 20 mg apigenin plus 20 mg EGCG daily had zero recurrences out of 14 patients, compared to a 20% recurrence rate (3 out of 15) in untreated controls. But this used a flavonoid mixture, not apigenin alone, and the sample was tiny.
The gap: There is a canyon between what apigenin does to cancer cells in a dish and what dietary apigenin does inside a living human. Lab studies use concentrations that far exceed what oral supplementation achieves in blood plasma. The Alzheimer's Drug Discovery Foundation classifies the cancer evidence as "MIXED" in humans and notes that observational studies in people have produced conflicting results. Apigenin is not an anti-cancer drug. It is a dietary compound with anti-cancer properties in controlled laboratory settings.
The bioavailability problem: why your body barely absorbs it
Every benefit described above runs into the same wall: apigenin is poorly absorbed. Under the Biopharmaceutics Classification System, apigenin is categorized as Class II: low solubility, high permeability. It crosses cell membranes easily once dissolved, but getting it dissolved in the first place is the bottleneck.
Only 5 to 10% of ingested apigenin gets absorbed in the small intestine. The remaining 90 to 95% travels to the colon, where gut bacteria break it down into smaller phenolic compounds. But less than 30% of the original apigenin is eventually excreted in feces, meaning a large portion gets metabolized by the microbiome into byproducts that may themselves have biological activity. Your gut bacteria are doing their own pharmaceutical chemistry with the apigenin you swallow.
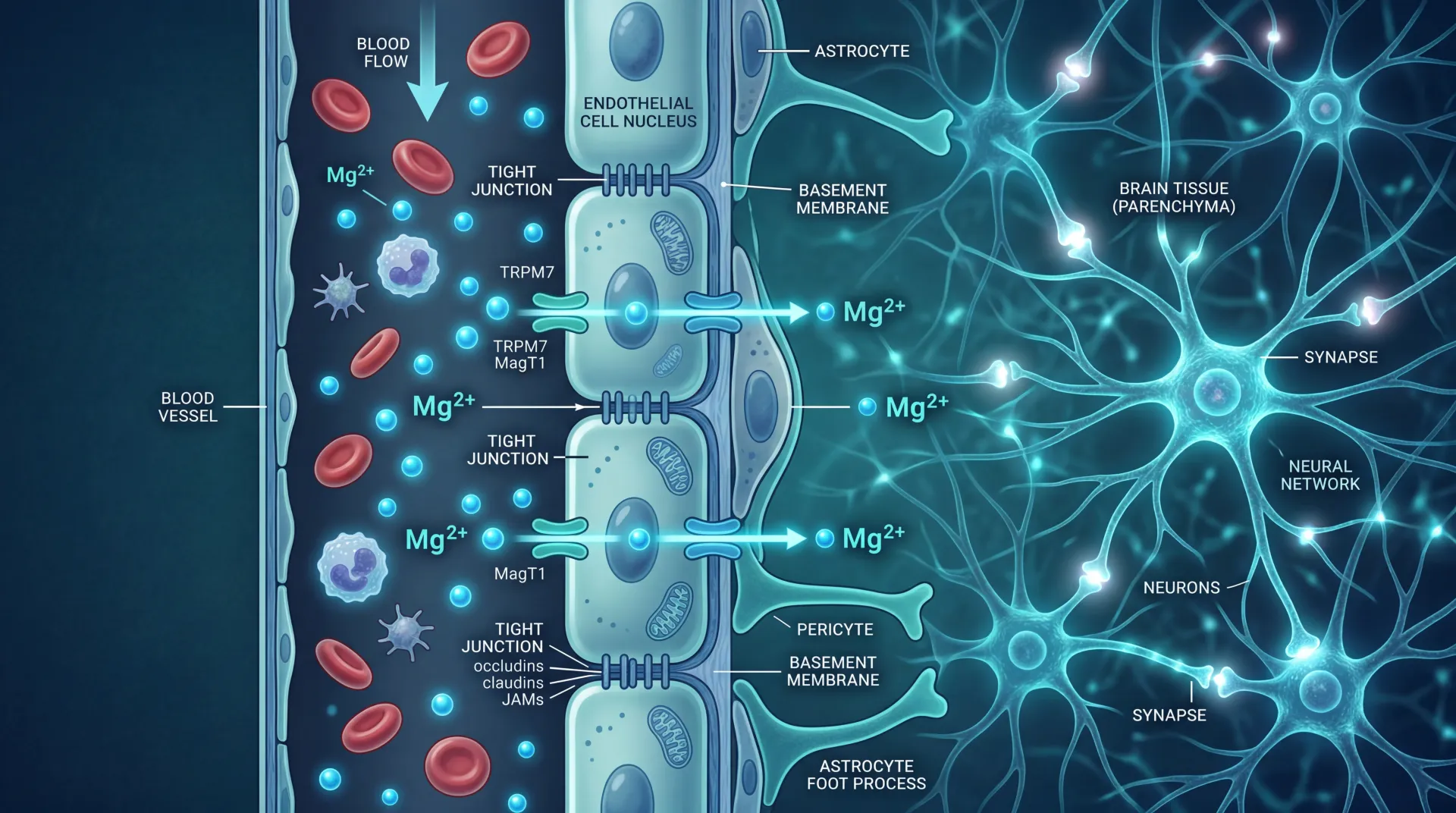
Once absorbed, apigenin sticks around. The ADDF reports a half-life of 91.8 hours, so it takes nearly four days for blood levels to drop by half. It also crosses the blood-brain barrier, which is relevant to the sleep and neuroprotective claims. But the initial absorption hurdle means that the amount reaching the bloodstream is a fraction of what you consume.
| Property | Value | Practical meaning |
|---|---|---|
| Small intestine absorption | 5-10% | Most of what you swallow does not reach blood |
| Reaches colon | 90-95% | Gut bacteria metabolize the majority |
| Fecal excretion | Less than 30% | Microbiome converts much of it to other compounds |
| Half-life | 91.8 hours | Once absorbed, it stays in circulation for days |
| Blood-brain barrier | Penetrant | Can reach brain tissue |
Supplement manufacturers have tried to solve the absorption problem. Isolated apigenin is unstable, so some formulations use nanoparticles, liposomes, or polymer-based carriers to improve solubility. Examine.com notes that isolated apigenin is rarely stable enough to be absorbed by the body and recommends choosing formulations that address this instability. The glycosidic forms of apigenin found naturally in food may actually have higher bioavailability than isolated supplements, which is an ironic twist: the food source might deliver the compound more effectively than the pill.
Typical supplements contain 50 mg per capsule. Dietary intake from a normal diet is estimated at less than 5 mg per day. The anxiolytic dose range suggested by animal research is 3 to 10 mg/kg body weight, which for a 70 kg person translates to 210 to 700 mg. Given 5 to 10% absorption, you would need to consume substantially more than that orally to approach those blood levels.
Who should think twice before taking apigenin
Apigenin has a reputation as safe, and the animal data generally supports this. Rodent studies have found no significant toxicity even at high doses. At doses of 30 to 100 mg/kg in mice, the main observable effect was sedation, not organ damage. At doses up to 80 mg/kg, it did not act as an anticonvulsant or muscle relaxant, which distinguishes it from benzodiazepines.
The primary safety concern is drug interactions. Apigenin is a potent inhibitor of CYP2C9, a liver enzyme responsible for metabolizing a long list of common medications. If CYP2C9 is suppressed, those drugs stay in your system longer and at higher concentrations than intended, potentially amplifying both effects and side effects.
Medications that rely on CYP2C9 for metabolism include NSAIDs, warfarin, fluoxetine, sulfonylureas, losartan, tamoxifen, fluvastatin, sildenafil, and amitriptyline. If you take warfarin (a blood thinner), adding high-dose apigenin could increase bleeding risk. If you take fluoxetine (an antidepressant), apigenin could raise blood levels of the drug. A mouse study also found that apigenin increased blood levels of venlafaxine, another antidepressant.

| Who should be cautious | Reason |
|---|---|
| People taking blood thinners (warfarin) | CYP2C9 inhibition may increase bleeding risk |
| People on antidepressants (fluoxetine, venlafaxine) | May raise drug blood levels |
| People taking diabetes medications (sulfonylureas) | May amplify blood sugar lowering effects |
| Pregnant or breastfeeding women | No safety data available; avoidance recommended |
| People scheduled for surgery | Potential bleeding interaction with NSAIDs/anticoagulants |
What has not been studied is long-term safety at supplement doses in humans. Only three clinical trials have included apigenin, none tested it alone, and they enrolled a total of just 161 people. Data assessing side effects and drug interactions from apigenin are currently limited, and available information comes from in vitro or animal studies. Pregnancy and lactation data are essentially nonexistent; avoidance is recommended.
If you are healthy, not pregnant, and not taking medications metabolized by CYP2C9, dietary apigenin from food is almost certainly safe. Supplementation at 50 mg is probably fine for most people, but the honest answer is that nobody has systematically studied it. Talk to your doctor before adding it to any medication regimen.
Frequently Asked Questions
Does apigenin directly improve sleep, or is that just the chamomile?
Animal studies show apigenin itself has sedative and anxiolytic properties through GABA-A receptor binding and NMDA receptor inhibition. Human studies have only tested chamomile extract, which contains many compounds besides apigenin. The sleep-promoting effects are likely a combination of multiple chamomile constituents, with apigenin contributing to but not solely responsible for the effect.
Can I get enough apigenin from food instead of supplements?
A typical Western diet provides less than 5 mg of apigenin daily. To match a standard 50 mg supplement, you would need roughly 23 grams of fresh parsley or about 2.5 cups of strong chamomile tea daily. Food-sourced apigenin may actually be more bioavailable than isolated supplements because the glycosidic forms in plants are more water-soluble. Eating parsley, celery, and chamomile tea regularly is a reasonable dietary strategy, though it will not approach the doses used in most research studies.
Will apigenin actually raise my testosterone levels?
There is no human evidence that apigenin raises testosterone. The theoretical pathway runs through CD38 inhibition, NAD+ elevation, and downstream effects on steroidogenic enzymes, but this chain has only been demonstrated in cell cultures and rodents. In vitro aromatase inhibition has been observed, but it is unclear whether oral apigenin achieves sufficient blood concentrations to replicate this effect in people. Treat testosterone claims about apigenin as unproven.
Is apigenin safe to take with other supplements like NMN or resveratrol?
No studies have specifically examined combinations of apigenin with NMN, NR, or resveratrol in humans. Since apigenin, NMN, and NR all aim to increase NAD+ levels through different mechanisms, combining them is a reasonable hypothesis but lacks clinical validation. The CYP2C9 inhibition by apigenin is the main interaction concern, and that applies primarily to pharmaceutical drugs rather than other supplements.
How long does it take for apigenin to have an effect?
In rats, the sedative effect of apigenin peaked between 90 and 120 minutes after oral administration. The exceptionally long half-life of 91.8 hours means that with regular daily dosing, blood levels would accumulate over about two weeks before reaching steady state. Any single-dose effect on relaxation may appear within a couple of hours, but broader biological effects like NAD+ modulation would require sustained intake.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.