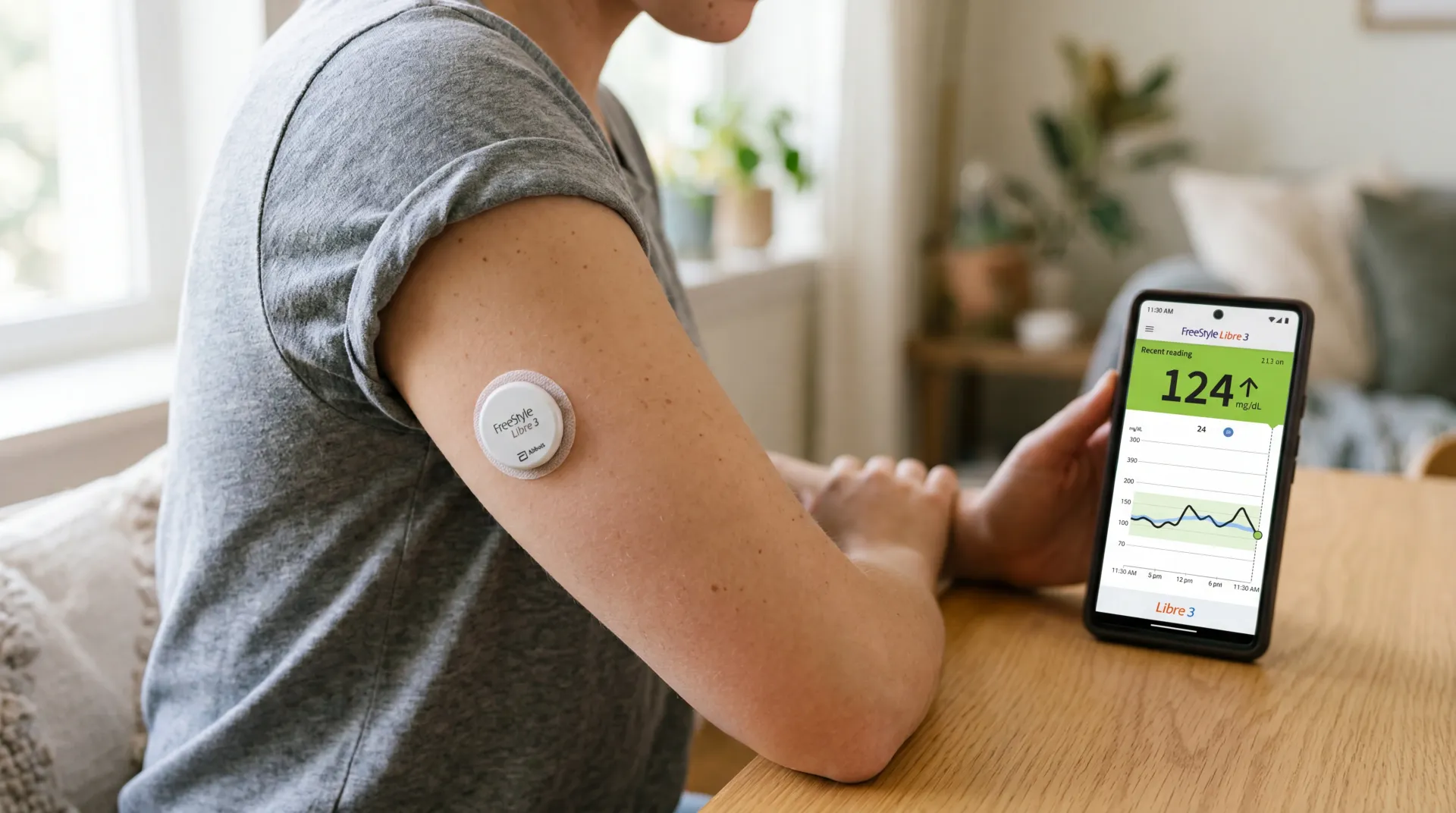
Your blood sugar tells a story you've never been able to read
On March 5, 2024, the U.S. Food and Drug Administration did something that would have seemed absurd a decade earlier: it cleared an over-the-counter continuous glucose monitor for anyone 18 and older, including people who don't have diabetes. The device was Dexcom's Stelo. Three months later, Abbott's Lingo followed. For the first time, healthy Americans could walk up to a screen, order a biosensor, stick it on their arm, and watch their blood sugar fluctuate in real time without a prescription or a single finger prick.
The market these companies are chasing is massive. Dexcom estimates that 125 million Americans have either type 2 diabetes managed without insulin or some form of prediabetes, most of it undiagnosed. According to William Blair analysts cited in MedTech Dive, roughly 700,000 to 800,000 people who don't take insulin were already using CGMs before these OTC devices even launched.
So what does a CGM actually do? Think of it as a weather station for your metabolism. A tiny filament sits just beneath your skin, sampling glucose levels in interstitial fluid every few minutes and streaming the data to your phone. The application process is surprisingly undramatic. Adrienne So, reviewing the Lingo for Wired, described it as feeling "like getting flicked with a finger." The sensor stays put for about two weeks, through showers and workouts, then you peel it off and replace it.
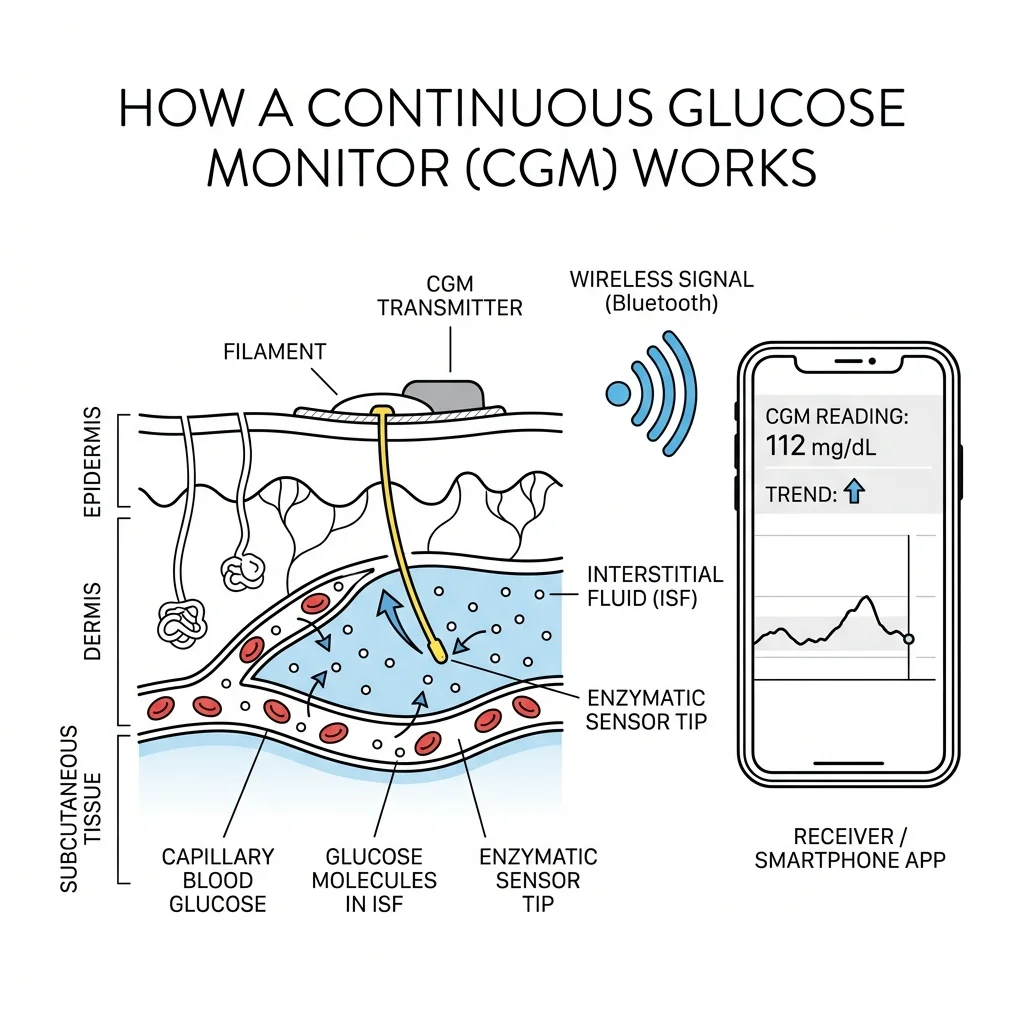
What the data reveals can catch people off guard. A 2023 review in the Journal of Diabetes Science and Technology by Dr. David C. Klonoff and colleagues at Mills-Peninsula Medical Center cataloged eight studies of healthy people wearing CGMs since 2007. In all of them, glucose stayed almost entirely within 70 to 140 mg/dL. That tight corridor is normal. But within it, the variation is wildly personal. Eat the same bowl of oatmeal as the person next to you, and your glucose curve might look nothing like theirs. A landmark study by Zeevi et al. tracked 800 adults for a week with CGMs, then built a machine learning model that could predict individual glucose responses based on factors ranging from gut microbiome to anthropometric data.
That individual variation is the core appeal for non-diabetics. Marilyn Tan, an endocrinologist at Stanford Medicine, told MedTech Dive that CGMs "allow for more individualized diet recommendations" because "each person reacts differently to different foods." Fasting glucose, hormonal cycles, stress hormones, sleep quality, and even altitude all shape the curve. For someone trying to understand why they crash after lunch or why their energy drops at 3 p.m., a CGM can provide answers that generic dietary advice never could.
Abbott Lingo vs Dexcom Stelo: picking the right sensor for your arm
Abbott and Dexcom took notably different approaches to the OTC market. Dexcom's Stelo is designed primarily for people with type 2 diabetes who manage without insulin, though its broad FDA label also allows use by anyone. Abbott split its lineup: Lingo targets wellness-minded consumers without diabetes, while a separate device called Libre Rio competes for the type 2 non-insulin market. According to MedTech Dive, Rio can measure glucose up to 400 mg/dL, while Lingo caps at 200 mg/dL since wellness users won't see values that high.
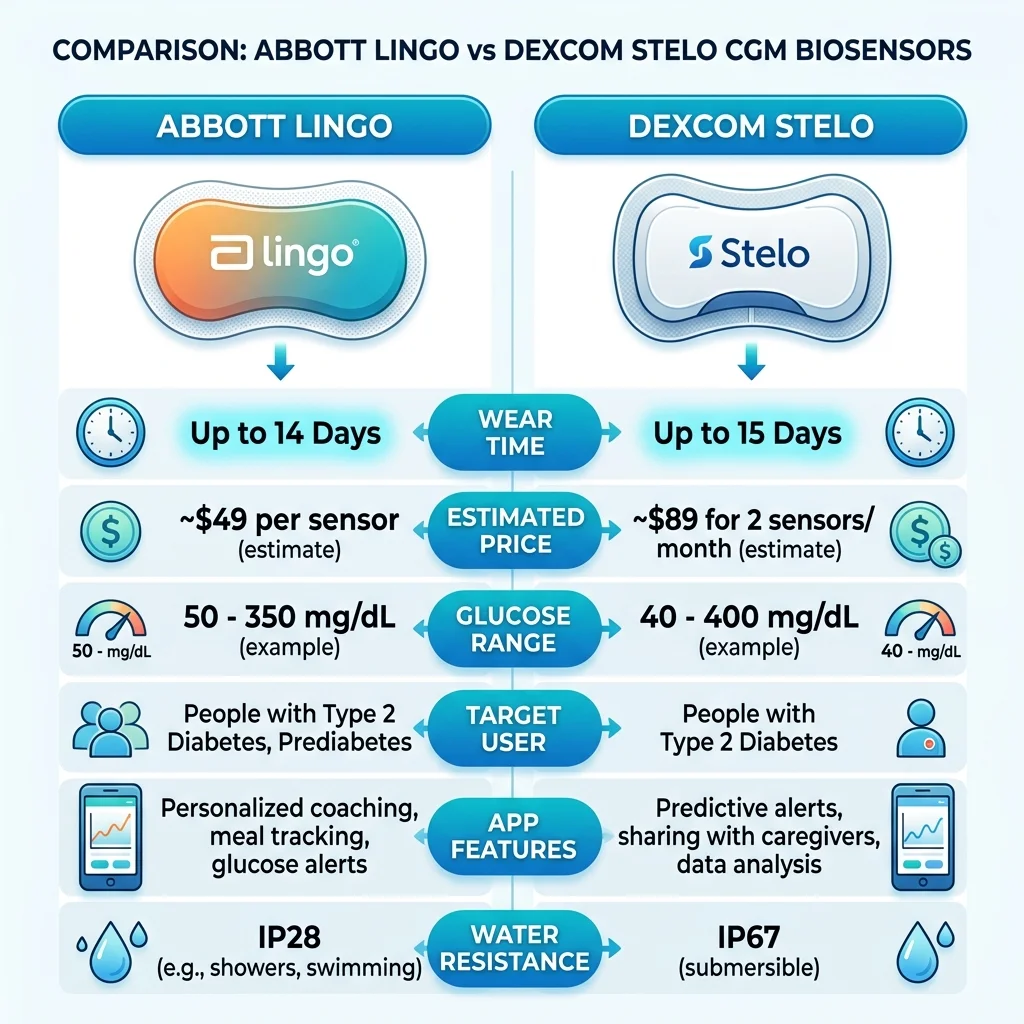
| Feature | Dexcom Stelo | Abbott Lingo |
|---|---|---|
| FDA clearance | March 2024 | June 2024 |
| Wear time | Up to 15 days | Up to 14 days |
| Price | $99 single pack / $89/month subscription | ~$49 per sensor (~$98/month) |
| Water resistance | Waterproof (highest rating) | Water-resistant |
| Glucose range | Standard iCGM range | Capped at 200 mg/dL |
| Primary target | T2 diabetes (no insulin) + general wellness | General wellness / non-diabetics |
| Key app feature | Spike and pattern detection | Lingo Count (proprietary metabolic stress score) |
| Integrations | Apple Watch, Oura Ring | Apple Health sync |
| FSA/HSA eligible | Yes | Yes |
Jake Leach, Dexcom's chief operating officer, told MedTech Dive the Stelo app was built to onboard people who have never used a CGM before, with education about what blood glucose readings mean and how daily fluctuations are normal. Lingo takes a different approach with its proprietary "Lingo Count," which quantifies the metabolic stress from each glucose spike as a single number. Wired's review found the app clear and practical, giving it an 8 out of 10.
The integration story matters if you already wear other devices. Dexcom has an Apple Watch app and a partnership with Oura, which is a meaningful advantage for anyone who tracks sleep and wants glucose data in the same ecosystem. Abbott's Lingo syncs workout data from Apple Health into its app, and the company recently made a strategic investment in Whoop, which raised $575 million in March 2026. Both companies are FSA and HSA eligible, which shaves the sting off the out-of-pocket cost.
A practical note: if you only want to learn how your body responds to food, you may not need a permanent subscription. Michael Fang, an epidemiologist at Johns Hopkins, suggested that "maybe letting people wear the sensors once or twice is enough. After they learn about what foods do to their glucose levels, they'll know how to adjust their behaviors."
The skin doesn't want your vitamins (mostly)
While CGM patches are reading data from your body, a different category of wearable patch claims to deliver substances into it. Vitamin patches for B12, iron, magnesium, and melatonin have become a social media staple. The pitch is appealing: skip the pill, skip the digestive system, absorb nutrients directly through your skin. The problem is that your skin evolved specifically to prevent this.
Michelle Spear, Professor of Anatomy at the University of Bristol, explained the barrier in The Conversation. The skin's outermost layer, the stratum corneum, works like a brick wall. Dead skin cells are the bricks; a waxy mix of lipids is the mortar. Only small, fat-soluble, uncharged molecules can slip through that barrier. Nicotine fits the bill perfectly, which is why nicotine patches have been a proven smoking cessation tool for decades. Estradiol (used in hormone replacement therapy) and fentanyl (for chronic pain) also work transdermally because they share those molecular properties.
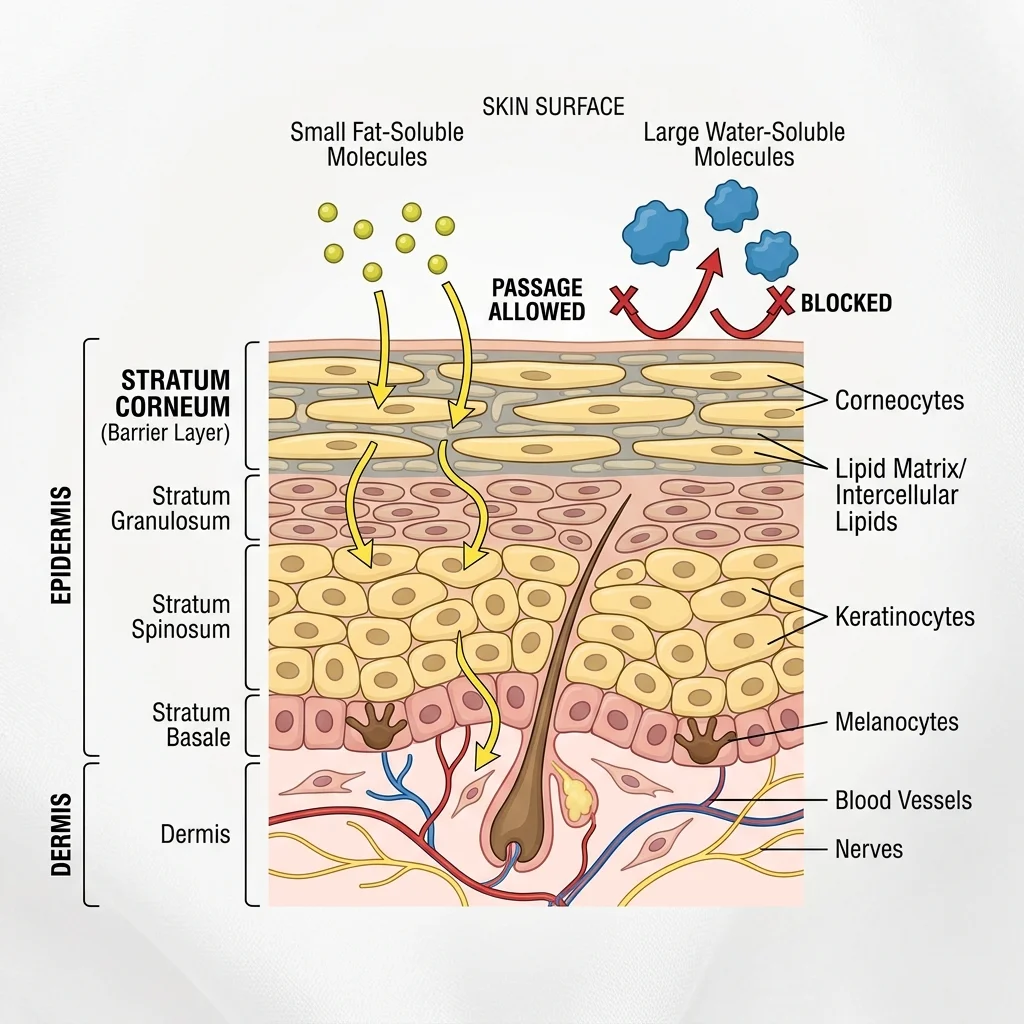
Most popular vitamin patch ingredients don't share those properties. Carol Johnston, professor of nutrition at Arizona State University, put it bluntly to National Geographic: "It's a barrier. That's what the skin is designed to do." Vitamin B12, magnesium, and iron are typically too large or too water-soluble to cross the skin in meaningful amounts. Nial Wheate, a professor at Macquarie University, added that "patches cannot hold anywhere near as many vitamins and minerals as a tablet can."
The clinical evidence is mixed but largely discouraging. A study of gastric bypass patients found that those using a multivitamin patch were more likely to have vitamin D deficiency than those taking oral supplements. A separate trial in athletes with low iron showed that iron pills raised iron levels while the patch produced no beneficial effects. One brighter result: a UK trial found that a vitamin D patch increased blood levels after eight weeks in healthy adults, though vitamin D is fat-soluble, which at least gives it a plausible absorption pathway.
Melatonin is the strongest candidate among supplement patches, and for the same molecular reason that makes nicotine work: it's small and lipophilic. A study cited by the Sleep Foundation found that transdermal melatonin patches helped maintain sleep during daytime hours, reduced premature awakenings, and increased time in both stage 2 and REM sleep. The trade-off is delivery speed. Oral melatonin hits the bloodstream faster but wears off quickly; a patch provides slower, sustained release, which makes it better suited for staying asleep rather than falling asleep.
Evaluating a vitamin patch: Does it contain small, fat-soluble molecules? Does the label state the dose in milligrams and the delivery rate? Does it use a controlled-release system (matrix or reservoir)? If the answer to all three is yes, there's at least a scientific basis. If it just says "infused with essential oils," save your money.
Why checking drug levels still means a needle in your arm (for now)
The most technically ambitious category of wearable patches doesn't deliver vitamins or read glucose. It monitors drug levels in real time, something that currently requires a trip to a phlebotomist and a wait for lab results.
Conventional therapeutic drug monitoring works by drawing blood at one or two time points, sending it to a lab, and getting back a number that tells the clinician whether the drug concentration is in the right range. For drugs with a narrow therapeutic window, this matters enormously. Too little means the drug doesn't work; too much means toxicity. The problem is that a snapshot at one time point tells you almost nothing about the drug's actual trajectory through a patient's body.

A 2025 study published in Nature Communications demonstrated a system that could change this. Researchers built a Microneedle-based Continuous Biomarker/Drug Monitoring (MCBM) system that simultaneously tracks both glucose and metformin, the most widely prescribed type 2 diabetes drug, in skin interstitial fluid. The dual-sensor microneedle uses a layer-by-layer nanoenzyme strategy to achieve high sensitivity, and it feeds data to a smartphone app for real-time pharmacokinetic analysis. In vivo trials showed the system could precisely track both biomarkers at once while maintaining biocompatibility for extended wear.
This is significant because roughly 90% of diabetes cases are type 2, and metformin is the first-line treatment for most of them. Yet most patients follow a one-size-fits-all dosing schedule that ignores individual differences in how they metabolize the drug. A wearable that continuously monitors drug levels could let clinicians personalize dosing in a way that blood draws every few months never could.
The technology isn't limited to diabetes drugs. Carol Johnston at Arizona State told National Geographic that researchers are actively exploring microneedle technology to improve transdermal delivery and sensing. "That's where the research is right now," she said, pointing to the intersection of CGM-style sensors and pharmaceutical monitoring.
What CES 2026 revealed about where biosensors are headed
CES 2026 in Las Vegas offered a preview of what's coming next. The show floor was dense with health tech, and several devices pointed toward a future where patches do far more than read glucose.
The device that drew the most attention was the PF-Sweat Patch from Point Fit Technology, a spinoff from the Hong Kong University of Science and Technology. It won a CES 2026 Innovation Award in Digital Health. The device is described as the world's first ultra-thin wearable skin patch that tracks health through sweat analysis, powered by proprietary nanomembrane technology. Its first biomarker is lactate, which is relevant for endurance athletes and mitochondrial health. The company says the modular design will support cortisol, creatinine, and glucose in future versions. Point Fit claims the patch has been clinically validated against gold-standard blood biomarker tests.

Abbott also made moves at CES 2026, unveiling a new Libre Assist app feature that uses AI to tell people with diabetes how their meals may affect glucose levels. And the Peri wearable, another CES debut, demonstrated a body-worn patch that detects menopausal symptoms like night sweats, anxiety, and hot flashes by sticking directly to the torso.
These devices point in the same direction: biosensors are moving from single-analyte devices (glucose only) toward multi-marker platforms. Sweat chemistry and interstitial fluid analysis are getting miniaturized into wearable form factors, alongside even urine analysis. Lab diagnostics and consumer wearables are converging, though slowly.
What the hype cycle leaves out
The enthusiasm for wearable patches runs ahead of the evidence in several important ways, and the experts who study this technology most closely are the ones saying it loudest.
Elizabeth Selvin, a diabetes researcher and epidemiology professor at Johns Hopkins, told the Bloomberg School of Public Health that "we don't actually know that monitoring or manipulating CGM glucose levels in people without diabetes can improve health." Her colleague Michael Fang was even more direct: "In people without diabetes, we don't really know how to act on differing glucose patterns. All the clinical information about how to interpret and act on the information from CGMs is for people with diabetes."
The numbers back up the caution. A 2024 review of randomized trials found that CGM feedback reduced hemoglobin A1C by 0.3% and time in range by 7%, both small improvements. And Fang pointed out that the FDA's decision to allow OTC CGMs "whether they actually improved health outcomes was not a factor."
| Patch type | What works | What doesn't (yet) |
|---|---|---|
| CGM (glucose monitoring) | Accurate glucose tracking, FDA-cleared, proven for diabetics | No clinical trials proving health benefit for non-diabetics |
| Melatonin patches | Small lipophilic molecule, some evidence for sleep maintenance | Limited studies, not FDA-regulated as supplement |
| B12/iron/magnesium patches | Theoretical basis if fat-soluble formulation | Most molecules too large or water-soluble; clinical evidence weak |
| Drug monitoring biosensors | Lab-validated accuracy for glucose + metformin | Still in research stage; no consumer products available |
| Sweat biosensors | CES 2026 prototypes clinically validated for lactate | Single-biomarker; multi-marker versions still in development |

There's also a psychological risk. Priya Tew, a registered dietitian specializing in eating disorders, told the BBC that she's seeing patients in clinic who arrive with CGM reports and say they "can't eat any of these foods because they give me a big spike." Sports dietitian Renee McGregor described athletes who, after using CGMs, developed "a fear of carbohydrates" and started cutting food groups unnecessarily, leading to injuries. Selvin at Johns Hopkins offered a concrete example of why glucose data alone can mislead: "If you substitute a high-salt, high saturated-fat food like a sausage for an orange at breakfast, your glucose may not rise as much, but that is not necessarily a good trade-off."
For vitamin patches, the evidence gap is even wider. David Seres, a professor of medicine at Columbia University, explained to National Geographic that the reason nicotine and fentanyl patches work is that "they're rigorously tested." Most vitamin patches haven't undergone anything comparable. And Nial Wheate at Macquarie University offered the most practical advice: "Save your money. You do not need them unless your doctor has told you that you were deficient."
None of this means the technology is useless. CGMs are transformative for people with diabetes. Melatonin patches have plausible science behind them. Drug monitoring biosensors could change how clinicians dose medications. The question is whether the consumer versions of these products, marketed to healthy people willing to spend $89 a month, deliver value that matches the price tag. Right now, the honest answer is: we don't have enough data to know.
Frequently Asked Questions
Do I need a prescription for a continuous glucose monitor?
Not anymore for the consumer versions. Both the Dexcom Stelo and Abbott Lingo are available over the counter without a prescription. Stelo launched in August 2024, and Lingo followed shortly after. You can order them online and they're eligible for FSA and HSA spending accounts. However, prescription CGMs like the Dexcom G7 and Abbott FreeStyle Libre, which are designed for insulin-dependent diabetics, still require a prescription and are typically covered by insurance.
Can vitamin patches actually deliver nutrients through the skin?
It depends entirely on the molecule. Small, fat-soluble compounds like melatonin have a plausible absorption pathway because they can pass through the skin's lipid barrier. But most popular supplement patch ingredients, including vitamin B12, iron, and magnesium, are too large or too water-soluble to cross the skin in therapeutic amounts. A study of gastric bypass patients found that patch users were more vitamin D deficient than those taking oral supplements. The few vitamin patches with evidence behind them tend to contain fat-soluble molecules and use controlled-release delivery systems.
Are CGMs worth it if I don't have diabetes?
Experts are divided. If you're curious about how specific foods affect your body, even a single two-week session can provide useful personal data. Michael Fang at Johns Hopkins has suggested that wearing a sensor once or twice might be enough to learn your patterns. But no major clinical trials have demonstrated that CGMs improve health outcomes for people without diabetes, and there are risks of developing an unhealthy fixation on glucose numbers. The technology costs $89 to $99 per month without insurance, so the value proposition depends on how actionably you use the data.
What is a microneedle biosensor patch?
Microneedle biosensor patches use arrays of microscopic needles that painlessly penetrate just below the skin surface to sample interstitial fluid. Unlike traditional blood draws, they can continuously monitor biomarkers over hours or days. A 2025 Nature Communications study demonstrated a dual-sensor microneedle that tracks both glucose and metformin simultaneously, feeding real-time data to a smartphone app. The technology is still primarily in the research stage, but CES 2026 showed commercial versions for sweat-based lactate monitoring are approaching market readiness.
What wearable health patches were shown at CES 2026?
The PF-Sweat Patch from Point Fit Technology won a CES 2026 Innovation Award for its sweat-based lactate monitoring using nanomembrane technology, with plans for cortisol and glucose measurement in future versions. Abbott showed its AI-powered Libre Assist feature for personalized meal-glucose predictions. The Peri wearable demonstrated a torso-worn patch for detecting menopausal symptoms. The overall trend was toward multi-biomarker platforms that go well beyond glucose monitoring.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.