A $1,500-per-night test got replaced by a ring on your finger
Polysomnography remains the gold standard for measuring sleep. It captures brainwaves, eye movements, muscle activity, heart rhythm, and breathing patterns simultaneously. It also costs over $1,500 per night in the United States, requires a trained technician, and involves sleeping in a laboratory wired to electrodes. For decades, anyone who wanted objective data about their sleep had exactly one option, and it was neither affordable nor repeatable.
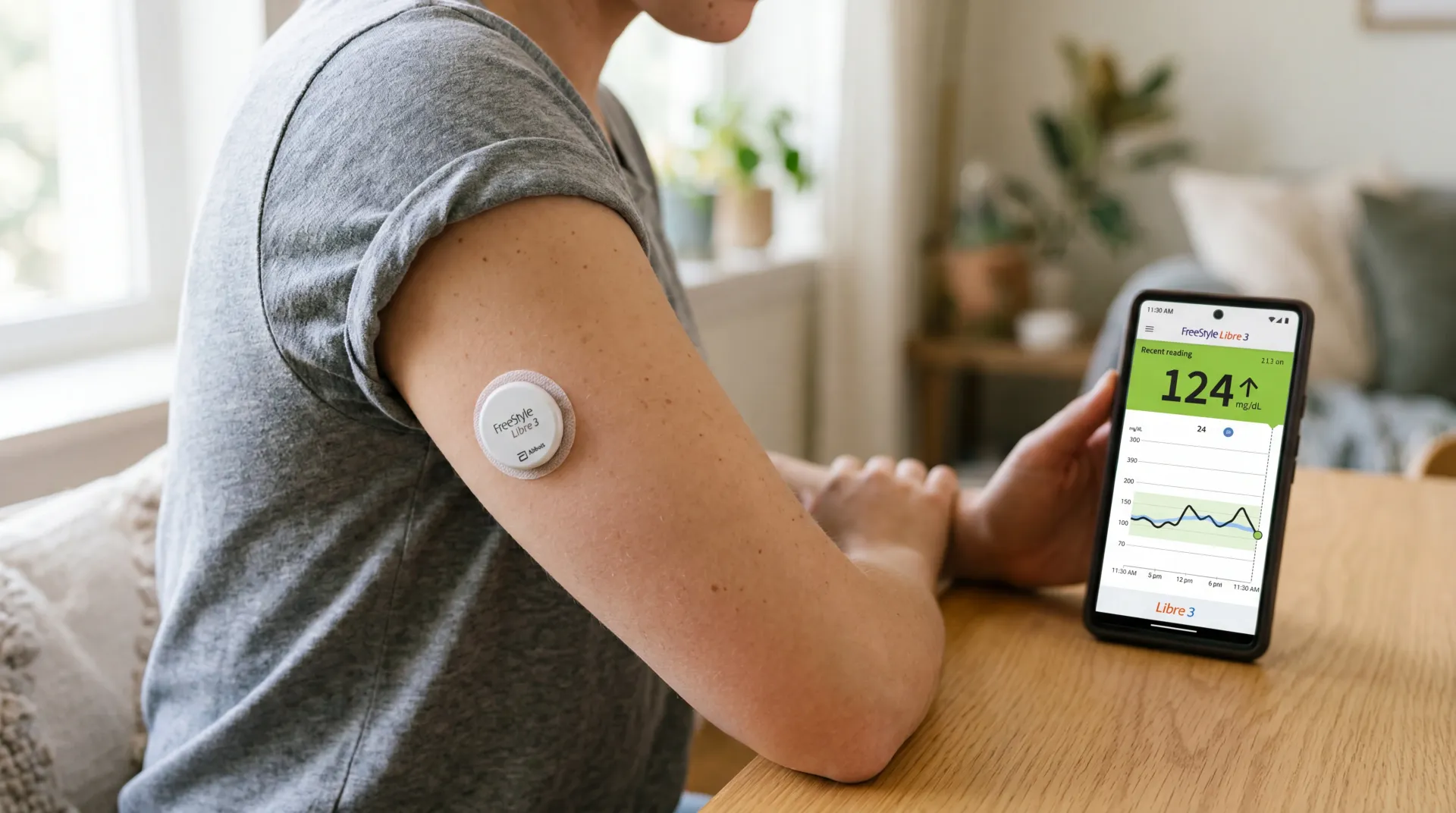
Consumer wearables changed that equation. Today, roughly 30% of American adults use a wearable device to collect health data, and sleep tracking has become one of the primary reasons people buy them. The shift happened gradually: early fitness bands from the 2010s used accelerometers to guess when you were asleep based on whether you were moving. The approach was crude. If you lay still reading a book, the device counted it as sleep. If you thrashed around during a nightmare, it might register you as awake.
The numbers tell the story of demand. A 2019 global survey found that 80% of adults wanted to improve their sleep quality, and by 2025, 37% of American adults reported dissatisfaction with their sleep. Meanwhile, over 70 million Americans have a diagnosed sleep disorder and a third get less than seven hours per night. The market responded. In 2019, wearable sleep trackers represented 44% of global smart sleep-tracking products.
But the real transformation is not that these devices got cheaper or smaller. It is that they stopped being passive observers. The newest generation of sleep technology does not just record what happened last night. It intervenes during the night, adjusting temperature, vibration patterns, and environmental conditions based on what its sensors detect in real time. Think of it like the difference between a security camera and an actual security guard: one watches, the other acts.
That distinction between watching and acting is where the technology stands right now, and it raises a set of questions that the first generation of Fitbits never had to answer.

Your ring collects the data, but a neural network decides what it means
When you check your sleep score in the morning, the number you see has been processed through multiple layers of artificial intelligence before it reaches your screen. The raw signals your wearable captures, including heart rate variability measured by photoplethysmography, wrist movement from accelerometers, and skin temperature from thermistors, are fed into machine learning models that attempt to classify each 30-second chunk of your night into a sleep stage.
The most common approach uses convolutional neural networks. A 2025 scoping review published in JMIR examined 46 studies on AI-powered wearable devices for sleep disorders and found that convolutional neural networks appeared in 37% of studies, followed by random forest models at 30% and support vector machines at 26%. The studies relied on respiratory data as the primary input in 54% of cases, heart rate data in 48%, and body movement in 37%.
A research team at the University of Massachusetts built an open-source sleep staging framework specifically for the Apple Watch. Their long short-term memory (LSTM) model, trained on data from 47 healthy adults who wore Apple Watch Series 6 units for up to seven consecutive nights, achieved 71% accuracy when classifying every 30-second epoch into four stages: wake, light sleep, deep sleep, and REM sleep. That might sound modest, but consider the comparison: two independent human technicians scoring the same PSG recording agree with each other only about 80% of the time.
Consider the scale. Samsung reported collecting over 716 million nights of sleep data through its Galaxy Watch series between June 2021 and May 2023. Each of those nights feeds back into model training, helping the algorithm handle edge cases: the person who sleeps with a cat on their chest, the shift worker whose 2 PM bedtime looks nothing like a standard night, the 70-year-old whose sleep architecture bears little resemblance to the 25-year-olds the model was originally trained on.
There is a gap between what AI can do with sleep data in research papers and what it actually does on your wrist. Academic teams publish models with specific accuracy metrics against PSG. Companies adapt these approaches into proprietary algorithms, but the specifics are almost never disclosed. You get a sleep score. You do not get to see the model's confidence intervals, its known failure modes, or how last week's software update redefined what "deep sleep" means for your particular device.
Rings, watches, bands, and mattress sensors are measuring the same signals differently
The wearable sleep tracking market has fragmented into distinct form factors, each with trade-offs that matter more than marketing materials suggest. Wrist-worn devices dominate, representing more than 58% of the wearable sleep tracking segment as of 2024, but rings, mattress sensors, and bedside devices are each carving out a niche.
The most rigorous head-to-head comparison comes from Dr. Rebecca Robbins and colleagues at Harvard Medical School and Brigham and Women's Hospital, who tested three devices against PSG in 35 healthy adults during a single-night inpatient study. Their findings, published in 2024:
| Device | Sleep vs. wake sensitivity | Sleep stage sensitivity | Sleep stage precision | Notable bias |
|---|---|---|---|---|
| Oura Ring Gen3 | 95%+ | 76.0-79.5% | 77.0-79.5% | Not significantly different from PSG in any stage |
| Fitbit Sense 2 | 95%+ | 61.7-78.0% | 72.8-73.2% | Overestimated light sleep by 18 min, underestimated deep sleep by 15 min |
| Apple Watch Series 8 | 95%+ | 50.5-86.1% | 72.7-87.8% | Underestimated deep sleep by 43 min, overestimated light sleep by 45 min |
A couple of things stand out. All three devices perform well at the most basic task: figuring out whether you are asleep or awake (sensitivity of 95% or higher). The real challenge is sleep staging, where the Oura Ring performed most consistently across stages, while the Apple Watch showed the widest performance range.
A living systematic review and meta-analysis of Apple Watch accuracy, published in 2026, synthesized data from 82 studies involving 430,052 participants. It found moderate accuracy for sleep metrics and confirmed that heart rate measurement showed a mean bias of only -0.27 beats per minute, meaning the watch is reliable for cardiac signals even if its sleep stage classification is less precise. The Apple Watch is also the most widely owned wearable device globally, with over 100 million users.
Mattress sensors and bedside devices take a different approach entirely. Instead of measuring signals from your body directly, nearables like the Withings Sleep Mat detect movement, heart rate, and respiration through a sensor placed under the mattress. Bedside devices like the SleepScore Max use sonar to track breathing and movement from across the room. They avoid the discomfort of wearing something to bed, but their distance from the body means less direct physiological data.
What none of these comparisons capture is how the devices perform over weeks and months of real-world use, which is the entire point of consumer sleep tracking. Validation studies typically cover one to seven nights in controlled conditions. Your actual sleep involves travel, alcohol, illness, stress, sharing a bed, and a hundred other variables that lab studies deliberately exclude.
Your bed now adjusts its temperature based on what sleep stage you are in
Passive tracking tells you what happened. Active optimization tries to change what is happening while you are still asleep.
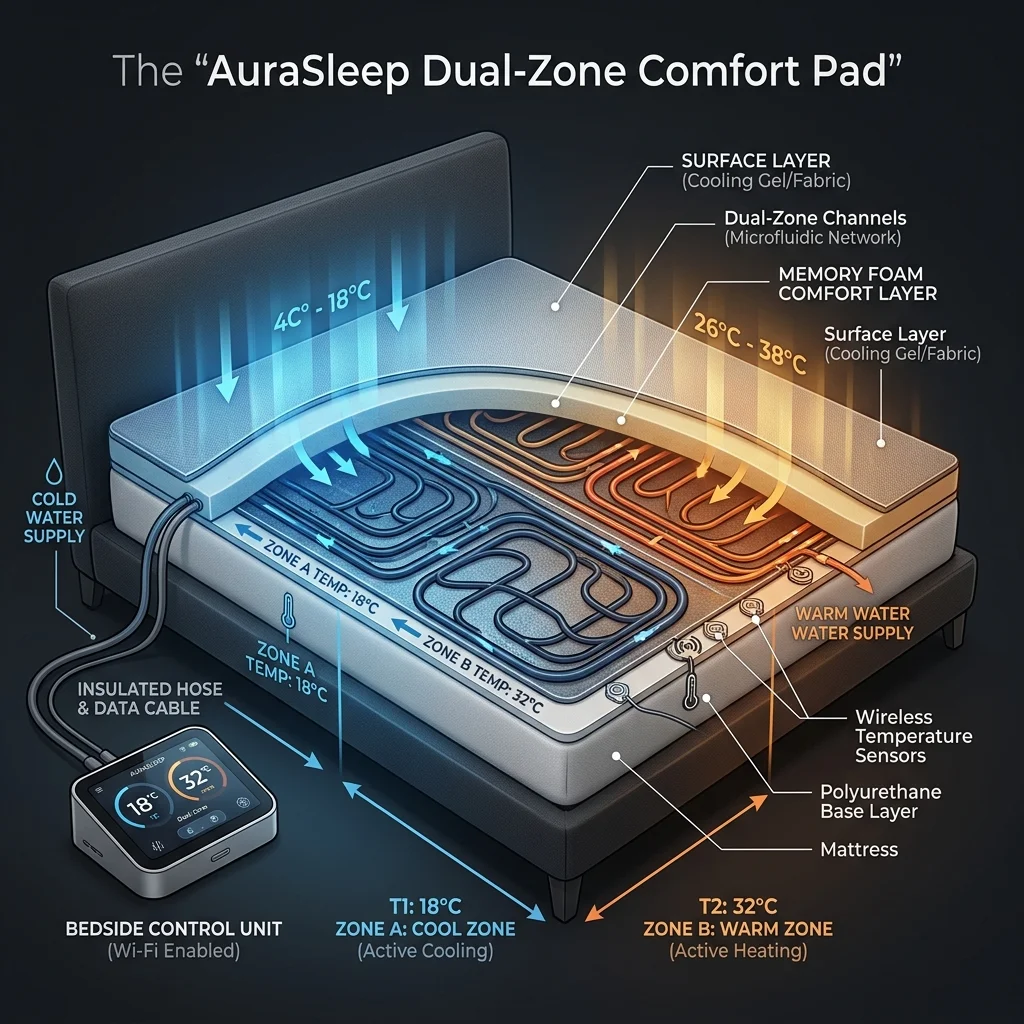
The science behind it starts with thermoregulation. Maintaining skin temperatures within 33.5 to 35.5 degrees Celsius during sleep is considered optimal. Deviations outside this range increase sleep disturbances, reduce deep sleep time, and cut total sleep duration. Your body naturally drops its core temperature as you fall asleep and continues cooling during deep sleep, then warms slightly during REM periods. The problem: bedrooms, mattresses, blankets, and bed partners all interfere with this thermal regulation.
Dr. Nicole Moyen and colleagues conducted the first controlled study of the Eight Sleep Pod, a temperature-regulated mattress cover that allows each side of the bed to be set independently between 13 and 43 degrees Celsius. Fifty-four subjects slept with the device for eight nights each with temperature regulation on and off. The results were statistically significant: men sleeping at cooler temperatures in the first half of the night gained an additional 14 minutes of deep sleep, a 22% mean increase (p=0.003). Women sleeping at warmer temperatures in the second half saw 9 additional minutes of REM sleep, a 25% mean increase (p=0.033).
The cardiovascular numbers moved too. Sleeping heart rate dropped by 2% and heart rate variability improved by 7% with temperature regulation active (p less than 0.01). Lower sleeping heart rate and higher HRV are both associated with better cardiovascular recovery.
Key finding: Women prefer approximately 1.5 to 2 degrees Celsius warmer sleep environments than men, which explains why dual-zone temperature control matters. A single thermostat for both sides of the bed is a compromise that works for neither person.
Eight Sleep's newer Autopilot system takes this further by adjusting temperature in real time based on the sleep stage it detects. A study presented at the SLEEP 2025 conference tracked 34 individuals wearing Oura Rings as a third-party measurement device. With Autopilot active, participants showed a 3% decrease in sleeping heart rate (-2.3 bpm), a 13% increase in HRV (+4.9 ms), and a 10% increase in deep sleep. The effects were most pronounced in people who started with the worst sleep: those with below-average baseline metrics saw a 16% increase in deep sleep, and women specifically saw a 19% increase in deep sleep.
The analogy here is climate control in a car versus a house. Traditional bedroom temperature management is like setting a thermostat to one temperature and hoping for the best. Active sleep optimization is closer to a car's automatic climate system that adjusts based on who is sitting where and what the external conditions are doing.
These studies are still short-term (one to two weeks), the sample sizes are modest, and the device manufacturer funded or conducted the research. But the underlying physiology is well-established: temperature affects sleep architecture. The question is whether active management of that temperature can produce durable improvements, and that data simply does not exist yet.
Your tracker is 95% right about whether you slept, and much less right about how
The gap between total sleep detection and sleep stage classification is the central tension in wearable sleep technology. Every major device on the market can tell you, with reasonable confidence, whether you were asleep or awake. The trouble begins when they try to tell you what kind of sleep you were getting.
A 2026 study by Dr. Rebecca Spencer's team at the University of Massachusetts tested four consumer devices (Fitbit Sense 2, Oura Ring, Withings Sleep Mat, SleepScore Max) against full PSG in both younger and older adults. The findings exposed a significant age-related accuracy problem. In older adults (ages 56-80), every device substantially underestimated total sleep time: the Oura Ring was off by 75.5 minutes (p less than 0.0001) and the Fitbit by 74.5 minutes (p=0.012).
Worse, the devices told older users the opposite of what was actually happening with their deep sleep. The Withings Sleep Mat overestimated deep sleep by 97.4 minutes (p less than 0.0001), and the SleepScore Max by 88.8 minutes (p less than 0.0001). This is not a minor calibration issue. An older adult checking their sleep data could see reassuring deep sleep numbers while their PSG would show the opposite pattern.
| What trackers measure well | What trackers get wrong |
|---|---|
| Total sleep time (in healthy young adults) | Deep sleep duration (especially in older adults) |
| Sleep vs. wake detection (95%+ sensitivity) | Wake after sleep onset (underestimated) |
| Heart rate during sleep (-0.27 bpm bias) | Sleep stage transitions |
| General sleep patterns over time | Single-night accuracy for clinical decisions |
The reasons are straightforward. Consumer wearables rely on proxy signals (movement, heart rate, temperature) rather than brainwaves. During deep sleep, your body is still and your heart rate drops, but these same patterns can occur when you are simply lying quietly awake. Older adults spend more time in lighter sleep stages and wake more frequently, but their physiological signals during these transitions are subtler. The algorithms, trained primarily on data from younger populations, misread these patterns.
Here is where the comparison to PSG itself is instructive. Even trained PSG technicians only agree with each other about 80% of the time when scoring the same recording. Sleep staging is inherently ambiguous at the boundaries between stages. A wearable that agrees with PSG 71-79% of the time is operating within shouting distance of human expert disagreement, but it is doing so from much less information.
A 2021 study found that sleep trackers accurately identified deep sleep only 59% of the time. That number has improved with newer algorithms and hardware, but the fundamental limitation persists: no amount of machine learning can extract brainwave-level information from a wrist-mounted accelerometer and optical heart rate sensor. The FDA does not regulate sleep trackers, so there are no minimum accuracy standards these devices must meet before reaching consumers.
For the average user tracking trends over weeks, this level of accuracy is probably useful. If your deep sleep percentage drops from 20% to 12% over a month, something has likely changed, even if neither number is perfectly calibrated. For anyone making specific health decisions based on a single night's data, the error margins are too wide to be reliable. Dr. Spencer's team concluded that "wearable and nearable consumer sleep-tracking devices should be used with caution in older adults."
Your sleep data is health data that nobody is required to protect
Every night you wear a sleep tracker, you generate a detailed physiological profile: when you went to bed, how long it took to fall asleep, your heart rate throughout the night, how often you woke up, your heart rate variability patterns, and estimated time in each sleep stage. Over weeks and months, this data can reveal stress levels, alcohol consumption patterns, illness onset, medication effects, and potential sleep disorders. It is, by any reasonable definition, health data.
It is also, by current law, largely unprotected. HIPAA does not cover wearable health data. The law applies only to "covered entities" like hospitals, insurance companies, and their business associates. Your sleep tracker manufacturer is none of those things. As a 2026 analysis in the UCLA Law Review put it: identical health information may be protected in a hospital setting but unprotected when collected through a smartwatch.
This is not a theoretical concern. A Federal Trade Commission study found that more than 12 mobile health applications and devices transmitted healthcare information to 76 third parties, including information that could be traced back to specific users.
Congress has noticed. Senator Bill Cassidy, chair of the Senate HELP Committee, introduced the Health Information Privacy Reform Act (HIPRA), which would require wearable developers to inform users that HIPAA does not protect their data and offer an option to prevent data sharing. Several states have moved independently: Washington requires entities collecting consumer health data to maintain transparent privacy policies and obtain consent, Connecticut imposed similar obligations, and California's CCPA gives residents the right to know what data is collected and opt out of its sale.
The regulatory patchwork means protection depends on where you live. A sleep tracker user in California has meaningful privacy rights. The same user in a state without consumer health data protections has essentially none beyond whatever the manufacturer's terms of service promise.
The privacy gap: Samsung collected 716 million nights of sleep data through its Galaxy Watch between 2021 and 2023. That dataset, aggregated from millions of users, has enormous commercial and research value. Users contributed it passively by wearing their watches to bed.
There is also a psychological cost to all this data. Dr. Kelly Glazer Baron at Rush University Medical Center coined the term "orthosomnia" in 2017 to describe patients who became preoccupied with perfecting their sleep tracker data. In her case studies, patients spent excessive time in bed trying to improve their tracker scores, which actually worsened their insomnia symptoms. One patient trusted her Fitbit data over her own polysomnogram results, asking "Then why does my Fitbit say I am sleeping poorly?" after a sleep study showed she was getting more deep sleep than average for her age.
This is more common than it sounds. Researchers estimate that about 20% of adults own a fitness tracker, and the obsessive pursuit of perfect sleep metrics is becoming common enough that clinicians are developing formal measurement scales for it. As behavioral sleep therapist Katie Fischer observed in The Guardian, "If you ask good sleepers what they do, they will usually say nothing. They're not thinking about sleep."
None of this means sleep tracking is harmful. But the data deserves the same skepticism you would apply to any single health measurement. Trends over weeks matter more than individual nights. How you feel after waking up is a data point your tracker cannot capture. And the information you generate about your sleep every night has value to people other than you, whether or not you have decided to share it.

Frequently Asked Questions
How accurate are consumer sleep trackers compared to a clinical sleep study?
Consumer sleep trackers are good at detecting whether you are asleep or awake, with sensitivity of 95% or higher across major devices. Sleep stage classification is less reliable. The Oura Ring achieves 76-79.5% sensitivity for sleep stages, while the Apple Watch ranges from 50.5-86.1% depending on the stage. These numbers are most accurate in healthy younger adults and become significantly less reliable in older adults.
Can a temperature-controlled mattress actually improve my sleep?
Peer-reviewed research suggests yes, with caveats. A controlled study of 54 subjects found that temperature-regulated sleep surfaces increased deep sleep by 22% in men and REM sleep by 25% in women, with improvements in heart rate and heart rate variability. However, these studies covered only one to two weeks, and the long-term durability of these effects is unknown.
Is my sleep tracker data protected by health privacy laws?
HIPAA does not cover data collected by consumer wearables. Protection depends on your state of residence. California, Washington, and Connecticut have consumer health data protections. Federal legislation (the HIPRA Act) has been proposed but not yet passed. Review your device manufacturer's privacy policy and data sharing practices.
What is orthosomnia and should I be concerned about it?
Orthosomnia is a term coined in 2017 by researchers at Rush University Medical Center describing an obsessive pursuit of perfect sleep tracker metrics that paradoxically worsens sleep quality. Warning signs include checking your sleep data first thing every morning, feeling anxious about low scores, and spending excessive time in bed to boost your numbers. If tracking your sleep causes more stress than insight, consider taking breaks from the data.
Which sleep tracker form factor is most accurate: ring, watch, or mattress sensor?
In the only published head-to-head comparison against PSG including all three types, the Oura Ring (finger-worn) showed the most consistent accuracy across sleep stages, with no statistically significant differences from PSG. Wrist-worn devices (Fitbit, Apple Watch) tended to overestimate light sleep and underestimate deep sleep. Mattress sensors avoid comfort issues but showed the largest deep sleep overestimation (up to 97 minutes in older adults).
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.