Quick start: If you only make one change, pair most starches with protein, fiber, and healthy fat. That single move usually softens blood sugar spikes more than chasing perfect GI numbers.
What the Glycemic Index Really Measures
The glycemic index (GI) ranks carbohydrate-containing foods by how quickly they raise blood glucose after eating. The concept is useful, but it is often simplified too much. GI testing is done under controlled conditions using a fixed amount of available carbohydrate, then compared with a reference food such as glucose. If you want the full technical definition, the NIH Endotext overview of GI and glycemic load explains the testing method and why results vary by food type and preparation.
In practice, GI is not a “good food vs bad food” label. It is a speed signal. Faster-digesting carbs usually have higher GI values, while slower-digesting foods with more fiber, intact structure, or natural fat and protein usually have lower values. The University of Sydney glycemic index database remains one of the best practical references for comparing specific foods and brands.
Clinically, GI can matter for people with prediabetes, type 2 diabetes, insulin resistance, and anyone trying to reduce energy crashes. But GI is one part of a bigger picture that includes portion size, total carbohydrate intake, dietary pattern quality, sleep, stress, and activity level.
| GI Range (glucose = 100) | Category | What It Usually Means | Examples |
|---|---|---|---|
| 55 or below | Low GI | Slower rise in blood glucose | Lentils, chickpeas, many non-starchy vegetables, most nuts, plain yogurt |
| 56 to 69 | Medium GI | Moderate glucose response | Brown rice (varies), whole wheat products (varies), some tropical fruits |
| 70 or above | High GI | Faster glucose rise | White bread, sugary cereals, many refined snacks, glucose drinks |
If you are managing glucose actively, GI can be a strong tactical tool, especially when combined with the basics already covered in our diabetes guide.
Why Glycemic Load Often Matters More Than GI Alone
GI tells you how fast carbs are absorbed. Glycemic load (GL) tells you how much total glucose impact a realistic serving may have. That is a critical difference. A food can have a high GI but very little total carbohydrate per serving, resulting in a modest GL. Watermelon is the classic example.
GL is calculated as:
GL = (GI × grams of available carbohydrate in the serving) / 100
This is why portion size still matters. A very large serving of a low-GI food can still raise glucose substantially, while a small serving of a high-GI food may have a smaller practical effect.
The landmark International Tables of Glycemic Index and Glycemic Load Values show how dramatically GI and GL can vary across preparation methods and food forms. A separate evidence base also suggests that lower-GI dietary patterns can improve glycemic control in many people with diabetes; for example, see this systematic review and meta-analysis evaluating low-GI and low-GL diets in diabetes management.
Bottom line: GI is useful, GL makes it practical, and both work best when you apply them to your normal portions.
Low-GI Foods That Are Actually Practical
Many low-GI lists include foods people rarely buy. Instead of theoretical picks, focus on affordable staples you can eat weekly. Legumes, intact whole grains, non-starchy vegetables, and minimally processed proteins are usually the backbone of stable-energy eating.
Below is a practical low-GI shortlist that works for real kitchens, not just nutrition charts.

| Food | Typical GI Pattern | Why It Helps | Easy Use |
|---|---|---|---|
| Lentils | Low | High fiber and protein slow digestion | Add to soups, grain bowls, or taco filling |
| Chickpeas | Low | Fiber-rich with steady energy release | Use in salads or blend into hummus |
| Steel-cut oats | Low to medium | Less processed than instant oats | Cook in batches for quick breakfasts |
| Plain Greek yogurt | Low | Protein blunts glycemic response | Pair with berries and nuts |
| Berries | Low | Lower sugar density and high polyphenols | Top oats or yogurt |
| Nuts and seeds | Low | Fat, protein, and fiber combination | Small handful with fruit |
| Broccoli and leafy greens | Very low | High volume, low carb density | Fill half the plate with vegetables |
| Al dente pasta | Lower than overcooked pasta | Texture slows digestion | Combine with protein and vegetables |
If you want extra recipe ideas around legumes and whole-food proteins, see our post on pulses and metabolic health.
One caveat: low-GI does not automatically mean nutrient-dense. Some low-GI processed foods still carry high sodium, low fiber quality, or unhelpful additive profiles. Use ingredient quality as your first filter, then GI as the second.
High-GI Foods That Spike Quickly
High-GI foods are not “forbidden,” but they are easier to overeat and more likely to create rapid glucose swings, especially when eaten alone. Typical examples include refined breads, sugary drinks, many breakfast cereals, candy, and starchy foods cooked in ways that increase digestibility.
The broader cardiometabolic context matters here: higher intakes of refined carbohydrates and added sugars are consistently linked with poorer health outcomes in many populations. The American Heart Association overview on simple carbohydrates, the CDC guidance on healthy eating with diabetes, and the WHO diabetes fact sheet all support reducing highly refined carbohydrate patterns and prioritizing whole foods.

| Common High-GI Choice | Why It Spikes Fast | Lower-GI Swap | Simple Upgrade |
|---|---|---|---|
| Sugary breakfast cereal | Highly processed starch + added sugar | Steel-cut oats or unsweetened muesli | Add chia seeds and plain yogurt |
| White toast with jam | Refined flour with low fiber | Sprouted grain toast | Add eggs or nut butter |
| Sweetened sports drink | Rapid liquid sugar absorption | Water or unsweetened electrolyte option | Use sugar only for true endurance sessions |
| Instant mashed potatoes | Highly gelatinized starch | Roasted potatoes with skin | Cool and reheat for more resistant starch |
| Pastries | Refined flour + sugar + low satiety | Fruit + nuts + protein | Reserve pastries for occasional treats |
This does not mean you can never eat high-GI foods. They are strategically useful in some settings, such as rapid treatment of hypoglycemia or targeted post-exercise refueling for endurance athletes. The key is context, serving size, and what else is on the plate.
Why the Same Carb Hits People Differently
Two people can eat the same meal and see very different glucose curves. Even the same person can have different responses from one day to the next. Reasons include insulin sensitivity, sleep quality, stress hormones, movement after meals, medication timing, and gut microbiome differences.
The NIDDK insulin resistance resource explains why underlying metabolic status changes how the body handles carbohydrate exposure. This is exactly why “average GI values” are helpful but never perfect.
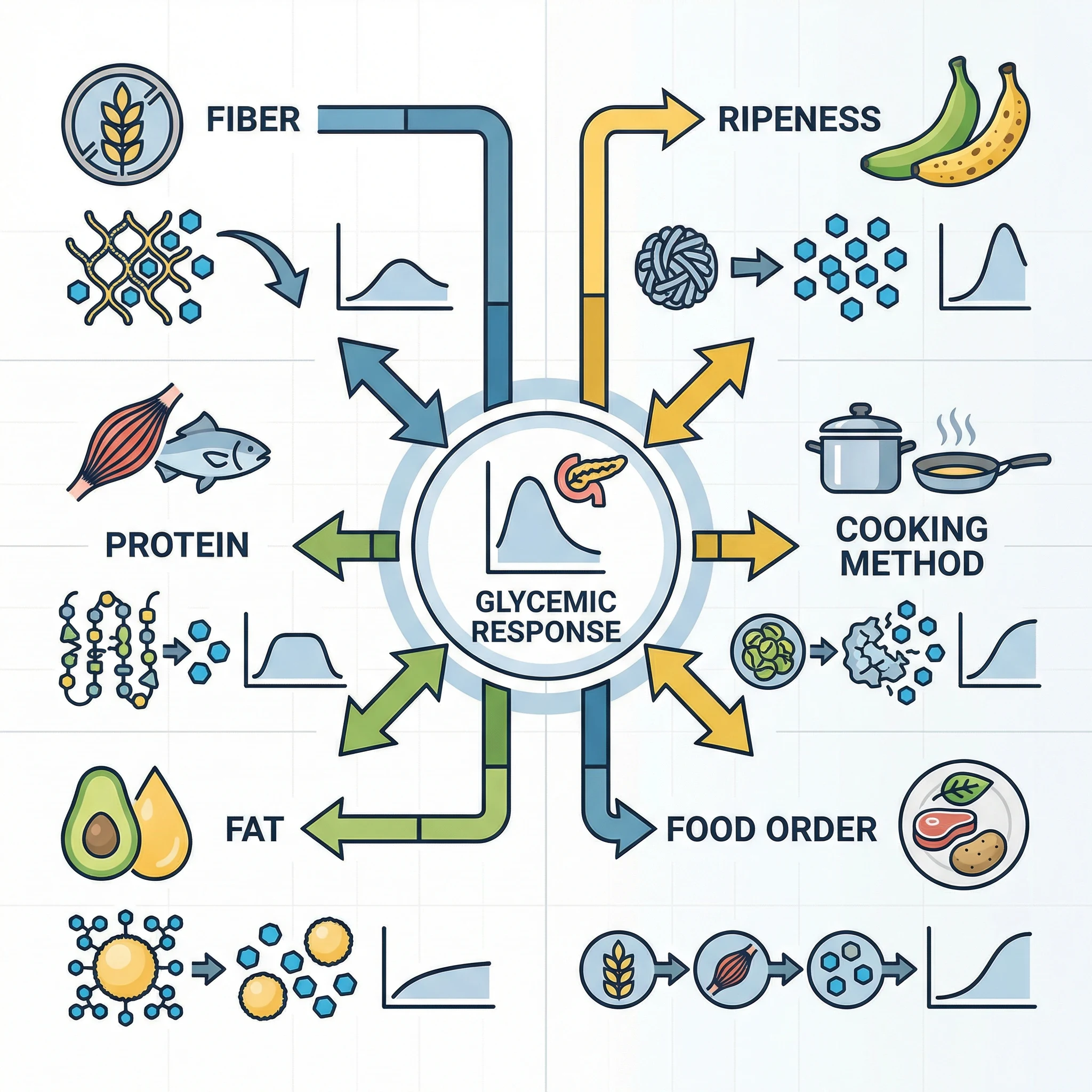
Food properties also shift glycemic impact:
- Fiber: Higher soluble fiber slows gastric emptying and carbohydrate absorption.
- Protein and fat: Mixed meals generally blunt post-meal glucose peaks versus carbs eaten alone.
- Ripeness: Riper fruit usually means faster available sugars.
- Cooking method: Longer cooking can increase starch digestibility.
- Food structure: Intact grains and legumes often digest slower than flours and purées.
- Meal order: Eating vegetables/protein before starch may reduce glucose excursions in some people.
If you already started reducing sugar dependence, our guide to a sugar-free lifestyle pairs well with GI-focused planning.
How to Build Lower-GI Meals Without Obsessing
The most sustainable approach is a repeatable meal formula. You do not need to calculate every GI number. You need a plate structure that lowers spikes by default.
Try this “3-2-1” method for most lunches and dinners:
- 3 parts non-starchy vegetables for volume and fiber.
- 2 parts protein-rich food such as fish, eggs, tofu, Greek yogurt, legumes, or poultry.
- 1 part slower carbohydrate such as lentils, beans, steel-cut oats, quinoa, or intact whole grains.
Then add one small fat source such as olive oil, avocado, tahini, or nuts. This pattern usually improves satiety and smooths glucose response. It also makes portion control easier without relying on strict calorie tracking.
For many readers, this is the bridge between broad nutrition advice and practical execution. If you want a wider food base for this style of eating, you can combine ideas from our article on diet patterns that support diabetes prevention with your preferred cultural foods.
Important nuance: lower GI does not mean low carbohydrate. It means choosing carbohydrate forms and combinations that your body handles better over time.
Myth vs Fact: Common Glycemic Index Mistakes
| Myth | Fact |
|---|---|
| “Low GI means I can eat unlimited amounts.” | Portion size still drives total glucose load; GL and meal context matter. |
| “All fruit is high GI and should be avoided.” | Many fruits have low-to-moderate GI and can fit well in balanced meals. |
| “GI alone predicts diabetes risk.” | Risk is multi-factorial; body weight, activity, sleep, genetics, and overall diet quality all matter. |
| “If a food is whole grain, it is always low GI.” | Processing level, particle size, and cooking can still produce medium or high GI responses. |
| “Artificial sweeteners solve blood sugar health automatically.” | They may reduce sugar intake short term but overall dietary pattern and behavior still determine outcomes. |
On that last point, we break down practical tradeoffs in our review of artificial sweetener risks and benefits. Substitutions can help, but the long-term goal is retraining taste preference and meal quality, not replacing one ultra-processed input with another.
Population-level evidence supports this bigger-picture view. For example, a large meta-analysis in the BMJ found associations between high free-sugar intake and cardiometabolic risk markers; see the BMJ review on sugar and health outcomes for a broad synthesis.
One-Day Low-GI Meal Blueprint
Use this example as a template and adjust portions to your needs, medications, and activity level.
| Meal | Example | Why It Works for GI/GL |
|---|---|---|
| Breakfast | Steel-cut oats + plain Greek yogurt + berries + walnuts | Fiber + protein + fat combination slows glucose rise |
| Lunch | Lentil and vegetable bowl with olive oil and herbs | Legume starch digests slowly with high satiety |
| Snack | Apple slices with peanut butter | Pairs natural carbs with fat/protein |
| Dinner | Salmon, quinoa, roasted broccoli, mixed greens | Balanced macronutrients and high fiber density |
| Optional dessert | Chia pudding with unsweetened cocoa | Lower added sugar and slower digestion profile |
If you want to personalize this further, track two weeks of meals and note your energy, hunger, and post-meal sleepiness. Even without a glucose monitor, these patterns usually show which foods are working for you.
A Three-Week Transition Plan That Sticks
Most people fail with glycemic index strategies because they try to change everything in one weekend. The better approach is a short transition cycle where each week has one clear job. This keeps friction low and helps you hold the habit long after motivation fades.
Week 1: Replace liquid sugar and refine breakfast. Remove sweetened drinks on normal workdays and build a protein-plus-fiber breakfast. This single shift often reduces afternoon cravings quickly. Think oats with yogurt and berries, or eggs with vegetables and a small fruit portion.
Week 2: Upgrade lunch carbohydrates. Keep your usual lunch format but replace refined starches with beans, lentils, or intact grains. If you currently eat white rice daily, swap in mixed portions first, then shift toward higher-fiber options over several days rather than forcing a sudden full switch.
Week 3: Build dinner around vegetables first. Before planning the starch, choose your non-starchy vegetables and protein. Add carbohydrate after that. This sequence naturally lowers total glycemic load and improves satiety at night, which can also reduce late-evening snacking.
This staged method aligns with classic international guidance on carbohydrate quality and meal composition, including the long-running FAO overview of GI and practical application in public health nutrition (FAO discussion paper on glycemic index and glycemic load).
To keep the plan realistic, set three simple metrics each week:
- Adherence metric: “How many meals followed my plate method?”
- Outcome metric: “How often did I feel a post-meal crash?”
- Recovery metric: “If I went off plan, how fast did I reset?”
That third metric is usually the most important. Sustainable nutrition is not about perfect streaks; it is about short recovery time after imperfect days. In practical terms, your target is to return to structure at the next meal, not “start over Monday.”
If you already track workouts, pair this with a 10 to 15 minute walk after your largest meal. Light post-meal movement can improve glucose handling and helps translate GI strategy into real-life physiology. You do not need intense sessions to get this benefit; consistency beats intensity for most people.
After three weeks, keep only the habits that gave visible benefits in energy, appetite control, and meal satisfaction. Drop the rest. Your long-term plan should feel repeatable, not restrictive.
Who Should Use Glycemic Index Carefully
GI is a strong educational tool, but some groups should apply it with medical context:
- People on insulin or glucose-lowering medication: abrupt carbohydrate changes can alter medication needs.
- Athletes in high-volume training: strategic high-GI carbohydrates can improve recovery and performance timing.
- People with under-eating risk or disordered eating history: strict food scoring can become counterproductive.
- Pregnancy and gestational diabetes: individualized planning with a qualified clinician is best.
GI should support your health decisions, not become an anxiety trigger. If tracking starts to feel rigid, step back to simple habits: whole foods, plate balance, regular movement, and consistent sleep.
Frequently Asked Questions
Is glycemic index the same thing as carbohydrate counting?
No. Carbohydrate counting tracks total grams of carbohydrate, while GI estimates the speed of glucose rise. You can combine both for better control: count total carbs first, then choose lower-GI options when possible.
Can I still eat potatoes and rice on a lower-GI plan?
Yes. Portion size, cooking method, and meal pairing matter. Eating smaller portions with protein, vegetables, and healthy fat usually reduces spikes compared with eating large portions alone.
Are low-GI diets proven to improve blood sugar in diabetes?
Evidence suggests they can help many people, especially when part of an overall quality diet. The strongest improvements happen when lower-GI choices are paired with sufficient fiber, weight management, and consistent activity.
Do I need to avoid fruit because of sugar?
Usually no. Whole fruit often fits well because fiber slows absorption. Problems are more likely with juices, very large portions, or fruit eaten alongside high-refined-carb meals.
What is the fastest way to lower meal glycemic impact today?
Build mixed meals: add protein and fiber to every carbohydrate source, reduce liquid sugars, and replace refined starches with legumes or minimally processed whole grains most of the week.
Related Articles
- Diabetes - A practical foundation on blood sugar regulation, warning signs, and long-term prevention strategy.
- Diets That Prevent and Help Diabetes - A broader dietary framework to pair with GI-focused food selection.
- Sugar-Free Lifestyle: Sugar Addiction Tips - Behavior-first tactics for reducing sugar dependence without extreme restriction.
- Artificial Sweeteners: Dangers and Benefits - Evidence-based pros and cons of sugar substitutes in daily life.
- List of Carbohydrate Foods for Healthier Eating - A practical carb awareness guide you can use for weekly meal planning.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.












